
AFGHANISTAN
Born Too Soon – Preterm Birth Rates
Rate: 11.5 Rank: 66
(USA Rate: 12.0% Rank: 54)
SOURCE: https://www.marchofdimes.org/mission/global-preterm.aspx#tabs-3
Afghanistan officially the Islamic Republic of Afghanistan, is a landlocked country located within south–central Asia. Afghanistan is bordered by Pakistan in the south and east; Iran in the west; Turkmenistan, Uzbekistan, and Tajikistan in the north; and in the far northeast, China.
Afghanistan is a unitary presidential Islamic republic with a population of 31 million, mostly composed of ethnic Pashtuns, Tajiks, Hazaras and Uzbeks. It is a member of the United Nations, the Organisation of Islamic Cooperation, the Group of 77, the Economic Cooperation Organization, and the Non-Aligned Movement. Afghanistan’s economy is the world’s 108th largest, with a GDP of $64.08 billion; the country fares much worse in terms of per-capita GDP (PPP), ranking 167th out of 186 countries in a 2016 report from the International Monetary Fund.
Health in Afghanistan is unsatisfactory but slowly improving. The Ministry of Public Health oversees all matters concerning the health of Afghanistan’s population. According to the Human Development Index, Afghanistan is the 15th least developed country in the world. Its average life expectancy at birth is reported at around 60 years. The country’s maternal mortality rate is 396 deaths/100,000 live births and its infant mortality rate is 66 to 112.8 deaths in every 1,000 live births.
There are over 100 government-run and private or internationally-administered hospitals in Afghanistan. The most advanced medical treatments are available in Kabul. The French Medical Institute for Children and Indira Gandhi Children’s Hospital in Kabul are the leading children’s hospitals in the country. The Kabul Military Hospital and the Jamhuriat Hospital are two of the popular hospitals in the country. In spite of all this, many Afghans still travel to Pakistan and India for advanced treatment
SOURCE: https://en.wikipedia.org/wiki/Health_in_Afghanistan
Our Focus for this blog is PREVENTION
Global prevention of preterm birth, maternal and infant mortality. Preventing/reducing PTSD for survivors, families and providers. Preventing and reducing health care provider shortages.

COMMUNITY
The Improvement of Health Care in Afghanistan – June 2016
Since 2002, the improvement of health care in Afghanistan has been great. According to USAID, “9 percent of Afghans lived within a one-hour walk of a health facility.” Today, over 50 percent of the population has access to a health care facility, the infant and child mortality rates have decreased and maternal mortality rates have declined as well.
The country’s turbulent history, filled with war and internal strife, has contributed a deteriorated health care system. The old Taliban regime stifled access to adequate medical facilities and professionals. With the help of groups like UNICEF, WHO and USAID the Afghan people are seeing tremendous progress within their country.
On May 16, 2016, a campaign to vaccinate every child under five years of age for polio was launched.
Afghanistan and Pakistan are the only two countries still struggling against the illness. According to WHO, the campaign could put an end to the disease in the next few months.
This is just one example of the efforts being made to improve health care in Afghanistan. U.S. support in the country has also led to success in fighting tuberculosis. Data from 2012 reports daily TB treatments to have a 91 percent success rate.
Women’s health has improved immensely over the last decade. With the help of the U.S. government, more trained midwives were available in Afghanistan. As a result, by 2010, 60 percent of women had care prior to birth. This is an enormous step forward from 2002 when only 16 percent had this same access.
Despite its progress, the country still has a long journey ahead in improving the health care system. According to the Thomas Reuters Foundation, nearly 1.2 million Afghans have been internally displaced.
These individuals have little to no access to healthcare, which is a major problem as they also struggle for food and clean water. Violence against medical facilities has not helped the issue either. In 2015, 42 people were killed in a Doctors Without Borders hospital in Kunduz.
Increased foreign aid and peace efforts are necessary to solve the health care crisis in Afghanistan. This will involve supporting organizations already involved in the country as well as increased pressure on foreign governments for humanitarian action.
– Saroja Koneru
SOURCE: https://borgenproject.org/the-improvement-of-health-care-in-afghanistan/

Bringing health care to Afghanistan’s vulnerable women

Published on Mar 12, 2014
YOUTUBE -CLICK ON PHOTO/VIDEO ABOVE-
Improving women’s access to medical care is helping reverse troubling trends in Afghanistan, one of the world’s most dangerous places to bear children.

The high price of premature births
Caitlin Mullen, Bizwomen contributor -Nov 6, 2018 bizwomen – The Business Journals
A March of Dimes report card shows the preterm birth rate has worsened from the previous year in 30 states.
As the country’s preterm birth rate rises again, health professionals and organizations say they’re taking steps to address issues like inequitable access to prenatal care.
The March of Dimes premature birth report card notes the rate of premature births rose to 9.9 percent in 2017 in the U.S, up from 9.8 percent in 2016. In looking at all 50 states, the District of Columbia and Puerto Rico, the maternal and infant health nonprofit reports the rate has risen for the third year in a row.
“Premature birth and its complications are the largest contributors to infant death in this country and globally,” per the report card. November is Prematurity Awareness
Earlier this year, Johns Hopkins University researchers reported that American babies are 76 percent more likely to die before turning one than babies in other wealthy countries like Canada, France or Japan, per Vox.
March of Dimes reports high stress levels can cause a baby to be born premature — earlier than 37 weeks — or a baby that weighs less than 5.5 pounds, and those born too small or too soon face greater risk for other health problems. An American Academy of Pediatrics study has found children born prematurely face higher risk of hospitalizations, doctor visits, and societal costs down the road.
Reasons for preterm birth can vary, but March of Dimes points to inequities in quality health care across the country; rates are higher in poverty-stricken communities.
Race, too, plays a part from the womb. Women of color are 50 percent more likely to deliver a preterm baby, and babies of color experience a 130 percent higher death rate than white infants, the report states.
In the past few years, racial disparities have worsened, NPR reports. Chronic stress from racism may be to blame: research has shown it’s connected to a greater risk of preterm birth among black women.
Giving birth prematurely brings greater risks for moms, too. Mothers of babies born prematurely experience a high rate of postpartum depression, and researchers now recognize the experience associated with having a baby receive care in a NICU can lead to post-traumatic stress disorder, per The Atlantic.
“The experience of the neonatal intensive-care unit, the birth of a premature baby — it’s a very different kind of trauma from what we call single-incident trauma, like someone in a car accident or even a sexual assault,” Dr. Richard J. Shaw, psychiatry and pediatrics professor at Stanford University’s Lucile Salter Packard Children’s Hospital, told The Atlantic.
The monetary cost of preterm birth is another blow. One study found preterm births cost employer-sponsored health insurance plans $6 billion. Even after insurance coverage kicks in, parents might be on the hook for hundreds of thousands of dollars.
The March of Dimes report card showed the preterm birth rate had worsened from the previous year in 30 states. Mississippi and Louisiana were the states with the highest rates, at 13.6 percent and 12.7 percent. Vermont, with a rate of 7.5 percent, was the only state to receive an A grade.
Among the country’s cities with the highest number of births, Irvine, Calif., had the lowest rate — 5.5 percent — while Detroit had the highest, at 14.5 percent.
But progress was made in some states, with efforts like greater collaboration among March of Dimes, state officials and health care providers in Rhode Island; addressing issues like smoking and early elective deliveries in Raleigh, N.C.; and tailored programs like group prenatal care in Knox County, Tenn. Each location saw its preterm birth rate drop.
Group prenatal care may be making a difference in South Carolina, too. Per Vox, infant deaths there have dropped 28 percent since 2005, and experiments like Dr. Amy Crockett’s — holding large group appointments where women receive prenatal care — could be a contributing factor.
Women who’ve gone through these appointments are less likely to have premature babies, Vox reports, and appreciated that the group appointments offered a bit of community with women in the same situation.
“South Carolina has absolutely been at the forefront, from a state perspective. I think they do serve as a model for what can be done nationwide,” Jessica Lewis, Yale University infant health researcher, told Vox.
HEALTH CARE PARTNERS
The availability, well-being, safety and development of our Neonatal Womb/Preterm Birth Community healthcare partners must be a community priority. Our access to healthcare is critical to the health and vitality of our community.

Violence against health workers
Health workers are at high risk of violence all over the world. Between 8% and 38% of health workers suffer physical violence at some point in their careers. Many more are threatened or exposed to verbal aggression. Most violence is perpetrated by patients and visitors. Also in disaster and conflict situations, health workers may become the targets of collective or political violence. Categories of health workers most at risk include nurses and other staff directly involved in patient care, emergency room staff and paramedics.
WHO, ILO, ICN and PSI jointly developed Framework guidelines for addressing workplace violence in the health sector to support the development of violence prevention policies in non-emergency settings, as well as a questionnaire and study protocol to research the magnitude and consequences of violence in such settings. For emergency settings, WHO has also developed methods to systematically collect data on attacks on health facilities, health workers and patients.
SOURCE: https://www.who.int/violence_injury_prevention/violence/workplace/en/
Attacks on Health Care in Afghanistan: January 2018 – October 2018
We are sharing this article/data to represent an example of healthcare targets of collective or political violence. Violence and lack of healthcare access significantly traumatizes our neonatal womb/preterm birth community globally, increasing preterm birth rates and infant and maternal mortality.
Map from World Health Organization, US Agency for International Development, Health Cluster Published on 20 Oct 2018

SOURCE: https://reliefweb.int/map/afghanistan/attacks-health-care-afghanistan-january-2018-october-2018

Taking steps to prevent violence in health care workplace
We are sharing this article as an example of healthcare targets perpetrated by patients and visitors.
06/14/16  Amy Farouk
Amy Farouk
A new report by the AMA Council on Science and Public Health responds to increasingly common violence directed at physicians and other health care professionals where they work, looking at the trends in violence, solutions that have been tested and barriers to addressing the problem. The AMA adopted policy to help prevent violent acts in the health care setting.
An unacceptable hazard of the job
The U.S. Bureau of Labor Statistics reports that workplace assaults from 2011 to 2013 were 23,540-25,630 annually, with upwards of 70 percent occurring in health care and social service settings. Health care workers are three to four times more likely than other private sector employees to sustain injuries that involve days of work missed.
“Emergency department, mental health and long-term care providers are among the most frequent victims of patient and visitor attacks,” the report said. “A nationwide survey of emergency medicine residents and attending physicians found that 78 percent of respondents had reported at least on workplace violence act in the previous year, and 21 percent had reported more than one type of violent act.”
Addressing violence: Barriers and steps
One of the biggest obstacles to fully understanding the scope of the problem and taking corrective action is the fact that many incidents go unreported. “Reasons for not reporting can be as simple as health care workers not knowing what constitutes an act of workplace violence or a reporting process that is too cumbersome and time consuming,” the report said. “Other reasons for not reporting include a perception that workplace violence is ‘normal’ or a part of the job, fearing the response they may receive when reporting these events (blaming the victim), and lacking support from leadership to encourage reporting.” Some hospitals and health systems are taking steps to prevent violence, according to the report. They range from more traditional facility safety to more clinical approaches. Henry Ford Hospital in Detroit, for instance, has installed metal detectors at its entrances to prevent people from bringing weapons into the buildings. In the first six months of screening, the hospital confiscated 33 handguns, 1,324 knives and 97 chemical sprays.
The Veterans Health Administration, meanwhile, flags patient records to help clinicians and others identify patients who may pose a threat to themselves or others. Patients are flagged in tiers, one for those who are high risk for violent or disruptive behavior based on a history of violence and credible threats, and another for patients with other high-risk factors, such as drug-seeking behavior, a history of wandering or spinal cord injuries.
Physicians call for enforced standards
Delegates at the 2016 AMA Annual Meeting adopted policy that calls on all parties to take an active approach to increase the safety of health care workers:
- New policy calls on the Occupational Safety and Health Administration to develop and enforce a standard addressing workplace violence prevention in health care and social service industries.
- The AMA will encourage Congress to provide additional funding to the National Institute for Occupational Safety and Health to further evaluate programs and policies to prevent violence against health care workers, and asks the National Institute for Occupational Safety and Health to adapt the content of their online continuing education course on workplace violence for nurses into a continuing medical education course for physicians.
- The AMA is urging all health care facilities to adopt policies to reduce all forms of workplace violence and abuse; develop reporting tools that are easy for workers to find and complete; make prevention training courses available; and include physicians in safety and health committees.
- Updated policy also encourages physicians to take an active role in their safety by participating in training to prevent and respond to workplace violence threats, report all incidents of workplace violence and promote a culture of safety within their places of work.
“As violent incidents continue to plague hospitals, emergency departments, residential care settings and treatment centers, we must do everything we can to protect the health and well-being of our health care workers,” AMA Board Member William E. Kobler, MD, said in a news release. “We urge the federal government to develop and enforce a federal standard for health care employers to help shield health care workers from workplace violence.”
Why Physicians Are More Burned Out Than Ever
 Elizabeth Métraux -Dec 7, 2018
Elizabeth Métraux -Dec 7, 2018
I sat knee to knee with a nurse practitioner at a school-based clinic in rural Ohio. Choking back tears, she described a patient she couldn’t get out of her head: a middle-school girl, accompanied by her mother and a social worker. Just days prior, the girl was dropped off at her father’s home for the weekend. Before the promised Friday night football game, she discovered him unconscious on the bathroom floor. Within the hour, paramedics were laying a sheet over his body. Another victim of an opioid overdose in a region of the country that has been devastated by the epidemic.
That was only part of the story.
As I spoke with the NP, she described the girl entering the exam room, listless and distant. Mom was shouting at the social worker and insisting it was a “good thing” the girl’s father was “finally” out of the picture. Her daughter would get over it, she said.
The NP noticed the girl furiously scratching the back of her head. She lifted the girl’s hair to examine her scalp.
Lice. Hundreds of nits covered the girl’s head, with spots rubbed raw and scabbed over. She had likely had them for weeks, maybe longer. The girl looked down at her feet in shame. Her mother, picking up on the encounter, eyed her daughter with disgust.
“And just like that,” the NP said, “the mother left. She just left. She couldn’t stand to look at her own daughter.” She began to cry.
“How do you process that?” I asked.
What we’re witnessing isn’t a failure to thrive in America’s clinics; it’s a failure to act in America’s communities.
Through sobs, she said she doesn’t. It just stays with her. For herself and colleagues like her — soldiers in the trenches of our nation’s health care system — she says, “It hardens us all. It’s the poverty and the brokenness and the addiction and the inequity and the hate. But what can we do? The public won’t act, so we have to.”
Her story is no different than hundreds I’ve listened to over the course of the year — along the southern border, in community health centers, in prisons, on Native American reservations, in the hallways and exam rooms of some of the most esteemed academic medical centers in our country.
I listened to these stories as part of my work with Primary Care Progress, a national nonprofit working to strengthen primary care teams and clinicians. As I spoke with several health care providers about the realities of their work, I expected to hear the usual concerns: the rise of the electronic medical record, cumbersome administrative burdens, the frenetic pace and long hours. These pain points certainly came up.
What I didn’t expect to discover, however, was our own central role — my role as a patient and member of the public — in so much of their professional trauma. Burnout is a real issue, and we’re contributing to it.
It’s easy for those of us on the outside the burnout epidemic to wonder why professionals so skilled at healing seem unable to heal themselves. Indeed, who among us doesn’t feel overworked and undervalued?
But there’s something deeply disturbing about this growing crisis in medicine. What we’re witnessing isn’t a failure to thrive in America’s clinics; it’s a failure to act in America’s communities.
Take, for example, the brutal shooting in Thousand Oaks, California, this past November. In a hospital waiting room, a trauma surgeon changed her bloodied scrubs. She stood in front of a bathroom mirror to rehearse the name of a victim so she didn’t accidentally say the name of the one she worked on an hour earlier. Then, donning her starched white coat and well-trained detachment, she met with the family to notify them that their 22-year-old son was dead. Her team had done all they could. She was sorry. Later that day, she mourned the deaths. Alone.
Days later, a row between the National Rifle Association and health care professionals ensued over the NRA’s remarks that doctors should “stay in their lane” when it comes to gun violence. Providers hit back with a powerful, viral social media campaign to draw attention to their critical role in treating victims of gun violence.
While the NRA and clinicians nationwide debated the issue, an important point was missing from the dialogue: Gun violence shouldn’t have to be physicians’ responsibility; preventing it should be in the public’s responsibility.
Yet there are countless ways in which we — the public — abdicate that responsibility, instead putting the onus on clinicians to treat victims of our hate, our neglect, and our bigotry. Community health workers offer care in homeless encampments and outpatient drug treatment facilities nationwide. Nurses treat thousands of children in detention facilities on America’s southern border. Health care providers work with millions of incarcerated men and women in our country’s overcrowded prisons.
At a recent visit to a community health center in suburban Seattle, I asked a group of doctors to share the best part of their week. One clinician noted that after days of negotiating with a local power company, she was able to get her patient’s electricity turned back on. “It was important,” she said, “because she’s on medication that requires refrigeration.” Another glowed when talking about the clinic’s new food pantry that had opened to serve its food-insecure patients.
All that is laudable — and an absolute travesty. It’s a sobering testament to the fact that America is content to neglect social and structural determinants of health.
William Osler famously remarked, “Listen to your patients; they’re telling you their diagnosis.” We also need to listen to our clinicians. Story by story, they’re telling us that our nation is in crisis.
Those of us who aren’t in clinics or emergency rooms every day can look away when we see injustice. Health care professionals don’t have that luxury. While they’re checking their clothes to make sure there’s no visible blood before they break the news to a family, the rest of us listen to so-called experts tell us it’s “too soon” to address gun reform in the wake of another mass shooting. While an oncologist tries to figure out how to treat a mother’s cancer when she can’t afford her medications, policymakers explain why it would be imprudent to tackle health care coverage or rising prescription costs.
Our health care providers don’t get to turn a blind eye to symptoms of America’s divisions and inactions. They also don’t get to decide who deserves treatment. The victim or the shooter. The immigrant or native born. The nationalist or the progressive. For clinicians, they’re all patients. But health care professionals do suffer the consequences of inaction.
William Osler famously remarked, “Listen to your patients; they’re telling you their diagnosis.” We lso need to listen to our clinicians. Story by story, they’re telling us that our nation is in crisis. Too many people are dying too unnecessarily from too many treatable conditions by too many factors that we can control.
Sure, no one likes the electronic medical record. But that’s not at the heart of burnout. Inaction is driving our collective burnout — not just in health care, but in all care. Again and again, providers across the country are put in a position of saying, “We did all we could.”
They may have done all they could, but the rest of us haven’t.
Why should the public care about the well-being of a well-heeled workforce? Because when the problem is on us, so is the solution. Instead of asking physicians if they’re burned out, let’s start asking: Did we do all we could to heal our nation? Maybe then we can be a part of healing the healers.
A special thanks to Dr. Krisda Chaiyachati for your important contribution to this piece.

Reducing Health Care Burnout: Preventive Tips for Organizations & Caregivers
Working in the healthcare industry can be both gratifying and challenging. The unrelenting chronic stress of being exposed to life and death issues, long hours and loads of work can progressively evolve into burnout. If fact, the odds are pretty high that burnout will affect every healthcare professional at some point in their career. Burnout is defined as the consequence of mental and physical exhaustion that is caused by stress resulting in depersonalization and a profound decrease in personal accomplishment.
Working in this high-stress industry can become emotionally draining, especially when hospitals are understaffed; the caregiver can begin to experience emotional exhaustion, and fatigue. All of this can lead caregivers to an emotional detachment from their work and to begin to see patients as objects, thereby reducing the safety and quality of care provided.
According to a study by NSI Nursing Solutions, the average national turnover rate among all hospital healthcare workers is 16.5%. And the costs are high:
- Each additional percentage point increase in turnover can cost the average hospital another $359,650
- It takes hospitals between 36 to 97 days to hire a replacement for an experienced RN
- The average cost of turnover for a bedside RN ranges between $44,380 and $63,400To prevent burnout, employers should create a culture that sustains resilience and supports employee wellbeing. It’s important to take the time to identify the signs and symptoms of burnout, some of which may include:
- Chronic emotional and physical fatigue
- Reduced feelings of sympathy or empathy
- Poor work-life balance
- Depersonalization
- Hypersensitivity or complete insensitivity to emotional material
- Withdrawal from friends, family, and other loved ones
- Loss of interest in activities previously enjoyed
- Feeling blue, irritable, hopeless, and helpless
- Changes in sleep patterns
- Getting sick more often
- Irritability3,4
How Organizations Can Prevent Burnout
As a healthcare employer, there are things your organization can do to help your providers stay healthy and succeed:
Take an active role: Know your employees’ concerns – Provide a forum for feedback and address problems before they get to a unrecoverable level.
Encourage breaks: Taking breaks helps employees walk away from stress ensuring that the staff is not overworking themselves to the point of burnout.
- Support healthy habits: Implementing health and wellness programs can be invaluable and they don’t have to cost a lot money to be effective. Include healthy recipes in your newsletters, sponsor workout classes, create a relaxation room, or offer meditation classes.5
How Caregivers Can Prevent Burnout
As a caregiver, adopting healthy behaviors can prevent compassion fatigue and burnout:
Take Time to Care for Yourself
Practicing good self-care will significantly help your resilience and reduce your vulnerability to stress.
- Balanced, healthy diet
- Regular exercise
- Routine schedule of restful sleep
- Balance between work and personal life
- Drink alcohol in moderation
Adopt Positive Coping Strategies
Positive coping strategies can be used at work or at home to help ease your response to stressful situations.
- Deep breathing
- Meditation
- Taking a walk
- Talking with a friend
- Relaxing in a hot bath
If you still feel that you are not getting enough out of mindful techniques, and are still feeling emotionally vulnerable, chronically stressed and overwhelmed, seek help. Seeing a therapist can help you process your feelings and put things in better perspective, which can help you successfully implement the strategic techniques that will help you move toward a healthy work-life balance.

PREEMIE FAMILY PARTNERS
Omega-3 Fatty Acids May Reduce Risk of Premature Birth
11/17/18 – By Traci Pedersen
Expectant women who increase their intake of omega-3 long-chain polyunsaturated fatty acids can reduce the risk of premature birth, according to a new study published in the Cochrane Review.
“We know premature birth is a critical global health issue, with an estimated 15 million babies born too early each year,” said Associate Professor Philippa Middleton from Cochrane Pregnancy and Childbirth and the South Australian Health and Medical Research Institute (SAHMRI).
“While the length of most pregnancies is between 38 and 42 weeks, premature babies are those born before the 37-week mark — and the earlier a baby is born, the greater the risk of death or poor health.”
Infants born prematurely are at greater risk of a range of long-term conditions including visual impairment, developmental delay and learning difficulties.
Middleton and a team of Cochrane researchers have been looking closely at long-chain omega-3 fats and their role in reducing the risk of premature births; particularly docosahexaenoic acid (DHA) and eicosapentaenoic acid (EPA) found in fatty fish and fish oil supplements.
For the study, they reviewed 70 randomized trials and found that for pregnant women, increasing the daily intake of long-chain omega-3s:
- lowers the risk of having a premature baby (less than 37 weeks) by 11 percent (from 134 per 1,000 to 119 per 1,000 births);
- reduces the risk of having an early premature baby (less than 34 weeks) by 42 percent (from 46 per 1,000 to 27 per 1,000 births);
- lowers the risk of having a small baby (less than 5.5 pounds or 2,500g) by 10 percent.
“There are not many options for preventing premature birth, so these new findings are very important for pregnant women, babies and the health professionals who care for them,” Middleton says.
“We don’t yet fully understand the causes of premature labor, so predicting and preventing early birth has always been a challenge. This is one of the reasons omega-3 supplementation in pregnancy is of such great interest to researchers around the world.”
This review was first undertaken back in 2006. At that time, the researchers had concluded there wasn’t enough evidence to support the routine use of omega-3 fatty acid supplements during pregnancy. Over a decade later, however, this updated review concludes that there’s high quality evidence for omega-3 supplementation to be used as an effective strategy for preventing preterm birth.
“Many pregnant women in the UK are already taking omega-3 supplements by personal choice rather than as a result of advice from health professionals,” Middleton said.
“It’s worth noting though that many supplements currently on the market don’t contain the optimal dose or type of omega-3 for preventing premature birth. Our review found the optimum dose was a daily supplement containing between 500 and 1000 milligrams (mg) of long-chain omega-3 fats (containing at least 500mg of DHA) starting at 12 weeks of pregnancy.
“Ultimately, we hope this review will make a real contribution to the evidence base we need to reduce premature births, which continue to be one of the most pressing and intractable maternal and child health problems in every country around the world.”

GAPPS – SUPPORTING PARENTS GRIEVING A LOSS
At GAPPS, we want to recognize parents whose lives have been impacted by losing a baby to stillbirth or caring for a premature baby. Preterm birth and stillbirth impact the lives of parents, families, and infants all over the world, regardless of geography or socioeconomic status, and it is our goal to better understand the causes of preterm birth and stillbirth and ways to prevent them. This work is dedicated to parents dealing with the loss of a baby through stillbirth, and to those struggling to care for premature infants.
We recognize the profound pain and loneliness of grieving parents and extend our sincerest sympathy. There are many organizations available to help parents navigate loss, connect with others and move forward with their lives, as well as support for parents of premature babies. Explore these resources for more information.
Below are some additional links to organizations with information that may be useful for those caring for preterm newborns or dealing with the loss of a baby.
First Candle
First Candle is one of the nation’s leading nonprofit organizations dedicated to safe pregnancies and the survival of babies through the first years of life. Their current priority is to eliminate stillbirth, Sudden Infant Death Syndrome and other Sudden Unexpected Infant Deaths through research, education, and advocacy programs.
International Stillbirth Alliance
The International Stillbirth Alliance is a nonprofit coalition of organizations dedicated to understanding the causes of and working on the prevention of stillbirth. Their mission is to raise stillbirth awareness, promote global collaboration in the prevention of stillbirth, and to provide appropriate care for parents who have lost a baby to stillbirth.
SANDS: Stillbirth & Neonatal Death Society (UK)
SANDS supports anyone affected by the death of a baby, works in partnership with health professionals to improve the quality of care and services offered to bereaved families, and promotes research and changes in practice that could help to reduce the loss of babies’ lives.
The Tears Foundation
The TEARS Foundation is a non-profit organization that seeks to compassionately assist bereaved parents with the financial expenses they face in making final arrangements for their baby who has died.
March of Dimes
March of Dimes helps moms have full-term pregnancies and focuses on researching problems that threaten babies’ health.
Hayden’s Helping Hands
Hayden’s Helping Hands is a non-profit foundation that assists Oregon and Washington families after the birth of a stillborn baby by paying for a portion or all of their hospital delivery medical expenses.
SOURCE: https://www.gapps.org/Home/ParentSupport
INNOVATIONS

Psychologist Sue Makarchuk with Alberta Health Services interacts with Anna Strachan, 2, who needed a dose of caffeine as a preemie to help her breathe. Photos by Riley Brandt, University of Calgary
New study shows premature babies’ developing brains benefit from caffeine therapy
December 12, 2018 – By Pauline Zulueta, Cumming School of Medicine
UCalgary’s Abhay Lodha shows early caffeine treatment of premature babies born less than 29 weeks’ gestation has no long-term negative effects on brain development. Calgary mom Avril Strachan says she’s pleased to learn the results of the study as her daughter, Anna, was treated with caffeine.
For many, starting the day off with caffeine from a cup of coffee is a must. In neonatal intensive care units, or NICUs, premature babies born under 29 weeks are given a daily dose of caffeine to ensure the best possible start to life. A new study by University of Calgary researchers shows the earlier the dose of caffeine can be given, the better.
“Caffeine is the most commonly used drug in the NICU after antibiotics,” says Dr. Abhay Lodha, MD, associate professor in the departments of paediatrics and community health sciences at the Cumming School of Medicine and staff neonatologist with Alberta Health Services (AHS). “It’s important that we understand the long-term effects of caffeine as a treatment and ensure these babies are not only surviving, but have quality of life down the road.”
Born prematurely at 27 weeks at the Foothills Medical Centre, Kyle and Avril Strachan’s baby, Anna, was given caffeine to help her breathe and to boost lung function.
“The doctors told us, with premature babies, their brain hasn’t developed quite enough to let them do all the things their bodies should be doing on its own, like breathing,” says mom Avril. “In the first few weeks, when Anna was feeding, she would slow down or even forget to breathe. This would cause her heart to slow and for her to not get enough oxygen.”
To help her breathe more easily, Anna needed a continuous positive airway pressure, or CPAP, machine to deliver constant airflow to her lungs.
A 2014 study by Lodha showed starting caffeine therapy within two days after birth shortened the amount of time babies needed to use ventilators. It also reduced the risk of bronchopulmonary dysplasia (BPD), a form of chronic lung disease caused by damage to the lungs from use of a ventilator. What was not known was how that dose of caffeine affected brain development.
Lodha collaborated with researchers from the Universities of British Columbia, Montreal, Toronto and Mount Sinai Hospital in Toronto to analyze data from 26 NICUs across Canada. They found early caffeine treatment has no long-term negative effects on neurodevelopment, and is actually associated with better cognitive scores, and reduced odds of cerebral palsy and hearing impairment. The findings are published in Pediatrics.
The team examined data from followup assessments conducted at age 18 to 24 months. During these followups, children were assessed for their cognitive, language and motor development using the Bayley Scales of Infant and Toddler Development, a standardized scoring system to assess developmental functioning in infants and toddlers.
“We look at how children are constructing their understanding, such as solving simple problems or figuring out three-dimensional objects and toys,” says Dr. Dianne Creighton, PhD, research assistant professor in the Department of Paediatrics and retired psychologist with AHS. “We also assess how the little ones are able to understand simple words, or recognize the name of a picture, as well as their motor skills like climbing, crawling, balance and co-ordination.”
Lodha says it’s believed that caffeine may increase the growth of dendrites, the small branches of a neuron that receive signals from other neurons. “Caffeine may also improve better lung stretch and expansion, cardiac output and blood pressure in premature infants, which improves oxygen supply throughout the body and brain, reducing the duration of mechanical ventilation and the risk of chronic lung disease and injury on the developing brain.”
Now two years old, Anna has completed multiple followup assessments and is participating in dance classes, gymnastics lessons and swimming like a fish, says her mom.
“She’s very mechanical. She likes to build things, take it apart and figure out how it works,” Avril says. “It’s wonderful to know that the caffeine treatment has no adverse effects and that if researchers are getting positive findings, it should continue to be the standard of care for premature babies. In that case, I think parents would have no hesitation in having caffeine as part of their child’s treatment.”
This study was conducted with data from the Canadian Neonatal Network and the Canadian Neonatal Follow-up Network, which is supported by the Maternal-Infant Care Research Centre at Mount Sinai Hospital. Abhay Lodha and Dianne Creighton are associate members of the Alberta Children’s Hospital Research Institute.
WARRIORS:

As the New Year approaches and we create our lives with vitality and curiosity one of the most important things we can choose to do daily is to connect with Source and engage in peaceful connections within and throughout. May Peace be with us as we journey.

YOUTUBE -CLICK ON PHOTO/VIDEO ABOVE-
GUIDED MEDITATION: 4 MINUTE STRESS BUSTER –
The Honest Guys – Meditations – Relaxation
Afghani Pro Surfer Afridun Amu

Afridun Amu was the first Afghan athlete to internationally represent Afghanistan in surfing. He participated in the International Surfing Association World Surfing Games in Biarritz, France in May 2017. Amu also won the first official Afghan surfing championship (men) in 2015 in Ericeira, Portugal. He is the reigning Afghan surf champion.
Amu was born in Kabul, Afghanistan on June 23, 1987. He spent his childhood in Moscow, Russia, where his father worked as a diplomate. His family moved to Germany as political refugees in 1992. He graduated in law, cultural science and design thinking. He works as an expert in Constitutional law at the Max Planck Foundation for International Peace and the Rule of Law and is a lecturer on Design thinking at the Hasso Plattner Institute.
YOUTUBE -CLICK ON PHOTO/VIDEO ABOVE-
Published on May 23, 2017
At 29, surfer Afridun Amu is thrilled to be participating in his sport’s world championships in Biarritz, and even more so to be representing his native country: land-locked Afghanistan. A political refugee, Amu grew up in Germany, and hopes his performance this week might help people to see his country differently.



























 Published: September 14, 2017
Published: September 14, 2017




























 TEDx Talks
TEDx Talks



















 Neonatal Research Institute at Sharp Mary Birch Hospital for Women & Newborns
Neonatal Research Institute at Sharp Mary Birch Hospital for Women & Newborns 
 How do we help preterm birth partners in countries at war? Human Security, physician/health care provider access and simple, effective, portable resources are things to consider.
How do we help preterm birth partners in countries at war? Human Security, physician/health care provider access and simple, effective, portable resources are things to consider.










 … Oh, Panama…………
… Oh, Panama…………





 Remarkable Improvements in Maternal and Child Health Care in
Remarkable Improvements in Maternal and Child Health Care in 


 Autism spectrum disorder and prematurity: towards a prospective screening program.
Autism spectrum disorder and prematurity: towards a prospective screening program. Success of
Success of 




 , another opens
, another opens 



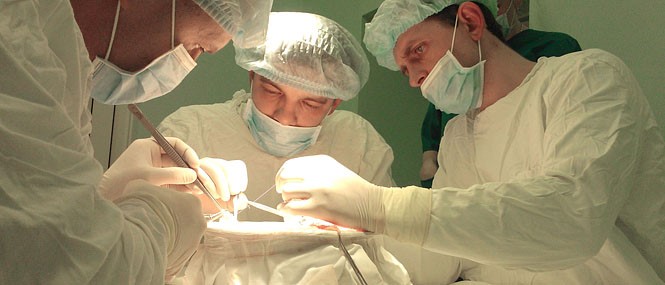 A kidney transplant surgery is performed at the Grodno Oblast Clinical Hospital
A kidney transplant surgery is performed at the Grodno Oblast Clinical Hospital




 Kat and I were pleased to read a copy of a recent letter sent by APHA to Washington DC encouraging support of federal research and promoting known interventions and community initiatives related to preterm birth.
Kat and I were pleased to read a copy of a recent letter sent by APHA to Washington DC encouraging support of federal research and promoting known interventions and community initiatives related to preterm birth.
























 Premature birth test being trialed
Premature birth test being trialed






 BRASIL
BRASIL








 By Robert Preidt, HealthDay Reporter
By Robert Preidt, HealthDay Reporter

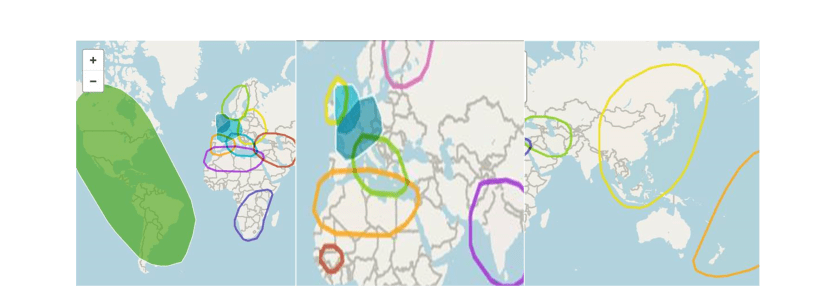 Genealogy of my maternal and paternal strands is pictured above. My brother Seth, sister Ciara and I took our DNA tests and found out our genetic make up is as shown in the photos above. Ethnically we are Western and Eastern European, Scandinavian, North African Berber, Senegalese/Central African, South African, Middle Eastern, South and East Asian, Latin, Indigenous to the Americas, and Polynesian.
Genealogy of my maternal and paternal strands is pictured above. My brother Seth, sister Ciara and I took our DNA tests and found out our genetic make up is as shown in the photos above. Ethnically we are Western and Eastern European, Scandinavian, North African Berber, Senegalese/Central African, South African, Middle Eastern, South and East Asian, Latin, Indigenous to the Americas, and Polynesian.































