Botswana, officially the Republic of Botswana, is a landlocked country in Southern Africa. Botswana is topographically flat, with approximately 70% of its territory being a part of the Kalahari Desert. It is bordered by South Africa to the south and southeast, Namibia to the west and north, Zambia to the north, and Zimbabwe to the northeast. With a population of slightly over 2.4 million people and a comparable land area to France, Botswana is one of the most sparsely populated countries in the world. While it is not enshrined by statutory law, Botswana is de facto the nation state of the Batswana people, who constitute nearly 80% of the population while legally undistinguished Kalanga people, who account for another 11%, are the single largest ethnic minority.
Botswana is a parliamentary republic governed by the Constitution of Botswana. It is the longest uninterrupted democracy in Africa. Its seat of government is in Gaborone. Botswana’s governing institutions were established after it became an independent nation in 1966. Botswana’s governmental structure is based on both the United Kingdom’s Westminster system and the Tswana people’s tribal governments. Botswana has a centralised government in which national law supersedes local law. Local laws are developed by local councils and district councils. They are heavily influenced by tribal governments, which are led by the tribe’s chief.
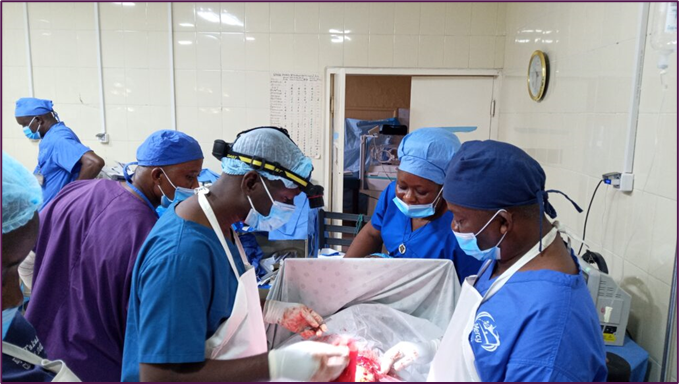
Botswana provides universal healthcare to all citizens through a public healthcare system, but privately run healthcare is also available. The government operates 98% of all medical facilities. Healthcare in Botswana is delivered through a decentralised model with primary healthcare being the pillar of the delivery system. Botswana has an extensive network of health facilities (hospitals, clinics, health posts, mobile stops) in the 27 health districts. In addition to an extensive network of 104 clinics with beds, 195 clinics without beds, 338 health posts and 844 mobile stops primary health care (PHC) services in Botswana are integrated within overall hospital services, being provided in the outpatient sections of all levels of hospitals. It is through these structures that a complement of preventive, promotive and rehabilitative health services as well as treatment and care of common problems are provided.
For a general check-up, citizens are charged 5 pula, unless they are under five or over 65, in which case check-ups are free. The network of public hospitals is organized between primary hospitals, which function as general hospitals and equipped to deal with most diseases and immediate threats to health, district hospitals, which have more beds and are equipped to deal with more serious medical issues, and referral hospitals, which are highly advanced facilities equipped to deal with specialized problems. There are also two private hospitals in the country. The government pays for the treatment of patients referred abroad for medical procedures.
Source: https://en.wikipedia.org/wiki/Health_in_Botswana
- GLOBAL PRETERM BIRTH RATES – Botswana
- Estimated # of preterm births: 12 per 100 live births
- (Global Average: 10.6)
- Source- https://worldpopulationreview.com/country-rankings/preterm-birth-rates-by-country

COMMUNITY

Each year, nearly 300,000 women die during childbirth. The vast majority of these deaths are preventable – yet maternal survival is still determined by where a woman lives, her access to care and the strength of the health system around her.
The leading cause of maternal death is postpartum hemorrhage (PPH)—a condition that, with appropriate quality care, is almost entirely preventable. Yet, due notably to limited access to the full range of recommended lifesaving, quality-assured medicines and devices, 86,000 women die of PPH each year. Most of these deaths occur in sub-Saharan Africa, where a woman is 130 times more likely to die in childbirth than a woman in Europe or North America.
These preventable deaths of women and adolescent girls have an enormous impact on families and communities. Data shows that infants who lose their mothers are 35 times more likely to die within the first six months of life.
We know the causes, and we know the solutions. With proven interventions, access to quality assured life-saving commodities and sustainable investment, we can eliminate preventable maternal deaths and save millions of lives.
SafeBirth Africa is a collaborative initiative addressing barriers to effective postpartum hemorrhage care in Africa.
Funded by the European Union in the framework of the Team Europe Initiative on Sexual and Reproductive Health and Rights in Africa and a Flagship project of the Global Gateway strategy, co-led by Unitaid and the United Nations Population Fund (UNFPA) and in partnership with African authorities, SafeBirth Africa aims to accelerate the access to World Health Organization (WHO)-recommended lifesaving tools for prevention, detection and treatment of PPH that are not yet widely used in Africa, while implementing innovative delivery solutions.
Unitaid and UNFPA are working with health authorities in five African countries as well as partners and communities to overcome barriers that limit access to these tools, ensure their routine quantification, procurement and supply, strengthen health systems’ readiness to use them appropriately, and disseminate the latest WHO recommendations on the management of PPH.
SafeBirth Africa is working with health authorities five African countries to address the leading cause of death of women in childbirth.
As part of this project, Unitaid leads the efforts to tackle market barriers related to demand, cost, quality, supply and the optimal use of lifesaving medicines and diagnostic tools, including support for regional production. This initiative builds on Unitaid’s existing US$45 million investment to increase access to lifesaving health products that prevent and treat PPH aiming to drive scalable, evidence-based solutions.
UNFPA brings its technical expertise in emergency obstetric and newborn care and midwifery models of care. By training providers in evidence-based practices and supporting the quantification and procurement of quality-assured PPH commodities through its Supplies Partnership, UNFPA contributes to strengthening health supply chains and building the readiness of health systems to uptake the full range of recommended products.
This initiative complements UNFPA’s Maternal and Newborn Health Fund, which provides catalytic support to strengthen public health systems in countries with high maternal mortality and morbidity, focusing on providing quality maternal and newborn care and integrated SRH services in line with the UNFPA Start with Her Strategy.

Source: https://unitaid.org/uploads/SafeBirth-Africa-Reducing-preventable-deaths-in-childbirth.pdf


Botswana has taken a major step toward modernizing its healthcare system with the launch of a national medical delivery drone programme. President Duma Boko unveiled the initiative in Chanoga, describing it as a transformative move to improve access to life-saving medicines across the country.
The drone programme is designed to strengthen the medical supply chain by ensuring faster and more reliable delivery of essential medicines, particularly to remote and underserved communities. President Boko emphasized that the innovation aligns with the government’s commitment to equitable healthcare, stating that no citizen should be denied timely access to critical treatment.
The deployment of medical drones marks a significant advancement in Botswana’s efforts to build a modern, inclusive and resilient healthcare system. The technology is expected to enhance emergency response, reduce delivery times and support healthcare workers in rural areas.
Officials say the programme reflects Botswana’s broader strategy to leverage technology in improving public services and safeguarding the well-being of all citizens.

In remote areas across Tanzania, nurses and midwives like Saraphina and Janeth are dedicating their lives to making childbirth and motherhood safer. And their hard work is paying off. The country has witnessed remarkable progress in reducing maternal mortality, roughly 80% in just seven years (2016-2022). With this momentum, the country stands on track to achieve the global target of the Sustainable Development Goals (SDGs) of less than 70 deaths per 100,000 live births by 2030, and advance the commitments set in the country’s Health Sector Strategic Plan V (2021–2026) to reduce maternal and newborn mortality.
The drive guiding Saraphina – a midwife working in a labor ward – is clear: “My vision is to ensure that every woman in the community knows the importance of going to a health facility as soon as they become pregnant. They should follow the advice offered by healthcare providers because the baby she is carrying is the nation of tomorrow.”
She utilizes new skills and tools like labor care guides to monitor all stages of labor and delivery, reducing risks even in remote and low-resource settings, so women can safely give birth.
That care and dedication is making a lasting impact on some of the most vulnerable moments of a mother’s life: “What made me come here [the health center] is to get good service, and give birth safely,” explains Herena, a mother to twins. “I am grateful to the nurse who helped me during delivery…giving me words of encouragement, and even making me laugh.”
Herena’s decision to deliver in a health facility also reflects current national trends, with 85 per cent of births assisted by skilled providers (TDHS2022).
For some healthcare workers, it is often their personal experience that motivates the work that they do: “I’ve volunteered my life to help pregnant women,” highlights midwife Janeth. “From a young age, I have always loved [this work] because I saw what challenges my mother went through in motherhood that she would then tell me.”
To maintain this momentum, midwives like Janeth and Saraphina are being supported through 2gether 4 SRHR, a joint United Nations regional programme, funded by Sweden, that aims to advance sexual and reproductive health and rights in Tanzania, and across the region.
The programme is helping increase access to sexual and reproductive health and rights, HIV, and GBV prevention and response information and services in some of the most needed areas. One key component of this work has focused on improving maternal health outcomes for women like Herena, by enhancing service delivery, rolling out guidelines on improved, evidence-based healthcare, and training healthcare workers on issues like intrapartum care, postpartum family planning, and comprehensive post-abortion care.

HEALTHCARE PARTNERS

In this powerful episode of FEM, MD, Dr. Lauren Umstattd sits down with ENT surgeon-turned-author Frances Mei Hardin to discuss her debut memoir and the hidden emotional cost of surgical training. Frances Mei speaks candidly about the anger she carried out of residency and how writing became the vehicle that transformed it. From resident-on-resident hostility and weaponized reporting systems to the psychological toll of perfectionism, sleep deprivation, and hierarchy in the OR, this conversation pulls back the curtain on what many physicians experience but rarely say out loud. They explore: • The cultural legacy of The House of God — and why its themes still ring true • How narrative nonfiction differs from anonymous venting and why accountability matters • Neurodivergence as both vulnerability and superpower in medicine • The role of hypnosis therapy in healing trauma and reclaiming focus • Perfectionism, emotional intelligence, and the cost of brittle excellence • Psychological safety in the operating room and how hierarchy without respect harms patient care • Resident-on-resident toxicity and the bystander effect in surgical culture Frances Mei shares what it means to “write through the anger.” What began as revenge writing evolved into a reckoning with her own blind spots, emotional immaturity, and survival mechanisms. The result is a memoir that examines burnout, identity, agency, and reinvention inside academic medicine. This is an honest, nuanced conversation about: surgical residency culture, physician mental health, neurodivergence in medicine, emotional intelligence, trauma recovery, mentorship, and what happens when the system beats the love of the work out of someone. If you are a medical student, resident, attending physician, or simply someone navigating ambition in a high-pressure field — this episode will resonate.

While Certified Child Life Specialists (CCLS) have been actively involved in most children’s hospitals for years, the role and function of CCLS are relatively new in most neonatal intensive care units (NICUs). Because of this, most staff in NICU settings are unaware of the many ways a CCLS can participate in creating a family-centered care culture and environment. Annie Jacobson provides FCC Taskforce members with insights into the role of CCLS and describes ways CCLS can enhance the NICU team, help implement family-centered care principles, and maximize the health outcomes of both babies and families in the NICU setting.
What is a Certified Child Life Specialist (CCLS)?
Many people may be under the impression that a Child Life Specialist is a volunteer brought into a hospital setting to provide activities for children during their hospitalization. In fact, that perception could not be further from the truth. Child Life Specialists are certified professionals who are experts at the intersection of a child’s social, emotional, and cognitive development and the effect of stress and trauma on that development. They are extensively trained in both child development and the impact of trauma on children and their families. CCLSs are required to maintain credentialing and minimum standards of care, and professional organizations such as the American Academy of Pediatrics have issued policy statements stating that CCLSs should be included as essential team members in hospital-based pediatric care.
What is the Role of a Certified Child Life Specialist?
CCLSs specialize in developing individualized plans of care for hospitalized children of all ages. These care plans focus on promoting optimal development, positive coping, and support for the entire family, including siblings. Among the many services provided are developmental support for children, education for families to better understand treatment plans, preparing both patients and families for surgery and other procedures, and assistance in aligning family and medical goals of care. Their role is especially important in helping siblings understand why their brother or sister is hospitalized.
CCLSs also serve a vital role in bereavement and end-of-life discussions. In that role, they can facilitate difficult conversations, support siblings, and create keepsakes and memories.
Certified Child Life Specialists in the NICU
The services of a CCLS can greatly help develop a family-centered care environment in the NICU. Specific to NICU babies, their training and input can help create developmentally supportive policies and pain management plans. However, the role of a CCLS can go much further, empowering parents to recognize the important role they play in their baby’s care and helping them better understand treatment plans. Examples of ways in which CCLSs can help integrate parents into their child’s care include reading programs, parent orientation classes, and assistance with discharge planning. In addition, CCLS are especially well trained to recognize siblings’ needs and to identify and address the concerns and fears siblings may not openly express. This intervention can expand a policy of sibling visitation into a comprehensive support program to minimize the trauma experienced by older brothers and sisters. CCLSs are uniquely trained to address these needs.
Source:https://neonatologytoday.net/newsletters/nt-mar26.pdf

Somewhere between the kid who wanted to be a doctor and the physician you are now, something broke. A third of clinicians cannot even remember why they chose medicine, and the gap between the dream and the daily practice is where burnout settles in. Brian Sayers, a rheumatologist who has run an anonymous counseling program for almost 4,000 physician visits, argues that the way back starts with a 10-minute exercise most doctors have never done.


PREEMIE FAMILY PARTNERS

ABSTRACT
Background
Around half of preterm births lack identifiable causes, indicating the need for further investigation to understand preterm birth risk factors. Existing studies on the intergenerational association of preterm birth showed inconsistency in effect size and direction.
Objective
This systematic review and meta-analysis aimed to review existing studies and provide comprehensive evidence on the intergenerational association of preterm births.
Search Strategy
We searched MEDLINE, Embase and Maternity and Infant Care databases, from the inception of each database to 04 April 2024.
Selection Criteria
Eligibility criteria included studies that reported on women who had given birth and had recorded information about a family history of preterm birth in one or both of the child’s biological parents.
Data Collection and Analysis
Data were extracted by two independent reviewers. A random-effects model was used to compute pooled estimates using odds ratios.
Main Results
Sixteen eligible studies with a total of 2 271 612 mothers were included. The findings indicated a 1.44 (OR = 1.44, 95% CI: 1.34, 1.54) fold increase in odds of giving preterm births among women who were born preterm. Additionally, having a sibling born preterm (OR = 1.53, 95% CI: 1.24, 1.87) and having a partner born preterm (OR = 1.12, 95% CI: 1.01, 1.25) were associated with increased likelihood of giving preterm births among women.
Conclusion
The study revealed that women with a family history of preterm birth face an increased risk of giving preterm births. Screening pregnant women for a family history of preterm birth is essential, with those having a positive family history requiring closer follow-up. *** A video is embedded in article!!!
Source: https://obgyn.onlinelibrary.wiley.com/doi/full/10.1111/1471-0528.17924

Key Points
Your baby’s NICU stay may also impact your family and friends, making them feel sad and worried.
It’s important to ask for help from family and friends when your baby is in the NICU.
Talking openly with your child’s grandparents may reduce your stress during your baby’s NICU stay and help them understand more about your needs during this time.
Your older children may have a hard time coping when their baby sibling is in the NICU. If possible, try to include them in your baby’s care and prepare them for what to expect in the NICU.
What emotions are common for family and friends in the neonatal intensive care unit (NICU)?
Your baby’s NICU stay may impact members of your family, like your older children, parents, and friends. They may be sad, worried, and show these emotions in many ways. Share your feelings with your family or friends so you can support each other. Here are some things to keep in mind about you, your partner, and your families:
- People cope with grief in different ways. Some partners may not express their emotions openly, which can sometimes be misunderstood as not caring. Open communication can help both people feel seen and supported.
- You may have similar feelings but not always at the same time. You may not always be on the “same page.”
- You may react differently to a situation. Talk about your feelings. Listen to each other and try to understand others’ feelings.
- You and your partner may not always feel the same about what to tell others. Some people don’t want to share many medical details, especially if they feel stressed or blame themselves for the baby’s condition. Try to listen to each other and agree on what you both feel okay sharing.
How can friends and family members help when your baby’s in the NICU?
Because this may be a very stressful time in your life, it’s important to get help from others. It may not be easy for you to ask but many people want to help. They just don’t always know how. Here are some ideas of how friends and family can help you. They can:
- Bring a meal to you and your family
- Do your grocery shopping, laundry, or clean your home
- Help with your older children
- With your OK, share updates about your baby through blogs, email, or social media
- Drive you to and from the hospital
- Go with you to meetings at the hospital and take notes. These meetings can be with your baby’s healthcare team, the NICU social worker, or hospital financial staff.
- Sit with your baby in the NICU so that you can take a break, if the NICU allows visitors to be with your baby without you there.
What emotions are common for grandparents in the NICU?
Your baby’s grandparents have their own unique experience in the NICU. They may feel joy over the arrival of a grandchild, but also may worry about the health of the baby. They also may be worried about how you and your partner are coping with the baby’s stay in the NICU. As a parent and a grandparent, they have a very important role during this time.
Grandparents may have mixed feelings after their grandchild is born. They may feel:
- Concerned about your baby’s medical condition
- Angry about the difficulties you and your baby are facing
- Worried about how everyone in the family is coping
- Frustrated by not being able to help or ease your family’s distress
- Pride and joy over the latest addition to your family
How can you help your baby’s grandparents understand what you need when your baby’s in the NICU?
Talking openly with your child’s grandparents may reduce your stress during your baby’s NICU stay. It may also help your child’s grandparents understand more about what you need during this time. Here are some things you can talk about:
- Tell them that you and your partner need time alone with your baby. But let them know when there is a good time for them to come to the NICU to spend time with their grandchild. You may feel more comfortable leaving the NICU if a trusted family member stays with your baby. Check with the NICU staff to make sure grandparents can be with your baby while you’re not there.
- Share your feelings and be patient with each other. Share how you’re coping with your baby’s NICU stay and talk with them about their feelings too. All members of the family are under stress and may sometimes be overwhelmed and short-tempered.
- Give them ideas of how they can help you. Grandparents may want to help, but may not know how. Their support outside of the NICU is just as important as inside the NICU. Whether they live nearby or far away, grandparents can do lots of things to help your family while your baby’s in the NICU.
How can you help your older children cope when your baby’s in the NICU?
You may wonder how you’re going to help your children cope when you’re having trouble coping yourself. And how will you find time for your other children when your baby needs you, too? There are a lot of things you can do to help your older children. These things can help reassure your children that you love them. Here are some ways you can help your children:
- Be honest with them. Your children may have a lot of questions but may not know how to ask them. Tell them what’s going on with you and with their baby brother or sister in words they can understand.
- Try not to change your children’s daily routine. This can help make the situation less stressful for them. When you can’t be at home, ask a relative or other caregiver to take your children to the playground or do other things your children enjoy.
- Try to create some quality time with your children. This will help reassure them that they are important to you too. For example, you can take them to the park to get fresh air for them and for yourself. If you can’t be home, you can call to check in on their school day or read a bedtime story.
- Let other caregivers know about your baby’s NICU stay. Talk to your children’s caregivers, such as day care providers and school teachers, about your baby’s NICU stay. They can give your child additional support and let you know about any problems or behavior changes.
How can you include your older children in your baby’s care in the NICU?
It’s important for your children to become involved with their newborn sibling from the start. The birth of a baby is a big event for the whole family, and you don’t want your older children to feel left out. Here are activities your children can do at home to help care for the baby while they’re in the NICU:
- Color pictures to put up near the baby’s bed
- Pick a favorite photo of themselves or the family to have near the baby’s bed
- Put together a photo album of pictures of the baby
- Create a story book about the birth of their baby brother or sister
- Help get the nursery ready for when the baby comes home
- Record their voice reading a book to the baby
How can you prepare your older children for the NICU?
Many children can’t wait to meet the new baby. Each NICU has its own guidelines about children visiting. Some NICUs only allow siblings who are over a certain age or allow visits during certain hours. Find out what the rules are in your NICU, then talk to your children before they go to the NICU about what they may see and hear. Here’s how you can prepare for their visits to the NICU:
- Plan to keep visits short (less than 30 minutes)
- Describe what they may see or hear
- Explain what equipment in the NICU does
- Tell your children what they can do and how to behave in the NICU
Talk to your children after they spend time in the NICU. Ask if they have any questions about the baby or the equipment. Answer their questions simply but honestly.

(Section of Back to Basics, Bonding and Attachment In The Neonatal Unit Irish Neonatal Health Alliance)
You might worry that you won’t be able to bond with your premature baby in the NICU. It’s true that you are separated from your baby because he needs to be cared for in the hospital. You might not be able to see and hold him early on, or even visit him as much as you’d like because of distance or older children. The worry about your baby’s health might also get you down. But there is a lot you can do in the NICU to feel close to your baby and develop a bond.
Even though your baby was born early, your baby ‘knows’ you – your voice and your smell. Your presence will give your baby a sense of familiarity and comfort. This is a great starting point for bonding. Here are some ideas to help you and your baby bond while he/she is in the NICU.
Watch your baby.
Premature baby body language is different from that of full-term babies but over time, you’ll learn how to tune into your baby and know whether he wants closeness, or whether he has had enough stimulation. The medical staff can help you start reading your baby’s signs.
The underlying principle involved in learning to read your baby’s body language is to observe and understand your baby’s developing ability to achieve balance i.e homeostasis. This means that your baby can have the neurological capacity under the right circumstances to move from an unbalanced (disorganized ie. fussy or crying) state to achieve a more balanced state (organised state i.e calm, alert). Sometimes your baby will require the help of a carer to move from a disorganized to an organised state. Under certain circumstances your baby can achieve this change from disorganised to organised themselves. This developing ability in premature infants is called self-soothing or self-regulation.
When observing your baby’s behaviour you should observe the sequence of events more than individual behaviours. There are 5 interconnected levels of baby behaviour and observations at one level will have an effect on one or more of the other levels.
Five Levels Of Infant Behaviour
1. The physiological level.
2. Muscle tone and quality of physical movements.
3. The level of state and alertness.
4. The level of interactive behaviour.
5. The stress level.
Physiological Signs
These are signs which can be observed directly by watching your baby closely.
Breathing and Pattern of Breathing
Note the skin colour around your baby’s mouth, eyes, hand and feet. Is your baby experiencing repeated hiccuping or excessive yawning?
Motor Tone and Motor Control
Motor tone consists of passive and active muscle tone. Passive muscle tone refers to how your baby resists stretching his limbs during caregiving. Passive muscle tone can by hypertonic (high), normal tone or hypotonic (low or floppy).
Active muscle tone refers to your baby’s tendency to keep or bring his limbs flexed or extended when he is alone. Your baby’s active muscle tone can be observed in the arms, legs, neck and body. As your baby develops he can more actively flex and extend his limbs with improved neuro-motor control.
Motor control can also be observed in terms of smooth or jittery, tremor like movements. Good motor control is seen as fluent and elegant movements with little or no tension/tremors/startles whereas poor motor control may appear as having little or no smooth movement and moderate levels of tremors or jitteriness.
3. Sleeping and Waking Behavioural States
Babies have six characteristic levels of arousal but it is not always easy to tell which is which in a premature baby as these states are immature and often fleeting.
Deep Sleep– Also referred to as “Quiet Sleep” because your baby does not move apart from occasional small startles and has higher overall muscle tone. Breathing is slower and more regular than other times. This state becomes more noticeable after 32 weeks gestation.
Light Sleep– Also referred to as “Active Sleep” because your baby moves about more. Rapid Eye Movements (REM) may be observed: breathing tends to be faster and more irregular than in quiet sleep with lower overall muscle tone.
Drowsy- This is an important part of the sleep cycle and your baby may appear “half awake” as if in transition from sleep to awake or awake to sleep. Some babies may require your assistance to go to sleep (comforting hold) or to wake up (see if your baby opens his eyes in response to your greeting).
Quietly Alert– It may be some time before you see your baby with his eyes open and in the early days the facial expression may appear strained or glazed. During periods of quiet wakefulness you can watch how your baby responds to you does he turn his head towards you when you speak? When he needs some time out does he turn away from your voice? It is important to read your baby’s cues in particular during moments of stress or when he needs a break and to respond appropriately. Some babies will close their eyes and go to sleep when they are feeling overwhelmed and others get hiccups, yawn or sneeze.
Actively Awake-Premature babies are often quite active with their eyes closed and it can be difficult to know they are awake or not. Fussy behaviour indicates that your baby requires something to change or stop. Over time you will discover methods of settling your own baby.
Crying-Premature babies seldom cry but demonstrate that they are upset with agitated movements, grimaces and a crying facial expression.
4. Interactive Behaviour
Your baby’s ability to achieve and maintain an alert state is an important developmental step. Babies can begin to process and learn from interaction when in a quiet alert state When your baby is able to stay awake or alert for a short time you can begin to observe his interaction with you or objects. If your baby is experiencing discomfort or over-stimulation from the environment he is less able to interact. It is advisable to ascertain if your baby is “available” or “not available” to interact by observing his behaviour.
Opportunities to observe interaction
– Note your baby’s reaction when you place your face close to your baby’s face and speak softly.
– How does your baby respond to sounds and voices in the surrounding environment?
– How does your baby respond to touch, handling and soothing?
Cues that your baby is ready to interact:
Babbling
– Soft smooth movement with arms and legs.
– Soft slow chewing. l Relaxed, open facial expression/movements.
– General muscle tone is average or lower.
– Little or no physical movements. l His breathing is regular and relaxed.
– His limbs are /relaxed/tucked/flexed close to his body.
– His mouth is relaxed and slightly open.
– His eyes are open or open in response to your voice.
– He calms upon hearing your voice
5. The Stress Level: Cues that your baby requires time to rest:
– He closes his eyes or turns away.
– His breathing becomes irregular.
– He may stretch or wriggle or arch his back.
– His body becomes limp or stiffens or the arms and legs straighten.
– He places his hand over his face (palm outward with fingers splayed).
– He frowns, grimaces, yawns*, grunts of hiccups.
– He falls asleep.
– His skin appears mottled or pale.
– Paroxysmal (at the extremities), circumoral (around the mouth) or periocular (around the eyes) cyanosis (blue colour) is visible.
– He displays roving eye movements or tight blinking.
When your baby is trying to achieve homeostasis (balance or a more organised calm state) he may display the following coping/self-soothing behaviours:
– Brings his hand to his mouth or his touches face. l Covers his eyes and ears.
– Clasps his hands or press one foot over the other. l Moves his body, lift or turn his head to get comfortable.
– Sucks his hand.
– Presses his feet against the bedding or cot. Grabs or hold onto the bedding, tubes or clothing.
– Brings his hands to the center line of his body.
– Turns away from strong stimuli.
Source: https://inha.ie/wp-content/uploads/2024/11/Back-To-Basics-Booklet.pdf

INNOVATIONS

Abstract
International collaborations between investigators in low-and-middle-income countries (LMICs) and high-income countries (HICs) in neonatal and fetal medicine have expanded over the past decade. This narrative review documents a rise in HIC–LMIC publications since 2014, with a plateau and transient dip during the COVID-19 pandemic. It analyses leadership, patient recruitment, and how HIC-based technologies and laboratory platforms shape research agendas. Many influential trials are conceived and sponsored by HIC institutions, with recruitment concentrated in LMICs because of higher disease burden, larger eligible populations and lower costs. Meanwhile, LMIC centers report growing readiness to support randomized controlled trials, and LMIC-conceived, led and completed multicentre studies are increasingly reported. Ongoing concerns include misalignment between donor priorities and national agendas, inequities in authorship and leadership, and ethical challenges related to standards of care, post-trial access, consent and compensation. The review compares regulatory, consent and insurance processes in India and the United States, and highlights enabling factors such as harmonised guidelines, global registries, political goodwill and professional networks. It anticipates a doubling of HIC–LMIC collaborative studies over the next decade, rapid growth of South–South partnerships, and gradual, though incomplete, correction of authorship and leadership imbalances in global neonatal and fetal medicine.
Source: https://www.sciencedirect.com/science/article/abs/pii/S1744165X26000399

A new era for Botswana’s healthcare system has begun. President Duma Boko has officially partnered with the Susan Thompson Buffett Foundation to transform maternal and reproductive health services in Botswana. At the heart of this groundbreaking move? A bold, tech-forward plan to digitize healthcare, save lives, and build long-term resilience in the system. With support from global health leader Dr. Senait Fisseha, this partnership brings serious funding and innovation to: ✅ Expand maternal health services ✅ Digitize Botswana’s healthcare delivery ✅ Address non-communicable diseases ✅ Strengthen national surgical and gynecological strategy 📊 “Data is power,” says Dr. Fisseha — and Botswana plans to use it wisely. 🌍 Could Botswana’s model lead the way for the rest of Africa? Tune in to find out — only on Snap Flash, where African progress meets real reporting. Botswana & Buffett Foundation Unite to Revolutionize Healthcare | President Boko’s Bold Vision.

Tiny Tech: Innovations Reshaping Neonatal Care
By Juliane Crafton, MSN RNC-NIC
Imagine—on a bright summer day in 1901, you walk into the Pan-American Exposition, a world’s fair in Buffalo, New York. Struck by the foreign architecture and bold colors, you explore. From fine art to horticulture to a Native American village, all the western hemisphere’s best advancements are on display. Soon, you find yourself in a room lined with unfamiliar machines and nurses, showcasing the tiniest babies you have ever seen.
The incubator was a landmark innovation, marking the beginning of a technological revolution in neonatal care (“Baby incubators at the Pan-American Exhibition,” 1901; Reedy, 2003). Over the 20th century, the incubator was joined by a wave of other life-saving technologies, such as pulse oximetry, phototherapy, and transcutaneous carbon dioxide monitors (Brennan et al., 2019; Hay, 2005; Parga & Garg, 2017).
Today, the pace of innovation is accelerating, demanding that neonatal nurses continuously adapt to improve safety and efficiency in caring for these tiny patients. This rapid evolution not only introduces new tools for care but also fundamentally reshapes the neonatal nurse’s role, demanding new skills in data interpretation and raising complex ethical considerations.
What’s New and What’s Coming
The technological boom of the late 20th century ushered in a new era for neonatal care. While innovations like transcutaneous carbon dioxide monitors and ECMO are now widely used, their adoption is relatively recent, becoming standard only in the past few decades. Now, even more sophisticated technologies are emerging.
Krbec et al. (2024) describe emerging innovations, including remote sensing technologies that could rid the NICU of wired monitoring of vital signs. Developments in camera technology and improved affordability have led to an increase in the study of their use in health care. The focus has been on adult applications with pilot studies exploring the use of visible light, infrared light, and radar-based technologies to monitor vital signs (Chung et al., 2020; Krbec et al., 2024). Chung et al. (2019) describes a wireless epidermal system with in-sensor analytics studied for neonatal use. Go to https://www.science.org/doi/10.1126/science.aau0780 to see images of the system on a neonate. Preliminary study has shown advanced capabilities in monitoring, along with a skinlike profile that reduces skin breakdown and reduces barriers for skin-to-skin contact.
Beyond passively monitoring vital signs, the next frontier involves artificial intelligence (AI) actively interpreting this data. Though there are many challenges and limitations, AI deep learning models have shown promising capability to detect features like subtle changes in movements or skin color and correlate them with vital sign changes and various pathologies (Krbec et al., 2024). Kwok et al. (2022) describes the use of deep learning models for prediction of neonatal mortality and morbidity, identifying patterns within data, interpreting data in relation to neuroimaging, performing image recognition, and predicting responses to neonatal treatment. Many NICUs already use some combination of early warning systems and scoring models to determine risk and predict adverse outcomes. Adding the additional layer of AI to deepen the ability to predict has great implications for providers and caretakers of this patient population.
Telehealth is emerging as a powerful tool to democratize neonatal expertise, bridging the critical gaps of distance and resources that can impact care. Through applications like remote specialist consultations and virtual grand rounds, these systems connect providers across different levels of NICUs, fostering collaboration that leads to improved outcomes. For instance, a tele-NICU program in Arkansas gives patients in rural hospitals unprecedented access to leading specialists through bidirectional information sharing (Arkansas Children’s, 2025). This model is not unique; similar pilot programs are being implemented in NICUs worldwide, demonstrating a global shift toward leveraging technology to overcome geographical barriers to care (Arkansas Children’s, 2025; Wagenaar, 2025).
On the cutting edge of regenerative medicine, three-dimensional (3D) bioprinting holds profound potential for neonatal care. Tottoli et al. (2020) describe a technique to create custom hydrogel scaffolds by “printing” a combination of biomaterials and a patient’s own cell cultures directly onto a wound. See Figure 5 in Tottoli et al.’s 2020 article. The resulting structure acts as a bioactive dressing—a living bandage that actively supports and accelerates skin regeneration, integrating concepts from cell therapy and tissue engineering. Although clinical applications for infants have not been thoroughly explored, the implications are significant (Tottoli et al., 2020). For premature infants with extremely fragile skin prone to injury, 3D bioprinting could one day offer a revolutionary approach to healing, minimizing scarring and the risk of infection. For premature infants with extremely fragile skin prone to injury, 3D bioprinting could one day offer a revolutionary approach to healing, minimizing scarring and the risk of infection.
Evolving Tools, Evolving Roles
The integration of these emerging tools does more than change workflows: it fundamentally redefines the identity and responsibilities of the neonatal professional. Already hands-on caretakers, nurses are evolving to add new responsibilities as critical data interpreters and technology managers who must validate predictions and facilitate care alongside sometimes-remote specialists. This evolution brings many important ethical considerations. The use of AI shows promise for predicting adverse outcomes but raises questions about algorithmic bias, data privacy, and accountability when a predictive model is wrong. Similarly, while telehealth can give low-access regions access to specialists, it introduces challenges in maintaining the human connection essential to care and ensuring equitable access for families with technological or resource barriers.
The emerging role of the neonatal caregiver is not just to be technologically proficient but to be a vigilant, ethical advocate, ensuring that these new, powerful tools are applied in a way that is safe and equitable and enhances compassionate, patient- and family-centered care.
Conclusion
From the simple, life-sustaining warmth of the first incubators to the complex predictive power of AI learning models, the evolution of neonatal care is a story of technological advancement. Innovations like remote sensing, telehealth, and 3D bioprinting are the tangible future, promising to further improve survival and long-term outcomes for the most fragile infants.
As these tools are integrated into practice, they demand an evolution in the role of the neonatal nurse: from a hands-on caregiver to a sophisticated clinical data analyst, technology facilitator, and ethical guardian. The ultimate challenge and opportunity lie not just in adopting the new technology but also in thoughtfully combining it with compassionate, human-centered care to ensure that every innovation serves the ultimate goal: helping the tiniest humans thrive.
Source: https://nann.org/publication/feature-35/



Step into the heart of Botswana’s Okavango Delta, where water gives life to everything it touches. In this short travel documentary, I explore the sacred relationship between nature, wildlife, and the waters that define this incredible region. From vast floodplains to close encounters with elephants, this film is a reflection of how deeply water shapes every step we take in the African wilderness.


Caring for the World That Helped Us Survive: A Summer Reflection from the Neonatal Womb Warriors Community
As summer approaches, many of us begin spending more time outdoors — walking along waterfronts, visiting parks, gathering with family, and reconnecting with nature after long winters and busy seasons of life. For the Neonatal Womb Warriors community, this season also offers something deeper: an opportunity to reflect on the world we are helping shape for future generations of children and families.
Climate change and environmental health are no longer distant issues. They are directly connected to the health and wellbeing of communities around the world — especially vulnerable populations such as premature infants, medically complex children, and families navigating fragile health journeys.
Air quality, extreme heat, pollution, natural disasters, access to clean water, and environmental instability all influence maternal and neonatal health outcomes. Research continues to show that environmental stressors can increase risks during pregnancy and impact neonatal and pediatric health. For families who have experienced NICU stays, neonatal complications, or the lifelong journey of prematurity, these realities feel especially personal.
But alongside these challenges comes hope — because communities everywhere are stepping forward to make a difference.
Summer often brings local opportunities for environmental conservation and neighborhood engagement: park cleanups, waterfront restoration projects, recycling initiatives, community gardens, tree planting events, and volunteer-driven beautification efforts. These moments may seem small, but collectively they reflect something powerful: people choosing to care for the environments that sustain all of us.
This summer, I will personally be participating in the Charles River Esplanade Cleanup in Boston — helping clean and preserve one of the city’s most treasured public spaces. For me, this is about more than environmental stewardship. It is about giving back to the communities and environments that support health, healing, resilience, and connection.
As preemie survivors, NICU families, healthcare workers, advocates, and supporters, we understand survival in a deeply human way. Many within our community began life fighting for every breath, every ounce of strength, and every milestone forward. That perspective often creates a unique appreciation for life, compassion, and community responsibility.
Environmental conservation is another form of protecting life.
- It is protecting cleaner air for children with chronic lung disease or asthma.
- It is preserving safe public spaces for families and children to gather.
- It is helping create healthier futures for the next generation of babies entering the world.
- And it is reminding ourselves that even small acts of service matter.
The Neonatal Womb Warriors community has always been rooted in resilience, advocacy, and hope. This summer, we encourage our community members to consider participating in local environmental or community service efforts in whatever way feels meaningful and accessible to them — whether that means joining a cleanup event, planting flowers, reducing waste, supporting conservation organizations, or simply spending intentional time caring for the spaces around us.
Every effort counts.
Together, we are not only survivors.
We are builders of healthier, kinder, and more compassionate communities.
And that includes caring for the world future womb warriors will inherit.


Jul 21, 2025
Ubongo Kids is an animated educational TV series produced in Tanzania and viewed across 40 countries in Africa. It targets children between the age of 7-14 and covers Science, Technology, Engineering and Mathematics (STEM) subjects and social emotional learning (SEL). Join Kibena, Kiduchu, Koba and Baraka as they go on adventures and use their brains to solve problems in Kokotoa Village, with the help of the animals of Kokotoa Forest!