

PRETERM BIRTH RATES – SUDAN
Rank: 34 –Rate: 13.2% Estimated # of preterm births per 100 live births
(USA – 12 %, Global Average: 11.1%)
Sudan, officially the Republic of the Sudan is a country in Northeast Africa. It shares borders with the Central African Republic to the southwest, Chad to the west, Egypt to the north, Eritrea to the northeast, Ethiopia to the southeast, Libya to the northwest, South Sudan to the south and the Red Sea. It has a population of 45.70 million people as of 2022 and occupies 1,886,068 square kilometres (728,215 square miles), making it Africa’s third-largest country by area, and the third-largest by area in the Arab League. It was the largest country by area in Africa and the Arab League until the secession of South Sudan in 2011, since which both titles have been held by Algeria. Its capital is Khartoum and its most populated city is Omdurman (part of the metropolitan area of Khartoum).
Islam was Sudan’s state religion and Islamic laws were applied from 1983 until 2020 when the country became a secular state. The economy has been described as lower-middle income and largely relies on agriculture due to long-term international sanctions and isolation, as well as a long history of internal instabilities, to some extent on oil production in the oil fields of South Sudan, Sudan is a member of the United Nations, the Arab League, African Union, COMESA, Non-Aligned Movement and the Organisation of Islamic Cooperation.
Health services in Sudan are provided by the Federal and State Ministries of Heath, military medical services, police, universities, and private sector. The districts or localities which are the closest to people are mainly pro Policies and plans in Sudan are produced at three levels federal, state, and district (also called locality) providing primary health care, health promotion, and encouraging community participation in caring for their health and surrounding environment. They are responsible for water and sanitation services as well. This well-established district system is a key component of the decentralization approach pursued in Sudan which gives in turn a broader space for local management, administration and allow for overcoming the leadership and supervision efforts by superior bodies.
There is one Federal Ministry of Health (FMOH) and 18 State Ministries of Health (SMOH). The federal level is responsible for provision of nation-wide health policies, plans, strategies, overall monitoring and evaluation, coordination, training, and external relations. The state level is concerned with state’s plans, strategies, and based on federal guidelines funding and implementation of plans. While the localities are mainly concerned with implementation and service delivery.
Source:https://en.wikipedia.org/wiki/Sudan
Kat and I intend for our exploration within the preterm birth community to exist on a solid foundation that recognizes, promotes, and celebrates collaboration. This month’s blog highlights the impact, necessity, and joy engagement in collaborative interaction provides. Wishing you joyful collaboration!
- “I can do things you cannot, you can do things I cannot: together we can do great things.”- Mother Teresa
- “When “I” is replaced by “we” even “illness” becomes “wellness”.-Scharf
- “It is amazing what you can accomplish if you do not care who gets the credit.”- Harry Truman

COMMUNITY

Fragile Infant and Family-Centered Developmental Care Evidence-Based Standards: The Value of Systems Thinking
Carol Jaeger, DNP, RN, NNP-BC, Carole Kenner, PhD, RN, FAAN, FNAP, ANEF

Abstract: Infant and Family-Centered Developmental Care (IFCDC) requires systems thinking – a re-examination of all the factors that interact to create/support the implementation of these care practices. This article will explore what systems thinking means and how it must be considered a cornerstone for implementing IFCDC.
Background: Systems thinking is a way to make sense of an institution’s or unit’s component parts, their intra- and interrelationship, and their function over time. It provides a process to explore those elements that contribute to an outcome.
In healthcare organizations, systems thinking is the big-picture view of the relationship between values, mission, infrastructure, education, practice, innovation, change, evaluation, and the sustainment of care over time. Further, systems thinking shows the factors that influence culture –the attitudes, relationships, and behavior – of the interprofessional staff, parents, and families. Consequently, the articulated values, mission, evidence-based education, practice, and change process guide the culture and, ultimately, the organization’s or unit’s operational practice.
The Infant and Family Centered Developmental Care (IFCDC) Consensus Committee has been using systems thinking to guide the implementation of IFCDC within the Intensive Care Unit. Assimilating the principles in the mission, vision, values, professional performance, education, clinical practice, continuous improvement process, and sustainment over the continuum of care and time is challenging in intensive hospital settings, at best. Since the onset of the pandemic, systems and systems thinking were, by necessity, interrupted. Implementing strict infection control practices has put limitations on staff, parents, and families access to the intensive care unit (ICU) and the associated disruption of consistent system-wide care practices. Parent and family member presence was severely restricted, personal contact and voice recognition was inadequate, appropriate communication with families was intermittent, and education for continuing care was limited. Relationships between staff and among staff and parents/family members were affected. The “normal” flow of activity was altered, and healthcare team members became siloed in their respective specialty roles and functions. Their interactions with each other and families were done individually and not as a team approach to care. The result was fragmented, often disjointed care approaches, where disciplinary views took precedence over a “big picture” holistic care effort.
In many, if not most, ICUs, the workforce was evaluated and limited to “essential staff” and practice. Continuous improvement processes were focused on safety occurrences; thus, practice improvement was curtailed. Consequently, operational budgets were reduced. Medical, nursing, and interprofessional student access to clinical experiences was eliminated in exchange for a simulation experience, or if clinical rotations did occur, the hospital staff acted as a preceptor instead of the usual clinical faculty. Healthcare interprofessional students graduated with limited patient/family contact.
Why are these changes important to IFCDC implementation from a systems perspective? Because these factors impact the unit’s system and culture of how care is provided. The focal point for care decisions moved from family-centered or baby-focused to one of staff availability and infection thwarting. The worst of the pandemic is over, yet the ramifications from a systems’ thinking view are not.
As the restrictions of the pandemic are released, the unit operational budgets are not as quick to rebound to pre-pandemic levels, and staff shortages across all healthcare professions are common. As new hires enter the workforce, they begin to practice with limited specialized clinical skills and likely little knowledge of IFCDC. They may have never experienced the family as an essential caregiver since entering the workforce. So, their worldview of what is “usual practice” is altered. Care is probably focused more on physical needs and not developmental support. Igniting the excitement for IFCDC practice – often viewed as “fluff” or nice but not necessary to care – is like starting over with the reluctance that comes with fear, apathy, and inertia. With the development of evidence-based standards, IFCDC is essential to care for the baby and family in intensive care, yet with the impact of the pandemic, there have been policy and practice changes that have impeded progress in their implementation.
Regardless of the experience and sensitive approach to the baby’s needs, healthcare staff cannot provide the connection of a parent. The baby’s need for neurophysiological and psychosocial support in the nurturing care of his/her parents is still essential. However, most importantly, staff need to comprehend and demonstrate competence in the skill of connecting and supporting the baby, parents, and family members. This relationship is the sustaining factor throughout the lifespan, and the foundation is established in intensive care. Systems thinking is essential to a leader’s assessment, planning, implementation, improvement, and continual monitoring of the mission, values, practice, outcome, and sustainment of a healthcare organization, an ICU, and thus is instrumental in affecting clinical care for babies and their families. As the pandemic recedes to an endemic, the interprofessional team and parents need to use systems thinking and a trusting, collaborative relationship to re-invest in the essential practice of infant and family-centered developmental care.
Source:nt-jul22.pdf (neonatologytoday.net)


Roaa Muhammad Naim – Asyad Al-Lawari – New Sudanese 2021 clips
12,357,089 views – Nov 26, 2020

رؤى محمد نعيم – اسياد اللواري – جديد الكليبات السودانية


Patterns and outcome of neonatal surgery in Sudan
Enas Ismail, A. Elnaeema, I. Salih Published 2019

Background: Sudan is one of the largest countries with a high birth rate (33.1/1000); with 40% of the population being children. Like many low income countries (LIC) neonatal surgery is overlooked, and for surgically affected neonates the situation is well below optimal. This study was conducted to determine the burden of neonatal surgery in Sudan and to find our own figures regarding patterns of disease and outcome. Patient and methodology: This is a prospective descriptive cross sectional hospital based study conducted over a six months period from July-December 2017 from five pediatric surgery units. Results: A total of 202 patients were studied. Males were predominant (54.5%) with a male to female ratio of 1.2:1. Most patients were term babies (78.2%) with normal body weight (2500-3000 g). One hundred thirty patients (64.4%) presented within the first week of life (mean 7.8±7.2). Ninety two percent of the diagnoses were congenital in origin. The most affected system was gastrointestinal (47.7%), but the most striking result is the high incidence of neural tube defects (26.2%). The most common acquired condition is NEC (3.5%). One hundred twenty two patients underwent surgical intervention, 12 of them needed a second intervention during neonatal period. Fifty nine patients (29.2%) needed surgical intervention but surgery was delayed (neural tube defects, HSD, and omphalocele). Fourteen percent of the population needed ICU admission , 6.5 % needed mechanical ventilation, and 12.2% needed TPN, the percentage of patients who actually received these services were (11%), (5%) and (2.5%) respectively. One fifth of the patients (20.8%) died during the study period with sepsis as a major cause of death. Bowel atresia is the most common diagnosis associated with mortality

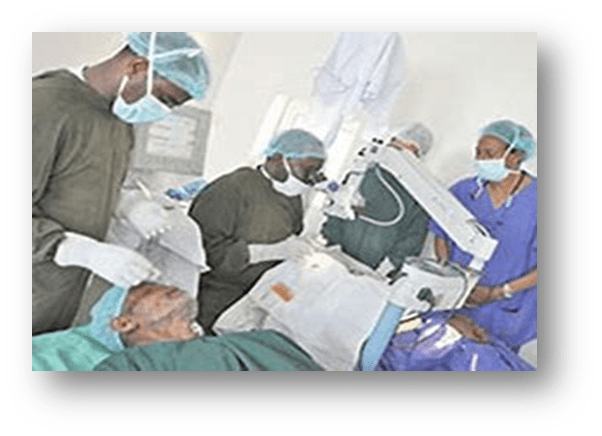
Using technology to promote safe maternal health practices in Nigeria
Using technology to promote safe maternal health practices in Nigeria

Summary
In sub-Saharan Africa, especially Nigeria, maternal and infant mortality remains a persistent and serious health challenge. Information and Communication Technology (ICT) interventions offer an effective approach to alleviate this challenge and improve health outcomes. From the experiences of health workers, this study found that using ICT to care for women during and after pregnancy increased the demand for health services and had a positive effect on maternal-infant deaths. It reaffirms that ICT tools (mobile phones, the Internet, television/digital video disk (DVD) and radio) are important for appointment reminders, communication of health tips and referrals of emergencies. Findings indicate that it is imperative to subsidise the cost of access, repackage messages in a language and style to suit mothers, and harmonise and integrate existing ICT-based projects for nationwide implementation in order to expand access and improve the care of women during and after pregnancy.
Background
The United Nations’ Sustainable Development Goal 3 (SDG 3) specifies the need to ensure healthy lives and promote well-being for all ages. Target 3.1 of the SDG specifically underscores the need to reduce the global maternal mortality ratio to less than 70 per 100,000 live births by 2030 from the 533 deaths per 100000 live births currently experienced in Sub-Saharan Africa. To realize this target, both improving access to health care and the use of Information Communication Technology (ICT) to communicate maternal health information have been found to be vital to place health information within reach of this vulnerable group, and therefore save lives. ICT has already proven efficient and valuable for disseminating information and delivering care services to patients in underprivileged groups. To maximize the gains of ICT for maternal and child health care (MCH), an in-depth understanding of the value of ICT tools, especially mobile phones, is imperative to improve practicability, acceptability and evaluation of such interventions.
Description of study
Having personally suffered a miscarriage and experienced complications at delivery, as well as watched mothers, gasp for breath in childbirth, the pain and misery of mother and infant death is deeply relatable and has inspired this field of inquiry.
The study identified and interviewed health care providers in nine clinics with ICT-based interventions for maternal and child health care in four Nigerian states (Ondo, Imo, Gombe and Kaduna.) The ICT-based interventions or projects for maternal and child health utilize ICT tools (like mobile phones , IPAD, computers) by health care providers to care for pregnant women and nursing mothers with their infants. Data collected were analysed using Nvivo (software program) to identify themes relevant to the objective of the study. The study was initiated in December 2018 and completed in August 2020.
This work is unique because previous Nigerian studies on ICT-based interventions for maternal and child health (MCH) explored the use of ICT mostly from the patient’s perspective. The views and experiences of health care providers in ICT-based projects for MCH add an important perspective of the value of ICT for MCH care; these multiple perspectives will be valuable to scale up existing health care models for ICT-based interventions targeted at pregnant women and mothers with infants.
This research is based on a solid foundation of literature from field practitioners on the use of ICT to reduce the mortality of mothers and their infants in Nigeria. The imperative to tackle this public health challenge is even more urgent in the pandemic and post-pandemic era, because ICT-enabled remote consultation, information dissemination and education enable less frequent visits to antenatal clinics, thus limiting exposure to infection and ensuring compliance with COVID-19 protocols. The use of ICT has been accelerated by COVID-19 in other sectors, including government, academia and business, to transact business, communicate, counsel, hold meetings and deliver lectures. Perhaps a silver lining of the pandemic may be increased investment in ICT by the government, the private sector and NGOs to accelerate the establishment of a robust ICT infrastructure and to strengthen the capacity of health workers to serve expectant mothers and their babies remotely.
Study outcomes
The average age of the participants was 45.6 yrs. Participants reported using mobile phones, the Internet, television/digital video disk (DVD), and radio to provide maternal health care. Other tools such as laptops/projectors for PowerPoint slides and public address systems were used during antenatal classes for maternal health education. The same ICT tools were also used for appointment reminders, communicating health tips, and referrals during emergencies. Participants reported challenges such as unreliable power supply, the cost of using ICT and irrelevant calls. Using ICT to care for women during and after pregnancy increased the demand for health services and a decrease in infant mortality In one clinic the turnout increased from 10 to 60 women going for antenatal service in a day which is attributed to an increase in awareness of health information and services provided at the clinic.
Participants (health care providers) report that the use of ICT tools made their jobs more interesting because of the association of ICT tools for patient care with advanced clinics. The health care providers also reported enhanced ability to promptly refer pregnant women and infants during emergencies – for example, one of the respondents highlighted a reduction in infant death within the first week of life noting that after the Safe Motherhood mhealth project was launched, the death of newborns within the first seven days of life had reduced. Using ICT tools for MCH care also encourages maternal health practices including the uptake of immunization and health facility utilisation.
The study synthesizes information from published literature and field practitioners to provide health care providers, designers of ICT-based interventions for MCH and policymakers data to inform design and formulate policies to expand and improve access to and delivery of care that can save the lives of mothers and infants.
Lessons
The major lesson from this study is that it is important to go beyond the perspective of patients to also capture the perspective of health services providers to design, implement, introduce, and evaluate ICT-based interventions. Harmonised and integrated ICT-based projects must be replicated nationwide to ptimize ICT in order to improve maternal and child health outcomes.
Impact
This study provides valuable information to formulate policy and fortify ICT use for maternal and child health care in low resource settings. It also promotes the adoption of healthy practices among pregnant women. The study has also led to my new research project, on communication design (styles, formats and languages) in maternal health for poor, illiterate mothers who often are excluded from e-health interventions for maternal health. Adaptation of e-health strategies for maternal and child health care must account for local context, addressing the views, needs and challenges of all stakeholders.
HEALTHCARE PARTNERS

No sonographer, no radiologist: New system for automatic prenatal detection of fetal biometry, fetal presentation, and placental location
Published: February 9, 2022 https://doi.org/10.1371/journal.pone.0262107

Abstract
Ultrasound imaging is a vital component of high-quality Obstetric care. In rural and under-resourced communities, the scarcity of ultrasound imaging results in a considerable gap in the healthcare of pregnant mothers. To increase access to ultrasound in these communities, we developed a new automated diagnostic framework operated without an experienced sonographer or interpreting provider for assessment of fetal biometric measurements, fetal presentation, and placental position. This approach involves the use of a standardized volume sweep imaging (VSI) protocol based solely on external body landmarks to obtain imaging without an experienced sonographer and application of a deep learning algorithm (U-Net) for diagnostic assessment without a radiologist. Obstetric VSI ultrasound examinations were performed in Peru by an ultrasound operator with no previous ultrasound experience who underwent 8 hours of training on a standard protocol. The U-Net was trained to automatically segment the fetal head and placental location from the VSI ultrasound acquisitions to subsequently evaluate fetal biometry, fetal presentation, and placental position. In comparison to diagnostic interpretation of VSI acquisitions by a specialist, the U-Net model showed 100% agreement for fetal presentation (Cohen’s κ 1 (p<0.0001)) and 76.7% agreement for placental location (Cohen’s κ 0.59 (p<0.0001)). This corresponded to 100% sensitivity and specificity for fetal presentation and 87.5% sensitivity and 85.7% specificity for anterior placental location. The method also achieved a low relative error of 5.6% for biparietal diameter and 7.9% for head circumference. Biometry measurements corresponded to estimated gestational age within 2 weeks of those assigned by standard of care examination with up to 89% accuracy. This system could be deployed in rural and underserved areas to provide vital information about a pregnancy without a trained sonographer or interpreting provider. The resulting increased access to ultrasound imaging and diagnosis could improve disparities in healthcare delivery in under-resourced areas.
Full Article: https://journals.plos.org/plosone/article?id=10.1371/journal.pone.0262107

Usefulness of the Parental Electronic Diary During Medical Rounds in a NICU
Taittonen L, Pärus M, Lahtinen M, Ahola J, Bartocci M. Usefulness of the Parental Electronic Diary During Medical Rounds in a NICU. J Perinat Neonatal Nurs. 2022 Jul-Sep 01;36(3):E7-E12. doi: 10.1097/JPN.0000000000000627. PMID: 35894731.

Parental involvement in the care of their baby in family rooms in neonatal intensive care units (NICUs) can be improved. This could be done with an electronic medical report completed by the parents, which is then linked to the patient record system. The parents selected for this study completed an electronic diary during their stay in the NICU, while the staff answered a questionnaire about their opinion on the usefulness of the parents’ diary. The length of stay, length of time the baby spent in Kangaroo care, breastfeeding, time given to breastfeeding, feeling of tiredness, the capability of identifying the newborn’s signals, and parents’ opinion on the diary were variables in the study. The NICU staff’s opinion about the usefulness of the diary in decision-making was sought using a questionnaire. Eleven mothers and three fathers completed the diary. The median time for staying in the ward was 20 hours/day. The median time in Kangaroo care was 3 hours/day. The majority of mothers were breastfeeding on average 5 times per day. The commonest length of time for breastfeeding was 1 to 2 hours/day. The parents felt somewhat tired during their stay. All parents recognized their child’s signals mostly or all the time. Most parents were happy with the diary. The nursing staff’s opinions on the usefulness of the diary too were uniformly positive, whereas the doctors’ opinions varied from positive to critical in nature. In conclusion, the diaries provided us with new information about parents’ perceptions in the NICU. The nurses found the diary useful whereas the doctors were more critical.
Source:https://pubmed.ncbi.nlm.nih.gov/35894731/

Midwives save lives in Sudan
02 July 2021- Anna Sambrook

Abstract
UK-based charity Kids for Kids is committed to upskilling midwives in Darfur, Sudan thus empowering women to provide safer care for mothers and babies in remote areas
Darfur, Sudan is one of the most deprived and impoverished areas in the world. The people here live lives of unimaginable hardship. At the forefront of climate change, flooding and droughts are a regular occurrence and now inflation is over 363% (Trading Economics, 2021), a result of the ongoing economic crisis. Families are struggling to feed their children and healthcare is a luxury not many people can afford, and in remote villages, it is unavailable. Rural hospitals have, at best, basic and little equipment. While living conditions have improved in other areas of the country, Darfur has been left behind.
Sudan has a Maternal Mortality Rate (MMR) of 295 deaths per 100 000 pregnancies (United Nations Population Fund, 2020), higher than the global average and staggeringly larger than the seven deaths per 100 000 recorded here in the UK. However, Darfur itself has one of the highest MMR rates in the world recording 727 deaths per 100 000 pregnancies in 2013 (Reliefweb, 2014). With Darfur mainly consisting of small, interspersed villages, the nearest hospital is usually several hours away, and can only be accessed via a donkey and cart, leaving many women at risk of death during childbirth from causes that could be prevented. The reason for this high number of maternal deaths is the lack of trained and skilled midwives in rural areas who are able to detect high-risk pregnancies. The most the majority of villages can hope for is an untrained traditional birth attender as there is no other healthcare available.
Kids for Kids has supported children and their families in Darfur for 20 years. By providing community led sustainable projects, Kids for Kids has adopted over 106 villages and helped over 550 000 people. It quickly became apparent to our Founder, Patricia Parker MBE, that something must be done to help expectant mothers in this area get access to trained medical care. Our health projects are a priority to the charity.
Therefore, Kids for Kids funds the training of two midwives from each village, in the regional capital El Fasher. We have also built a training school to enable 40 villages midwives to be trained. Once training is complete, we provide each midwife with leather sandals, a medical kit in a secure tin box to avoid contamination by insects in the desert, a mobile phone and strong cross-bred donkey, the main mode of transport in Darfur and the only way to cross the sand of the desert to reach her patients. A solar lantern is also provided, with no electricity supply in villages deliveries usually take place by the light of a fire.
Every 14 months, Kids for Kids trains 40 midwives. These women are then a beacon of hope to expectant mothers in their villages. They are trained to diagnose high-risk pregnancies, manage difficult births but also help to educate against female genital mutilation (FGM). Although this practice is now illegal in Sudan since 2020, the idea of FGM is ingrained culturally in many villages in Darfur and our midwives are trained to identify and report any instances they may come across. Because they are from the villages in which they work, mothers trust them and it is therefore much more likely that they will not ask to be resewn, or for their daughters to submit to the practise. Additionally, and an unexpected outcome for the charity, is that trained midwives are able to register births. This is inestimably important both for the individual and authorities. During the COVID-19 pandemic when people could not travel to El Fasher to register births, the Kids for Kids’ villages are unique in having births registered.
In the absence of healthcare in villages, and the danger of travel from the moment that conflict erupted in Darfur in 2003, Kids for Kids has also funded two first aid workers in each village. We also provide the drugs for a Revolving Drug Scheme in each community and train the midwives and first aid works in accountability and bookkeeping to enable them to run the scheme. They are overseen by committees we also train in each community and answer to the village as a whole at a review meeting each year.
Although there is an agreement with the State Ministry of Health to share the costs of training with Kids for Kids and to pay salaries once the midwives are trained, the Ministry has not had the funding to pay salaries for some time. Sudan is struggling with huge debts and is striving to recover from years of corruption and neglect by the previous regime. Expectant mothers therefore often pay village midwives in kind—from a chicken or a goat, to goat’s milk or seeds.
Where a village has been running the Kids for Kids’ projects well, they are able to request a health unit. To date, there are eight such brick-built units in our villages but many more are needed.
One of our midwives, Manal, was chosen by her village to undertake the training to become a midwife for her community. She graduated in 2018 and returned to her home village of Hashab Braka.
Manal delivered her first baby during the first week of her return. Since then, Manal delivers 4–5 babies every month in her village but her skills have been needed in the neighbouring villages where access to antenatal care is also limited. Because of her training, Manal now has the skills and confidence to identify difficult births and refers the mothers to the nearest health clinic in Mallit.
By becoming midwives, Manal and other women in Darfur are able to earn a living and are also given status in their communities. A lot of the work of Kids for Kids centres around empowering women and making sure they have a voice in their community.
To date, Kids for Kids have trained over 500 midwives, helping to deliver countless babies, and saving countless lives. Mothers are receiving proper healthcare and support, and maternal mortality rates are decreasing in the villages where we work.
While conditions improve in the villages we partner with, there are still thousands of women who still have no access to antenatal care in Darfur. As a result of the pandemic, many maternal health clinics in the towns closed across the country (United Nations Office for the Coordination of Humanitarian Affairs, 2021). We need to reach more women and we are only able to do so with the help from our supporters.

The benefits of agreeing on what matters most: Team cooperative norms mediate the effect of co-leaders’ shared goals on safety climate in neonatal intensive care units
Kuntz, Ludwig; Scholten, Nadine; Wilhelm, Hendrik; Wittland, Michael; Hillen, Hendrik Ansgar Health Care Management Review: 7/9 2020 – Volume 45 – Issue 3 – p 217-227 doi: 10.1097/HMR.0000000000000220

Abstract
Background:
Safety climate research suggests that a corresponding climate in work units is crucial for patient safety. Intensive care units are usually co-led by a nurse and a physician, who are responsible for aligning an interprofessional workforce and warrant a high level of safety. Yet, little is known about whether and how these interprofessional co-leaders jointly affect their unit’s safety climate.
Purpose:
This empirical study aims to explain differences in the units’ safety climate as an outcome of the nurse and physician leaders’ degree of shared goals. Specifically, we examine whether the degree to which co-leaders share goals in general fosters a safety climate by pronouncing norms of interprofessional cooperation as a behavioral standard for the team members’ interactions.
Methodology/Approach:
A cross-sectional design was used to gather data from 70 neonatal intensive care units (NICUs) in Germany. Survey data for our variables were collected from the unit’s leading nurse and the leading physician, as well as from the unit’s nursing and physician team members. Hypotheses testing at unit level was conducted using multivariate linear regression.
Results:
Our analyses show that the extent to which nurse–physician co-leaders share goals covaries with safety climate in NICUs. This relationship is partially mediated by norms of interprofessional cooperation among NICU team members. Our final model accounts for 54% of the variability in safety climate of NICUs.
Conclusion:
Increasing the extent to which co-leaders share goals is an effective lever to strengthen interprofessional cooperation and foster a safety climate among nursing and physician team members of hospital units.

What’s New in Practice Improvements in Neonatal Care?
Harris-Haman, Pamela DNP, APRN, NNP-BC; Section Editor Advances in Neonatal Care: August 2022 – Volume 22 – Issue 4 – p 281-282 doi: 10.1097/ANC.0000000000001025

In the Practice Improvements in Neonatal Care section of Advances in Neonatal Care (ANC), we encourage authors, novice as well as experienced, to share manuscripts that are fundamental to neonatal nursing practice. Let’s start with what is fundamental. What you do daily is fundamental to the care you provide to your patients?
Practice improvement and quality improvement are the “combined and unceasing efforts of everyone in the caregiving setting to make changes that will lead to better patient outcomes, better system performance, and better professional learning.1,2 This is the responsibility of all healthcare providers. One of which is you, each one of you.
Quality improvement can be related to new caregiving protocols you have learned or experienced. Questions you can ask your team are as follows: “What evidence has shaped the way you provide care?” “Have you made a recent change to your policies?” “What is your unit implementing that has benefited patients?” “What is your unit implementing that is unique, or not so unique, but has had a positive impact or unpredicted outcome?” “What is a concept or disease process that you have difficulty grasping?” “What better way to gain further understanding of that disease process than to write about it?” Educating each other is a fantastic way to learn ourselves, actually one of the best. This means content within this section is not limited to what is defined as solely a quality improvement initiative. Any topic that is fundamental to neonatal intensive caregiving is suitable for this section of the journal.
As nurses we are constantly mindful of safety risks, how to minimize these risks, and prevent errors or events from occurring. Nurses are uniquely positioned to anticipate potential events1 (you know that gut feeling). Who better to provide information to our profession than the nursing providers at the bedside? We need to ask whether this is the best we can do? Is this practice or caregiving protocol in the context of person-centered care and are the experiences of the neonates and their parents used to guide how the practice is implemented. It is important to remember that real outcome measures in healthcare are not what immediately happens but what the neonates and their family experiences over the course of their life because of their time spent in the neonatal intensive care unit (NICU).
Numerous quality improvement initiatives have been developed in the NICU setting. Some of these topics are as follows:
- Pain assessment
- Reduction of central line–associated bloodstream infections (CLABSIs)
- Prevention of sepsis
- Prevention of necrotizing enterocolitis (NEC)
- Hand hygiene
- Mother–infant interactions
- Human milk nutrition
- Prevention of unplanned extubations
- Management of bronchopulmonary dysplasia (BPD)
- Prevention and management of hypothermia
- Magnetic resonance imaging without sedation
- Use of music therapy3
In addition, there are many processes that take place on an hourly, daily, and weekly basis that require standardization, care bundles, checklists, or even pathophysiological explanations relating to their use and development.1 There are diverse topics that you can share your learned experiences on:
- Improving our practice, by providing general information updates, reviews of the pathophysiology of a disease process, pharmacology principles of a specific medication, or pathophysiology of a certain disease process.
- Concept analysis of ideas central to neonatal nursing. You may have written one of these during your educational endeavors. To be publishable, you need to make sure the concept analysis is applicable in the real world.
- Clinical excellence related to specific problems. What has your unit been doing well that had had a positive effect on patient outcomes or that has positively affected parental satisfaction or participation.
- Descriptions of essential nursing care strategies for specific diagnosis.
- Neonatal concepts that pertain to all levels of nursing from the novice to the expert or targeted to a specific audience such as the new staff nurse or the advanced practice nurse.
- Quality improvement projects that promote practice and process improvement.
- Neonatal assessment processes.
Consider your own units. What is occurring that concerns you? What has been helpful? Look at the effects of the implementation of new care bundles, new equipment, new staffing models, or environmental issues. Work with the unit leadership when something new is implemented in your unit, equipment, practice bundle, or medication. Have you initiated a new task force? Document the effects of this practice. As NICU care provider, you are uniquely positioned to have a positive and lasting effect on the care provided in your institution. Share this with your colleagues. Pat yourselves on the back for the outstanding work you do and care you provide to our tiny patients and their families.
We want to use this section of ANC to capture the excellence of neonatal care that you are providing. Your unique educational and experiential viewpoints and your lived experiences are valuable. We look forward to reading your manuscripts. Many resources are available to assist you on this quest. These are in your units, hospitals, national associations, and this editorial board. Share your knowledge with our readers so that they may gain new knowledge that will enrich and expand their clinical knowledge and continue to improve the care we provide for our tiny precious patients.

Less Invasive Surfactant Delivery Works for Tiniest Newborns
Less requirement for mechanical ventilation adverse in very preterm infants by James Lopilato, Staff Writer, MedPage Today August 9, 2022
For extremely preterm infants with potential respiratory distress syndrome, less invasive surfactant administration (LISA) was associated with a significant decrease in the risk of adverse outcomes, a cohort study found.
There was a drop in requirement for invasive mechanical ventilation between those infants receiving LISA within the first 72 hours of life and those who didn’t (53.6% vs 8.3%), according to the study of over 6,500 infants in Germany.
Often performed early in the delivery room, LISA was safe and associated with decreased risks during the child’s primary stay in hospital:
- All-cause death (adjusted OR 0.74, 95% CI 0.61-0.90)
- Bronchopulmonary dysplasia (BPD; adjusted OR 0.69, 95% CI 0.62-0.78, P<0.001)
- BPD or death (adjusted OR 0.64, 95% CI 0.57-0.72, P<0.001)
Babies undergoing LISA also showed reductions in pneumothorax and retinopathy of prematurity, Christoph Härtel, MD, from University Hospital of Würzburg in Germany, and colleagues reported in JAMA Network Open.
LISA comprises less invasive delivery of surfactant to babies in respiratory distress. Important concepts of LISA include delayed cord clamping, facilitated fetal transition, initial continuous positive airway pressure support, maintenance of spontaneous breathing, caffeine administration, and early skin-to-skin contact, according to Härtel’s team.
The authors noted that LISA had been found to be beneficial for respiratory outcomes in earlier studies. Theirs may be the first large-scale report in “the most vulnerable preterm population,” however.
Last year’s OPTIMIST-A trial showed a nonsignificant trend of better survival in infants born at 25 to 28 weeks who received surfactant treatment.
Härtel and colleagues based their observational cohort study on the German Neonatal Network of 68 tertiary level neonatal ICUs. Infants born from 22 weeks 0 days to 26 weeks 6 days of gestation between April 2009 and December 2020 were eligible.
Data were collected from 6,542 infants (mean gestational age 25.3 weeks, 53.7% boys). Of these newborns, 38.7% received LISA.
Outcomes were adjusted for gestational age, small-for-gestational-age status, sex, multiple birth, inborn status, antenatal steroid use, and maximum fraction of inspired oxygen in the first 12 hours.
Nevertheless, some potential confounders may have been missed by the study authors.
They also acknowledged the potential for indication bias and selection bias, as well as the possibility that LISA does not avoid mechanical ventilation in some babies. “There is still an urgent need to better define those babies at high risk for failing a treatment strategy that includes LISA.”
Randomized clinical trials are needed to assess the effects of prophylactic LISA on vulnerable preterm infants, Härtel’s team suggested.
Less Invasive Surfactant Delivery Works for Tiniest Newborns | MedPage Today

Predictors of extubation success: a population-based study of neonates below a gestational age of 26 weeks
2022 – Ohnstad MO, Stensvold HJ, Pripp AH On behalf of the Norwegian Neonatal Network, et al, Predictors of extubation success: a population-based study of neonates below a gestational age of 26 weeks; Correspondence to Dr Mari Oma Ohnstad; mari.oma.ohnstad@ldh.no On behalf of the Norwegian Neonatal Network

Abstract
Objective The aim of the study was to investigate first extubation attempts among extremely premature (EP) infants and to explore factors that may increase the quality of clinical judgement of extubation readiness.
Design and method A population-based study was conducted to explore first extubation attempts for EP infants born before a gestational age (GA) of 26 weeks in Norway between 1 January 2013 and 31 December 2018. Eligible infants were identified via the Norwegian Neonatal Network database. The primary outcome was successful extubation, defined as no reintubation within 72 hours after extubation.
Results Among 482 eligible infants, 316 first extubation attempts were identified. Overall, 173 (55%) infants were successfully extubated, whereas the first attempt failed in 143 (45%) infants. A total of 261 (83%) infants were extubated from conventional ventilation (CV), and 55 (17%) infants were extubated from high-frequency oscillatory ventilation (HFOV). In extubation from CV, pre-extubation fraction of inspired oxygen (FiO2) ≤0.35, higher Apgar score, higher GA, female sex and higher postnatal age were important predictors of successful extubation. In extubation from HFOV, a pre-extubation FiO2 level ≤0.35 was a relevant predictor of successful extubation.
Conclusions The correct timing of extubation in EP infants is important. In this national cohort, 55% of the first extubation attempts were successful. Our results suggest that additional emphasis on oxygen requirement, sex and general condition at birth may further increase extubation success when clinicians are about to extubate EP infants for the first time.

PREEMIE FAMILY PARTNERS

Building Confidence and Parenting Skills When Your Baby Is in the NICU
Nursing License Map / Building Confidence and Parenting Skills When Your Baby Is in the NICU November 23, 2020
Having a child in the neonatal intensive care unit (NICU) can be a frightening or overwhelming experience for parents. As your newborn receives lifegiving support from NICU equipment and trained professionals, you may struggle to step into your role as parent or feel fearful, helpless or uncertain.
Understanding the inner workings of the NICU and connecting with the support available to families can help you gain confidence, find ways to participate and become an advocate for yourself and your baby. Learn more through the resources below.
Tips for Parents on Building Caregiving Skills With a NICU Baby
Understand your rights as the parent, including what you can ask for and expect during your baby’s stay; the NICU Baby’s Bill of Rights can be a useful resource.
Practice providing routine care for your baby, including changing clothes and giving baths; let your neonatal nurse practitioner or other provider know if and when you are ready to learn these skills.
Take care of your baby’s laundry if time allows; some parents say taking their baby’s clothes home to wash and bring back to the NICU helps them feel more involved.
Be present for feeding and bath times when possible, and collaborate with your nurse on participating.
Reach out to the lactation consultant if available at your hospital to create a plan for feeding your baby at home.
Choose the pediatrician who will help care for your baby after the NICU.
Notify your insurance provider to add your baby onto your policy.
COMMON TERMS TO KNOW IN THE NICU
Common Terms | Nationwide Children’s: Glossary of NICU-related terms organized alphabetically covering NICU equipment, procedures and health indicators.
Glossary of NICU Terms for Parents | National Perinatal Association (PDF, 568.65 KB): Glossary of neonatal terms organized by category, including the NICU team and medications used in the NICU.
Premature Birth: Diagnosis & Treatment | Mayo Clinic: An explanation of tests given to premature babies and treatment options available, including surgery, medication and specialized supportive care.
NICU Staff | March of Dimes: Descriptions of 29 types of staff members who may work in your hospital’s NICU and their roles.
GAINING CONFIDENCE IN THE NICU
- Caring for a Premature Baby: What Parents Need to Know | American Academy of Pediatrics
- How You Can Participate in the Care of Your Baby in the NICU | American Academy of Pediatrics
- When Your Baby’s in the NICU | KidsHealth
Support Resources for NICU Parents and Loved Ones
FEEDING (NICU AND BREASTFEEDING, BOTTLE FEEDING AND FORMULA)
Breastfeeding | Office on Women’s Health: A landing page for information on breastfeeding, including breastfeeding positions and guidance on pumping and storing milk.
Breastfeeding in the NICU: Advice from a Lactation Consultant | Hand to Hold: Practical advice for women breastfeeding premature babies and suggestions for loved ones to offer support.
Feeding Difficulties & Your Preemie | Hand to Hold: Information on feeding disorders and feeding therapy that a premature baby may need in their first days and months.
Feeding Your Baby After the NICU | March of Dimes: Answers to commonly asked questions about feeding preemies after a NICU stay, such as how to know when your baby is full and where to find support.
Feeding Your Baby in the NICU | March of Dimes: Description of feeding options for babies in the NICU, including breastfeeding, bottle, a feeding tube or intravenous line (IV).
Find a Lactation Consultant Directory | International Lactation Consultant Association: Online listings of board-certified lactation consultants and services offered, fees and medical coverage information.
How to Bottle Feed a Preemie | Verywell Family: Six tips for bottle feeding a premature baby, offered by a registered nurse in a tertiary-level NICU.
La Leche League Online Support Resources | LLLI: A landing page of breastfeeding resources available online for families around the world, including virtual support groups, publications and printable toolkits.
Nourishing Your Premature Baby in the NICU | Hand to Hold: An article from a neonatal registered dietitian on the feeding and growing processes unique to premature infants.
Practical Bottle Feeding Tips | American Academy of Pediatrics: Eight tips for safely and successfully bottle feeding an infant.
FINDING COMMUNITY AND SUPPORT
Blogs for NICU Parents | National Perinatal Association: List of blogs written by and for parents in the NICU.
For Our Families | Hand to Hold: A landing page of resources for families in the NICU that includes private Facebook communities, counseling services, bereavement support and information on requesting a peer mentor.
Four Ways Preemie Moms Can Say “No Thanks” to Visitors | Preemie Mom Camp: A blog post with advice on declining visitors in the NICU or at home, including sample scripts.
Get Help | La Leche League International (LLLI): Searchable map for finding a local support group with La Leche League, an international organization supporting breastfeeding mothers.
The MyPreemie App for Preemie Parents | Graham’s Foundation: A free app to help parents organize their calendar, track their baby’s progress and create a virtual baby book; available on the App Store and Google Play.
Where to Find Peer-to-Peer Support | National Perinatal Association: A list of organizations that connect families in the NICU or transitioning home with peers who can offer support.
AFTER THE NICU: GOING HOME
Home After the NICU | March of Dimes: Guidance for parents on the emotional experience of transitioning home, sleep safety, childcare and vaccinations.
Parents Corner: Information That Gives the Support You Need in the NICU | Baby First: Parents’ stories on transitioning home from the NICU and information on what to expect after discharge.
Resources at Home | Nationwide Children’s: A collection of articles on caring for your infant at home and knowing when to call a provider; topics range from burn prevention and infant cardiopulmonary resuscitation (CPR) to fever and fussiness.
Taking Your Preemie Home | KidsHealth: Advice for parents on preparing for discharge from the NICU, safety precautions to take once home and suggestions for self-care.
Transitioning Newborns from NICU to Home | Agency for Healthcare Research and Quality: Collection of fact sheets for families bringing a NICU baby home; topics covered include signs of illness, managing breathing problems, medication safety, immunization schedule and many more.
NICU AND INSURANCE
Affording the NICU: 6 Ways to Reduce the Cost | Hand to Hold: Description of financial safety nets available to help parents of premature babies pay for a NICU stay.
Get Help Paying Your Baby’s Hospital Bills | Verywell Family: Information about the possible costs of a NICU visit for families with and without insurance.
Health Insurance for Your Family | March of Dimes: A guide to understanding health insurance coverage for children under the Affordable Care Act (ACA).
Insurance for Newborns: Four Lessons From $27,000 Bill | CoPatient: An article about one family’s story with medical bills in the NICU and their suggestions for new parents navigating the NICU experience.
Paying for Your Baby’s NICU Stay | March of Dimes: Guidance for parents on the NICU and insurance coverage and questions to ask your health insurance representative to learn more.
NICU CLOTHES FOR BABIES, SUPPLIES AND BLANKETS
The Best Preemie Clothes for Extra Tiny Babies | What to Expect: Suggestions for where to buy premature baby clothes and accessories that are both comfortable and affordable.
Knitting Tips and Patterns for Preemies | The Spruce Crafts: Guidelines for knitting items for NICU babies, including patterns for socks, caps and baby blankets.
Knots of Love NICU Blanket Patterns | Knots of Love: Crochet and knit patterns for baby blankets specially made for neonatal babies.
Navigating the NICU: What to Bring to the NICU (Printable Checklist) | UnityPoint Health: A packing list for the NICU including clothes for both parents and babies, bedding, toiletries, entertainment and other essentials.
NICU PARENTS’ WELL-BEING
One in 10 New Dads Gets Postpartum Depression. Here’s How to Spot It (and Stop It). | Men’s Journal: An article on postpartum depression presenting in fathers and ways to offer support.
Postpartum Depression | Office on Women’s Health: Resources on postpartum depression in mothers and common types of treatment.
Postpartum Skincare | Lucie’s List: Recommendations for skincare after pregnancy and while breastfeeding, plus nursing-safe options.
Postpartum Support: Your New Life as a Parent | Lucie’s List: Encouragement for new mothers in managing the transition into parenthood and finding professional support when needed.
Self-Care for Parents | Program for Early Parent Support: A list of ideas for parents to meet their own physical, emotional, social and intellectual needs.
Share Your Story | March of Dimes: A landing page for March of Dimes’ blogs, forums and member groups that help parents make connections and find support.
Straight Talk | Lucie’s List: A collection of articles on the challenges of parenting babies and young children, from breastfeeding and sleep regression to tantrums and going back to work.
Taking Care of You: Support for Caregivers | KidsHealth: Tips on recharging and reaching out for help for parents of children with a serious illness.
Your Mental Health and Well-Being Are Important! | National Perinatal Association: A screening questionnaire for postpartum mental health conditions and resources for help with anxiety, depression and post-traumatic stress disorder (PTSD), among others.
RETURNING TO WORK AND CHILDCARE
Daycare and the Prematurity Factor | Hand to Hold: A discussion of the benefits and drawbacks of different childcare options specifically for preemies.
Finding Child Care for Your Premature Baby | Verywell Family: A consideration of care options for premature babies, including a stay-at-home parent, family caregivers, nannies and au pairs, home childcare and daycare.
Finding Childcare for Your Preemie | Graham’s Foundation: Advice for making childcare arrangements for preemies and their unique needs.
Going Back to Work After a Loss | Share: Ten practical suggestions to help grieving parents ease back into the workplace.
Going Back to Work After a Pregnancy Loss | Harvard Business Review: An article on the challenges that bereaved parents face in returning to work, with self-care strategies and advice for managers and colleagues.
Resources for Friends and Family
Loved ones can play an important role in helping NICU parents transition into their new roles. Read more in the resources below about supporting parents of neonatal infants during and after a NICU stay.
- 10 Ways to Support a Friend with a Baby in the NICU | Today’s Parent
- 10 Ways to Help NICU Parents | Seleni
- 27 Ways to Help Parents With Children in the NICU | The Mighty
- Unique Ways to Support NICU Parents: Ideas for a NICU Care Basket | Hand to Hold
The resources in this article are for informational purposes only; individuals should consult with a licensed health care provider before taking action.
Last Updated: December 2020
Source:https://nursinglicensemap.com/blog/parents-of-baby-in-nicu/

The Wisdom of Trauma, Official Trailer with Dr. Gabor Maté
Jul 19, 2020 Science and Nonduality
This website has been translated in the following languages: عربى, България, čeština, Deutsch, Français, עִברִית, Italiano, Lietuviškai, Magyar, Polskie, Português, Türkçe and subtitled in 27 languages.
Watch the movie at https://thewisdomoftrauma.com/ The film is available by donation.
*************************************************************
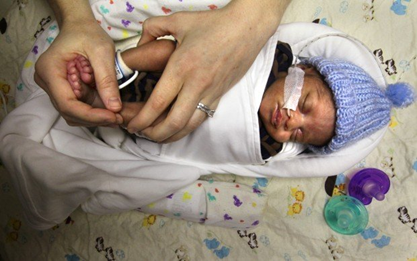
Welcoming a new life – Physical therapies for premature baby
KK Women’s and Children’s Hospital – Jun 23, 2020
When a baby is born more than three weeks earlier than the expected delivery date, the baby is referred to as ‘premature’ or “preemie”. Premature babies are at risk of developmental delay as their brains and bodies have to continue to grow rapidly in an external environment, outside of the mother’s womb. The Physiotherapist will assess and review your child regularly to ensure that your baby is developing appropriately for his/her age. Physiotherapists will also be available to assist you with learning how to handle and interact with your baby. Upon discharge, Physiotherapists will continue to monitor your child’s neurological and developmental progress until at least 18 months corrected age when he/she may then continue with therapy or be discharged, depending on his/her needs at that stage.

5 Tips to Support you Dad, in the NICU
Jun 15, 2022 CanadianPreemies

INNOVATIONS
Associations Between Prenatal Urinary Biomarkers of Phthalate Exposure and Preterm Birth A Pooled Study of 16 US Cohorts
Barrett M. Welch, PhD1; Alexander P. Keil, PhD2; Jessie P. Buckley, PhD3; et alAntonia M. Calafat, PhD4; Kate E. Christenbury, MBA5; Stephanie M. Engel, PhD2; Katie M. O’Brien, PhD1; Emma M. Rosen, MSPH2; Tamarra James-Todd, PhD6; Ami R. Zota, ScD7; Kelly K. Ferguson, PhD1; and the Pooled Phthalate Exposure and Preterm Birth Study Group JAMA Pediatr. Published online July 11, 2022. doi:10.1001/jamapediatrics.2022.2252

Key Points
Question Is phthalate exposure during pregnancy associated with preterm birth?
Findings In this pooled analysis of 16 studies in the US including 6045 pregnant individuals, phthalate metabolites were quantified in urine samples collected during pregnancy. Higher urinary metabolite concentrations for several prevalent phthalates were associated with greater odds of delivering preterm, and hypothetical interventions to reduce phthalate exposure levels were associated with fewer preterm births.
Meaning In this large observational study, urinary biomarkers of common phthalates used in consumer products were a risk factor for preterm birth.
Abstract
Importance Phthalate exposure is widespread among pregnant women and may be a risk factor for preterm birth.
Objective To investigate the prospective association between urinary biomarkers of phthalates in pregnancy and preterm birth among individuals living in the US.
Design, Setting, and Participants Individual-level data were pooled from 16 preconception and pregnancy studies conducted in the US. Pregnant individuals who delivered between 1983 and 2018 and provided 1 or more urine samples during pregnancy were included.
Exposures Urinary phthalate metabolites were quantified as biomarkers of phthalate exposure. Concentrations of 11 phthalate metabolites were standardized for urine dilution and mean repeated measurements across pregnancy were calculated.
Main Outcomes and Measures Logistic regression models were used to examine the association between each phthalate metabolite with the odds of preterm birth, defined as less than 37 weeks of gestation at delivery (n = 539). Models pooled data using fixed effects and adjusted for maternal age, race and ethnicity, education, and prepregnancy body mass index. The association between the overall mixture of phthalate metabolites and preterm birth was also examined with logistic regression. G-computation, which requires certain assumptions to be considered causal, was used to estimate the association with hypothetical interventions to reduce the mixture concentrations on preterm birth.
Results The final analytic sample included 6045 participants (mean [SD] age, 29.1 [6.1] years). Overall, 802 individuals (13.3%) were Black, 2323 (38.4%) were Hispanic/Latina, 2576 (42.6%) were White, and 328 (5.4%) had other race and ethnicity (including American Indian/Alaskan Native, Native Hawaiian, >1 racial identity, or reported as other). Most phthalate metabolites were detected in more than 96% of participants. Higher odds of preterm birth, ranging from 12% to 16%, were observed in association with an interquartile range increase in urinary concentrations of mono-n-butyl phthalate (odds ratio [OR], 1.12 [95% CI, 0.98-1.27]), mono-isobutyl phthalate (OR, 1.16 [95% CI, 1.00-1.34]), mono(2-ethyl-5-carboxypentyl) phthalate (OR, 1.16 [95% CI, 1.00-1.34]), and mono(3-carboxypropyl) phthalate (OR, 1.14 [95% CI, 1.01-1.29]). Among approximately 90 preterm births per 1000 live births in this study population, hypothetical interventions to reduce the mixture of phthalate metabolite levels by 10%, 30%, and 50% were estimated to prevent 1.8 (95% CI, 0.5-3.1), 5.9 (95% CI, 1.7-9.9), and 11.1 (95% CI, 3.6-18.3) preterm births, respectively.
Conclusions and Relevance Results from this large US study population suggest that phthalate exposure during pregnancy may be a preventable risk factor for preterm delivery.
Source: https://jamanetwork.com/journals/jamapediatrics/article-abstract/2794076

New target for therapies to treat preterm labour
August 9, 2022

Researchers have identified a cause of premature (preterm) labour, an enigma that has long challenged researchers. New research published in The Journal of Physiology suggests a protein, called Piezo1, is responsible for regulating the behaviour of the uterus. Piezo1 keeps the uterus relaxed ensuring that it continues to stretch and expand during the 40 weeks it takes a foetus to grow.
Preterm birth is the single biggest cause of neonatal mortality and morbidity in the UK. Every year around 60,000 babies are born prematurely in the UK. The identification of Piezo1 in the uterus, and its role to maintain relaxation of uterus through stretch-activation during pregnancy, paves the way for drugs and therapies to be developed that could one day treat or delay preterm labour.
The muscular outer layer of the uterus is peculiar because it is the only muscle that it is not regulated by nerves and it must remain dormant for the 40 weeks despite significant expansion and stretch as the foetus develops into a baby. The researchers from University of Nevada USA studied tissue samples of the smooth muscle of the uterus to explore the mechanistic pathways to better understand the dynamics controlling the uterus, how pregnancy is maintained and what maintains quiescence until labour.
Stretching the uterus tissue, to mimic what happens during pregnancy, activates Piezo1 channels. This drives the flow of calcium molecules generating a signalling cascade that activates the enzyme nitric oxide synthase to produce the molecule nitric oxide. This Piezo1 cascade promotes and maintains the dormant state of the uterus.
Piezo1 controls the uterus by working in a dose-dependent manner, where channel activity is stimulated by the chemical Yoda1 and inhibited by a chemical called Dooku1. When Piezo1 is upregulated, the uterus remains in a relaxed state. However, in preterm tissue, the expression of Piezo1 is significantly decreased (downregulated), which ‘switches off’ the dormant signalling to the muscle, so the uterus contracts and initiates labour.
Professor Iain Buxton, Myometrial Research Group at the University of Nevada USA said,
“Pregnancy is the most impressive example of a human muscle enduring mechanical stress for a prolonged period. Finding Piezo1 in the muscular layer of the uterus means the uterus is controlled locally and is coordinated by a stretch-activated mechanism rather than hormonal influence from the ovaries or the placenta, which has been the assumption.
“It is troubling that there are still no drugs available to stop preterm labour. Thanks to the Nobel Prize winning discovery of Piezo proteins, which are responsible for how the body responds to mechanical force, and our investigation we are now closer to developing a treatment. Piezo1 and its relaxation mechanism provide a target for us which we could potentially activate with drugs. We need to test this with further studies and we hope to carry out clinical trials in the future.”
Contraction and relaxation were assessed in tissue samples compared for the following gestational periods: non-pregnant, term non-labouring, term labouring, preterm non-labouring and preterm labouring. The presence of Piezo1 channels was discovered using molecular tools while pregnant tissues contracting in a muscle bath were stimulated with Piezo1 channel activator and inhibitor to characterize the regulation of quiescence.
More research is needed to improve our understanding of how all the molecular signals and steps involved in the Piezo1 channel regulate the relaxation of the uterus and whether more chemicals are working together with Piezo1.
Full paper title: Novel Identification and Modulation of the Mechanosensitive Piezo1 Channel in Human Myometrium. Link to paper https://physoc.onlinelibrary.wiley.com/doi/10.1113/JP283299
New target for therapies to treat preterm labour – The Physiological Society (physoc.org)




These 14 innovations are enabling young people to address their mental health needs
May 23, 2022 World Economic Forum

The World Economic Forum is the International Organization for Public-Private Cooperation. The Forum engages the foremost political, business, cultural and other leaders of society to shape global, regional and industry agendas. We believe that progress happens by bringing together people from all walks of life who have the drive and the influence to make positive change
Fun for the little ones!
African Animals for Children with pronunciation (and videos)

Welcome to the world of African animals! Learn with your children and students the names of African animals. Children will travel through this virtual safari by discovering Savannah African animals in English in a playful and entertaining way while seen moving, listening to the name in English with pronunciation and reading how to write.

Diving Sudan
This video was made during a live aboard in the Red Sea of Sudan with Red Sea Explorers. During the nine days of diving we visited the following dive site’s: – Shaab Ambar – Protector Reef – Karam Masamirit – Ed Domesh – Habili gab Miyum 1 – Dahrat Abid – Habili gab Miyum 2 – Dahrat Qab – Tamarsha – Pinnacolo – Shaab Jumna – Saganeb – Shaab Rumi – Umbria



