PRETERM BIRTH RATES – RWANDA
Rank: 101 –Rate: 9.5% Estimated # of preterm births per 100 live births (USA – 12 %, Global Average: 11.1%)
Rwanda, officially the Republic of Rwanda, is a landlocked country in the Great Rift Valley, where the African Great Lakes region and East Africa converge. One of the smallest countries on the African mainland, its capital city is Kigali. Located a few degrees south of the Equator, Rwanda is bordered by Uganda, Tanzania, Burundi, and the Democratic Republic of the Congo. It is highly elevated, giving it the soubriquet “land of thousand hills”, with its geography dominated by mountains in the west and savanna to the east, with numerous lakes throughout the country. The climate is temperate to subtropical, with two rainy seasons and two dry seasons each year. Rwanda has a population of over 12.6 million[8] living on 26,338 km2 (10,169 mi) of land, and is the most densely populated mainland African country.
The population is young and predominantly rural. Rwandans are drawn from just one cultural and linguistic group, the Banyarwanda. However, within this group there are three subgroups. Christianity is the largest religion in the country; the principal language is Kinyarwanda, spoken by most Rwandans, with English and French serving as additional official languages. The sovereign state of Rwanda has a presidential system of government. Rwanda is one of only three countries in the world with a female majority in the national parliament, the two other countries being Bolivia and Cuba.
The quality of healthcare in Rwanda has historically been very low, both before and immediately after the 1994 genocide. In 1998, more than one in five children died before their fifth birthday, often from malaria.
President Kagame made healthcare one of the priorities for the Vision 2020 development programme, boosting spending on health care to 6.5% of the country’s gross domestic product in 2013, compared with 1.9% in 1996.
In recent years Rwanda has seen improvement on a number of key health indicators. Between 2005 and 2013, life expectancy increased from 55.2 to 64.0, under-5 mortality decreased from 106.4 to 52.0 per 1,000 live births, and incidence of tuberculosis has dropped from 101 to 69 per 100,000 people. The country’s progress in healthcare has been cited by the international media and charities. The Atlantic devoted an article to “Rwanda’s Historic Health Recovery”. Partners In Health described the health gains “among the most dramatic the world has seen in the last 50 years”.
Rwanda also has a shortage of medical professionals, with only 0.84 physicians, nurses, and midwives per 1,000 residents. The United Nations Development Programme (UNDP) is monitoring the country’s health progress towards Millennium Development Goals 4–6, which relate to healthcare.
Source:https://en.wikipedia.org/wiki/Rwanda


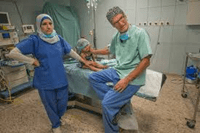
UNICEF/UN0321627/Kanobana Jemimah, right, sits with two other mothers in the Kangaroo Care room. Gahini Hospital did not always have the best care, but with more medical equipment and better trained doctors through the clinical mentorship programme, mothers like Jemimah feel safer and happier giving birth here.
Born too early: Rwanda’s smallest babies/UNICEF Rwanda
In Gahini Hospital, two paediatric mentor-trainers from the United Kingdom are training Rwandan doctors and nurses to better care for newborn babies who are born premature. The Rwandan health professionals then pass this knowledge to their peers and to the mothers and fathers of these babies.

COMMUNITY

Sweet, powerful, inspirational, chart topper Rwandan gospel music 2021. Enjoy!
Aline Gahongayire – Izindi Mbaraga featuring Niyo Bosco (Official Video 2021)
•Premiered Mar 5, 2021 #NiyoBosco #AlineGahongayire #newmusic

Commentary: Residency programs must address new interns’ divergent skills, experience
Jennifer R. Di Rocco, D.O., M.Ed., FAAP and Marissa H. Fakaosita, M.D., FAAP
March 17, 2021
We all have felt the strain of adapting to an ever-changing world of medical education during the COVID-19 pandemic.
Medical students and residents have been pulled from rotations, with some unable to experience core rotations in person or have experienced them much later in their clinical training, often at diminished capacity.
Standardized tests have been postponed or canceled, making it problematic for residency programs to evaluate candidates equally. Most visiting rotations were not possible, and interviews and hospital tours have been conducted exclusively on a virtual platform. This has made it exceedingly difficult to assess a candidate’s interpersonal skills and body language, which offer valuable, distinguishing information (Hammoud MM, et al. JAMA. 2020;324:29-30).
Residency programs and applicants alike have gone to great lengths to bolster their online presence. Yet, it feels like both sides are wearing blinders when making match lists outside of home institutions, as they base choices on virtual versions of people and places.
On Match Day 2021, filling an intern class and matching into an accredited residency program still will be the benchmark of a successful match. But where will we go from there?
Despite the numerous challenges and limitations that a virtual residency recruitment season brings, there are some benefits that could permanently transform what residency recruitment and the “interview trail” look like. Virtual recruitment naturally expands and diversifies a residency program’s applicant pool and allows for increased convenience in scheduling interviews. Further, the cost savings of forgoing travel allows for a more equal and consistent process for all applicants. Ultimately, remotely conducted meetings and interviews are not only modern, they have become the new normal. Programs that revert to a recruitment strategy that lacks any virtual component likely will be outliers.
Whatever results Match Day brings on March 19, each program will need to scrutinize its recruitment processes and strategies, looking forward to new national recommendations to shape the next match season.
Programs also will have to prepare for their new intern class. Students and residents in pediatrics have had much less clinical exposure in the inpatient and outpatient settings, with national volumes of pediatric patients being significantly lower during quarantine and school closure periods. Residency programs will need to accept that their intern class will have had widely variable clinical exposure and experience. Programs should look closely at transcripts and have discussions with incoming interns early in the academic year to appreciate their clinical exposure. Simulation-based learning exercises during intern orientation may help identify areas that need strengthening prior to the busy fall and winter seasons. Programs then should design individualized educational units to strengthen experiential learning and create tailored plans for resident success. Faculty also will need to adjust their expectations as we all strive to comprehend the practice gaps that may exist for our new interns and rising supervisory residents.
Competency-based assessment will be of the utmost importance as we won’t be able to measure time-based training in the same fashion, with interns starting the year with widely divergent skills and expertise. The Accreditation Council for Graduate Medical Education Pediatrics 2.0 Milestones are being finalized and hopefully will offer programs and residents a more streamlined, practical tool to assess these competencies.
This year’s match has presented many challenges, but some surprising benefits may change the way we interact with resident candidates moving forward. As we weather this storm in pediatric medical education, let us share ideas to prepare the next cohort of residents to become pediatricians during this uncertain time.
Dr. Di Rocco is an associate program director of the University of Hawaii Pediatric Residency Program and a pediatric hospitalist. Dr. Fakaosita is co-chair of the Recruitment and Selection Committee and directs the Individualized Educational Unit curriculum at University of Hawaii Pediatric Residency Program and is a pediatric hospitalist.
Copyright © 2021 American Academy of Pediatrics
Source: https://www.aappublications.org/news/2021/03/17/match-day-commentary-031721

Incivility and Bullying in the NICU

March 13, 2021
Nurses are known to be compassionate, caring, and committed to their patients. These same nurses can sometimes be harsh and uncaring toward their colleagues. In this episode, Jill and Beth Bolick address incivility and bullying in the NICU. Beth, Professor at Rush University Medical Center College of Nursing, is a national speaker on the topic of bullying and incivility. There are a variety of ways incivility and bullying seep into the NICU – from gossip, teasing, eye-rolling, withholding business information, to even physical altercations. Beth and Jill dive into how bullying goes beyond the dyad of just two colleagues and impacts your entire unit and even direct patient care. Listen in to learn more about how to create a unit that is more civil and welcoming to colleagues and patient families alike.
Visit http://stopbullyingtoolkit.org/ for some of the free resources Beth discusses.
Source: https://www.podbean.com/site/EpisodeDownload/PBFD7814UFFWJ

Physician Support Line – 1 (888) 409-0141

Our mission at Physician Support Lifeline is to offer free and confidential peer support to American physicians and medical students by creating a safe space to discuss immediate life stressors with volunteer psychiatrist colleagues who are uniquely trained in mental wellness and also have similar shared experiences of the profession.
Our Vision
We hope ultimately to build a sustainable community of peer support and wellness for physicians and medical students across the United States.
Our Goals
- To normalize pursuit of mental wellness by physicians and medical students
- To encourage unity and empathy among physician colleagues
- To provide a resource for physician and medical student emotional wellness to healthcare organizations and institutions
Welcome! We are here for you! Please see below for resources that you may find helpful. If you have called PSL and been referred to this page, thank you for reaching out! If you are just visiting and decide you need more support than what is below, please call 1-888-409-0141.
Coping with the Pandemic
- 25 Tips for Coping With Quarantine
- Wellness of Physicians During COVID19 Outbreak
- FACE COVID eBook – by Russ Harris
- WHO Mental Health Considerations for the general public, healthcare workers, leadership, and those who have been exposed
- Podcast: A Bit of Relief – Alone Together
- APA – Taking Care of Ourselves During Infectious Disease Outbreaks
- Living With Mental Illness During Covid19 Outbreak
Coping with Boredom
- Things To Do
- 10 University Art Classes You Can Take For Free Online
- Fun Things That Weren’t Free Before Coronavirus But Are Now
- Rosetta Stone (90 days free for students)
- Live Streaming Fitness Resources
Feel Better Right Now
- 5 Tiny Desk Concerts to Calm Your Mind
- The Well Being Initiative – Live and Pre-recorded Lift Sessions
- Podcast: Meditation Minis
- Podcast: The Happiness Lab
Sleep and Insomnia
Thoughtful Words
Anxiety
- JAMA Opinion Article: Understanding and Addressing Sources of Anxiety
- Progressive Muscle Relaxation
- Coronavirus Anxiety: Coping with Stress, Fear, and Uncertainty
- Covid19 Lockdown Guide: How to Manage Anxiety and Isolation During Quarantine
- Podcast: A Mindfulness Tool to Help With Coronavirus Anxiety
- Podcast: Ten Percent Happier – How to Handle Coronavirus Anxiety
Medical Practice-Related
- How To Convert Your Practice to Telemedicine
- Physicians Guide to COVID19
- Medicare Telemedicine Health Care Fact Sheet
- Telemedicine DEA Guidance
- AMA – Managing Mental Health During Covid19
Need Ongoing Care?
Supporting Your Children
- Managing Indoor Boredom for Kids
- How to Talk to Your Kids About Mental Health
- How to Talk to Your Kids About Covid19
- Ten Tips to Stay Mentally Healthy
- Dr. Panda Coronavirus YouTube Video for Kids
- The Coronavirus Explained YouTube Video
- Safety Measures for Coronavirus YouTube Video
Supporting Your Community
COVID19 For Providers and Community Leaders https://www.doctorlifeline.org/
PREEMIE FAMILY PARTNERS
Grandmothers -A Neglected Family Resource For Saving Newborn Lives
Across the globe, the well-being of newborns is significantly influenced by the knowledge and practices of family members, yet global health policies and interventions primarily focus on strengthening health services to save newborn lives. Predominant approaches to promote newborn survival in non-western cultures across the Global South are based on a western, nuclear family model and ignore the roles of caregivers within wider family systems, whose attitudes and practices are determined by culturally prescribed strategies. In this paper, [the author reviews] evidence of a neglected facet of newborn care, the role and influence of senior women or grandmothers.
Summary
- Interventions to promote newborn health and survival in the Global South primarily focus
on young mothers based on a Eurocentric view of nuclear family structure.
- Evidences from studies in numerous cultural contexts across Africa, Asia and Latin America reveal the significant role and influence of experienced older women, or grandmothers, on newborn care within multi-generational family systems.
- Research reviewed from non-western collectivist cultures across the Global South suggests that grandmothers play similar core roles with newborns through advising and direct caregiving while their culturally specific practices vary greatly.
- Future newborn policies and research should be grounded in a family systems frame that reflects the structure and dynamics of families in non-western collectivist cultures.
- Grandmothers’ knowledge is sometimes out of date, but given their proximity, authority and commitment to newborn survival they should be explicitly involved in newborn interventions in order to optimise this abundant local resource for newborn health and survival.
Full Article: https://gh.bmj.com/content/bmjgh/6/2/e003808.full.pdf

NICU nurses help dad pop the question | Humankind
The look on mom’s face when she walked in the room was one of absolute shock.

Yale study finds link between autism in children, premature birth of their parents
Researchers at the Yale School of Public Health conducted the first study revealing that the preterm birth and low birth weight of parents could mean a higher risk of their children being diagnosed with autism.
Sydney Gray – FEB 08, 2021
Autism spectrum disorder, or ASD, in children may be linked to the premature birth of their parents, according to a Yale School of Public Health study.
Assistant Professor of Epidemiology Zeyan Liew and graduate student Jingyuan Xiao GRD ’26 examined the medical records of nearly 400,000 mother-child and father-child pairs. The researchers found that children had nearly double the risk of ASD if their mothers and fathers were born at earlier than 32 gestational weeks compared to children whose parents were born at term. The study was published in the International Journal of Epidemiology on Jan. 7.
“The worldwide prevalence of autism spectrum disorder (ASD) is increasing, but scientific understandings regarding the etiology of this multifactorial and complex neurodevelopmental conditions are still limited,” Liew and Xiao wrote in an email to the News. “We conducted this study to evaluate whether adverse birth characteristics of the parents … could influence ASD risk in their offspring.”
The researchers analyzed data from a cohort of 230,174 mother-child and 157,926 father-child pairs in Denmark to examine the multigenerational risk factors that might contribute to the prevalence of ASD.
The scientists also collected data on the grandparents’ and parents’ sociodemographic factors, age when pregnant, geographical location and mental health to include in their statistical models. They said that Denmark’s national health care and centralized medical records system helped make this type of longitudinal family linkage research possible.
The researchers used a pregnancy term of 37 weeks and a birth weight of 2,500 grams as a baseline reference. They found that mothers and fathers who were born prematurely — at fewer than 37 weeks of gestation — or with a low birthweight had a 30 to 40 percent higher risk of having children with ASD. Meanwhile, parents born at fewer than 32 gestational weeks had nearly double the risk of later having children with ASD, compared to parents born at term.
In the past, many studies on ASD have focused on environmental risk factors such as prenatal exposure to air pollution. Additionally, studies of family members of children living with ASD have largely centered on siblings instead of multigenerational data, the scientists said.
“It is known that certain genetics and fetal exposure to environmental risk factors contribute to the risk of ASD, but these known factors don’t fully explain the occurrence of all ASD cases in populations,” wrote Xiao and Liew. “Recently, new hypotheses regarding multigenerational risk for ASD have been proposed in animal models, but epidemiological evidence is still lacking.”
The Autism Center for Excellence Program at Yale, or ACE, led by professor Katarzyna Chawarska, currently has ongoing projects examining the brain connectivity of school-age siblings of children with autism to better comprehend how this relates to the severity of autism symptoms. Another ACE project aims to identify genetic markers linked to autism by studying the biological differences during early development of the brain in sibling pairs where one or both siblings are diagnosed with ASD.
Chawarska said she was “peripherally” involved in contributing to Liew and Xiao’s study but declined to comment further.
Xiao and Liew noted that additional studies are required to elucidate how ASD is transmitted across generations.
“It might be important to study specific grandparental and environmental factors that can directly impact on parental in-utero development,” Xiao and Liew wrote.
The scientists explained that prior research on multigenerational factors and ASD suggests that grandmaternal smoking and the use of diethylstilbestrol — a compound given to pregnant women between 1938 to 1971 to prevent pregnancy complications — potentially hinder neurodevelopmental health in grandchildren.
Xiao and Liew said that future studies should follow the development of parents born with adverse birth characteristics, such as low birthweight or preterm birth, to identify other postnatal factors that may have contributed to ASD in their children. The researchers hope these paths for future investigation could be a means to mitigate ASD transmission pathways within families.
The Centers for Disease Control and Prevention estimates that 1 in 54 children has been diagnosed with ASD in the United States.
Sydney Gray | sydney.gray@yale.edu

Extreme Preemies Grow Up: Against the Odds
Mar 19, 2021


INNOVATIONS
Quality Improvement Approach to Reducing Admission Hypothermia Among Preterm and Term Infants
Alicia Sprecher, Kathryn Malin, Deanna Finley, Paula Lembke, Sally Keller, Ann Grippe, Genesee Hornung, Nicholas Antos and Michael Uhing Hospital Pediatrics March 2021, 11 (3) 270-276; DOI: https://doi.org/10.1542/hpeds.2020-003269
Abstract
BACKGROUND: Newborns, particularly premature newborns, are susceptible to hypothermia when transitioning from birth to admission to the NICU, potentially leading to increased mortality and morbidity. Despite attention to this issue, our rate of admission hypothermia was 39.8%.
METHODS: We aimed to reduce the rate of admission hypothermia for all inborn infants admitted to our institution to <10%. We undertook a quality improvement effort that spanned from 2013 through 2019 in our level IV NICU. Current state analysis involved investigating patient risk factors for hypothermia and staff understanding of hypothermia prevention. Improvement cycles included auditing processes, an in-hospital relocation of our NICU, expanded use of chemical heat mattresses and polyethylene bags, and staff education. Improvement was evaluated by using Shewhart control charts.
RESULTS: We demonstrated a reduction in admission hypothermia from 39.8% to 9.9%, which was temporally related to educational efforts and expanded use of chemical heat mattresses and polyethylene bags. There was not an increase in admission hyperthermia over this time period. We found that our group at highest risk of admission hypothermia was not our most premature cohort but those infants born between 33 and 36 6/7 weeks’ gestation and those infants prenatally diagnosed with congenital anomalies.
CONCLUSIONS: Expanded use of polyethylene bags and chemical heat mattresses can improve thermoregulation particularly when combined with staff education. Although premature infants have been the focus of many hypothermia prevention efforts, our data suggest that older infants, and those infants born with congenital anomalies, require additional attention.
- Copyright © 2021 by the American Academy of Pediatrics
Source: https://hosppeds.aappublications.org/content/11/3/270

A National Survey on Physician Trainee Participation in Pediatric Interfacility Transport

Pediatr Crit Care Med – 2020 Mar;21
Elizabeth A Herrup , Bruce L Klein , Jennifer Schuette , Philomena M Costabile , Corina Noje
Abstract
Objectives: To ascertain the national experience regarding which physician trainees are allowed to participate in pediatric interfacility transports and what is considered adequate education and training for physician trainees prior to participating in the transport of children.
Design: Self-administered electronic survey.
Setting: Pediatric transport teams listed with the American Academy of Pediatrics Section on Transport Medicine.
Subjects: Leaders of U.S. pediatric transport teams.
Interventions: None.
Measurements and main results: Forty-four of the 90 U.S. teams surveyed (49%) responded. Thirty-nine (89%) were university hospital-affiliated. Most programs (26/43, 60%) allowed trainees to participate in pediatric transport in some capacity. Mandatory transport rotations were reported for pediatric critical care (PICU) fellows (9/42, 21%), neonatology (neonatal ICU) fellows (6/42, 14%), pediatric emergency medicine fellows (4/41, 10%), emergency medicine residents (3/43, 7%), and pediatric residents (2/43, 5%). Fellow participation was reported by 19 of 28 programs (68%) with PICU fellowships, 12 of 25 programs (48%) with pediatric emergency medicine fellowships, and 10 of 34 programs (29%) with neonatal ICU fellowships. Transport programs with greater than or equal to 1,000 annual incoming transports were more likely to include PICU and pediatric emergency medicine fellows as providers (p = 0.04; 95% CI, 1.04-25.71 and p = 0.02; 95% CI, 1.31-53.75). Most commonly, trainees functioned as medical control physicians (86%), provided minute-to-minute medical direction for critically ill patients (62%), performed intubations (52%), and were code leaders for patients undergoing cardiopulmonary resuscitation during transport (52%). Most transport programs required pediatric residents, PICU, and pediatric emergency medicine fellows to complete a PICU rotation prior to participating in pediatric transports. The majority of transport programs did not use any metrics to determine airway proficiency of physician trainees.
Conclusions: There is heterogeneity with regard to the types of physician trainees allowed to participate in pediatric interfacility transports, the roles played by physician trainees during pediatric transport, and the training (or lack thereof) provided to physician trainees prior to their participating in pediatric transports.
Source: https://pubmed.ncbi.nlm.nih.gov/32142489/
Maternal participation on preterm infants care reduces the cost of delivery of preterm neonatal healthcare services

Background
Thailand, with an annual incidence rate of 12% ranks high in incidence of preterm birth. Preterm infants require specialized care which can be lengthy and costly both in terms of psychological and emotional stress and healthcare services. The rapid rise of cost of healthcare services is a major concern for Thai government and public.
Purpose
To assess and compare the growth patterns and cost of delivery of healthcare services of 50 preterm infants who were randomly assigned to either the control arm or the Maternal Participation Program (MPP) arm of the study.
Methods
25 infants in the control arm and 25 infants in the MPP arm were followed up from the day of transfer to the neonatal ward until they were discharged from the hospital. Data on clinical parameters and cost of healthcare delivery were collected by reviewing medical charts and from institutional financial databases. The principle of intention-to-treat analysis was used to analyze the data using the SPSS package (Version 23).
Results
The average hospital stay (53 days vs. 60, P = .427) and days of oxygen delivery (21 days vs. 45, P = .047) for infants in the MPP arm were shorter than the control. At discharge from hospital, growth velocity of infants in the control arm had caught up with the MPP arm. Overall costs of healthcare delivery services for the preterm infants in control arm were 1.75 times higher than those in the MPP arm, with the procedural services as the costliest. Costs of drugs and the other ancillary services for the control arm was about 3-fold higher than for the MPP arm.
Conclusion
There were similar growth patterns and weight gain between the preterm infants in the control arm and the intervention arm. However, health care cost in preterm infants in the control arm was no statistically significant higher than those of the MPP arm. The difference of health care cost may arise from healthcare services and clinical interventions. Innovative and simple alternative strategy such as MPP can be an effective approach to curb the escalating cost of healthcare services.
Source:https://www.sciencedirect.com/science/article/abs/pii/S1355184120300454#abs0010
Parents’ experiences of emotional closeness to their infants in the neonatal unit: A meta-ethnography

Abstract
Background
Physical and emotional parent-infant closeness activate important neurobiological mechanisms involved in parenting. In a neonatal care context, most research focuses on physical (parental presence, skin-to-skin contact) aspects; insights into emotional closeness can be masked by findings that overemphasise the barriers or challenges to parenting an infant during neonatal care.
Aim
To explore existing qualitative research to identify what facilitates and enables parents’ experiences of emotional closeness to their infants while cared for in a neonatal unit.
Study design
A systematic review using meta-ethnographic methods. Search strategy involved searches on six databases, author runs, and backward and forward chaining. Reciprocal translation was used to identify and compare key concepts of parent-infant emotional closeness.
Results
Searches identified 6992 hits, and 34 studies from 17 countries that involved 670 parents were included. Three overarching themes and associated sub-themes were developed. ‘Embodied connections’ describes how emotional closeness was facilitated by reciprocal parent-infant interactions, spending time as a family, and methods for parents to feel connected while physically separated. ‘Inner knowing’ concerns how knowledge about infant and maternal health and understanding the norms of neonatal care facilitated emotional closeness. ‘Evolving parental role’ relates to how emotional closeness was intertwined with parental identities of contributing to infant health, providing direct care, and being acknowledged as a parent.
Conclusion
Parent-infant closeness evolves and is facilitated by multifaceted biopsychosocial factors. Practice implications include creating private and uninterrupted family time, strategies for parents to maintain an emotional connection to their infant when separated, and neurobiology education for staff.
HEALTH CARE PARTNERS

The Next Generation of NICU Staff
Kelly Welton, RRT-NPS
2020 wreaked havoc on all of us. Life’s rhythm as we knew it in 2019 got transformed as we learned a new way to do almost everything in 2020. Although Zoom and Amazon saved many people from unnecessary trips to the office and the store, one thing remained unchangeable: healthcare, specifically patient care, is a hands-on business. Since patient care is a hands-on profession, training requires a mentor to show us the how-tos. It is one thing to learn how to set up a ventilator or an IV pump; another thing entirely to troubleshoot one that’s not doing what you set it to do. Thanks to SARS-Covid-19 [CoVid], many respiratory therapy and nursing school programs closed. First, clinical sites closed their doors so as not to expose students to this new virus that was spreading fast. Then schools closed their doors to in-person instruction. Forced to learn online, recent graduating classes will only get their ‘hands-on ‘experience once hired.
In the hospitals, current staff who want to be trained to work in NICU often need approval from their manager. In Southern California, there were two programs available that provided in-depth NICU classes and clinical training. Both programs have subsequently closed, leaving nowhere for therapists to get basic NICU training. Managers are also tasked with being chronically short staffed, unable to let a staff member shadow a NICU RT for a day because they are desperately needed in the other hospital areas. This situation has been true for decades; however, CoVid demanded all-hands-on-deck, and there was no time for any RT not to carry a workload.
As an RT Educator, my role has been to find the areas in which staff need additional training. Whether it is low-use equipment or training in a new area, competency in not just knowledge. Critical thinking and troubleshooting are also ‘musts.’ Although the NICU was not left untouched by Covid, when the CoVid dust settles, many RT’s and RN’s will either leave the field or seek solace in a place that is not calling a code every hour and losing 3-4 patients per shift. When these seasoned therapists retire, who will be left to care for patients? For these reasons, the Academy of Neonatal Care was formed. Initially, AoNC was designed to be a hands-on workshop. Participants learn the foundation of neonatal respiratory care and participate in workshops practicing correct fitting of nasal prongs, changing Oscillator circuits, surfactant instillation, and more. Covid has now challenged AoNC as well to translate learning to an online format. Clinical competency software and the ability to present live online courses where students can ask questions in real-time help AoNC fill the void.
As a non-profit 501 (c) 3, the Academy of Neonatal Care’s goal is to teach the highest level of care to beginners in NICU and seasoned therapists. RN’s are welcome to join, as are physicians.
Our secondary goal is to reach out to NICU babies’ parents and family to support them while their baby is in our care. Lastly, as a non-profit, we will give back by contributing to community outreach and support healthy pregnancy and healthy baby efforts across the world.
With the release of a CoVid vaccine, we look forward to presenting live and in -person. AoNC’s platform continues to change with the times, but our ‘base camp’ remains the same. We built day one for beginner RT’s and RN’s who have wanted to learn NICU but have never been given a chance to get into a NICU with a preceptor.
Day 2 is designed for the RT that floats to NICU occasionally and wants a refresher to reinforce skills and knowledge.
Day 3 is designed for current NICU staff who want to expand their knowledge on subjects such as Jet ventilation, iNO, Transports, and more. The way we are going, we may soon have a full 5-day course!
Academy of Neonatal Care’s vision is that when the first three days are completed, the RT has a certificate from AoNC that says, “I finished the entire AoNC course, and am now ready to work with a preceptor.” That certificate carries significant weight with the participant’s employer or director, enough so that the manager would feel confidant pairing the RT with a mentor to help them assimilate into NICU.
Kelly Welton, RRT-NPS President, Academy of Neonatal Care @ www.AcademyofNeonatalCare.org
Source: http://www.neonatologytoday.net/newsletters/nt-mar21.pdf

HEALTHCARE WORKERS
Healthcare is the fastest-growing sector of the U.S. economy, employing over 18 million workers. Women represent nearly 80% of the healthcare work force. Healthcare workers face a wide range of hazards on the job, including sharps injuries, harmful exposures to chemicals and hazardous drugs, back injuries, latex allergy, violence, and stress. Although it is possible to prevent or reduce healthcare worker exposure to these hazards, healthcare workers continue to experience injuries and illnesses in the workplace. Cases of nonfatal occupational injury and illness with healthcare workers are among the highest of any industry sector.
Source: https://www.cdc.gov/niosh/topics/healthcare/default.html

The Persistent Pandemic of Violence Against Health Care Workers
December 11, 2020 Ashleigh Watson, MD , Mohammad Jafari, HBSc , Ali Seifi, MD
The American Journal of Managed Care, December 2020, Volume 26, Issue 12
The problem of violence against health care workers has escalated across the world, and tackling this issue requires the support of administrators.
ABSTRACT
Violence against health care workers is an ever-present threat that has been increasing over the past several years. The majority of physicians and nurses report that they have been victims of workplace violence at least once throughout their careers. Such violent attacks negatively affect the delivery, quality, and accessibility of health care. Certain factors such as substance abuse and intense emotions increase an individual’s risk of committing an act of workplace violence against a health care worker. Encountering violent individuals has legal implications and can compromise the moral framework of physicians. With action from institution administrations, advocates, leaders, and government, this issue that detrimentally affects health care can be combatted and reduced. By implementing required staff training, increasing security, strengthening the doctor-patient relationship, using medical chaperones, and reforming policy, positive changes can be made to protect health care workers and the health care system.
Takeaway Points
- The support of health care administrators, leaders, and national advocates is essential and necessary for tackling health care workplace violence and protecting health care workers.
- Hospitals need to implement required staff training, increase security, strengthen the doctor-patient relationship, use medical chaperones, and reform policy, among many constructive steps necessary to decrease the incidence of violence against health care workers.
The Occupational Safety and Health Administration defines workplace violence (WPV) as “any act or threat of physical violence, harassment, intimidation, or other threatening disruptive behavior that occurs at the work site. It ranges from threats and verbal abuse to physical assaults and even homicide.” In 2014, it was reported that workers in the medical field encounter more nonfatal incidents of WPV than workers in any other profession. The risk of health care workers encountering violence in the hospital is ever present, and it appears that this violence is actually increasing. In this article, we will discuss the pandemic of violence and strategies that a physician can use to control explosive situations.
Violence against health care workers, especially in the hospital setting, is a global issue that affects both developed and developing countries. A comprehensive literature review shows that research studies have been conducted in the United States, United Kingdom, China, Iraq, Germany, Ethiopia, Jordan, Palestine, Nigeria, and many more nations, all indicating that the majority of physicians and health care workers have experienced some form of WPV. In fall 2014, a poll found that 71% of physicians in the United States had experienced at least 1 incident of violence at some point during their careers. Of the physicians in Michigan surveyed in 2002, 75% were victims of at least 1 incident of verbal threatening during a 12-month period, whereas 28.1% of respondents experienced physical assault. Nurses typically sustain the most WPV compared with other health care workers. A study in 2000 found that 82% of US nurses had been assaulted at least once during their careers, and 73% believed that assault was just part of their job. For physicians, the rate of violence is highest in the emergency department and among less-experienced physicians. Studies have shown that the most common acts of violence against nurses were shouting or yelling (60.0% by patients, 35.8% by visitors), swearing (53.5% by patients, 24.9% by visitors), and grabbing (37.8% by patients, 1.1% by visitors).
In 2016, 16,890 workers in the private industry experienced WPV that required days away from work. Of those victims, 70% worked in the health care and social assistance industry, according to the CDC.
The implications of WPV against health care workers are detrimental to not only the victimized individual but also the entire health care system. From physical injuries to psychological trauma, violence can lead to demotivation, poor job satisfaction, and early physician burnout. Overall, WPV affects the delivery of health care, decreasing quality and accessibility.
Numerous factors contribute to the escalating levels of violence against health care workers in the hospital setting. The majority of attacks come from patients or family members who have problems with substance abuse, a mental illness, or drug-seeking habits. Furthermore, the generalized fear, helplessness, and stress felt by individuals seeking medical attention and by their loved ones, especially when the patient is critically ill and there is frustration with the health care system, lead to increased risk of WPV in hospitals.2 These strong emotions and anger that individuals may harbor can emerge and be inappropriately directed toward health care workers. Additionally, a history of violence increases the risk that an individual will commit an act of WPV.
Currently, only 26 of 50 US states have any law to protect health care workers from assault, and the laws in the majority of these states protect only a small sector of the health care field. For example, penalties in Louisiana apply only to emergency department workers and those in Kansas apply only to mental health employees. In many states, the right to refuse treatment of abusive patients is allowed by law; however, under the Emergency Medical Treatment and Labor Act of 1986, emergency departments must treat all patients who present for care, regardless of abusive actions.
Encountering violent patients has serious ethical implications for physicians, potentially compromising the moral framework on which the practice of medicine was founded. The Hippocratic Oath clearly delineates that a physician should treat every patient, and no patient should go without the care they need. Physicians have an ethical obligation to practice nonmaleficence and beneficence regardless of minimal personal risk. However, if a patient or their family member is acting violently or aggressively at the hospital and abusing the physician, nurses, or other staff members, a personal decision can be made to refuse treatment during their violent episode. When contemplating refusing treatment, the welfare of the physician and staff must outweigh the responsibility to care for the patient. Complete termination of the patient-doctor relationship should be executed only in extreme circumstances, as abandonment of a patient is not ethically or legally permitted.
Physicians are also ethically obligated to respect patients as individuals and to exercise compassion and empathy in their interactions. When working with an abusive patient, physicians must block their personal emotions and assess some ethical challenges: Is the behavior voluntary? Does failure to assign responsibility to the patient undervalue them as an individual? Should they be held responsible for their actions or are they victims of their environment? The answers to these questions may differ with each incident, but they should be used to evaluate behavior and to judge the necessary steps for advancing with care.
Violence against health care workers at hospitals is a preventable problem, and the incidence rate can be diminished with collaboration, change, and reform. Required training that focuses on recognizing and responding to abusive patients and family members would better prepare health care workers to respond to violent individuals and mitigate escalation. Some hospitals use flagging systems that alert medical staff about patients’ histories of violence. This way, clinicians can be better prepared to defuse difficult situations. At the Portland Veterans Affairs Medical Center, for instance, the staff was alerted about patients with a history of violence; this resulted in reducing the number of violent attacks by 91.6%.
Increased security has also been proposed as a way to decrease WPV in health care environments. Henry Ford Hospital in Detroit, Michigan, recently installed metal detectors, and a New York City hospital also increased its security by effectuating an identification badge system, limiting patients and visitors to specific floors of the hospital. This effort reduced violent crimes by 65% over 18 months.
In addition, making subtle changes to the doctor-patient relationship may be advantageous in decreasing WPV. For instance, practicing increased empathy, shared understanding, and cooperation may help decrease patient and guest frustration, stress, and other potentially volatile emotions. This is evident from the results of a 2012 study concluding that nurse-patient relations have a significant impact on WPV and that empathic communication with patients can significantly reduce the chances of violent behavior. The use of a medical chaperone may also decrease the risk of WPV, potentially protecting the physician from abuse and violence. From personal experience, patients and families can experience less anger and frustration when health care professionals take some time to sit with them, show sympathy, listen, and potentially involve the palliative care team.
Motivating the leaders of health care institutions is instrumental in enacting positive change to combat the increasing levels of violence. If hospitals enforced a mandatory reporting policy in which the administration would fully support staff, WPV in the health care setting would be better documented and the necessary actions against offenders would be taken more effectively. Post event counseling should also be mandated, given the high percentage of health care workers who suffer from psychological trauma and decreased job satisfaction after experiencing WPV; efforts need to be taken to focus on the mental health and wellness of employees. In addition, the attitudes of both staff and society regarding WPV in health care settings need to be addressed. Violence should not be considered just “part of the job” from the perspective of health care workers, and society needs to know that it is unacceptable to treat health care workers in a violent or abusive manner.
The National Health Service of the United Kingdom launched its Zero Tolerance Policy in 1999 in hopes of protecting its employees and eliminating the “fear of violence, abuse, and harassment from patients or their relatives.” The Zero Tolerance Policy allows health care facilities to freely seek police assistance, remove violent patients from their practice if necessary, and encourage and enforce reporting of WPV.
The problem of violence against health care workers, especially in critical care units, prevails and escalates across the world. It has been confirmed time and again that the vast majority of physicians, nurses, and supporting staff fall victim to WPV during their careers. Patients, family members, and visitors commit these violent and abusive attacks due to substance abuse, mental illness, and/or powerful emotions that manifest themselves in destructive ways. Violence challenges the moral and ethical obligations of physicians, leading to difficult decisions that may need to be made to protect others. The power and support of administrators, leaders, and national advocates are essential and necessary for tackling this issue and protecting health care workers. Implementing required staff training, increasing security, strengthening the doctor-patient relationship, using medical chaperones, and reforming policy are constructive steps that will decrease the incidence of violence against health care workers.
Source: https://www.ajmc.com/view/the-persistent-pandemic-of-violence-against-health-care-workers

Safe Health Workers, Safe Patients
The COVID-19 pandemic has unveiled the huge challenges and risks health workers are facing globally. Working in stressful environments makes health workers more prone to errors which can lead to patient harm. Health worker safety is a priority for patient safety. Speak up for health worker safety!

Social media & COVID-19: A global study of digital crisis interaction among Gen Z and Millennials
26 March 2021
WHO, Wunderman Thompson, the University of Melbourne and Pollfish share the outcomes of a global study investigating how Gen Z and Millennials get information on the COVID pandemic
The unfolding of the COVID-19 pandemic has demonstrated how the spread of misinformation, amplified on social media and other digital platforms, is proving to be as much a threat to global public health as the virus itself. Technology advancements and social media create opportunities to keep people safe, informed and connected. However, the same tools also enable and amplify the current infodemic that continues to undermine the global response and jeopardizes measures to control the pandemic.
Although young people are less at risk of severe disease from COVID-19, they are a key group in the context of this pandemic and share in the collective responsibility to help us stop transmission. They are also the most active online, interacting with an average number of 5 digital platforms (such as, Twitter, TikTok, WeChat and Instagram) daily.
To better understand how young adults are engaging with technology during this global communication crisis, an international study was conducted, covering approximately 23,500 respondents, aged 18-40 years, in 24 countries across five continents. This project was a collaboration between the World Health Organization (WHO), Wunderman Thompson, the University of Melbourne and Pollfish. With data collected from late October 2020 to early January 2021, the outcomes provide key insights on where Gen Z and Millennials seek COVID-19 information, who they trust as credible sources, their awareness and actions around false news, and what their concerns are. Some key insights uncovered include: Science content is seen as shareworthy

When asked what COVID-19 information (if any) they would likely post on social media, 43.9% of respondents, both male and female, reported they would likely share “scientific” content on their social media. This finding appears to buck the general trend on social media where funny, entertaining and emotional content spread fastest.
Awareness of false news is high but so is apathy
More than half (59.1%) of Gen Z and Millennials surveyed are “very aware” of “fake news” surrounding COVID-19 and can often spot it. However, the challenge is in recruiting them to actively counter it, rather than letting it slide, with many (35.1%) just ignoring.
Gen Z and Millennials have multiple worries beyond getting sick
While it is often suggested that young adults are ‘too relaxed’ and do not care about the crisis, this notion is not reflected in the data, with over 90% of respondents were very concerned or somewhat concerned about the risk of infection. Beyond getting sick themselves, the top concerns of respondents (55.5%) was the risk of friends and family members contracting COVID-19, closely followed by the economy crashing (53.8%).
WHO wants young people to be informed about COVID-19 information, navigate their digital world safely, and make choices to not only protect their health but also the health of their families and communities. These insights can help health organizations, governments, media, businesses, educational institutions and others sharpen their health communication strategies. Ensuring policy and recommendations are relevant to young people in a climate of misinformation, skepticism and fear.
All key insights can be downloaded here and an Interactive Dashboard with a breakdown of all data has been developed. A detailed report and analysis will be published in April by the University of Melbourne.


Those of us who partake in utilizing social media are constantly being bombarded by a vast array of information. In reference to the WHO partnered Covid-19 social media study it was encouraging to learn that many of us who are Gen-Z and Millennials are interested, invested, and actively engaged in wanting up-to-date access to scientific information on our social media platforms. Knowing that many of us have expressed concern about the potential risk of Covid-19 negatively affecting the health, safety and well-being of us, our family, friends, loved ones and community is reassuring. Being able to actively engage in helping to educate each other, learn the facts and care for each other through social media sharing has helped many of us keep connected to the world around us, check in on friends and maintain relationships in a time where many of us may experience feeling isolation. Together, we can all do our part to better the health and safety of our community and world. Sending a big shout out to the researchers, social media services and advocates sharing credible resources and support services on their services to keep us educated and safe!

No surfing in Rwanda. Witness the beauty and joy expressed in the faces of our Rwandan family as they enjoy land-based action, moving like the ocean surf……

Sports and Culture Week / Kigali / Rwanda / One Team
Feb 19, 2020 – KIGALI – Anton Sahler
ONE TEAM. We provide children and youths all over the world with access to sports. Through sports, we promote education, health and equality. We team up with our supporters, sports clubs, associations and enterprises as well as our local partners in the project countries. ONE TEAM