 Join us in England where strategic long term preemie research continues to explore and empower our Global Neonatal Womb community. Enjoy Kat’s journey back into the NICU, and watch a film that takes us through a chilling yet thought-provoking immersion into the NICU infant experience.
Join us in England where strategic long term preemie research continues to explore and empower our Global Neonatal Womb community. Enjoy Kat’s journey back into the NICU, and watch a film that takes us through a chilling yet thought-provoking immersion into the NICU infant experience.
ENGLAND

7.0% (48,490) of live births were low birthweight
Rate: 7.8% Rank: 134 (United Kingdom)
Source: https://www.marchofdimes.org/mission/global-preterm.aspx#tabs-3
England: Birth place of preemies Winston Churchill and Sir Isaac Newton, The Beatles and The Queen ![]()
COMMUNITY
Epicure is a fascinating endeavor that continues to improve our understanding of the preterm birth experience and a great contributor towards the development of wellness resources for all of our community members!
Epicure creates population based studies of survival and later health status in extremely premature infants. EPICure (UK, Ireland) is a series of studies of survival and later health among babies and young people who were born at extremely low gestations – from 22 to 26 weeks. The first study was published in 1995.
Publications page: http://www.epicure.ac.uk/publications/publications-by-year/
Meet the team : The biggest contributors to the EPICure study are the paediatricians and neonatal nurses from all the maternity units in the UK and Ireland who contributed to the original data collection and made the whole thing possible and of course the parents and children who have taken part in the childhood studies, giving freely of their time, to help us collect this important information.
Premature Babies – a Success Story
One of the success stories in modern medicine has been the increasing survival of very premature babies. Over the past decade survival has improved dramatically for babies born at 26 weeks of gestation and above so that now over 80% survive. Normal pregnancy lasts 40 weeks, but babies may survive from as early as 22 weeks, although at these extremely low gestations (22-24 weeks) most babies are born too immature to survive. As with all advances in care, there is a cost in terms of disability suffered by some children among those that survive. This is the whole point of EPICure, as it allows us to quantify the outcomes and shows us where we need to target our care. For parents faced with the prospect of delivering a child before 26 weeks gestation, there has been little information available which describes outcomes from large numbers of children. Thus, until we carried out the first study it had been difficult to give parents accurate information regarding the chances of survival and the possibility of disability or other long term problems amongst survivors. Because care improves, and more babies survive, we hope outcomes also improve but we need to show this as well – hence EPICure2.
Why do we need to study extreme prematurity?
We know that disability increases as gestation at birth gets shorter. Births (and surviving children) at gestations below 27 weeks are relatively uncommon – being less than 1% of all births. Babies born this early need to stay in neonatal units for a long time and their care is very intense and costly. Because the number of extremely premature babies born is so small we need large studies to be accurate in describing their outcomes. The decision to admit a preterm baby for intensive care is made by doctors after discussion with the parents but until 2000 there were no national guidelines or data on which to build them. Data from EPICure have informed important national initiatives such as the report from the Nuffield Council on Bioethics describing many of the issues surrounding decision making in the period around birth (www.nuffieldbioethics.org). Some of these new guidelines have been based on the results of the EPICure studies (www.bapm-london.org/publications).The attitude of individual neonatologists and obstetricians may influence the management of different babies. The information on which that management is based needs to be impartial as possible as, on the basis of such decisions, treatments that are thought to be effective may be withheld. Clinicians, healthcare planners and parents need population based data relevant to modern intensive care practices for informed decision making. EPICure has given them this nationally based information, which can be used to help this process.
What are we up to now?
We have several major EPICure projects on the go at present:
Analysis of EPICure2 data – here we are studying the effects that the organisation of neonatal care has on outcomes – size of neonatal services that babies are born in, their staffing and the effects of transfers – all things important to parents and their babies. In this the premature babies charity Bliss are helping us. We have the data but need to reanalyse it in new ways.
EPICure@16 – in this project we are writing to all the 16 year olds and asking their permission to contact them personally in a few years to ask if they continue to help us with our studies as they are such an important group.
EPICure@19 – we are currently planning another assessment at 19 years and are currently applying for funding from the Medical Research Council to do this.
Parents and decisions – we are aware that the one area of the family we know little about is the effect that a birth so early has on the family and we are designing some new studies to start to tease out this important area.
SOURCE: http://www.epicure.ac.uk/

Experience this Docu-fiction feature that allows us to experience a preterm birth infant’s point of view.
MOVIE PREEMIE PERSPECTIVE:
SOURCE:http://sales.arte.tv/fiche/6377/LA_VIE_A_VENIR_360___VR____Dans_la_peau_d_un_premature
PREEMIE FAMILY PARTNERS

Perhaps the hardest lesson in life is the art of letting go; of control, expectations, patterns and predictability, and of having to know why and what is next. The preterm birth experience provides an opportunity to let go and love at levels we may never have anticipated we could choose. Resilience is strength. Flexibility and an open mind and heart promote growth and well-being. We have choices…
What Makes Us Resilient?
New research explores the psychology of resilience
Posted Apr 10, 2018
Resilience is all about being able to overcome the unexpected. Sustainability is about survival. The goal of resilience is to thrive. —Jamais Cascio
Mental health professionals working with trauma victims have long recognized that many people exposed to horrific experiences often seem able to cope successfully and even thrive afterward. Whether those experiences occur due to an abusive childhood, dealing with the traumatic aftermath of physical or sexual assault, or recovering from a disaster (man-made or natural), many survivors are still able to move on with the lives without developing the mental health problems often faced by others.
This ability to cope with adversity, often referred to as psychological resilience, has been examined in hundreds of research studies though we still have a limited understanding of what makes some people more resilient than others. Even identifying resilient people can be a problem since they often don’t develop the mental health problems that might otherwise bring them to the attention of health professionals. But is there more to resilience than simply not developing mental health problems? What about the people who are able to grow and flourish because of their ability to cope effectively with what they have experienced?
According to the resilience portfolio model proposed by John Grych of Marquette University, resilience has three primary components:
- Self-regulation, or the ability to control impulses, manage difficult emotions, and being able to carry on despite setbacks. As one example of this, research looking at children with a history of domestic violence has shown better outcomes in children depending on their capacity for emotional self-regulation. Self-regulation also seems related to personality factors such as perseverance or grit.
- Interpersonal relationships, particularly the supportive relationships that can come from family or friends. This also includes those qualities that help people maintain these relationships, even during times of personal crisis. Social support has long been recognized as an important protective factor for people dealing with traumatic life events or emotional distress. For people without this kind of support, loneliness can often contribute to the emotional aftermath of trauma and make recovery that much more difficult. Interpersonal support can also come from being part of a caring community.
- Meaning-making, or the ability to understand and to explain what someone is experiencing, no matter how traumatic. For people who are spiritual or religious, the meaning they find often reflects their beliefs about religion or a higher power but can also involve finding new purpose or hope as part of the process of recovery.
In the same way that a traumatic event is not going to affect everyone equally, people are going to differ in terms of the qualities that make them resilient. According to the resilience portfolio model, people need a range of different strengths to survive and prosper after adversity. Referred to by researchers as poly-strengths, it is the total number of different strengths in anyone’s resilience portfolio that makes survival possible. This is in contrast to “poly-victimizations” or the number of different adverse experiences a person might have which can make them increasingly vulnerable to psychological problems.
But what are the kind of poly-strengths that can protect against traumatic experiences? And why do similar traumas affect people in different ways? A new research study published in the journal Psychology of Violence explores these questions through a unique test of the resilience portfolio model.
A team of researchers led by Sherry Hamby of the Life Paths Appalachian Research Center in Monteagle, Tennessee recruited 2565 participants from the Appalachian region of three U.S. states to take part in the study. The participants had an average age of 30 (65.3 percent female) and included adolescents aged twelve or older. They were recruited through mass advertising and at local community events such as country fairs. This allowed the researchers to bring in people who might not ordinarily participate in psychological studies. Along with providing demographic information, all participants completed questionnaires asking about their history of adversity, their individual strengths as reflected by the resilience portfolio model, their current psychological functioning, and how effectively they were able to cope with their experiences. Posttraumatic growth, mental health, and psychological endurance were measured using standardized inventories.
Given that the participants were recruited from one of the most poverty-stricken areas of the country, it’s hardly surprising that over 98 percent of the participants in the study reported at least one form of adversity. This included physical intimidation or abuse, exposure to family violence or emotional abuse, neglect, or bullying. Other stressful events that were reported included unemployment, poverty, natural disasters, or the death of a family member. Many participants reported multiple traumatic experiences in their lives. Despite this history of adversity, however, most participants endorsed items such as “I discovered that I am stronger than I thought I was” and “I changed my priorities about what is important in life.” Less than half of the participants in the sample reported mental health problems resulting from what they experienced.
Overall, individuals reporting a strong sense of purpose reported greater subjective well-being, posttraumatic growth, and fewer mental health symptoms. Other protective factors that contributed to positive outcomes included optimism, emotional regulation and awareness, and psychological endurance. As the resilience portfolio model predicted, the more of these individual protective factors an individual had, the more successful they were at coping with adversity. This suggests that it is the total number of poly-strengths that is important in resilience rather than individual factors alone.
So, what can be learned from this research? Even though more research is needed, these results do highlight the importance of a strengths-based approach in helping people recover from trauma and learn to move on with their lives. While there are already treatment programs aimed at helping trauma victims, they are usually aimed at people already dealing with posttraumatic symptoms rather than helping people become more resilient. Programs teaching conflict negotiation and emotional learning are also available though they tend to ignore other sources of strength such as optimism or meaning-making.
Unfortunately, for most people, the only way to build up resilience is to experience trauma and loss for themselves. To quote Elizabeth Hardwicke, “Adversity is a great teacher, but this teacher makes us pay dearly for its instruction; and often the profit we derive, is not worth the price we paid.” While it might be possible someday to develop programs that can teach the different strengths which promote resilience, we don’t seem to be there yet.
Still, the lessons learned from people able to grow and prosper following trauma may provide vital clues that can help others do the same.
SOURCE: https://www.psychologytoday.com/us/blog/media-spotlight/201804/what-makes-us-resilient

Ted Talk
Psychologist Susan David shares how the way we deal with our emotions shapes everything that matters: our actions, careers, relationships, health and happiness. In this deeply moving, humorous and potentially life-changing talk, she challenges a culture that prizes positivity over emotional truth and discusses the powerful strategies of emotional agility. A talk to share.
Susan David, a Harvard Medical School psychologist, studies emotional agility: the psychology of how we can use emotion to bring forward our best selves in all aspects of how we love, live, parent and lead.
SOURCE:https://www.ted.com/talks/susan_david_the_gift_and_power_of_emotional_courage
INNOVATIONS
Interesting ventilator options from the UK and Tasmania, and the development of blood testing to predict preterm births follow…
Infant news – Draeger launches VentStar Helix heated hose system for high frequency ventilation

May 18, 2018 – The VentStar Helix heated hose system for high frequency ventilation.
The VentStar Helix heated (N) plus has been specifically developed for high frequency ventilation and for interaction with ventilators that have a high frequency ventilation function.It uses hoses that only expand slightly so that the ventilation pressure in the system is maintained, and small volumes of breathing gas can pass through the ventilation hose to the patient.A helical heating wire, which winds around the hose system as a double-helix, is designed to evenly heat the breathing gas from the outside. This means that the inside of the hose is free of heating wires, which allows the breathing gas to flow through the hose into the neonatal patient’s airway with low resistance.
SOURCE:http://www.infantjournal.co.uk/news_detail.html?id=289

Infant news – SLE and the University of Tasmania announce license of technology designed to reduce infant mortality
The OxyGenie technology will be incorporated into the SLE6000 ventilator
March 20, 2018
SLE Ltd and the University of Tasmania have announced that they have concluded a commercial licence that will see SLE begin incorporating the university’s patented algorithm (using a closed-loop control for optimised oxygen concentration in the blood circulation of infants) into the SLE6000 neonatal ventilator.
Branded OxyGenie, the technology has been developed over the last nine years by a team of scientists led by Professor Peter Dargaville of the Tasmanian Health Service and Dr Tim Gale of the School of Engineering and ICT at the University of Tasmania and is now being integrated into the SLE6000 in collaboration with the SLE engineering department.
Past multi-centre studies have shown that vulnerable infants are very susceptible to changes in the oxygen in their circulation. Maintenance of this blood oxygen in a narrow but critical band may reduce mortality, retinal damage and other long-term effects. OxyGenie technology, which is currently only licensed to SLE, will keep infants within the target range without the intervention of clinical staff.
Findings of a clinical study of the algorithm that reinforce its capacity to control oxygen delivery in tiny preterm infants under challenging clinical conditions will be presented at the Society for Paediatric Research meeting in Toronto in May this year.
SOURCE: http://www.infantjournal.co.uk/news_detail.html?id=272
 Premature birth test being trialed
Premature birth test being trialed
08Jun18 – BBC News
Scientists are trialling a blood test that may predict whether a pregnant woman will give birth prematurely.
Preliminary results, published in the journal Science, suggest it is accurate in up to 80% of high-risk women.
The team, at Stanford University, in the US, say it is also as accurate as ultra-sound scans at predicting due dates.
However, there is still far more work to do before it could be used clinically.
- Every year 15 million babies are born too early (before 37 weeks gestation) around the world
- Preterm birth is linked to a million deaths a year
- It is the leading cause of deaths among children under the age of five
The test measures the activity of genetic material, called RNA, coming from the foetus, placenta and mother that ends up in the bloodstream. The researchers started by taking blood samples from pregnant women every week to see how levels of different RNAs changed during pregnancy and which could be used to predict gestational age or a premature birth. The blood test was accurate 45% of the time at predicting gestational age in experiments involving 38 women, compared with 48% for ultrasounds, the researchers say. The test was also used to predict preterm birth up to two months ahead of labour starting. It was used in two separate groups of women – in one it was right six times out of eight, in the other it worked four times out of five. Mira Moufarrej, one of the researchers, told the BBC: “I’m really excited about the potential of all this. “If we can use a mother’s blood to make healthcare more accessible and affordable to people that don’t have access to ultrasounds, then hopefully that means healthier babies and healthier pregnancies.” However, she emphasised this was still only a pilot study and the results needed to be confirmed in much larger trials. Prof Basky Thilaganathan, a Royal College of Obstetricians and Gynaecologists spokesman, said: “Complications from premature birth are a leading cause of infant mortality and affect 7-8% of all births in the UK.
“However, the number of cases in the study were small and the accuracy of prediction was poor for premature birth. More research is needed to confirm the findings before it can be considered in clinical settings.”
SOURCE: https://www.bbc.com/news/health-44386367
HEALTH CARE PARTNERS
Enjoy this recent research regarding Reducing Alarm Fatigue in the NICU, Team Coaching/Rounding and the significant and selective effects preterm birth has on the functional networks of a child’s brain.

Reducing Alarm Fatigue in Two Neonatal Intensive Care Units through a Quality Improvement Collaboration
Author information: Johnson KR1,2, Hagadorn JI1,2, Sink DW1,2.
Division of Neonatology, Connecticut Children’s Medical Center, Hartford, Connecticut. Department of Pediatrics, University of Connecticut School of Medicine, Farmington, Connecticut.
Abstract
OBJECTIVE:
To reduce nonactionable oximeter alarms by 80% without increasing time infants were hypoxemic (oxygen saturation [SpO2] ≤ 80%) or hyperoxemic (SpO2 > 95% while on supplemental oxygen).
STUDY DESIGN:
In 2015, a multidisciplinary team at Connecticut Children’s Medical Center initiated a quality improvement project to reduce nonactionable oximeter alarms in two referral neonatal intensive care units (NICUs). Changes made through improvement cycles included reduction of the low oximeter alarm limit for specific populations, increased low alarm delay, development of postmenstrual age-based alarm profiles, and updated bedside visual reminders. Manual alarm tallies and electronic SpO2 data were collected throughout the project.
RESULTS:
Alarm tallies were collected for 158 patient care hours with SpO2 data available for 138 of those hours. Mean number of total nonactionable alarms per patient per hour decreased from 9 to 2 (78% decrease) and the mean number of nonactionable low alarms per patient per hour decreased from 5 to 1 (80% decrease). No change was noted in the balancing measures of percentage time with SpO2 ≤ 80% (mean 4.3%) or SpO2 > 95% (mean 23.7%).
CONCLUSION:
Through small changes in oximeter alarm settings, including revision of alarm limits, alarm delays, and age-specific alarm profiles, our NICUs significantly reduced nonactionable alarms without increasing hypoxemia.
Am J Perinatol. 2018 May 21. doi: 10.1055/s-0038-1653945. [Epub ahead of print]
Thieme Medical Publishers 333 Seventh Avenue, New York, NY 10001, USA.
SOURCE: https://www.ncbi.nlm.nih.gov/pubmed/29783270

Team coaching and rounding as a framework to enhance organizational wellbeing, & team performance
Becoming an effective front-line nurse manager is a complex and dynamic process, particularly when nurses progress to these roles within their own unit when multifaceted interpersonal factors may feature. This article reports on a project referred to as, ‘Coaching and Rounding’ in the neonatal intensive care unit of the Women’s Hospital in Qatar. This project integrated leadership coaching activities with staff rounding on nurses they supervised using a structured framework. This project was designed to equip front-line nurse leaders with enhanced skills and techniques to promote a framework for developing relational leadership styles. Evaluation involved the charge nurses and staff under their supervision. Results suggested that there was improved supervisor-supervisee relationships, increased motivation and more frequent constructive feedback. The challenges to sustain these initial gains are the focus of ongoing initiatives. Full Article:
SOURCE:https://www.journalofneonatalnursing.com/article/S1355-1841(17)30074-1/fulltext

Preterm birth leaves its mark in the functional networks of the brain
Date: February 26, 2018 Source: University of Helsinki
Summary:
Researchers have demonstrated that premature birth has a significant and, at the same time, a very selective effect on the functional networks of a child’s brain. The effects can primarily be seen in the frontal lobe, which is significant for cognitive functions.
Premature birth is globally the most important risk factor for life-time disorders and defects in neurocognitive functions. However, current methods have not shed much light on how premature birth affects the early activity of neurons in the frontal lobe, significant specifically to cognitive functions.
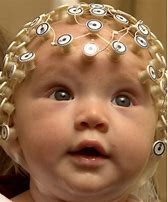
A study involving 46 infants exposed to very early prematurity and nearly 70 healthy and mature control infants was recently conducted at the University of Helsinki and the Helsinki University Hospital. Brain function in the infants was monitored and measured with the help of an EEG cap, developed earlier at the clinic, revealing new information on the subject.
“In this study, a new ‘source analysis’ method was used for the first time to measure functional networks in the infant brain: with the help of a computer model, the measured EEG signals were interpreted as activity in the infant cortex, which enabled the evaluation of the functional networking of neurons in a very versatile manner on the cortical level,” says Sampsa Vanhatalo, a professor in clinical neurophysiology and the head of the study.
It was found that there are several overlapping functional neural networks in the cortex of a newborn. Another finding was that premature birth has a significant, but also a very selective effect on these networks. The clearest effect can be seen in the functional networks of the frontal lobe, especially significant to cognitive functions.
“We were able to demonstrate how the strength of synapses in the frontal lobe is linked with the neurological abilities of infants. This provides an extremely interesting opportunity to use the functional networking of the brain as an early indicator in, for example, clinical trials that compare the effects of different treatments on brain development. The selective changes found in the study also provide a potential explanation for attention deficit and other cognitive issues often found in children who are prematurely born.”
Vanhatalo points out that functional MRI imaging does not show the functional coupling of an infant’s neurons, even though the method is still widely used all over the world for studying this very phenomenon.
“Therefore, our EEG findings are the first results that actually provide information on cortical functional networks in preterm infants.”
University of Helsinki. “Preterm birth leaves its mark in the functional networks of the brain.” ScienceDaily. ScienceDaily, 26 February 2018. <www.sciencedaily.com/releases/2018/02/180226090303.htm>.
SOURCE: https://www.sciencedaily.com/releases/2018/02/180226090303.htm
WARRIORS:

KAT: Returning to my NICU Home – Day 1
It was a beautiful sunny Spring day in Washington State. The cherry blossoms were beginning to peek through the tree tops, painting the outside entrance of the Medical Center in bursts of soft pinks and deep reds. My stomach felt as if it was going to burst as I put the car in park and gathered myself for the meeting about to transpire. I was a 21 year old woman taking footsteps back into the starting place of my life journey.
I arrived with sweaty palms to the hospital lobby and asked the volunteer at the check-in station directions to the Neonatal ICU Unit. Little did I know this station would soon become a familiar and frequent destination. Rounding the corner of the tiny café, I wound myself around a crowd of crisp lab coats, colorful scrubs, and anxious community members. Pressing the button of the Mountlake elevator I pondered what would take place. The elevator doors opened revealing a bright neon green sign that read “Neonatal Intensive Care Unit”. As a walked along the hallway, my eyes embraced a collage of beautiful portraits containing the short stories of various NICU Grads.
Enclosed behind sliding glass windows was the receptionist, who greeted me warmly. I told her my name and that I was meeting with the Medical Director. The kind receptionist escorted me to the unit lobby; a new glass enclosed structure that provided me with an outstanding view of South Lake Union. In nervous anticipation I sat admiring the ducks as I awaited the Director.
Soon, a nurse arrived and introduced me to a sturdy man with white hair, a perfectly trimmed beard, and twinkly blue eyes. Shaking hands with the physician I felt a wave of emotion come over me. Before me stood a renowned health-care provider who had helped save my life. As we spoke, I watched tears glisten in his eyes as the doctor shared with me that he had never met an adult NICU survivor that he had treated. I was shocked to learn that care providers like him so often never got the opportunity to be personally thanked by the tiny patients they served. In that moment I realized our meeting was not only meant for my own healing but for his as well. I realized that a gesture of gratitude may provide validation for the services health care providers contribute to their patients each day. I felt comforted hearing his condolences for the loss of my brother and he asked me about my mother. I learned about his passion for neonatal care and love for his family. He shared with me some of my medical history including my habit of pulling the oxygen tube out of my throat, setting off alarms. Our shared laughter sent us into a place of radiant joy. I expressed my interest in volunteering in the NICU and told him of my interest in medicine. With a hug we ended our meeting and I provided my contact information. While parting, he told me he would have the nurse manager contact me regarding volunteering. And so my journey back into the NICU began…..
*** In our March 16, 2018 blog (South Korea) we began to write our Writing For Wellness stories. Kat’s story continues in our next global adventure…….
Tandem Surfing UK
Published on Oct 10, 2016
What these people can do on a surfboard is incredible!





