
Saudi Arabia

GLOBAL PRETERM BIRTH RATES – Saudi Arabia
Estimated Number Of Preterm Birth Rates – 3.96per 100 live births
(Global Average: 10.6, USA: 9.56)
Source- WHO 2014- https://ptb.srhr.org/
Saudi Arabia, officially the Kingdom of Saudi Arabia (KSA), is a country in Western Asia. It covers the bulk of the Arabian Peninsula, and has a land area of about 150,000 km2 (830,000 sq mi), making it the fifth-largest country in Asia, the second-largest in the Arab world, and the largest in Western Asia and the Middle East. It is bordered by the Red Sea to the west; Jordan, Iraq, and Kuwait to the north; the Persian Gulf, Qatar and the United Arab Emirates to the east; Oman to the southeast; and Yemen to the south. Bahrain is an island country off the east coast. The Gulf of Aqaba in the northwest separates Saudi Arabia from Egypt. Saudi Arabia is the only country with a coastline along both the Red Sea and the Persian Gulf, and most of its terrain consists of arid desert, lowland, steppe, and mountains. Its capital and largest city is Riyadh. The country is home to Mecca and Medina, the two holiest cities in Islam.
Saudi Arabia is considered both a regional and middle power.[35][36] The Saudi economy is the largest in the Middle East; the world’s eighteenth-largest economy by nominal GDP and the seventeenth-largest by PPP. As a country ranks 35th, very high, in the Human Development Index, it offers a tuition-free university education, no personal income tax, and a free universal health care system. Saudi Arabia is home to the world’s third-largest immigrant population. It also has one of the world’s youngest populations, with approximately 50 per cent of its population of 34.2 million being under 25 years old.[ In addition to being a member of the Gulf Cooperation Council, Saudi Arabia is an active and founding member of the United Nations, Organisation of Islamic Cooperation, Arab League, Arab Air Carriers Organization and OPEC.
Health care in Saudi Arabia is a national health care system in which the government provides free health care services through a number of government agencies. Saudi Arabia has been ranked among the 26 best countries in providing high quality healthcare.
Source:https://en.wikipedia.org/wiki/Saudi_Arabia

Meaningful Manifestations for 2023
As we celebrate the year of 2022 and TRANSITION into the New Year, we would like to share a few of our aspirations for advancements within our global neonatal community for 2023. Feeling passion, we desire:
- Enhanced efforts to drive strong and focused innovation in preterm birth technology, preterm birth research and prevention, targeted diagnostic and treatment options, and effective healthcare workforce development.
- Collaborative global engagement focused towards provider/patient education and support, preemie-focused developmental and time sensitive interventional care, the development of Preterm Birth Community lifespan wellness, and focused health care/resource access for our global pre-term birth survivor community (10-12% of our total global population).
- Comprehensive research and associated development of effective diagnostics and impactful treatment for preterm birth related preverbal PTSD effecting preterm birth survivors of all ages.
- Longitudinal research targeted towards investigation of the gestational neurological development of the preterm birth population, with increased identification of gestational development and advanced cohort/diagnostic classifications in order to improve diagnostics, treatment planning, and best practices supporting neonatal health outcomes.
- Expansion of healthcare provider specialization in medical and mental health care targeting pediatric and adult preterm birth survivor needs and resources.
- Advancements towards holistic, comprehensive, and accurate diagnostic care management of preemie neurological development, health and wellness conditions free from potentially harmful bias and assumptions that similar symptom presentation in preterm neonates vs. non equates to similar diagnoses, etiology, treatment and time sensitive interventions.
Furthermore:
We stand firmly in the expectation that as innovation, technology, diagnostics, research, integrated care management, and global collaboration expands within the preterm birth community we will witness improvements in the quality of life for all members of our global preterm birth family.
Kathy, Kat, and our cat Gannon anticipate that 2023 will lead to the joyful amplification and manifestation of our shared hopes, wishes, dreams and more within the Global Neonatal Womb/Preterm Birth Community! Wishing us all a Joyful, Love-filled, Healthy, Satisfying, and Adventurous 2023!


COMMUNITY

Lack of innovation in neonatal respiratory care is the biggest problem for both preterm and term neonates: to be remembered on World Prematurity Day
Daniele De Luca 09 NOV 2022 https://doi.org/10.1152/ajplung.00323.2022
This is an editorial commissioned to the President of the European Society for Pediatric and Neonatal Intensive Care, on the occasion of World Prematurity Day 2022. It celebrates this important event by summarizing how the most crucial (and forgotten) problem in neonatal respiratory care is the lack of active translational research. Translational research is pivotal in this context, as it allows to understand the diseases, diagnose them, and imagine new strategic pathways. The lack of translational research means no innovation, and this is jeopardizing the possibility to improve healthcare for both preterm and term critically ill neonates. Historical and more recent examples of the problem are given, together with some basic suggestions to move forward.
On November 17 every year, many countries celebrate World Prematurity Day. Purple is the color of the initiative; thus, hospitals and monuments are highlighted, whereas gadgets and people show something with this color. Since 2011, this fruitful initiative succeeded in raising the attention on the problems related to prematurity, particularly on the care of preterm babies and the important role of parents. This is a commendable and needed initiative. In fact, neonatal care risks being perceived as something taken for granted in the Western world, where birth rates and infant mortality are low and the main current health problems, particularly in the COVID-19 era, are those of the adult age and elderly.
However, we cannot forget that preterm neonates are not the only ones at risk, and, as a matter of fact, the most crucial issue for neonatal medicine has been forgotten. In fact, although many focus on preterm developmental care and parental role, we must admit that neonatology has not meaningfully improved its global clinical results, as there have not been many relevant innovations in the last two decades.
This is particularly true for neonatal respiratory critical care which is, together with hemodynamics, the core problem to be addressed for most patients in life-threatening situations. After the introduction of prenatal steroids and surfactants, we have seen no other game changers for preemies. The situation is even worse for term neonates since the last improvement has been represented only by the introduction of whole body hypothermia for perinatal asphyxia. Thus, we still lack effective drugs and clear diagnostic-therapeutic strategies for bronchopulmonary dysplasia as well as for other disorders more typical of term neonates, such as refractory pulmonary hypertension or congenital diaphragmatic hernia and other congenital lung disorders.
The reasons behind this lack of innovation are many. The regulatory procedures are too strict, time-consuming, and do not consider the peculiarities of the newborn patient and the rarity of his diseases. They are supposed to protect the patient from “wrong” innovations, but they forgot to protect him from the lack of innovation, i.e., the unavailability of drugs or medical devices. Surfactant was intensively studied in the 1980s, following animal and bench experiments performed by Mary Allen Avery and Bengt Robertson. Most likely, this would be extremely difficult, if not impossible, with current regulations, and, if these basic experiments would have been needed today, no surfactant would be available.
The neonatal market is smaller than that represented by several adult medicine specialties, and the relatively low neonatal mortality has decreased the interest of many public grant programs; as a combination of these two factors, neonatal research often lacks specific funding and this is particularly true for respiratory research. Most of the neonatal ventilation research is done without public or industry fundings ; in other words, without the charities and the dedication of researchers, we would not have several respiratory support techniques such as the newest noninvasive ventilation modalities. Other cases are less lucky: some respiratory drugs [including potentially life-saving pulmonary vasodilators do not achieve enough clinical evidence, because they are not suitable from a marketing point of view (i.e., low price, rare use) despite strong translational and clinical data supporting them.
Nonetheless, we shall admit that, besides these problems, the difficulties in finding new solutions for neonatal respiratory care are also due to our own carelessness about what has been learned in close fields, such as anesthesiology, intensive care medicine, regenerative medicine, transplantation surgery, and other fields of adult healthcare. Neonatal respiratory care, and neonatology in general, has suffered a lack of cross-disciplinary awareness that has prevented or delayed important advancements. The reason behind this was the supposition that the neonate was completely distinct from all other patients; newborn physiology may be different in some aspects, but this cannot prevent to recognize similitudes and take advantage from experience accumulated in other fields. In 1964, Gilbert Hualt provided mechanical ventilation for the first time to a newborn infant with congenital tetanus. Without his vision, the introduction of neonatal ventilation would have been delayed; ironically, this technique is now considered the basis of intensive care. How many of us have the same vision regarding strategies, tools, and research lines investigated in adult respiratory care? I still remember a professor stating, no more than 15 years ago, that applying ECMO to neonates was technically impossible. Lung transplantation in neonates and infants is still regarded as an extreme procedure, but some centers practice it with satisfactory results. Are we enough interested in artificial organs and regenerative medicine applied to neonatal respiratory disorders?
The examples are countless and the combination of all these factors leaves many neonatal disorders without a full understanding of their pathobiology and orphan of diagnostic-therapeutic tools; this creates relevant clinical unmet needs.
Despite all of these problems, some innovations have been achieved, such as the recognition of neonatal acute respiratory distress syndrome (an entity that was forgotten for several decades; and the implementation of point-of-care lung ultrasound, following the adult intensive care experience (although its diffusion is still variable among countries. Nonetheless, translational research is essential if we really want to fill the many clinical unmet needs. Translational projects are important to understand the mechanisms of disease, how to “intercept” them with diagnostic tools, how to personalize the treatment as much as possible and to discover new therapeutic possibilities. Thus, neonatal translational research, particularly in the respiratory field, must receive greater attention, be facilitated in the regulatory process, and take advantage from quicker industry-academy and cross-disciplinary collaborations. The work might not be exclusively unidirectional. As neonates today are the patients of tomorrow, good results achieved by neonatal research can impact on patient health for several decades ahead. Although we celebrate World Prematurity Day, we shall remember that the actual main problem, both for preterm and for full-term neonates, is that there is no future without active research.
Source:https://journals.physiology.org/doi/full/10.1152/ajplung.00323.2022

US gets D+ grade for rising preterm birth rates, new report finds
By Jacqueline Howard, CNN Published 8:00 AM EST, Tue November 15, 2022
The US preterm birth rate peaked in 2006 at 12.8%, according to data from the National Center for Health Statistics.
Since then, some March of Dimes reports have found US preterm birth rates much higher than 10.5%, but those rates were based on calculations that have since been updated, according to March of Dimes.
“There are too many babies being born too soon: 1 in 10. If you were to have 10 babies in front of you and one of them is having to face the complications that comes with prematurity, that’s unacceptable, and we need to do better,” Henderson said, adding that those 1 in 10 are more likely to be Black, American Indian or Alaska Native.
March of Dimes data in the new report shows that infants born to Black and Native American mothers are 62% more likely to be born preterm than those born to White women.
States with the highest and lowest rates
The new March of Dimes report also highlighted state-by-state differences in the rate of babies born prematurely across the country.
The report grades a preterm birth rate less than or equal to 7.7% as an A and a preterm birth rate greater than or equal to 11.5% as an F.
The national preterm birth rate of 10.5% is graded as a D+.
No state has achieved an A rate, and only one has a state-level preterm birth rate that would be graded as an A-: Vermont, which has the lowest preterm birth rate in the US at 8%.
Meanwhile, nine states and one territory have preterm birth rates that received an F grade: Georgia and Oklahoma with 11.9%; Arkansas, Kentucky and Puerto Rico with 12%; South Carolina with 12.1%; West Virginia with 12.8%; Alabama with 13.1%; Louisiana with 13.5%; and Mississippi with the highest preterm birth rate of all states at 15%.
“The areas that have the worst grades are the same areas we’ve been seeing consistently for a long time, and it’s past time for us to do what we need to do to make health better and make our country a better place to give birth and be born,” Henderson said. “It’s unfortunate that we don’t have policies in place to protect the most vulnerable in our country, and without protecting our moms and babies, we can’t secure the health of everyone else.”
To address these state-by-state disparities in preterm births and help improve the national preterm birth rate as a whole, March of Dimes has been advocating for certain policies, Henderson said, including the Black Maternal Health “Momnibus” Act of 2021, a sweeping bipartisan package of bills to provide pre- and postnatal support for Black mothers – but most of the bills in the package are still making their way through Congress.
March of Dimes also has been urging more states to adopt legislation expanding access to doulas and midwives, among other maternal health care services, and reduce the prevalence of maternity care deserts across the country.
How Covid-19 plays a role
There are many potential factors contributing to the nation’s rising preterm birth rate, and Henderson said the Covid-19 pandemic remains one of the biggest.
“We cannot forget about the impact of the Covid-19 pandemic and recognize that there is likely a huge contribution of that, knowing that Covid-19 infection increases the risk of preterm birth,” she said. “But we also know that this pandemic brought many other issues to the forefront, knowing that issues around structural racism and barriers to adequate prenatal care, issues around access, were brought to the forefront during this pandemic as well.”
She added that many mothers in the United States are starting pregnancies later in life, and there has been an increase in mothers with chronic health conditions, who are at higher risk of having to give birth early due to pregnancy complications.
Pregnant women with Covid-19 may be at increased risk of preterm delivery, CDC study suggests
Henderson also said that preterm birth is one of the top causes of infant deaths and disproportionately affects babies born to women of color.
“The United States is one of the worst places to give birth and be born among industrialized countries, unfortunately. When we look at maternal deaths and infant deaths, we’re at the bottom of the pack among countries with similar profiles in terms of gross domestic product,” Henderson said. “It’s because of our disproportionate numbers of preterm births –particularly for populations that are disproportionately impacted, such as Black families and American Indian and Alaskan Native families – that our rates are so much higher than other countries.”
An ‘urgent public health issue’
Globally, about 10% of births are preterm worldwide – similar to the US preterm birth rate.
About 15 million babies are born preterm each year, amounting to more than 1 in 10 of all births around the world, according to the World Health Organization, which has called prematurity an “urgent public health issue” and “the leading cause of death of children under 5.”
Separate from the March of Dimes report, WHO released new guidelines Tuesday on how nations can improve survival and health outcomes for babies born too early, at 37 weeks of pregnancy or less, or too small, at 5½ pounds or less.
These WHO recommendations advise that skin-to-skin contact, also known as kangaroo mother care, be provided to a preterm infant immediately after birth, without any initial time spent in an incubator.
“Previously, we recommended that kangaroo mother care to only be for babies that were completely stable,” said pediatrician Dr. Karen Edmond, medical officer for newborn health at WHO, who was the lead on the new guidelines.
“But now we know that if we put babies in skin-to-skin contact, unless they are really critically ill, that this will vastly increase their chances of surviving,” she said. “So what’s new is that we now know that we should provide kangaroo mother care immediately after birth, rather than waiting until the baby’s stable.”
Edmond added that immediate kangaroo mother care can help infants better regulate their body temperature and help protect against infections, and she said that these guidelines are for on-the-ground health care providers as well as families.
The new WHO guidelines also recommend that emotional, financial and workplace support be provided for families of babies born too early or at low birth weights.
“Preterm babies can survive, thrive, and change the world – but each baby must be given that chance,” WHO Director-General Tedros Adhanom Ghebreyesus said in a news release.
“These guidelines show that improving outcomes for these tiny babies is not always about providing the most high-tech solutions,” he said, “but rather ensuring access to essential healthcare that is centered around the needs of families.”

RedOne ft. Enrique Iglesias, Aseel and Shaggy | Don’t You Need Somebody

platinumrecordsmusic 236,826,729 views Jul 27, 2016
* Aseel Omran (Arabic: أسيل عمران) is a Saudi Arabian singer


Consider What Happens When We Don’t Care for NICU Parents
— Here’s how hospitals can support parental mental health
by Alexa Grooms, BSN, RN December 23, 2022
Evidence shows opens in a new tab or window it is the emotional opens in a new tab or window, rather than the medical, complications of pregnancy that are most impactful on the long-term well-being of the parent and child. These emotional complications, known as perinatal mood and anxiety disorders (PMADs), may occur during pregnancy until the first few years after giving birth. PMADs include the most widely known postpartum depression, as well as the lesser-known postpartum anxiety, panic disorder, postpartum obsessive-compulsive disorder, post-traumatic stress disorder, and postpartum psychosis.
Neonatal intensive care unit (NICU) parents are particularly vulnerable to PMADs. Parents rarely expect their child to require intensive care, and the journey is emotional and unpredictable. Studies most often focus on mothers, or the birthing parent, rather than fathers or the supporting parent. However, we know that NICU parents have 28-70% higher opens in a new tab or window incidences of depression. At a minimum, being separated from your child can cause distress and impaired bonding.
As a NICU nurse, I can testify that staff know parent mental health is pervasive. So why aren’t we addressing it? Unfortunately, few of us have the tools, resources, and confidence to intervene. After all we were hired to take care of babies, and adults can be intimidating, especially on such a stigmatizing topic. However, hospitals and healthcare professionals must ask ourselves: What are we missing if we do not also care for the family? Parents are the key to their child’s emotional and cognitive wellness and the effects last a lifetime, for the positive or negative. Mood disorders can be debilitating both for the individual and the family.
This year, a cross-sectional study opens in a new tab or window by Cooper Bloyd, MD, MS, and fellow researchers surveyed which NICUs were incorporating mental health screening and treatment following the 2015 release of the National Perinatal Association guidelines. Among respondents, 44% routinely screened parents for disorders, most often depression. They also found that 47% offered mental health education to families, and between 3-11% employed some type of mental health specialist in their unit. The figures, they acknowledged, were likely high because of low study participation and the respondents wanting to advertise their practices.
As the National Perinatal Association outlines opens in a new tab or window, mental health initiatives can be implemented with families via universal distress screening; “layered levels of support” through education, especially peer support groups; and employment of mental health professionals. Here are my recommendations for how these may be best incorporated into standard care.
Incorporate Universal Screening
Screening can be integrated by making it part of the admission and discharge educational packages. For example, when parents are filling out initial admission forms or upon discharge when families either transfer to another facility or go home with their follow-up pediatrician appointments. There are also opportunities to screen families during infant care milestones, such as 100 days in the NICU. Whenever possible, screening can be placed alongside standard information such as safe sleep and feeding education to minimize stigma. The Edinburgh Postnatal Depression Scale is a validated screening tool specific to postpartum depression. Other useful screening tools may include the PHQ-2 for depression or PTSD-5 for trauma. Positive results should trigger follow up with a unit-based mental health provider such as a social worker, psychologist, psychiatrist, psychiatric nurse practitioner, or nurse with extensive perinatal mental health training.
This year, a cross-sectional study opens in a new tab or window by Cooper Bloyd, MD, MS, and fellow researchers surveyed which NICUs were incorporating mental health screening and treatment following the 2015 release of the National Perinatal Association guidelines. Among respondents, 44% routinely screened parents for disorders, most often depression. They also found that 47% offered mental health education to families, and between 3-11% employed some type of mental health specialist in their unit. The figures, they acknowledged, were likely high because of low study participation and the respondents wanting to advertise their practices.
As the National Perinatal Association outlines opens in a new tab or window, mental health initiatives can be implemented with families via universal distress screening; “layered levels of support” through education, especially peer support groups; and employment of mental health professionals. Here are my recommendations for how these may be best incorporated into standard care.
Incorporate Universal Screening
Screening can be integrated by making it part of the admission and discharge educational packages. For example, when parents are filling out initial admission forms or upon discharge when families either transfer to another facility or go home with their follow-up pediatrician appointments. There are also opportunities to screen families during infant care milestones, such as 100 days in the NICU. Whenever possible, screening can be placed alongside standard information such as safe sleep and feeding education to minimize stigma. The Edinburgh Postnatal Depression Scale is a validated screening tool specific to postpartum depression. Other useful screening tools may include the PHQ-2 for depression or PTSD-5 for trauma. Positive results should trigger follow up with a unit-based mental health provider such as a social worker, psychologist, psychiatrist, psychiatric nurse practitioner, or nurse with extensive perinatal mental health training.
Additional follow up could also take the form of obstetricians reaching out to patients prior to the 6-week postpartum follow up. Screening and support should also include pediatrics, as pediatricians are in a unique position to continuing assessing the child’s development and parent-child relationship.
Education for Parents and Staff
There are many opportunities to enhance parent and staff education. Parent support groups are especially therapeutic. Parents should be welcomed in by other parents as they go through this unexpected journey together. Veteran NICU families often play an important role in facilitating and leading these groups. Parents who pump also find exceptional reward and meaning in donating breast milk back to other NICU infants.
In terms of staff, mental health education should be ongoing, as going into pediatrics means partnering with families. Patient psychosocial history and discussion about how to support families should be incorporated into daily provider rounds.
Seeing It Through With Usable Referrals
Parents who want or require psychiatric care after discharge must be referred. Most importantly, these referrals must be usable. I will argue that hospitals must guarantee NICU parents’ appointments or spots in follow up care. We cannot build the trust of these families only to refer them to help that is a dead end. Hospitals will argue it is impossible to guarantee appointments, as demand for psychiatric care is high. However, hospitals must recognize the risk of both child and parent hospital readmission if they aren’t connected to care. There is also the added benefit of building patient loyalty. Labor and delivery are where most families first interact with medical care, and a good experience can lead them to return for future care.
Of course, adding mental health staff and resources will come at a cost. As cost is an understandable concern, the value of these services can be demonstrated first in low- to zero-cost quality improvement or nurse residency projects before investing dollars. Once value is demonstrated, hospitals can leverage funding from Magnet or Baby Friendly Hospital designation budgets. Applications for these hospital designations are lengthy but worth pursing as funds are allocated for pilot projects such as these.
Final Thoughts
It is clear NICU parents need our help. My recommendations are clear and feasible, and unit staff can help integrate them into standard care practices. Hospitals have a responsibility to be part of the solution and allocate funding from existing initiatives to offset costs. Staff must be educated to support parents, and hospitals must create systems within existing infrastructure to address mental health concerns. We can no longer omit parents’ health when we care for their child.
Source:https://www.medpagetoday.com/opinion/second-opinions/102346

PREEMIE FAMILY PARTNERS
The NICU: The palliative care team would ask us, “How do you feel about what you just heard?”

Courageous Parents Network Nov 6, 2019
The palliative care team would ask us, “How do you feel about what you just heard?” Parents of a baby son who was born with Arteriovenous Malformation (AVM) and died at age 3 months, talk about how the palliative care team interacted with and supported them, and helped manage their son’s pain and consider the future. “They really saw us as people and as parents. It was an awesome help to have them there.”


Holding Your Baby in Intensive Care
Published on Jun 19, 2022

“Yes, your baby can be held today!”
Hearing these words can trigger strong emotions. Every parent is eager to hold their baby. But holding a baby who is very small or on a breathing machine with lots of tubes and wires can be scary (even for experienced parents). Below are some common questions parents have about holding their baby in intensive care and our recommendations.
“I know I will want to hold my baby, but isn’t it better to just let my baby rest in bed?”
Babies are born needing your touch. Your touch is very different than touch from the hospital staff.
When you hold your baby, you help your baby:
- Get to know you and develop an attachment
- Maintain body temperature
- Develop and grow brain connections
- Learn language
- Develop muscles and strength
- Gain weight
- Feel less pain
- Cry less
- Stabilize breathing and heart rate
- Sleep better
- Reduce stress
- Feel safe and protected
Holding your baby also helps you:
- Feel more confident as a parent
- Feel connected to your baby
- Reduce stress
- Produce milk for your baby, if you pump
“Holding my baby for the first time feels like a big deal. How can I prepare when it is time to hold my baby?”
- Request a comfortable chair with arms and a footrest.
- Choose a time when you can take your time and are not rushed.
- Go to the restroom, and make sure you eat beforehand.
- For moms who pump, pump before holding your baby.
- Have a water bottle nearby in case you become thirsty.
“I want to hold my baby, but I don’t know whether it is safe, and I feel nervous. What are some tips?”
- It’s never too early to start a conversation with your nurse about when your baby will be ready to be held. If your baby is not yet ready, ask your nurse, “What are some signs that tell me my baby is ready to be held?”
- Talk to your baby’s therapists (e.g., occupational therapists, physical therapists) about suggestions for how to hold your baby.
- Ask your baby’s nurse for ideas about how to make your baby comfortable.
- Remember that sometimes babies have a little stress while being moved out of bed but then become very comfortable in your arms.
- All babies (not just premature babies) benefit from skin to skin holding, which is called kangaroo care. Kangaroo care has amazing benefits for children and parents and is encouraged whenever possible. To learn more about kangaroo care, please see the Skin to Skin Care (Kangaroo Care) handout in the patient family education manual (13:B:08).
- Before holding your baby, take some calming deep breaths.
- Ask the social worker or psychologist for tips on how to feel more comfortable holding your baby.
- Remember that the more you hold your baby, the easier and more comfortable it will become!
“My baby’s team says my baby is not yet ready to be held. What else can I do?”
If your baby is not ready to be held, your touch is still important!
- “Hand hugs” are a great option when your baby is not yet ready to get out of bed. This will also support your baby’s growth and your relationship.
- Gentle, constant touch to your baby’s head, chest or feet can have a calming effect.
- If your baby is in a warmer bed or isolette, ask for a taller chair so you can sit comfortably next to your baby and be together.
Source:https://www.chop.edu/health-resources/holding-your-baby-intensive-care
Mom shares story of premature baby now hospitalized with RSV

Nov 17, 2022 – Nov 17, 2022
On World Prematurity Day, a Southern California mom is sharing her story about having a premature baby who is now hospitalized with RSV. The three-month-old has been at Children’s Health of Orange County for more than three weeks, but his story is similar to other families whose children are being treated right here in San Diego.

Respiratory syncytial virus (RSV

Respiratory syncytial virus (RSV) What is RSV Respiratory syncytial virus (abbreviated as RSV) is a virus that can cause cold-like symptoms but can also lead to severe breathing difficulties or even a severe infection of the lung. Almost all children have already once been infected with RSV by their second birthday. Since there are a lot of different forms of RSV, one can be infected several times in life.1 At risk for an RSV infection Everybody can be infected by RSV. Usually people don’t really note this, but have a cold or sniffle and recover within a few days. But the virus can also cause a very severe infection. Certain people are at risk for a more severe infection and may require hospitalisation, need of oxygen therapy and long-term damages like asthma.
Symptoms of an infection with RSV:
The symptoms of an infection with RSV are similar to common cold symptoms, like runny nose, coughing or wheezing (a whistling sound during breathing) and a decreased appetite. An adult infected with RSV can show symptoms, but does not have to, while children usually do show symptoms. Especially in very young children the symptoms might consist of irritability and decreased activity and appetite. Also breaks in breathing (apnoea) might occur. Fever can be a symptom, but is not always present. At the beginning, the symptoms might be relatively low pronounced, but especially in people at risk for a more severe infection it can lead to hospitalisation and severe inflammation of the small airways in the lung (bronchiolitis) and infection of the lungs (pneumonia).1 Ways of transmission of the virus The virus is mainly spread by droplets from a person who is infectious to another person. This means by sneezing or coughing of an infected person into the air. When a person inhales these droplets or when they touch the mouth, nose or eye, this can lead to an infection. Also a direct or indirect contact with nasal or oral secretions from a contagious person can lead to an infection. Be aware that also kissing can lead to a transmission of the virus. Another possible form of being infected with RSV is by touching something (surfaces, toys, doorknobs, gloves,…) that an infectious person had touched before and then rubbing eyes or nose. People who are infected with the virus, but do not show symptoms or only light symptoms can still be contagious for others.
At Risk for Severe Infection:
– preterm babies young children (particularly up to 6 months)
– children with heart or lung disease (especially up to 2 years)
– certain congenital anomalies (for example trisomy 21)
– children with a neuromuscular disease (for example children who cannot swallow easily or have – – problems clearing mucus secretions)
– elderly people who have a weak immune system
Additional Risk Factors for the babies:
– multiple birth
– male siblings in early childhood
– passive smoking close domestic conditions
– malnutrition
– lack of breastfeeding
– family history of allergic diseases or asthma
You can help protect your baby by taking some precautions:
The virus is able to survive quite a long time on hands (about half an hour), tissues (up to an hour) and toys/surfaces (several hours).
Therefore the following precautions and recommendations are very important to be followed:
Don’t share your mug, plate or cutlery with others Avoid rubbing your nose or eyes If possible, avoid interaction with high-risk children if you have cold-like symptoms When coughing or sneezing cover your mouth and nose with a tissue and throw it away afterwards Stay at home when you have cold-like symptoms Don’t kiss high-risk children while you or they show cold-like symptoms High-risk children should spend little time in potentially infectious places (for example child-care centres) Don’t smoke near your child. Wash your hands after smoking Breastfeeding reduces the risk for an infection with RSV Wash your hands frequently and wipe hard surfaces with soap and water (15-20 seconds!) or disinfectant.
Treatment of RSV Most people who are infected with RSV only show a mild form of infection and usually do not need treatment at all. For the ones suffering from a more severe form of the disease, there is no causal therapy and only the symptoms can be treated by for example lowering fever and drinking enough. Some children may even require hospitalisation and need help with breathing.4 Vaccination against RSV At the moment there is no vaccine that can help prevent RSV infection.3 Nevertheless, there may be options to prevent contracting the virus. And of course, you can help avoid RSV infection by following the already mentioned tips for hygiene! For further questions please ask your paediatrician.

A Stay in Neonatal Care – Preparing to Take Your Baby Home

The NICU Foundation Oct 14, 2021
Funded by The NICU Foundation and created in partnership with The South West Neonatal Network, this animation was created to support parents, as they navigate their journey home following a stay in neonatal care with a premature or sick baby.
*** Ask your healthcare provider what community resources are available to support you, your family, and your baby. Knowing resources in advance will empower your ability to be proactive and prepared!


INNOVATIONS

Stanford Fetal Therapy VR: An inside look at complex fetal conditions

Stanford Medicine Children’s Health Apr 29, 2022
Stanford Fetal Therapy VR gives patients and doctors an unprecedented view of two complex fetal conditions—spina bifida and twin-to-twin transfusion syndrome—and how we can treat them using cutting-edge surgical techniques.

Clinical outcomes for babies born between 27 – 31 weeks of gestation: Should they be regarded as a single cohort?
Abdul Qader Tahir Ismail a,b,*, Elaine M. Boyle a, Thillagavathie Pillay a,c, For the OptiPrem Study Team
Journal of Neonatal Nursing 29 (2023) 27–32
- Introduction
Within the UK, babies born below 27 weeks of gestation are recommended to be born in maternity services attached to neonatal intensive care units (NICU). For those babies born between 27 and 31 weeks of gestation, care can be delivered in maternity services attached to either a NICU or a local neonatal unit (LNU). While the first recommendation is evidence based (Marlow et al., 2014; Watson et al., 2014), our systematic review found a paucity of evidence for optimal location of birth and care for babies born between 27 and 31 weeks (Ismail et al., 2020).
This reflects a more general lack of research aimed at babies born between 27 and 31 weeks of gestation. During our systematic review we found that most of the data available for this population comes from subgroup analyses in studies of larger gestational age ranges (Ismail et al., 2020; Lasswell et al., 2010). Of these, most report outcomes for this group as a whole rather than by gestational week (Watson et al., 2014). Neonatal research is logistically difficult, especially in relation to very preterm babies, as the population size decreases with each extra gestational week of prematurity. Therefore, it is common practice to cohort babies. While not ideal, this makes more sense for certain gestational age ranges than others.
Babies born between 27 and 31 weeks do not form a ‘natural’ cohort as do those born extremely preterm. There is a significant degree of heterogeneity in the clinical presentation between babies born at either end of this spectrum. Over this five-week period the foetus is undergoing significant growth and developmental changes in-utero. In this review we describe the limited available literature on the variation in clinical presentation and outcomes for babies born between 27 and 31 weeks of gestation in the context of fetal developmental biology and preterm birth. In doing so, we highlight the importance of future research reporting gestation specific outcomes for preterm babies in general, but especially this cohort.
- Survival and key morbidities for babies born at 27–31 weeks
Table 1 and Fig. 1 summarises outcomes for major neonatal morbidities by each week between 27 and 31 weeks of gestation. They include international mortality data from national statistical bodies. An identical trend is evident for all, demonstrating increasing incidence with decreasing gestational age and substantially different outcomes for the most preterm babies within this gestational age range compared to the most mature. There is, on average, a greater than 4-fold difference in mortality between babies born at 27 weeks of gestation compared to 31 weeks, and a 4-fold increase in rates of survival to discharge without morbidity for babies born at 30 weeks compared to 27 weeks.
- Understanding postnatal outcomes through the lens of foetal development
The medical and nursing care required for babies in this group is likely to be more intense for those at the lower than the higher end of the gestational age spectrum, based on their degree of immaturity, and existence of co-morbidities.
- Respiratory system
Babies born at the lower end of this gestational age range are often first supported with non-invasive ventilation (NIV) if they display sufficient respiratory drive and have a good heart rate. Those that do not will be intubated and invasively ventilated within delivery suite, and a proportion of those who initially managed on NIV may require subsequent intubation and ventilation due to significant apnoea and/or respiratory failure. These babies may benefit from a dose of surfactant and regular caffeine, with the aim to extubate onto NIV as soon as appropriate, to minimise ventilator associated lung injury while still providing an adequate level of support, which may be required for several weeks. In contrast, the majority of babies born at the upper end of this gestational age range will only require a brief period of NIV, usually in the form of high flow nasal prong oxygen or continuous positive airway pressure (CPAP) support.
How can we understand this in the context of foetal development? In-utero breathing stimulates lung growth (Harding and Hooper, 1985). By 24–28 weeks, fetal breathing movements occur for 10–20% of the time, increasing to 30–40% by 30 weeks (Fraga and Guttentag, 2012). Correspondingly, during the saccular stage of fetal lung development (24–26 weeks to 36–38 weeks), surface area for gas exchange increases as does vascularisation and surfactant production. Following preterm birth, this immaturity of central respiratory drive manifests as periods of hypoventilation and apnoea, the incidence falling from 54% at 30–31 weeks to 7% at 34–35 weeks (Henderson-Smart, 1981). In those born at 24–27 weeks, apnoeic episodes are more likely to continue for longer compared to those born ≥28 weeks (Eichenwald et al., 1997). Therefore, respiratory compromise, the need for mechanical ventilation and intensive care support is more likely with increasing prematurity, with the incidence of RDS at 60–80% for babies born at 26–28 weeks, falling to 15–30% by 32–36 weeks [14]. The more immature the lung, the greater the risk of ventilator associated lung injury, abnormal development, and chronic lung disease (CLD) [15]. Its incidence is nine times greater in babies born at 27 weeks than at 31 weeks of gestation (Bolisetty et al., 2015; Egreteau et al., 2001).
- Cardiovascular system
Babies born at 27 weeks of gestation who are difficult to successfully extubate will often be found to have a haemodynamically significant patent ductus arteriosus (PDA) on echocardiography (although clear evidence is lacking for a causal relationship – (El-Khuffash et al., 2019; Benitz et al., 2016)). Management protocols vary unit to unit, but many will commence pharmacological treatment with ibuprofen, or more recently paracetamol. If this is unsuccessful, and on serial echocardiograms there is evidence of developing heart failure, the baby will be referred for surgical ligation. While some babies born at 31 weeks may have clinical signs of a PDA (i.e., a murmur, easily palpable femoral pulses), it is unlikely to be haemodynamically significant and can be left to close on its own. If at the time of discharge these signs are still present, an echocardiogram can provide a definitive diagnosis to arrange appropriate follow-up.
Following preterm birth, constriction of the ductus arteriosus is less likely to occur because of reduced vessel tone and pulmonary clearance of prostaglandins, to which the ductus in preterm babies is more sensitive (Clyman, 2012). This explains the increase in incidence of patent ductus arteriosus (PDA) at day 7 of life with reducing gestation (68%, 33%, and 2% at 26–27 weeks, 28–29 weeks, and ≥30 weeks, respectively) (Clyman, 2012), and a 10-fold increase in the likelihood of requiring surgery for a clinically significant PDA in those born at 27 weeks gestation when compared to those at 31 weeks (Bolisetty et al., 2015).
- Ocular system
Babies born at the lower end of this gestational age range most often require supplemental oxygen as part of their respiratory support. This is recognition receptors (including toll like receptors) continue development until 33 weeks, however, for up to 28 days after preterm birth at <30 weeks, toll like receptor responses are significantly reduced (Marchant et al., 2015). Regarding the complement system, average levels of terminal pathway components, C5, C6, and C8 in preterm babies are at 60–73%, 36–39%, and 29%, respectively, compared to adult levels (McGreal et al., 2012). Considering overall functional capacity, CH50 assay results increase from 32 to 36% at 26–27 weeks, to 52–81% at term.
Physical and external contributing factors, such as skin barrier integrity, repeated invasive procedures and indwelling plastic catheters, are also related to degree of prematurity.
3.6. Renal system
Babies born at the lower end of this gestational age range receive a significant proportion of their hydration/nutrition intravenously, while simultaneously exposed to nephrotoxic drugs, e.g., gentamicin for treatment of suspected EOS, ibuprofen for treatment of a haemodynamically significant PDA, and vancomycin for treatment of CLABSI, warranting close monitoring of their electrolytes, renal function, and fluid balance. In contrast, babies born at the upper end of this gestational age range relatively quickly establish enteral feeds and much less frequently require treatment with nephrotoxic drugs.
The incidence of renal failure is 2-fold higher for a baby born at 27 weeks compared with 30 weeks of gestation (Walker et al., 2011; Jetton et al., 2017). Two thirds of new nephrons form between 28 and 36 weeks, after which no new glomeruli develop (Stritzke et al., 2017; Hinchliffe et al., 1991). Following preterm birth, nephrogenesis can continue for up to 40 days (Rodriguez et al., 2004; Black et al., 2013), but a significant proportion of new glomeruli have cystic dilatation of the Bowman’s capsule (Sutherland et al., 2011).
3.7. Neurological system
As routine, babies born at the lower end of this gestational age range will have a cranial ultrasound scan (CrUSS) within the first few days of life, which will be repeated two to three times within the first month. It is not uncommon to diagnose uni/bilateral grade I-II intraventricular haemorrhage (IVH) and increased echogenicity in the periventricular areas even in those babies without any discernible risk factors except prematurity. However, for the more unwell (who may have required a degree of resuscitation, intubation and invasive ventilation, periods of hypoxaemia, hyper/hypocapnia and acidosis, and hypotension requiring fluid expansion and inotropic support), more severe grades of IVH (III/IV) and cystic periventricular leukomalacia (PVL) are more common. This would necessitate increasing the frequency of scanning to monitor for complications (e.g., post-haemorrhagic hydrocephalus) and plan for longer term neurodevelopmental follow-up and support. Babies born at the upper end of this gestational age range are much less likely to experience this degree of homeostatic disturbances and so are routinely scanned once within the first week of life and may not have a second scan until term equivalent or ready for discharge.
This variation in scanning frequency is based on the inverse correlation gestational age at birth has with risk of IVH (Brouwer et al., 2008; Synnes et al., 2001). Babies born at 27–28 weeks have a 2-fold increased risk of developing intraventricular haemorrhage (IVH) of any grade, compared to those born at 31 weeks (Brouwer et al., 2008; Synnes et al., 2001). Severe IVH (stage III/IV) is three times more common in those born at 27 weeks than 31 weeks.
The germinal matrix has a dense supply of fragile blood vessels that are prone to rupture with fluctuations in cerebral blood flow, causing the bulk of what is described in the literature as IVH. The risk is increased due to immature cerebral autoregulation, in which hypoxaemia, hypercapnia, hypocapnia, and acidosis cause pressure passivity (Soul et al., 2007; Tsuji et al., 2000). This, combined with increasing severity of respiratory illness and homeostatic disturbances in the more preterm baby, may explain the inverse correlation of IVH with gestational age.
The trend is similar for periventricular leucomalacia (PVL) (Luan-ying, 2011). Non-cystic PVL is characterised by hypomyelination (Volpe, 2009). By 28–30 weeks, increasing differentiation of oligodendrocyte progenitors (pre-OL) coincides with the start of myelination (Jakovcevski et al., 2009; Tau and Peterson, 2010), stimulated by microglia that are also proliferating (Menassa and Gomez-Nicola, 2018; Gould and Howard, 1991; Billiards et al., 2006). Hypoxia, infection or inflammation cause pathogenic activation of microglia and death of pre-OL cells through release of reactive nitrogen and oxygen species (RNS/ROS) (Merrill et al., 1993; Haynes et al., 2003).
Preterm babies with severe IVH (grade III/IV) and cystic PVL are at increased risk of cerebral palsy (Himmelmann and Uvebrant, 2014). There is a nearly 2-fold increase in incidence of cerebral palsy for a baby born at 27 weeks compared with 31 weeks of gestation, but the absence of cranial ultrasound abnormalities does not always mean normal neurodevelopment for babies born preterm. In utero, cortical volume increases from 13% at 28 weeks to 53% at 34 weeks. Babies born preterm have reduced growth trajectories of their cerebrum, cerebellum, and brainstem compared to the foetus within the last trimester (Bouyssi-Kobar et al., 2016). Each extra week of maturity at birth between 27 and 32 weeks is associated with an increased IQ of 2.5 points (Johnson, 2007).
- Implications for practice
The degree of clinical support that a preterm baby may receive is graded into intensive care, high dependency and special care (BAPM, 2011). Most babies born at the lower end of this gestational age spectrum require some degree of intensive care support, based on the clinical manifestations of their prematurity. In contrast, the majority of ‘well’ preterm babies at the upper end may never require intensive care support, but rather high dependency and special care support. This dichotomy in their clinical presentation means that grouping them into a single cohort may have the following consequences:
a) Cohorting this group in terms of decision-making regarding place of birth and care may mean over utilisation of intensive care support for those babies at the upper end of the spectrum. This in turn may limit intensive care availability for those babies who need it, especially in resource and cost constrained environments.
b) Grouping them as a single cohort in the literature makes it more likely significant outcomes for babies at the lower end of this spectrum will be obscured.
5. Conclusion
This review highlights the variation and range of clinical profiles and associated outcomes for babies born between 27 and 31 weeks of gestation, and how these relate to key aspects of organ/system development occurring in-utero during this 5-week period. The data summarised in Table 1 and graphically represented in Fig. 1 consistently demonstrate a gradient of risk across multiple outcomes with rates of mortality and morbidity increasing from birth at 31 to 27 weeks. Outcomes at the two extremes of this range may differ significantly, yet babies born between 27 and 31 weeks of gestation are often regarded as a single entity with respect to place of birth and care, and for research purposes. In future studies relating to very preterm birth, understanding gestation specific morbidities and outcomes may be more informative, compared to outcomes as a single collective group. This may be a useful concept for policy makers involved in preterm health service delivery, and might allow more finely tuned, appropriate utilisation of resources for this group of babies.
Full Report, Data, Charts/References

https://www.sciencedirect.com/science/article/pii/S1355184122000588

HEALTHCARE PARTNERS

AAP Issues Reports on Point-of-care Ultrasonography Applications in the NICU
11/28/22

Point-of-Care Ultrasonography (POCUS) can be performed at the bedside of patients in neonatal intensive care units (NICU). If performed in a timely fashion, POCUS has the potential for enhancing quality of care and improving outcomes. The clinical report, “Use of Point-of-Care Ultrasonography in the NICU for Diagnostic and Procedural Purposes,” along with an accompanying technical report, are published in the December 2022 Pediatrics (published online Nov. 28). Although the performance and interpretation of ultrasonography have traditionally been limited to pediatric radiologists and pediatric cardiologists, POCUS refers to ultrasonography performed at the bedside by non-radiology and non-cardiology practitioners in the NICU for diagnostic, therapeutic, and procedural purposes. The reports, written by the Committee on Fetus and Newborn and the Section on Radiology, state that the technology is increasingly used worldwide. Yet, there are no published guidelines on implementation of point-of-care ultrasonography programs in U.S. neonatal intensive care units. The AAP suggests institutional guidelines for the use of point-of-care ultrasonography and other steps to help overcome barriers in use of the technology.
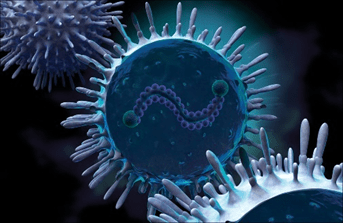
RESPIRATORY SYNCYTIAL VIRUS INFECTION (RSV)For Healthcare Providers

Healthcare providers should consider RSV in patients with respiratory illness, particularly during the RSV season.
Respiratory syncytial virus (RSV) was discovered in 1956 and has since been recognized as one of the most common causes of childhood illness. It causes annual outbreaks of respiratory illnesses in all age groups. In most regions of the United States, RSV circulation starts in the fall and peaks in the winter, but the timing and severity of RSV season in a given community can vary from year to year. Scientists are developing several vaccines, monoclonal antibodies, and antiviral therapies to help protect infants and young children, pregnant people (to protect their unborn babies), and older adults from severe RSV infection.
Clinical Description and Diagnosis
In Infants and Young Children
RSV infection can cause a variety of respiratory illnesses in infants and young children. It most commonly causes a cold-like illness but can also cause lower respiratory infections like bronchiolitis and pneumonia. One to two percent of children younger than 6 months of age with RSV infection may need to be hospitalized. Severe disease most commonly occurs in very young infants. Additionally, children with any of the following underlying conditions are considered at high risk:
- Premature infants
- Infants, especially those 6 months and younger
- Children younger than 2 years old with chronic lung disease or congenital heart disease
- Children with suppressed immune systems
- Children who have neuromuscular disorders, including those who have difficulty swallowing or clearing mucus secretions
Infants and young children with RSV infection may have rhinorrhea and a decrease in appetite before any other symptoms appear. Cough usually develops one to three days later. Soon after the cough develops, sneezing, fever, and wheezing may occur. In very young infants, irritability, decreased activity, and/or apnea may be the only symptoms of infection.
Most otherwise healthy infants and young children who are infected with RSV do not need hospitalization. Those who are hospitalized may require oxygen, intubation, and/or mechanical ventilation. Most improve with supportive care and are discharged in a few days.
In Older Adults and Adults with Chronic Medical Conditions
Adults who get infected with RSV usually have mild or no symptoms. Symptoms are usually consistent with an upper respiratory tract infection which can include rhinorrhea, pharyngitis, cough, headache, fatigue, and fever. Disease usually lasts less than five days.
Some adults, however, may have more severe symptoms consistent with a lower respiratory tract infection, such as pneumonia. Those at high risk for severe illness from RSV include:
- Older adults, especially those 65 years and older
- Adults with chronic lung or heart disease
- Adults with weakened immune systems
RSV can sometimes also lead to exacerbation of serious conditions such as:
- Asthma
- Chronic obstructive pulmonary disease (COPD)
- Congestive heart failure
Clinical Laboratory Testing
Clinical symptoms of RSV are nonspecific and can overlap with other viral respiratory infections, as well as some bacterial infections. Several types of laboratory tests are available for confirming RSV infection. These tests may be performed on upper and lower respiratory specimens.
The most commonly used types of RSV clinical laboratory tests are
- Real-time reverse transcriptase-polymerase chain reaction (rRT-PCR), which is more sensitive than culture and antigen testing
- Antigen testing, which is highly sensitive in children but not sensitive in adults
Less commonly used tests include:
- Viral culture
- Serology, which is usually only used for research and surveillance studies
Some tests can differentiate between RSV subtypes (A and B), but the clinical significance of these subtypes is unclear. Consult your laboratorian for information on what type of respiratory specimen is most appropriate to use.
For Infants and Young Children
Both rRT-PCR and antigen detection tests are effective methods for diagnosing RSV infection in infants and young children. The RSV sensitivity of antigen detection tests generally ranges from 80% to 90% in this age group. Healthcare providers should consult experienced laboratorians for more information on interpretation of results.
For Older Children, Adolescents, and Adults
Healthcare providers should use highly sensitive rRT-PCR assays when testing older children and adults for RSV. rRT-PCR assays are now commercially available for RSV. The sensitivity of these assays often exceeds the sensitivity of virus isolation and antigen detection methods. Antigen tests are not sensitive for older children and adults because they may have lower viral loads in their respiratory specimens. Healthcare providers should consult experienced laboratorians for more information on interpretation of results.
Prophylaxis and High-Risk Infants and Young Children
Palivizumab is a monoclonal antibody recommended by the American Academy of Pediatrics (AAP) to be administered to high-risk infants and young children likely to benefit from immunoprophylaxis based on gestational age and certain underlying medical conditions. It is given in monthly intramuscular injections during the RSV season, which generally starts in the fall and peaks in the winter in most locations in the United States.
Source:https://www.cdc.gov/rsv/clinical/index.html


“Diversity really means becoming complete as human beings – all of us. We learn from each other. If you’re missing on that stage, we learn less. We all need to be on that stage.”
– Juan Felipe Herrera

Daniel Laurie from Call the Midwife | Our Voice Interviews




A Little Book About Bravery by Rick DeLucco

A Kids Co. Sep 20, 2021
A Little Book About Bravery


Kiteboarding with Jasmina: Saudi Arabia Special

Bo Van Wyk Apr 14, 2016
Kiteboarding Saudi Arabia I had the chance to go kiting at two amazing spots in Saudi Arabia. Let me take you to this unusual place. Enjoy!



