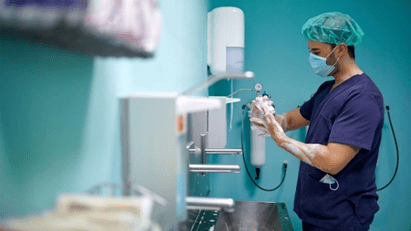
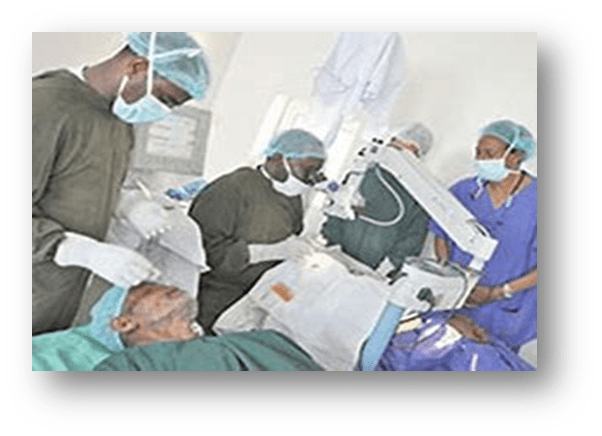
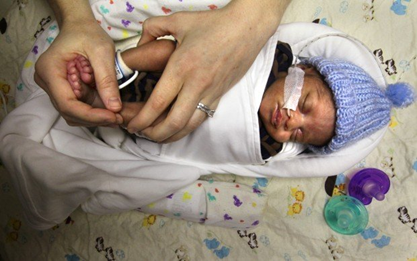
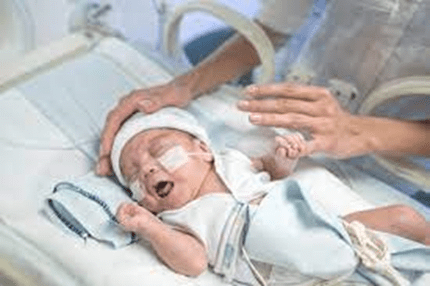
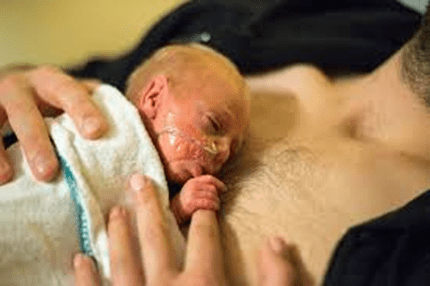
GLOBAL PRETERM BIRTH RATES – Latvia
Estimated # of preterm births: 5.40 per 100 live births
(USA Global Average: 9.56)
Source- WHO 2014- https://ptb.srhr.org/
Latvia, officially the Republic of Latvia, is a country in the Baltic region of Northern Europe. It is one of the Baltic states; and is bordered by Estonia to the north, Lithuania to the south, Russia to the east, Belarus to the southeast, and shares a maritime border with Sweden to the west. Latvia covers an area of 64,589 km2 (24,938 sq mi), with a population of 1.9 million. The country has a temperate seasonal climate. Its capital and largest city is Riga. Latvians belong to the ethno-linguistic group of the Balts; and speak Latvian, one of the only two surviving Baltic languages. Russians are the most prominent minority in the country, at almost a quarter of the population.
Latvia is a developed country, with a high-income advanced economy; ranking very high in the Human Development Index. It performs favorably in measurements of civil liberties, press freedom, internet freedom, democratic governance, living standards, and peacefulness. Latvia is a member of the European Union, Eurozone, NATO, the Council of Europe, the United Nations, the Council of the Baltic Sea States, the International Monetary Fund, the Nordic-Baltic Eight, the Nordic Investment Bank, the Organisation for Economic Co-operation and Development, the Organization for Security and Co-operation in Europe, and the World Trade Organization.
The Latvian healthcare system is a universal programme, largely funded through government taxation. It is among the lowest-ranked healthcare systems in Europe, due to excessive waiting times for treatment, insufficient access to the latest medicines, and other factors. There were 59 hospitals in Latvia in 2009, down from 94 in 2007 and 121 in 2006.
Source:https://en.wikipedia.org/wiki/Latvia

COMMUNITY

How to Protect Staff and Patients From Violence in the Hospital
From detection tools to staff training, children’s hospitals are upping their security measures in response to growing violence across the country. By Megan McDonnell Busenbark – Published Oct. 21, 2022

Mark Moore has spent his life in the business of protection. Since serving in the United States Marine Corps for more than a decade, he has provided security services for business leaders and world events—from Bill Gates to the Olympic Games. His first foray into the health care industry came in 2018 when he joined Dayton Children’s Hospital in Ohio as corporate director of Protective and Support Services, where he’s charged with keeping 27 locations safe—from the main campus to clinics and all other locations dedicated to care.
His first order of business: approaching senior leaders about new ways of protecting staff, patients and families from violence in the hospital—specifically, shootings. He quickly gained approval from his leadership team to make a million-dollar investment in gunshot detection technology. Since that time, the need for such measures has only grown.
“The events of the world have created a sense of urgency,” says Moore. When COVID-19 turned the world on its head, the health care setting saw increased incidents of violence brought on primarily by higher levels of patient and family stress, frustrations due to mask and visitation policies, and staffing shortages. The vulnerability of health care facilities has been coming to new light over the last year, as staff have been injured or killed in shootings in the workplace across the country. On a single day back in June, four staff members were fatally shot in two different adult hospitals—one in Dayton, Ohio, and the other in Tulsa, Oklahoma, where the shooter blamed his surgeon for his back pain.
These and other shootings have raised concerns about the health care setting becoming more of a soft target, like schools—prompting new discussion and action on security approaches to keep patients, families and staff safe in both inpatient and outpatient settings. This is coming in many forms—from increased staff training and safety officer deployment to visitor management strategies and weapon detection systems. It’s placing children’s hospitals in a delicate balancing act: deploying the most effective safety and security measures without losing the warm, welcoming environment they’ve worked for years to create.
Detection tools
In the past year, the University of Vermont Children’s Hospital in Burlington has experienced an unprecedented surge in violence in its emergency department. “The number of assaults on staff members has increased significantly,” says Stephen Leffler, M.D., president and COO at Vermont Children’s. “The number of episodes where weapons are discovered on someone who’s made it into the ED or even an inpatient floor has gone from essentially zero to happening more than occasionally—and they are very scary.”
As part of a larger hospital system, the emergency department serves both adults and children. Adding metal detectors became a necessity for staff safety, even though Leffler and his team were concerned about the effect it would have on patients’ experience and perception. “Clearly, going through metal detectors is not what you’re hoping for in the entrance of your ED. It sets a certain potential tone,” he says. “But we decided that in the interest of the safety of everyone, this was the right thing to do. And it was a tough decision.”
Since installing the detectors a couple of months ago, violence has already decreased, Leffler says. And so far, patients are more accepting of them than he anticipated. “We haven’t had many complaints, and they’re grateful to know we’re thinking about their safety,” he says. This sentiment is in line with published research showing that most patients respond favorably to the presence of metal detectors in pediatric emergency departments, feeling safer.
Metal detectors come with other challenges, however. They require enough space to install and to allow for adequate traffic flow. They require capital to purchase and maintain, as well as cash flow to keep them staffed 24 hours a day by officers who are trained in using the equipment and in responding to visitors who refuse to give up their weapon. At Vermont Children’s, two security officers operate the detectors—a job which includes searching bags and escorting contraband to secure lockers before visitors are allowed into the ED.
One potential drawback of metal detectors in emergency departments is patients having to wait in long lines, Leffler says. Even if the weather isn’t an issue, someone waiting might have an urgent medical need. To solve that, Vermont Children’s has an EMT evaluating those in line to determine if someone needs triage or prioritization. “Although these drawbacks are not ideal, this is the best thing we can do to help keep our patients, families and staff as safe as we possibly can,” Leffler says.
Many of the drawbacks and limitations of metal detectors can be circumvented with newer detection technology. Children’s National in Washington, D.C., is piloting a touchless security screening system that combines metal detection and artificial intelligence to spot concealed weapons. Unlike traditional screening systems—like those in airports—a person can walk through this unobtrusive device without stopping, without removing anything from their pockets or bags, without taking off their jewelry or belts. “You’re looking to provide care to people quickly—so you want to get them into your building in the most convenient and safest way possible,” says Paul Quigley, executive director of security, parking and transportation at Children’s National.
The system will alarm when someone brings anything that is shaped like a weapon and will show the security team exactly where the potential weapon is located on that individual. “It shows a picture of the person and a region of the body or bag or cart they’re wheeling in,” he says. “But the alarm is not alerting on keys, cell phones or change in your pocket because of the advanced analytics. So, most people walking through it don’t get detected in any way.”
In addition to keeping all patients, families and staff—including security—safer, it keeps the line moving and the visitor experience positive. During a one-day demo in June, more than 1,000 people entered the hospital through this system, and 90% of them were never stopped. The security team was able to process the other 10% within five seconds each time, once the individual opened their jacket or bag, according to Quigley—and there was never a line of people waiting to enter the building.
“During our demo, it did what it was supposed to do,” Quigley says. “That is, making the staff feel comfortable because we’re screening everybody coming through—and the patients and families loved it too, because they were able to feel like the hospital was safe.” Additionally, the screening system can be branded, making the technology fit into the environment.
In the emergency department, Quigley’s team uses metal detection wands in behavioral health cases and “if there’s a fear that some harm is going to be done toward either a provider or the patient themselves,” he says, adding that families have always understood the need for the wands in such instances. “This is to keep your family member safe and our staff safe,” he says. “That’s the thing that ends up making people feel more comfortable being in our environment.”
In addition to x-ray machines and walk-through detection systems, other detection and prevention methods children’s hospitals have implemented include K-9 security dogs, video surveillance, and weapon detection systems that integrate with security cameras. Generally, detection tools are more common in emergency departments where violence most frequently occurs and traffic is high.
These tools focus on detecting guns and weapons before they enter the building, but Dayton Children’s has also installed technology that detects guns after they are fired inside the hospital. Originally developed by the U.S. Department of Energy, the technology reads the energy instead of the sound of the gunshot, which helps reduce false alarms. The system alerts first responders in seconds—and the sensors are so specific, they can detect what caliber gun was used in the shooting. And because they look like smoke detectors, they blend right in with the hospital environment.
Moore and his team collaborated with about 10 groups across the hospital to test and implement the technology—from senior leadership and facilities to IT and systems integration. “We ran the technology in a sandbox for 30 days,” he says. “We had to make sure it played nicely with our access control system, our video management system and our mass notification system before going live.” Along with this rollout came Crisis Prevention Institute (CPI) training for staff, including active shooter response classes.
Staff training
Nick Markham, assistant vice president of facilities, has been with Cook Children’s Health Care System in Fort Worth, Texas, for 19 years. While training staff to reduce risk in the case of a shooting or other act of violence has long been a priority, the team has upped its game in the face of the events of the past year.
“We can create videos, webinars and just-in-time training for any event that takes place,” Markham says, citing a 20-minute training video that was created for staff within one week of the Tulsa shooting. Ongoing safety and security training covers situational awareness, de-escalation strategies and active criminal event response. The training, while not required, is available to all staff—and features active shooter drills where the instructor wears a body camera to simulate a shooting.
“He’s in the active shooter role, and he shows people what happens should a person enter the building and how quickly the escalation takes place,” says Markham. “So, he shows how people gain access to the back of house or the back of a clinic; how they try to get through a locked door; how easy it is to jump a reception desk—those types of things.” Then, he teaches staff about Avoid, Deny and Defend, meaning how to run, how to barricade yourself or how to fight back when faced with an incident.
Public safety officers
Both Cook Children’s and Dayton Children’s employ uniformed, armed public safety officers. Neither sees them as the traditional “officer” but rather an integral part of the hospital family and patient care.
“The officer should not be an opposing figure. This should be someone who’s protective, nurturing and offering assistance,” says Markham. Public safety officers at Cook Children’s are licensed police officers in the state of Texas, with compassion as part of their training.
“You have no idea what a person is going through—families are in a very hard place when they’re here with a sick child,” Markham says. “Our officers understand that. There’s a huge compassion component when you’re an officer.”
Another huge component is the connection with patients. The personification of that is Officer Louis White. “Everybody knows Officer Louis,” says Markham. “He is everywhere. He’s at orientation, he interacts with patients on our rehab unit—he is part of the care team that goes to that unit and does music therapy with the kids. So, we have folks ingrained into the organization in ways that go far beyond the role of a security officer.”
At Dayton Children’s, special care is taken when it comes to the role of behavioral health officers. They wear a different uniform in behavioral health units and don’t look the usual part of a public safety officer, which can help keep situations from escalating, Moore says. “They are still very clearly Dayton Children’s public safety officers, but they have none of what you would consider the tools of policing,” he says. “No handcuffs, no baton, no Taser, no pepper spray—they even have cloth Velcro badges.”
Across the board, children’s hospitals are reevaluating their approach to public safety officers, asking how many to deploy, what level of weaponry to carry, and what kind of protection to wear. Some officers carry pepper spray, others firearms; some wear ballistic vests, others plain clothes. Many hospitals, including Children’s National, hire off-duty law enforcement, who are armed, in addition to staff security. These officers enforce compliance during high-threat situations, deal with weapon-related incidents, and aid in arrests when necessary, says Quigley.
Managing visitors
While much of the work being done is focused on those who may be entering a facility with bad intent, the pressures are higher than ever to manage those who are supposed to be there—including families and other visitors. At the same time, children’s hospitals have always been built to be accessible—where staff can move patients easily and families can visit their children quickly and conveniently.
To help satisfy the need for safety and mobility, Cook Children’s uses an extensive network of cameras throughout the hospital. The cameras monitor visitors and all other activity in the hospital—as well as panic buttons in strategic places, like nurse stations and areas with a psychiatric component, to help minimize risk around potential events involving visitors.
At Children’s National, the team at the welcome desk checks all visitors against a robust database, ensuring all personnel, vendors and patient visitors are authorized to be there and pose no known threat. They also work closely with the staff upstairs in the care units to help determine which visitors—and how many—should be in a patient’s room at any time.
Because of the pandemic, Vermont Children’s reduced its number of visitor entrances to three, including the emergency department, to screen for COVID-19, and they decided to keep the limited number of entry points to better monitor visitors. Most floor entrances are locked as well, including the pediatric and mother-babies areas. They would like to implement strict visitor policies and management tools, but as with other security initiatives, staffing remains an obstacle.
Social workers
The Social Work Interventions with Families and Teams (SWIFT) program at Children’s National is designed to protect the frontline care team from incidents with patients and families inside the hospital while also ensuring those patients and families feel heard and supported. Verbal escalation, threatening behavior, physical aggression or impeding care on the part of a parent or other visitor often stem from the stress of having a sick or injured child in the hospital and being unable to communicate properly, says Brenda Shepherd-Vernon, director of the Department of Family Services at Children’s National Hospital. With SWIFT, social workers help mitigate such incidents to make staff feel safe, make families feel heard, and, ultimately, keep those families at the child’s bedside when possible.
“As social workers, we’re going to be impartial and look at what happened during the encounter—and we’ll work with the family and the team to resolve it,” Shepherd-Vernon says.
“In the past, the model dictated that security would be called if a parent was upset. Now, we’re trying to hear more about the families’ concerns and deal with those concerns in real time.”
Still, security is a close partner in SWIFT, along with a committee that reviews all cases of individuals who are asked to leave the premises due to aggressive behavior. The team also shares the expectations of conduct with the families to build a shared understanding and help prevent further incidents. There is also a huddle with the care team after an incident to discuss the concerns of the family and how to best address them going forward, as well as the resolution shared with the family and the plan to keep the staff safe.
Like none other
Leffler is part of a multi-sector collaborative that is seeking broader solutions to target the root causes of violence before it ever makes it to the children’s hospital. “What we’re seeing is just a piece of what is happening everywhere right now,” he says. “We want to come up with some recommendations to try and think about this problem in a bigger way than only once they arrive at the door of the hospital.”
For Moore’s part, protecting people, property and assets from harm has been at his core for the better part of 35 years. But he’s found that the children’s hospital setting is a world unto itself—one where keeping everyone safe physically, mentally and emotionally is paramount and constant.
“When I was running a protection team in my previous life, there were ebbs and flows,” he says. “We would ramp up to go on round-the-world trips with our protectees, working 16 to 18 hours a day—then we’d come home, catch our breath and ramp up for the next big thing. Here, the pace of the hospital is relentless. It never stops, it never closes. And everybody here wants to make the place better.”
Source:How to Protect Staff and Patients From Violence in the Hospital (childrenshospitals.org)
Empowering Parent and Educator resource. See the essential components as identified by this innovative resource provider!


Preterm Birth Information for Education Professionals

These five learning resources have been developed to improve your knowledge and confidence in supporting prematurely born children in the classroom.
- What is preterm birth?
- Educational Outcomes following preterm birth
- Cognitive and Motor Development following Preterm Birth
- Behavioural, social, and emotional outcomes following preterm birth
- How can education professionals support preterm children?
EXAMPLE:
Introduction
This section provides advice on how education professionals can support children born preterm. You may not know if a child was born preterm. Some parents are in favour of the school knowing their child’s birth history, but others prefer not to disclose this information. Don’t assume a child was born preterm just because they fit the profile described here. There are many reasons a child may have difficulties at school.
Regardless of whether you know a child’s birth history, the advice and strategies provided in this section are likely to be beneficial to any child with the difficulties described.
Children and young adults born preterm, and their parents, were asked what they wished their teachers had known about how they think and learn, and about how their preterm birth may have affected them later in life. Select the icons to hear some of their answers.

Source:https://www.nottingham.ac.uk/helm/dev/prism/rlo5/1.html#

Aminata – Maiga Vara (Acoustic video)

Ticking timebomb: Without immediate action, health and care workforce gaps in the European Region could spell disaster
40% of medical doctors are close to retirement age in one third of countries in Europe and central Asia, finds new WHO/Europe report
14 September 2022
All countries of the WHO European Region – encompassing 53 Member States across Europe and central Asia – currently face severe challenges related to the health and care workforce, according to a new report released today by WHO/Europe. An ageing workforce is chief among them. The analysis finds that 13 of the 44 countries that reported data on this issue have a workforce in which 40% of medical doctors are already aged 55 years or older.
An ageing health and care workforce was a serious problem before the COVID-19 pandemic, but is even more concerning now, with severe burnout and demographic factors contributing to an ever-shrinking labour force. Adequately replacing retiring doctors and other health and care workers will be a significant policy concern for governments and health authorities in the coming years. WHO/Europe is urging countries to act now to train, recruit and retain the next generation of health and care workers.
Another key finding of the report is the poor mental health of this workforce in the Region. Long working hours, inadequate professional support, serious staff shortages, and high COVID-19 infection and death rates among frontline workers – especially during the pandemic’s early stages – have left a mark.
Health worker absences in the Region increased by 62% amid the first wave of the pandemic in March 2020, and mental health issues were reported in almost all countries in the Region. In some countries, over 80% of nurses reported some form of psychological distress caused by the pandemic. WHO/Europe received reports that as many as 9 out of 10 nurses had declared their intention to quit their jobs.
“My own personal journey through this pandemic has been a rollercoaster,” said British nurse Ms Sarah Gazzard. “I was holding a phone next to a dying woman’s ear while her daughter said her final goodbyes. That was very, very difficult for me, so I sought out some support to help me cope.”
Mixed picture across the Region
While the 53 countries of the Region have on average the highest availability of doctors, nurses and midwives compared to other WHO regions, European and central Asian countries still face substantial shortages and gaps, with significant subregional variations.
Health worker availability varies 5-fold between countries. The aggregate density of doctors, nurses and midwifes ranges from 54.3 per 10 000 people in Türkiye to over 200 per 10 000 people in Iceland, Monaco, Norway and Switzerland. At the subregional level, central and western Asian countries have the lowest densities, and northern and western European countries have the highest.
“Personnel shortages, insufficient recruitment and retention, migration of qualified workers, unattractive working conditions, and poor access to continuing professional development opportunities are blighting health systems,” said Dr Hans Henri P. Kluge, WHO Regional Director for Europe.
“These are compounded by inadequate data and limited analytical capacity, poor governance and management, lack of strategic planning, and insufficient investment in developing the workforce. Furthermore, WHO estimates that roughly 50 000 health and care workers may have lost their lives due to COVID-19 in Europe alone.”
Dr Kluge warned, “All of these threats represent a ticking time bomb which, if not addressed, is likely to lead to poor health outcomes across the board, long waiting times for treatment, many preventable deaths, and potentially even health system collapse. The time to act on health and care workforce shortages is now. Moreover, countries are responding to the challenges at a time of acute economic crisis, which demands effective, innovative and smart approaches.”
Ms Annika Schröder is a midwife from Germany who works in a hospital where around 950 births take place every year. There, the challenges mirror those seen across the Region. “I often work shifts without even the possibility to go to the toilet, without breaks or time to eat,” she told WHO/Europe.
“The doorbell and the phones ring while we rush from one room to the other. On average, I take care of 2 women in labour at a time. This is not how I imagined my profession or my everyday working life to be. I am often exhausted and tired. The shortage of midwives makes births unsafe. And since the pandemic, things have got even worse. It is affecting the physical and mental health of us midwives, of mothers, women in labour and babies,” Ms Schröder explained.
Based on the latest data available for 2022, the Region has on average:
- 80 nurses per 10 000 people
- 37 doctors per 10 000 people
- 8 physiotherapists per 10 000 people
- 6.9 pharmacists per 10 000 people
- 6.7 dentists per 10 000 people
- 4.1 midwives per 10 000 people.
In WHO’s 2016 Global Strategy on Human Resources for Health, the threshold for aggregate health worker density was set at 44.5 doctors, nurses and midwives per 10 000 people. All countries in the Region are therefore currently above the threshold, but this does not mean they can afford to be complacent. There are serious gaps and shortages in the health and care workforce, which will only get worse with time without policies and practices to address them.
Rising to the challenge: country examples
“Countries will need to rethink how they support and manage their health workforce. They will need to design strategies that reflect their own contexts and needs, because there is no one-size-fits-all approach,” said Dr Natasha Azzopardi-Muscat, Director of the Division of Country Health Policies and Systems at WHO/Europe.
“The Region is at a critical juncture: strategic planning and smart investment are crucial next steps to make sure our health workers have the tools and support they need to care for themselves and their patients. Society will pay a heavy price if we fail to rise to this challenge. This new report and the data it includes about each of our Member States offer solutions and opportunities we shouldn’t miss.”
Many countries across the Region have already begun taking bold and innovative steps. In Ireland, where more people will be over the age of 65 than under the age of 14 by 2028, the Government has introduced the Enhanced Community Care programme to help the ageing population maintain independence. The programme releases pressure on the hospital system by bringing enhanced community care services to older people in towns and villages across the country.
In Kyrgyzstan, the Government has introduced a pay-for-performance system in primary health care. The aim is to attract more doctors by increasing salaries for those who perform well in their duties. The system also includes an offer for specialists to retrain as family doctors, as 30% of family doctors were of retirement age in 2020.
In the United Kingdom, the Government has been steadily recruiting foreign-trained nurses and midwives to replace those who are retiring or leaving the profession. At present, almost 114 000 foreign-trained nurses are registered there – a 66% increase since 2017/2018. Conversely, the number of nurses trained in the European Union (EU)/European Economic Area (EEA) dropped by nearly 18% over the same period. This is likely driven by the United Kingdom’s decision to leave the EU, and reflects a major shift from recruiting nurses from the EU/EEA to recruiting from other regions and countries, notably India, Nigeria and the Philippines.
Despite progressive steps in many places, much more investment, innovation and partnership are needed to avert further health and care workforce shortages in the future. WHO/Europe is urging all Member States – even those that currently have above-average workforce densities – to waste no time by taking the following 10 actions to strengthen the health and care workforce:
- align education with population needs and health service requirements
- strengthen professional development to equip the workforce with new knowledge and competencies
- expand the use of digital tools that support the workforce
- develop strategies that recruit and retain health workers in rural and remote areas
- create working conditions that promote a healthy work–life balance
- protect the health and mental well-being of the workforce
- build leadership capacity for workforce governance and planning
- improve health information systems for better data collection and analysis
- increase public investment in workforce education, development and protection
- optimize the use of funds for innovative workforce policies.
HEALTHCARE PARTNERS

A new patient population for adult clinicians: Preterm born adults
Amy L. D’Agata Carol E. Green Mary C. Sullivan Open Access Published: January 28, 2022

What if a single event could sway health, exercise capacity, learning style, social interactions, and even personal identities–yet individuals had no memory of the event? Adults born preterm are an under-recognized and vulnerable population. Multiple studies of individuals born prematurely, including our 35-year longitudinal study, have found important health concerns that adult healthcare providers should consider in their assessments. Concerns include increased rates of cardiovascular disease, metabolic syndrome, depression, anxiety and attention problems, lower educational attainment and frequency of romantic relationships.
A Nordic study of over six million individuals found a linear relationship between gestational age and protection against early adult mortality, with preterm individuals showing 1⋅4 times increased likelihood of early mortality as full-term peers.
At the same time, surviving premature birth has become increasingly common. For the last several decades, nearly one in nine U.S. babies is born early, and now more than 95% survive.
Global prevalence and survival data indicate more than 15 million preterm birth survivors annually reach adulthood.
This suggests a new population of individuals with emerging healthcare needs for adult health providers.
Birth history should be part of every patients’ medical record.
Due to the varied risks and prevalence of premature birth, all healthcare practitioners should be aware of the potential for long-term effects. With one in ten 30-year-old patients born preterm, clinical specialists who treat long-term complications of prematurity (i.e., neurology, psychiatry, cardiology) may have more preterm-born patients. Recognizing preterm birth as a cumulative, lifelong risk factor is the first step.
As clinicians and researchers, we have observed the medical community, like society at-large, tends to view prematurity as a health event localized to infancy-something kids outgrow. Ironically, some pediatric providers report limited training and understanding of health complications for children born preterm, and little evidence exists regarding adult practitioners’ knowledge to care for these adults.
Preliminary adult primary care guidelines were recently created to screen and manage prematurity-related health complications.
Health risks from prematurity are also risks to equality and justice. Women who bear social risk factors are more likely to give birth early. This includes Black women, those living in socio-economically depressed areas, and women with two or more Adverse Childhood Experiences.
The many arms of racism and caste-based inequalities can complicate and worsen the health of people already at risk from preterm birth.
Attention also needs to be drawn to the prematurity research community. To date, research has focused on younger age groups and predominantly White populations. Future research needs to seek out ethnically diverse populations and comprehensively examine potential life course complications of early birth. This is especially important when considering how socioeconomic factors may influence the allostatic load of individuals.
For many born preterm, prematurity is not just a health concern, it’s a matter of who they are. Their perception of health over time, or health related quality of life (HRQL), is a critical outcome. To date, this evidence varies with age, degree of prematurity and reporter; clinicians and parents tend to rate HRQL more negatively than survivors.
Preterm-born individuals may not have event memories but, early birth repercussions can reverberate through family narratives and unique life experiences. Some identify as typically developed individuals who happen to have been born early, others as functional and well-adapted “preemies”, and others see prematurity as having colored their lives in negative ways.
As prematurity researchers, we aim to uncover and bring awareness to the health outcomes and risks from early birth. A critical need exists for more evidence about adult health following preterm birth and yet, how do we protect individuals with statistically increased risk without unnecessarily pathologizing them?
In clinical practice and research settings, we can take the opportunity to listen to people who were too young as patients to speak for themselves but have riveting and complex stories about preterm birth’s effects. We are aware of just one other published qualitative study about the experiences of adults born preterm.
Because most adult healthcare providers have yet to acknowledge and factor this experience into patient care, individuals born preterm are finding alternative avenues to be seen. Adults born preterm report seeking online community and support, connecting globally with people over shared early life experiences, while simultaneously making their needs and identities known.
As a research team, we strive to avoid labels for people born early but have nonetheless found that they are, in often subtle ways, a special group. They beat the odds as infants. Their birth and subsequent survival affected their families and communities in unprecedented ways. As clinicians and researchers, we can attend to the health risks of those born premature while acknowledging and celebrating their unique strengths and perspectives, often resulting from their early life experiences.
Source: https://www.thelancet.com/journals/lanam/article/PIIS2667-193X(22)00005-9/fulltext

WHO advises immediate skin to skin care for survival of small and preterm babies
15 November 2022

WHO today launched new guidelines to improve survival and health outcomes for babies born early (before 37 weeks of pregnancy) or small (under 2.5kg at birth).
The guidelines advise that skin to skin contact with a caregiver – known as kangaroo mother care – should start immediately after birth, without any initial period in an incubator. This marks a significant change from earlier guidance and common clinical practice, reflecting the immense health benefits of ensuring caregivers and their preterm babies can stay close, without being separated, after birth.
The guidelines also provide recommendations to ensure emotional, financial and workplace support for families of very small and preterm babies, who can face extraordinary stress and hardship because of intensive caregiving demands and anxieties around their babies’ health.
“Preterm babies can survive, thrive, and change the world – but each baby must be given that chance,” said Dr Tedros Adhanom Ghebreyesus, WHO Director-General. “These guidelines show that improving outcomes for these tiny babies is not always about providing the most high-tech solutions, but rather ensuring access to essential healthcare that is centred around the needs of families.”
Prematurity is an urgent public health issue. Every year, an estimated 15 million babies are born preterm, amounting to more than 1 in 10 of all births globally, and an even higher number – over 20 million babies – have a low birthweight. This number is rising, and prematurity is now the leading cause of death of children under 5.
Depending on where they are born, there remain significant disparities in a preterm baby’s chances of surviving. While most born at or after 28 weeks in high-income countries go on to survive, in poorer countries survival rates can be as low as 10%.
Most preterm babies can be saved through feasible, cost-effective measures including quality care before, during and after childbirth, prevention and management of common infections, and kangaroo mother care – combining skin to skin contact in a special sling or wrap for as many hours as possible with a primary caregiver, usually the mother, and exclusive breastfeeding.
Because preterm babies lack body fat, many have problems regulating their own temperature when they are born, and they often require medical assistance with breathing. For these babies, previous recommendations were for an initial period of separation from their primary caregiver, with the baby first stabilized in an incubator or warmer. This would take on average, around 3-7 days.
However, research has now shown that starting kangaroo mother care immediately after birth saves many more lives, reduces infections and hypothermia, and improves feeding.
“The first embrace with a parent is not only emotionally important, but also absolutely critical for improving chances of survival and health outcomes for small and premature babies,” said Dr Karen Edmond, Medical Officer for Newborn Health at WHO. “Through COVID-19 times, we know that many women were unnecessarily separated from their babies, which could be catastrophic for the health of babies born early or small. These new guidelines stress the need to provide care for families and preterm babies together as a unit, and ensure parents get the best possible support through what is often a uniquely stressful and anxious time.”
While these new recommendations have particular pertinence in poorer settings that may not have access to high-tech equipment, or even reliable electricity supply, they are also relevant for high-income contexts. This calls for a rethink of how neonatal intensive care is provided, the guidelines state, to ensure parents and newborns can be together at all times.
Throughout the guidelines, breastfeeding is strongly recommended to improve health outcomes for preterm and low birthweight babies, with evidence showing it reduces infection risks compared to infant formula. Where mother’s milk is not available, donor human milk is the best alternative, though fortified ‘preterm formula’ may be used if there are no donor milk banks.
Integrating feedback from families gathered through over 200 studies, the guidelines also advocate for increased emotional and financial support for caregivers. Parental leave is needed to help families care for the infant, the guidelines state, while government and regulatory policies and entitlements should ensure families of preterm and low birthweight babies receive sufficient financial and workplace support.
Earlier this year, WHO released related recommendations onantenatal treatments for women with a high likelihood of a preterm birth. These include antenatal corticosteroids, which can prevent breathing difficulties and reduce health risks for preterm babies, as well as tocolytic treatments to delay labour and allow time for a course of corticosteroids to be completed. Together, these are the first updates to WHO’s preterm and low birth weight guidelines since 2015.
NEW Guidelines: https://www.who.int/publications/i/item/9789240058262https://www.who.int/news/item/15-11-2022-who-advises-immediate-skin-to-skin-care-for-survival-of-small-and-preterm-babies

Neonatal Brain Protocol
Ultrasound Protocols Sonographic Tendencies Mar 23, 2021
How I do it. Neonatal Brain Ultrasound Protocol As I’ve said before, every institution may do it a bit different but these are required views.
Blogpost: https://sonographictendencies.com/201… Medical Disclaimer: https://sonographictendencies.com/about/


Patent to be Issued to LSU Health New Orleans for Technology to Diagnose Life-Threatening Preemie Condition
November 7, 2022
US Patent 11,493,515 will be issued to LSU Health New Orleans on November 8, 2022, for a noninvasive test that more accurately diagnoses a potentially fatal condition in premature infants. Sunyoung Kim, PhD, Professor of Biochemistry and Molecular Biology at LSU Health New Orleans Schools of Medicine and Graduate Studies, led a research team that invented a diagnostic biomarker test for necrotizing enterocolitis (NEC) called NECDetect.
According to the National Institute of Child Health and Human Development, NEC is the most common, serious gastrointestinal disease affecting newborn infants. The tissue lining the intestine becomes inflamed, dies, and can slough off. Health care providers consider this disease as a medical and surgical emergency. X-rays are now used to diagnose advanced disease, but their sensitivity can be as low as 44%. Conversely, the noninvasive NECDetect biomarker panel performed on stool samples identifies 93% true positives and 95% true negatives in diagnosing the disease.
In 2017, Dr. Kim founded Chosen Diagnostics Inc, a spinout company, to develop and commercialize the technology. An Express License for Faculty Startups (ELFS) agreement executed by LSU Health and Chosen Diagnostics Inc in 2020 grants the company the exclusive license to this portfolio of patent and patent applications.
“This patent is an important milestone in protecting the commercial potential of molecular diagnostic tools in intensive care units,” notes Dr. Kim. “Necrotizing enterocolitis continues to be a devastating disease for preemie babies who require long hospital stays. This utility patent is attractive to diagnostic companies that already provide equipment to hospital pathology labs and for drug companies interested in tackling gut disease therapies.”
The National Institute of Child Health and Human Development estimates that NEC affects about 9,000 of the 480,000 infants born preterm each year in the United States. The population most at risk for NEC is increasing because the number of very low birth weight babies who survive continues to grow due to technological advances in care. The percentage of very low birth weight infants who develop NEC remains steady, however, at about 7%. NEC continues to be one of the leading causes of illness and death among preterm infants, although it can also affect full-term babies, usually those with another serious illness or risk factor. Fifteen to forty percent of infants with NEC die from the disease. Surgical survivors require lifelong care.
Rebecca Buckley, PhD, LSU Health New Orleans Research Assistant Professor of Biochemistry (and former postdoctoral research associate), is a co-inventor and Chosen Diagnostics’ Chief Operating Officer. LSU Health inventors also included two other females — Dr. Duna Penn, a member of the Neonatology faculty at the time, and Zeromeh Gerber MD, a former LSU Health neonatology fellow, along with Carl Sabottke, a medical student at the time of the initial application.
“This patent is a rarity in that the majority of the team are women,” adds Dr. Kim. “In the 2020 United States Patent and Trademark Office database of all patents issued, only four women in Orleans Parish are inventor-patentees for the whole year. This number has not changed much since 1976.”
Chosen Diagnostics Inc has been awarded $3M in SBIR and STTR grants, and NECDetect’s development was fast-tracked with a Breakthrough Device Designation by the Food and Drug Administration (FDA).
“Intellectual property is the foundation upon which successful biotech businesses are built,” says Patrick Reed, RTTP, LSU Health New Orleans Assistant Vice Chancellor, Innovation & Partnerships. “Working with external counsel, the inventors, and Chosen Diagnostics, we have ensured that this important work is adequately protected, enabling Chosen to attract investment for further R&D and commercialization.”
In addition to this US patent, patent applications are pending in Canada, Europe, Hong Kong, Australia, New Zealand, and China.

PREEMIE FAMILY PARTNERS

Preterm Birth – What you need to know about babies born early and a NICU hospitalization
Week 24 of pregnancy is a HUGE milestone as it means the developing baby now has greater than 50% chance of survival with medical help if born today! This week we cover the big things to know about baby’s chances if born early, what some of the concerns are for babies born early, and some tips for new parents with a baby in the neonatal intensive care unit (NICU).


Lost in Transition: Health Care Experiences of Adults Born Very Preterm—A Qualitative Approach
Front. Public Health, 30 November 2020 Anna Perez1*†, Luise Thiede1†, Daniel Lüdecke2, Chinedu Ulrich Ebenebe1, Olaf von dem Knesebeck2 and Dominique Singer1 Section Neonatology and Pediatric Intensive Care Medicine, Center for Obstetrics and Pediatrics, University Medical Center Hamburg-Eppendorf, Hamburg, Germany – Center for Psychosocial Medicine, Institute of Medical Sociology, University Medical Center Hamburg-Eppendorf, Hamburg, Germany
Introduction: Adults Born Very Preterm (ABP) are an underperceived but steadily increasing patient population. It has been shown that they face multiple physical, mental and emotional health problems as they age. Very little is known about their specific health care needs beyond childhood and adolescence. This article focuses on their personal perspectives: it explores how they feel embedded in established health care structures and points to health care-related barriers they face.
Methods: We conducted 20 individual in-depth interviews with adults born preterm aged 20–54 years with a gestational age (GA) below 33 weeks at birth and birth weights ranging from 870–1,950 g. Qualitative content analysis of the narrative interview data was conducted to identify themes related to self-perceived health, health care satisfaction, and social well-being.
Results: The majority (85%) of the study participants reported that their former prematurity is still of concern in their everyday lives as adults. The prevalence of self-reported physical (65%) and mental (45%) long-term sequelae of prematurity was high. Most participants expressed dissatisfaction with health care services regarding their former prematurity. Lack of consideration for their prematurity status by adult health care providers and the invisibility of the often subtle impairments they face were named as main barriers to receiving adequate health care. Age and burden of disease were important factors influencing participants’ perception of their own health and their health care satisfaction. All participants expressed great interest in the provision of specialized, custom-tailored health-care services, taking the individual history of prematurity into account.
Discussion: Adults born preterm are a patient population underperceived by the health care system. Longterm effects of very preterm birth, affecting various domains of life, may become a substantial burden of disease in a subgroup of formerly preterm individuals and should therefore be taken into consideration by adult health care providers.
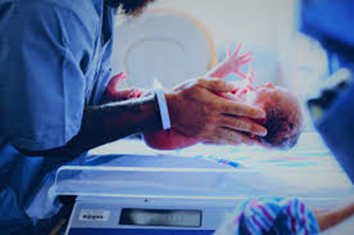
Sensors are first to monitor babies in the NICU
An interdisciplinary Northwestern University team has developed a pair of soft, flexible wireless body sensors that replace the tangle of wire-based sensors that currently monitor premature babies in hospitals’ neonatal intensive care units (NICU) and pose a barrier to parent-baby cuddling and physical bonding. The team recently completed a series of first human studies on premature babies at Prentice Women’s Hospital and Ann & Robert H. Lurie Children’s Hospital of Chicago. The researchers concluded that the wireless sensors provided data as precise and accurate as that from traditional monitoring systems. The wireless patches also are gentler on a newborn’s fragile skin and allow for more skin-to-skin contact with the parent. Existing sensors must be attached with adhesives that can scar and blister premature infants’ skin.


After premature birth: your emotions

Key points
- Mixed and powerful emotions are common after premature birth.
- All emotions are OK. Accepting and talking about emotions can help you cope.
- It can help to focus on your baby’s successes and milestones.
- When you look after yourself, you’ll be in better shape to care for your baby.
Your emotions after premature birth: what to expect
It’s natural to have many mixed, powerful and conflicting emotions about premature birth.
There are positive emotions, of course, like joy and love for your newborn.
But it’s common to wonder about what happened and what caused the premature birth. You might feel helpless, sad, guilty, anxious or traumatised by the birth experience. There might also be concern, fear and confusion about seeing your premature baby in the neonatal intensive care unit (NICU) or special care nursery (SCN).
Some parents might feel angry at themselves or their doctors. Or they might feel angry at their premature baby for making them feel this bad or for being born early. This might mean they feel reluctant to hold their baby or visit the neonatal intensive care unit (NICU). This is OK too.
Many people feel like things aren’t quite real. And it’s easy to feel powerless or as if you have no control over the future. It’s common to feel lonely. Some people find it hard to see themselves as parents while their premature baby is in the NICU.
Many parents find it very hard to leave their premature baby at the hospital while they go home.
Over time, there are generally fewer challenges, and they get easier to cope with. And as your premature baby gets bigger and more medically stable, you’ll be able to hold and care for them more often. As you get to know the NICU, it will feel more comfortable too. The nursing staff and other members of your baby’s care team will help you as well as care for your baby.
All of this can help you to feel more confident, less anxious and better able to connect and bond with your premature baby.
Tips for managing emotions about premature birth
Here are some ideas that might help you manage your emotions.
Managing emotions
- Accept your feelings, whatever they are – don’t push them away. Acknowledging and naming your emotions is a healthy thing to do.
- Be kind to yourself, and remind yourself that you’re doing the best you can.
- If you can, get to know other parents who are in a similar situation. It helps to hear how other parents are coping, but remember that there’s no one right way to feel or respond.
- Accept your partner’s way of coping if it’s different from yours. Try to let your partner do things their own way, and find out how your partner is feeling by talking to each other and listening to each other.
Looking after yourself
- Eat healthy food, do physical activity, and get as much rest as you can. It’s also a good idea to limit caffeine and alcohol and other drugs.
- Surround yourself with people who help you to feel supported.
- Avoid unnecessary stress, if you can. It’s OK to let some things go or not do things the way you usually do while you focus on your premature baby and your family for a while.
- Take a day off from the NICU every now and then so you can do things for yourself as well.
- Take time to relax and do things you enjoy each day, even for just a few minutes. For example, do breathing exercises, listen to your favourite music, or go for a walk around the block. You can also do breathing exercises or listen to music while sitting next to your baby in the hospital.
Being with your baby
- Celebrate successes, positives and progress – yours and your premature baby’s. Your baby might be in the NICU, but they’ll be reaching their own goals and milestones.
- Get involved in your premature baby’s day-to-day care. This can help you bond with your baby, which is good for your baby and good for you.
- Find out how you can help your premature baby. For example, you might learn about one piece of technology or your baby’s stress signs, or about how to change a nappy gently. Just focus on one thing at a time.
- Remember that there are things only you as a parent can do. Your touch, smell and voice are all very important for your premature baby. You’re also your baby’s most important advocate.
Seeking support
- Talk with trusted family members or friends about your emotions. It’s OK to share negative feelings and to say what you need. This might be someone just to listen or someone who doesn’t mind if you cry.
- Seek support only from people you feel comfortable with. It’s OK to not to seek support from people who cause you tension and stress.
- Ask your nurse if you can speak with someone at the hospital who can help you manage your emotions.
- Speak with your GP, who can guide you to an appropriate mental health professional.
- Contact Lifeline, Beyond Blue or your state or territory parent helpline.
It’s important to look after yourself in these early days and weeks of your premature baby’s life. When you look after yourself, you’ll be in better shape to care for your baby.
More than baby blues: postnatal depression after premature birth
Mood changes are common after you’ve had a baby. They can vary from mild to severe.
Many birthing mothers experience the ‘baby blues’ – a mild depression in the days after childbirth. If it continues and becomes more severe, it could become postnatal depression (PND). Non-birthing parents can suffer from PND too.
Signs of PND include a persistent feeling of sadness, low mood, feelings of hopelessness, lack of energy, low self-esteem and sleep problems.
If you think you’re experiencing the signs of postnatal depression in birthing mothers or postnatal depression in non-birthing parents, it’s important to get professional help as soon as you can. Your GP is a good place to start. With proper diagnosis, treatment and support, you can make a full recovery.

INNOVATIONS
Late-Onset Sepsis Among Very Preterm Infants
Dustin D. Flannery, DO, MSCE; Erika M. Edwards, PhD, MPH; Sarah A. Coggins, MD; Jeffrey D. Horbar, MD;Karen M. Puopolo, MD, PhD

OBJECTIVES:
To determine the epidemiology, microbiology, and associated outcomes of late-onset sepsis among very preterm infants using a large and nationally representative cohort of NICUs across the United States.
METHODS:
Prospective observational study of very preterm infants born 401 to 1500 g and/or 22 to 29 weeks’ gestational age (GA) from January 1, 2018, to December 31, 2020, who survived >3 days in 774 participating Vermont Oxford Network centers. Late-onset sepsis was defined as isolation of a pathogenic bacteria from blood and/or cerebrospinal fluid, or fungi from blood, obtained >3 days after birth. Demographics, clinical characteristics, and outcomes were compared between infants with and without late-onset sepsis.
RESULTS:
Of 118 650 infants, 10 501 (8.9%) had late-onset sepsis for an incidence rate of 88.5 per 1000 (99% confidence interval [CI] [86.4–90.7]). Incidence was highest for infants born ≤23 weeks GA (322.0 per 1000, 99% CI [306.3–338.1]). The most common pathogens were coagulase negative staphylococci (29.3%) and Staphylococcus aureus (23.0%), but 34 different pathogens were identified. Infected infants had lower survival (adjusted risk ratio [aRR] 0.89, 95% CI [0.87–0.90]) and increased risks of home oxygen (aRR 1.32, 95% CI [1.26–1.38]), tracheostomy (aRR 2.88, 95% CI [2.47–3.37]), and gastrostomy (aRR 2.09, 95% CI [1.93–2.57]) among survivors.
CONCLUSIONS:
A substantial proportion of very preterm infants continue to suffer late-onset sepsis, particularly those born at the lowest GAs. Infected infants had higher mortality, and survivors had increased risks of technology-dependent chronic morbidities. The persistent burden and diverse microbiology of late-onset sepsis among very preterm infants underscore the need for innovative and potentially organism-specific prevention strategies.
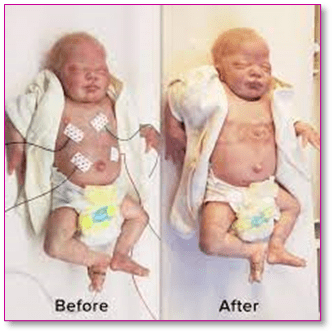
New wireless monitors let premature babies have skin-to-skin contact even in the NICU

Premature and ill babies thrive with direct contact, but wires from traditional sensors get in the way
Parents may feel helpless when their children are in the neonatal intensive care unit (NICU), and they can develop anxiety, depression, and anger. Seeing their infants isolated and entangled in wires that tether them to massive medical devices for monitoring vital signs is gruesome and heart-wrenching.
Approximately 450,000 babies are born premature in the US every year, sometimes weighing as little as 500 grams. They need constant clinical monitoring in the NICU as they might develop complications by being born unusually early in development. An additional 480,000 children spend time in the NICU or pediatric intensive care unit annually because of a critical illness.
Biosensors indeed enhance the quality of neonatal and pediatric clinical care by allowing parents to hold their babies, feed them conveniently, and clean them in a timely manner.
Precise monitoring of NICU patients is essential but invasive, typically requiring specialized catheters inserted into the patient’s tiny veins. Wired monitoring can cause scarring and increase the risk of infections and complications, such as blood clots and blood vessel blockage. Wires also get in the way of feeding and cleaning. Above all, a major disadvantage of wired monitoring is that it impedes skin-to-skin contact between parent and newborn, which has been scientifically shown to have clinical advantages for the newborn.
New technology developed by a group of American, Chinese, and Korean researchers headed by Debra Weese-Mayer, John Yoon Lee, and John Rogers may solve many problems introduced by wired monitoring of NICU patients. The first of its kind, these non-invasive, wireless biosensors can continuously monitor vital parameters by merely attaching as a patch on a skin surface.
The wireless biosensor consists of two parts, a chest and a limb unit, both of which fit inside the palm of an adult hand. The chest unit can be gently mounted on to the infant’s chest or back, while the limb unit has can go around a foot, palm, or toe. This means that the biosensor covers a wide range of infant ages and anatomies, including interfaces such as wrist-to-hand and foot-to-toe sensing. Researchers have demonstrated its successful clinical use in extremely premature infants, as young as 27 weeks of gestational age but who have been out of the womb for 6 weeks. At that point, they are about the size of a head of lettuce.
The sensor can simultaneously monitor a range of health indicators, including breathing and blood oxygen levels, at a level that is comparable to standard FDA-approved monitoring systems. It harbors an accelerometer that measures chest vibrations to generate a seismocardiogram (SCG), which provides similar information as an electrocardiogram (EKG) that monitors cardiac muscle activity and valve motion, but is better suited for small infants because it provides a direct assessment of the mechanical activity of the heart. The device also records an infant’s cries, which can be used to analyze an infant’s pain and stress levels.
The previous prototype of biosensors created by the researchers worked wirelessly, although it lacked several features compared to the current design, such as relaying the recorded patient data to a computer system placed far from the sensor. Another challenge was fixing the fragile nature of the sensor without compensating its flexibility, which is key to recording on highly curved surfaces such as the chest, ankles, and toes.
A year later, the same researchers came up with a novel model with additional built-in features that solve many of the issues that the earlier version had. The electronic components of the device are sandwiched between waterproof silicone covers, so they sit comfortably on the sensitive skin of infants. The sensor can draw power from onboard batteries or from a nearby antenna placed 30-50 cm away from the biosensor, ensuring that it never lose’s track of it’s patient’s vital signs.
The device uses Bluetooth and can transmit data into a computer system 10 meters away, meaning they can take records within a standard-sized patient room. The sensors can be sterilized between patients, and they do not generate heat for up to 24 hours, making them reliable and safe to use.
Biosensors enhance the quality of neonatal and pediatric clinical care by allowing parents to hold their babies, feed them conveniently, and clean them in a timely manner. The design is also inexpensive, durable, cost-effective, and can even be used outside a hospital setting with the data being recorded on a tablet or a cell phone.
This simple technology can be expanded beyond infants and children. Patients who need outpatient monitoring, such as those sent home after a surgery, or those with chronic conditions, could also use the device. Sharing the monitoring data with a physician online could also cut down on non-emergency hospital visits.
Although this technology is wonderful, it will probably be some time before it can be used in hospitals. This is one of the first studies to record data in real NICU patients, so more confirmation is required to ensure the reliability of these biosensors.
A physician’s human touch gives an emotional connection, but if parents are comfortable, this biosensor technology can serve as a boon by monitoring infants continuously to watch out for anomalies.

Role of Neurosonography in Critically Ill Neonates in NICU
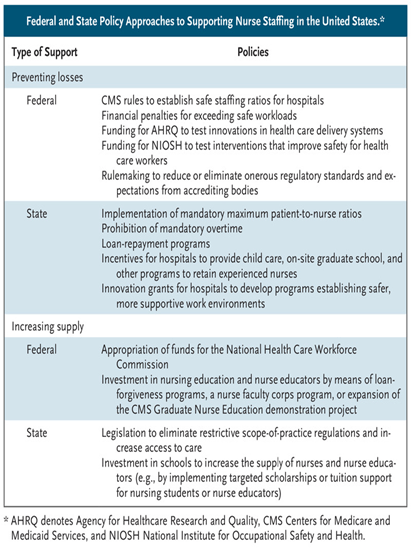
Rupesh Rao, Amar Taksande, Sneh Kumar+2View all authors and affiliations Volume 36, Issue 3https://doi.org/10.1177/09732179221113674
Abstract
Background
Neurosonography has been commonly used for screening in neonatal intensive care unit (NICU), for early detection of defects in the central nervous system (CNS) which include findings like intracranial hemorrhage, hydrocephalus, cerebral edema, and other structural abnormalities.
Aim
To detect the CNS abnormality in critically ill neonates by neurosonography.
Materials and Methods
This was a cross-sectional study done in the NICU of AVBR Hospital, Sawangi Meghe, Wardha. Neonates were defined as “critically ill” after taking their detailed history and performing a complete physical examination. Following this, the newborns who fulfilled the studies’ inclusion criteria were subjected to neurosonogram. The following factors were considered: gestational age, clinical examination, investigations, neurosonography findings, and outcomes.
Results
A total of 150 critically ill newborns were subjected to neurosonography, 24 of them had abnormal findings. There was a significant correlation of gestational weeks, mode of delivery, and diagnosis of critically ill neonates with abnormal neurosonography (P = .000, P = .000, and P = .000). Prematurity was the most common diagnosis followed by meningitis. A total of 16% of the newborns had abnormal results in neurosonography. About 6.67% of these had hydrocephalus, 5.34% had an intraventricular hemorrhage (IVH), 1.34% had periventricular echogenicity, 0.66% had cerebral edema, 0.67% had germinal matrix hemorrhage, and 0.66% had brain abscess. A total of 109 (72.67%) participants in the study had a positive outcome at the time of discharge from NICU; whereas, 27 (18%) unfortunately did not survive.
Conclusion
Neurosonography is thus a valuable, safe, and effective diagnostic tool used for screening critically ill neonates for abnormalities of the brain.
Source:https://journals.sagepub.com/doi/abs/10.1177/09732179221113674


For our little family members! A fun story…
Joy by Corrinne Averiss



Why Happiness Matters
Think how wonderful the world would be if we all did what made us happy. Wouldn’t it be amazing to live in a world where we let go of the “should” and followed our hearts to what was truly important to us?
By Nathalie Thompson, Contributor Feb 1, 2016, 04:47 PM EST|Updated Dec 6, 2017
“Happiness is the meaning and the purpose of life, the whole aim and end of human existence.” – Aristotle
Happiness matters, more than you might realize. It’s important to your physical and mental health, your resiliency in the face of obstacles and crises, and believe it or not, your happiness is important to the happiness of the world at large.
Your Happiness Matters to the Whole World
Yes, you heard me — your personal happiness is important to the happy quotient of the entire world. But somewhere along the way, we’ve picked up this horribly damaging belief that wanting to be happy is selfish and arrogant. We’ve made ourselves believe that what we want most in life is not important, and that we don’t deserve it.
We’ve somehow managed to twist ourselves so out of alignment with Who We Really Are that we’ve come to believe that suffering is expected, and even virtuous! We’ve come to believe that in pursuing our own happiness, we will somehow destroy or negate the happiness of others. And so we give up on believing that our own happiness matters and we resign ourselves to a lifetime of misery because we don’t want to hurt anyone and we don’t want anyone to think badly of us.
But here’s the thing: Being happy yourself is one of the best things you can do to help other people be happy, too! We’ve all had the experience of knowing someone who seems to light up a whole room when they enter it — the kind of person who makes other people feel happy, just be being around them. Happiness has a ripple effect far beyond a single individual — when you are happy, other people (your partner, your kids, your friends, etc.) notice and are themselves influenced by your mood.
This is not just anecdotal, there’s scientific evidence: When you are happy, you boost the moods of everyone you encounter and (here’s where it gets really cool) those people whose moods you have affected will then affect the moods of everyone they encounter, too!
The Happiness Cascade Effect
This happiness “cascade effect” was documented in a study published in 2008 in the British Medical Journal. Researchers from Harvard and the University of California, San Diego discovered that “clusters of happiness result from the spread of happiness and not just a tendency for people to associate with similar individuals” and that the happiness of single individuals affects even those they don’t know… through three degrees of separation!
That means that if you are happy, not only does it make your friends happier, it also makes their friends happier and their friends’ friends happier, too!
If one person is happy, that increases the chances of happiness in a friend living within a mile by 25 percent. The “cascade” effect, as the researchers put it, continues: a friend of the friend has almost a 10 percent higher likelihood of being happy, and a friend of that friend has a 5.6 percent increased chance.
See? Happiness is contagious! So, far from being a selfish thing, the pursuit of your own happiness can be seen as a generous public service — and perhaps even a civic duty of sorts, to increase the happiness of society as a whole!
Think how wonderful the world would be if we all did what made us happy. Wouldn’t it be amazing to live in a world where we let go of the “shoulds” and followed our hearts to what was truly important to us?
Your happiness matters — to all of us. So figure out what makes your heart sing… and then go out there and do it.
Source:https://www.huffpost.com/entry/why-happiness-matters_b_9126862


Author Sheryl Sandberg said happiness is made up of numerous small moments of joy. The more you experience joyous emotions, the happier you are. Learning to shift our perspective to a positive one can greatly impact our outlook on navigating life. Through my life experience I have learned over time that choosing happiness is a skill. Thus, making the choice to become more aware of what brings us joy in life can help us cultivate our own happiness.
There is joy in the daily things we do if we just pay attention. Discovering what brings us joy through our passions, purpose, daily activities, interest, and close relationships can drive “the happiness cascade” in how we interact with the world and others around us.
What are the small moments in your life that bring you great joy?
For me, the simplicity of enjoying my daily workout, greeting my cat after the workday, catching up with internationally located friends, cooking with my mom and going on walks throughout the city with a coffee in hand brings snippets of joy into my daily life.
As we move into the holiday season, we wish you and yours great joy and happiness in the big and small moments in life.


#News #Reuters #adventuresports
Mar 28, 2021: A group of friends in Latvia have adapted their hobby to the harsh weather conditions to create a new sport they have dubbed ‘kiteskating.’