ALGERIA

RATE: 7.4 Estimated number of preterm births per 100 live births RANK: 147
(US Rate: USA – 12% Rank: 54)
SOURCE: https://www.marchofdimes.org/mission/global-preterm.aspx
Algeria, officially the People’s Democratic Republic of Algeria is a country in the Maghreb region of North Africa. The capital and most populous city is Algiers, located in the far north of the country on the Mediterranean coast. With an area of 2,381,741 square kilometres (919,595 sq mi), Algeria is the tenth-largest country in the world, and the largest in Africa.[12] Algeria is bordered to the northeast by Tunisia, to the east by Libya, to the west by Morocco, to the southwest by the Western Saharan territory, Mauritania, and Mali, to the southeast by Niger, and to the north by the Mediterranean Sea. The country is a semi-presidential republic consisting of 48 provinces and 1,541 communes (counties). It has the highest human development index of all non-island African countries.
Health: In 2002, Algeria had inadequate numbers of physicians (1.13 per 1,000 people), nurses (2.23 per 1,000 people), and dentists (0.31 per 1,000 people). Access to “improved water sources” was limited to 92% of the population in urban areas and 80% of the population in the rural areas. Some 99% of Algerians living in urban areas, but only 82% of those living in rural areas, had access to “improved sanitation”. According to the World Bank, Algeria is making progress toward its goal of “reducing by half the number of people without sustainable access to improved drinking water and basic sanitation by 2015”. Given Algeria’s young population, policy favors preventive health care and clinics over hospitals. In keeping with this policy, the government maintains an immunization program. However, poor sanitation and unclean water still cause tuberculosis, hepatitis, measles, typhoid fever, cholera and dysentery. The poor generally receive health care free of charge.
SOURCE: https://en.wikipedia.org/wiki/Algeria
Kat and I were not able to find preterm birth stories to share from Algeria but we did find a very fun love ![]() song by Algerian Mok Saib that we are choreographing for a Zumba routine. The beauty of Love and the Zumba community is the recognition and celebration of the oneness of our global family and how our Love for each other has the power to enrich our lives and nourish the planet we live on. A little Music Therapy we can all enjoy!
song by Algerian Mok Saib that we are choreographing for a Zumba routine. The beauty of Love and the Zumba community is the recognition and celebration of the oneness of our global family and how our Love for each other has the power to enrich our lives and nourish the planet we live on. A little Music Therapy we can all enjoy!
Mok Saib – Je M’en Fous – موك صايب [Clip Officiel]
48,867,679 views Published on Jan 26, 2018

COMMUNITY
Most Pervasive Major Diseases in Algeria and their Prevention
June 2017
With 40 million citizens, Algeria is the largest country in Africa, and for the past 40 years, its government has worked hard to improve health care by providing it for free to its citizens. Free health care in Algeria is funded by taxes, social security and economic growth. It has helped millions of Algerians, providing medical care and services to extend the lives of millions. Early intervention through infant vaccines, for instance, has prevented many major diseases in Algeria.
The free system remains lacking. A shortage of doctors means that people seeking medical treatment have long waits and sometimes do not receive proper screening that might prevent curable diseases.
The Algerian government recently passed a new health care bill to improve access for the poor, provide patient e-files to better access medical records, and help in the detection and care of disease. The bill added programs to facilitate organ transplants, tissue and cell transplants and treatments for infertility.
Early detection is key to improving the lives of millions of citizens, as many of the major diseases in Algeria are treatable. Others are preventable. Here are the most major diseases in Algeria, according to the Institute for Health Metrics and Evaluation:
- Coronary artery disease and coronary heart disease, also known as ischemic heart disease, which results in a reduced blood supply to the heart.
- Cerebrovascular disease, which affects blood flow to the brain and may cause strokes. High cholesterol is a leading cause of cerebrovascular disease. Cholesterol drugs are expensive in Algeria. Ministers of health since 2002 have tried to lower the cost of these drugs by allowing local pharmaceutical companies to open and manufacture cost-efficient medication.
- Neonatal preterm birthis another medical issue that causes multiple medical issues and death. Infants born earlier than 37 weeks are considered preemies. Babies born this early are susceptible to heart and lung issues and permanent disabilities including cerebral palsy, blindness, deafness and learning disabilities. Some learning disabilities can not be detected until the child reaches school age.
- Prenatal education can help prevent and improve the chances of full-term births. Some risks that can cause premature birth if left untreated are high blood pressure and diabetes. Early intervention increases the odds that a baby will be born healthy.
- Diabetes is among the major diseases in Algeria. This silent and sometimes debilitating illness, which can result in blindness, loss of limbs and death, can be treated, and certain diabetes drugs are being produced locally. Proper nutrition and exercise can help prevent diabetes.
- Congenital anomalies result in the deaths of children within the first month of life, according to the World Health Organization. Those babies who survive will need long-term medical care. Proper diet, prenatal vitamins, vaccines and early screenings can help. Prenatal care has increased over the last several years in Algeria with improved health care.
- Chronic kidney diseaseis another slow, progressive disease that results in the need for long-term medical care. Medication alone is not enough for the treatment of this disease. In severe cases, people need to go on kidney dialysis to help filter their blood. This process is both painful and expensive. With early monitoring of diabetes and high blood pressure, kidney disease can sometimes be prevented.
- Alzheimer’s disease is another growing issue in Algeria. There is some early treatment medicine on the market today, but such treatment can only slow down the illness. Alzheimer’s is a growing concern as life expectancy rises in Algeria. The progression of Alzheimer’s diseaseis very slow, causing memory loss and dementia. As the disease worsens, people suffering forget all sense of themselves and their loved ones. People with Alzheimer’s eventually lose the ability to care for themselves in the most basic of functions. People with Alzheimer’s eventually need long-term care, which can put a strain on family and caregivers. There has been an increase in privately-owned nursing homes in Alegria. An estimated 250 nursing homes have opened up thus far, with more expected in the future.
SOURCE: https://borgenproject.org/major-diseases-in-algeria/
Global Coalition calls for better care and stronger legislation to save babies on the brink of death
PTBi-CA Contributes to Major Global Report Urging Specialized Treatment for Premature Infants–December 12, 2018
We are thrilled to have participated in a major global report that recognizes, for the first time, the essential role of parents as partners in the care of sick and small babies throughout every recommendation. The report, Survive and Thrive: Transforming care for every small and sick newborn, was created by UNICEF and WHO, with support from partners including USAID, Every Preemie Scale, Save the Children, LSHTM, and the Gates Foundation. PTBi co-principal Investigator, Linda Franck, contributed to the landmark technical report and explains, “This report could impact our ability to double-down on our efforts to reduce disparities in access and quality of care for all babies needing special care at birth to reduce the unacceptable rates of death and disability worldwide. Transforming care for today’s 30 million vulnerable newborns is the smartest investment we can make in our future.” According to the report, the world will not achieve the global target to achieve health for all unless it transforms care for every newborn. Without rapid progress, some countries will not meet this target for another 11 decades. To save newborns, the report recommends:
- Providing round-the-clock inpatient care for newborns seven days a week.
- Training nurses to provide hands-on care working in partnership with families.
- Harnessing the power of parents and families by teaching them how to become expert caregivers and care for their babies, which can reduce stress, help babies gain weight and allow their brains to develop properly.
- Providing good quality of care should be a part of country policies, and a lifelong investment for those who are born small or sick.
- Counting and tracking every small and sick newborn allows managers to monitor progress and improve results.
- Allocating the necessary resources, as an additional investment of US$ 0.20 cents per person can save 2 of every 3 newborns in low- and middle-income countries by 2030.
Almost three decades ago, the Convention on the Rights of the Child guaranteed every newborn the right to the highest standard of health care, and it is time for countries around the world to make sure the legislative, medical, human and financial resources are in place to turn that right into a reality for every child, the report says.
SOURCE: https://pretermbirthca.ucsf.edu/news/ptbi-ca-contributes-major-global-report-urging-specialized-treatment-premature-infants
University of California San Francisco – Who We Are 
Mission: Our mission is to eliminate racial disparities in preterm birth and improve health outcomes for babies born too soon, through research, partnerships and education grounded in community wisdom.
Vision: We believe all parents deserve healthy pregnancies, and all newborns deserve healthy starts in life.
People: The California Preterm Birth Initiative lives at the intersection of research, community partnerships and education to create positive change for black and brown families. The UCSF California Preterm Birth Initiative is an innovative, multi-year research enterprise funded by Lynne and Marc Benioff. We’re led by Principal Investigator Larry Rand and co-Principal Investigator Linda Franck. Our community advisory boards help to determine our research priorities.
We’re a community of researchers, parents, lactation consultants, doulas, nurses, doctors, community practitioners, public servants and innovative thinkers determined to change this persistent and urgent issue. Our work in California is based in Oakland, Fresno and San Francisco. Our sister project is the East Africa Preterm Birth Initiative.
What We are Facing: More than one-third of infant deaths in California are related to being born too soon, and babies born prematurely who do survive can face a lifetime of health complications. The stark reality of premature birth in California is one of health inequity. While 1 in 12 babies are born too soon, the rate of preterm birth among Black women is 47 percent higher than the rate among all other women. We assert that structural and interpersonal racism along with other key social determinants are important drivers of an epidemic that disproportionately affects women of color in our state, and nationally.
Our Role: Our work is deeply rooted in place, drawing strength from and developing capacity with our academic and community partners in Fresno, Oakland, and San Francisco. We strive to address questions that have been prioritized by women with lived experience of preterm birth and vetted by our community advisory boards.
SOURCE: https://pretermbirthca.ucsf.edu/news/ptbi-ca-contributes-major-global-report-urging-specialized-treatment-premature-infants

We spent some time today on the University of Washington Campus where the Cherry Blossoms are in Bloom and Love and Renewal are in the air. We sprinkled a few pictures from our wander throughout the blog. Spring in the Northwest is finally here! Let’s celebrate!

PREEMIE FAMILY PARTNERS
Lullaby-Playing Pacifier Helps Premature Babies Thrive UCLA Health Newsroom
 UCLA Health Published on Feb 11, 2019
UCLA Health Published on Feb 11, 2019
Babies who are born premature often struggle with feeding and the reflex to suck, breathe and swallow, which is pivotal for their development. And when parents watch their premature newborns in the neonatal intensive care unit (NICU), they often feel helpless. Now, researchers with the music therapy program at UCLA Mattel Children’s Hospital are testing whether an unusual device, which plays a lullaby recorded by the baby’s parents when a baby successfully sucks on the connected pacifier, can empower parents by helping them bond with their babies — and strengthen the babies by improving their oral abilities, which play a crucial role in the ability to feed. A family with triplets participated in the research and used the pacifier-activated lullaby (PAL) device to aid in their babies’ development.
Learn more about the music therapy program at : https://ucla.in/2lrCgoz

Forgotten fathers: New dads also at risk for postpartum depression
Study provides an in-depth look at new fathers’ experiences with PPD Date: March 7, 2019 Source: University of Nevada, Las Vegas
Summary: A new study offers an in-depth view of new fathers’ experiences with postpartum depression (PPD). The study explores issues they encounter and how they can move beyond barriers they face in receiving diagnoses and treatment of the little-known phenomenon.
It’s increasingly common to hear about new moms suffering from the baby blues. But what about new dads?
A new UNLV study, published last week in the Journal of Family Issues, offers an in-depth view of new fathers’ experiences with postpartum depression (PPD). The study explores issues they encounter and how they can move beyond barriers they face in receiving diagnoses and treatment of the little-known phenomenon.
Between 5 and 10 percent of new fathers in the United States suffer from PPD, according to U.S. Centers for Disease Control and Prevention data. One study shows that the risk goes up to 24 to 50 percent for men whose partners suffer from PPD.
A team of researchers, led by UNLV Couple and Family Therapy professor Brandon Eddy, scoured blogs, websites, forums, and chat rooms for first-hand accounts from new dads. Six themes emerged:
- Needing education. Fathers didn’t know men could suffer from PPD and were surprised to learn others experienced it. Women who saw PPD in men were unsure of what to call it. Men complained about pushback or not receiving information from doctors or therapists, or frustration that the PPD resources they did manage to find focused solely on how to help their wives.
- Adhering to gender expectations. Many dads felt pressured to espouse traditional “tough guy” stereotypes. In fact, one man who told another father to “suck it up” said he knew it was bad advice but explained that it’s what’s expected of men.
- Repressing feelings. Men were reluctant to share their feelings for fear of sounding ridiculous or looking weak to their wives, who were the primary caregivers.
- Overwhelmed. Many of the new dads found it difficult to express their emotions of confusion, exhaustion, helplessness, loneliness, and feeling trapped. Parents often suffer from lack of sleep after birth, which can exacerbate stress and depressive symptoms — making them more irritable to their children’s crying.
- Resentment of baby. While many fathers expressed joy and excitement for the arrival of their children, others resented their baby’s constant needs and attention. A few talked about suppressing urges to hurt the baby or themselves.
- Experience of neglect. The dads felt lost, forgotten, and neglected — by their wives, the health care system, and society. One father described “uncomfortably laughing” while reading PPD screening questions typically asked of women during routine checkups: “I began to feel like someone should be asking me the same questions.” Another said men, who must simply wait while women do the hard work of pregnancy and labor and lack an umbilical cord connection to their children, had often shared with him similar stories of struggling with PPD: “There’s no truly acceptable place or context for men to publicly reveal being challenged — much less rocked to the core — by what I call ‘sudden parenthood’.”
Overall, the findings complement previous studies on barriers for fathers suffering from PPD. UNLV researchers said encountering a lack of information and stigma often causes dads to distance themselves from their child and has been associated with marital difficulties.
Previous research elsewhere has found that paternal involvement has many positive outcomes for children, such as boys displaying less hostile behavior then children with absent dads, reduced delinquency for both sexes, considerably higher IQ scores for children in their early development years, and lower levels of emotional distress. That’s on top of studies showing fathers who suffer from PPD report lower levels of communication with their partners, as well as increased rates of substance abuse and domestic violence.
“The expectations society gives to men of what they are supposed to be, what they are supposed to do, and how they do it was a significant factor on how many of these men chose to cope with life stressors,” the UNLV researchers wrote.
“Because men are already less likely than women to seek professional help for depression, it is vital that the stigma of PPD decreases,” they added. “Because paternal involvement is a significant factor in the healthy development of children, it would seem wise to make information about paternal PPD more available in order to combat its negative impact on families.”
The U.S. Preventative Services Task Force — an independent coalition of national experts — recently recommended that all women be screened for depression before and after giving birth. There is no current assessment designed to specifically screen men for PPD.
“With the vast amount of research conducted on the importance of paternal involvement and the rising rates of PPD in fathers,” researchers wrote, “it seems logical that fathers should also be included in this recommendation.”
Story Source:Materials provided by University of Nevada, Las Vegas. Original written by Keyonna Summers. Note: Content may be edited for style and length.
Journal Reference:Brandon Eddy, Von Poll, Jason Whiting, Marcia Clevesy. Forgotten Fathers: Postpartum Depression in Men. Journal of Family Issues, 2019; 0192513X1983311 DOI: 1177/0192513X19833111
 (SOURCE: https://newsroom.uw.edu/postscript/lullabies-soothe-nicu-babies-and-parents-too)
(SOURCE: https://newsroom.uw.edu/postscript/lullabies-soothe-nicu-babies-and-parents-too)
Lullabies soothe NICU babies, and parents, too
UW MEDICINE/NEWSROOM – March 20, 2019-
Research suggests that parents singing to their children actually lowers blood pressure and helps neural development.
Shannon Turner said that even humming to his daughter, Kassie, seems to calm her.
Shannon Turner claims he can’t carry a tune. His preemie daughter seems to disagree.
Although she’s only 32 weeks old and weighs 3 pounds, Kassie Turner has made her preferences known: When her dad, Shannon, sings in his gravelly baritone, or even hums, her heart rate and blood pressure drop. This simple act soothes Shannon, too.
“I’ve noticed when I’m here, and I start to hum, whether she’s getting her nose mask readjusted (to help her breathe) or her diaper changed, it helps calm her down,” he said.
Lullaby writing and singing give Turner and his wife Danielle a way to bond with Kassie, and to center themselves when their circumstances feel unmanageable. They arrived Feb. 5 at UW Medical Center’s Neonatal Intensive Care Unit (NICU), with Danielle experiencing superimposed preeclampsia, a condition caused by hypertension. Kassie was born that same day, two months early, at 28 weeks.
A few weeks later, UW Medicine’s neurologic music therapist Gayle Cloud appeared, asking if they’d like to create a custom lullaby. She began offering music therapy in the hospital’s NICU four years ago, and has adapted everything from Dave Matthews tunes to standards like “Twinkle, Twinkle, Little Star.”
They chose the melody of “Jesus Loves Me” to reflect their faith and, with Cloud’s help, crafted lyrics to fit their family, adding the names of Kassie’s three siblings into the chorus.
Creating a lullaby is more than a distraction for stressed parents. The positive effects of singing to newborns, especially premature infants, is well-established in the medical community. A 2013 study showed that music decreases the stress response and helps babies devote more energy to neural and other development. The choice of the song didn’t seem to matter, according to the study. Other observations indicate music aids babies’ sucking responses and oxygen saturation.
Cloud has lost track of the number of families she’s worked with. The diversity of new parents has enabled Cloud to facilitate lullabies in French and Spanish, and even to transform Korean melodies.
“The moms will often tell me they don’t have a singing voice,” she said. “But I always say that the baby loves your voice, no matter what you sound like. Your baby has heard your voice all throughout your pregnancy while in the womb.”
The best music for a baby is live music sung in person by mom or dad, Cloud noted. Live music allows the music therapist and parents to match babies’ mood or heart rate, slowing or softening the lullaby in the moment. Recordings are more difficult to modulate rhythm and volume.
“I thought it was great that we could create this,” Danielle Turner said as Kassie, wrapped in a furry pink snuggly, cooed in her arms. “She will not only have this lullaby in the NICU, but it is something she can treasure for the rest of her life.”
For details about this story or UW Medical Center’s music therapy program, contact Barbara Clements: bac60@uw.edu, 206.221.6706.
SOURCE: https://newsroom.uw.edu/postscript/lullabies-soothe-nicu-babies-and-parents-too
 Bill and Melinda Gates Center/UW Washington Campus-Innovation in Process!
Bill and Melinda Gates Center/UW Washington Campus-Innovation in Process!
INNOVATIONS

![]()
Scientists gain new insight on triggers for preterm birth
University of Texas Medical Branch at Galveston-February 12, 2019
Summary:
A group of scientists have gained new insight on a poorly-understood key player in the timing of labor and delivery. This new information brings scientists closer to being able to prevent preterm births.
A group of scientists led by Ramkumar Menon at The University of Texas Medical Branch at Galveston have gained new insight on a poorly-understood key player in the timing of labor and delivery. This new information brings scientists closer to being able to prevent preterm births. This study is in Scientific Reports.
According to the World Health Organization, an estimated 15 million infants are born too early each year. Complications from preterm birth are the leading cause of death among children under five years old, responsible for about one million deaths each year globally. In the U.S., approximately 1 of every 10 infants was born prematurely in 2017.
When a woman is at the end of her pregnancy, the normal childbirth process begins when the fetus releases chemicals signaling that his/her organs have matured enough for delivery. This chemical release shifts the mother’s hormone levels, which increases inflammation in the uterus and begins labor and delivery.
“There’s another component of the biological clock that contributes to the timing of birth — a type of cell-to-cell communication between the maternal and fetal cells called paracrine signaling,” said senior author Menon, UTMB associate professor in the department of obstetrics and gynecology. “Because little is known about what this type of signaling does during pregnancy, we investigated the role of paracrine signals called exosomes in the timing of labor and delivery.”
The researchers collected blood plasma samples from pregnant mice and isolated the exosomes. Exosomes collected during either early or late pregnancy were injected into a separate group of pregnant mice during the human equivalent of the beginning of the third trimester.
“We showed that injecting a high concentration of late pregnancy exosomes was able to cause labor-associated changes without the other hormonal and chemical triggers usually involved in this process. Injections of the early pregnancy exosomes had no effect,” said Menon. “This shows that exosomes play a more important role in labor and delivery that has never been reported before.”
UTMB’s Samantha Sheller-Miller, the primary author of this work, conducted the animal model experiments that produced this novel finding. Other authors include UTMB’s Jayshil Trivedi as well as Steven Yellon from Loma Linda University.
Story Source: Materials provided by University of Texas Medical Branch at Galveston.
SOURCE: https://www.sciencedaily.com/releases/2019/02/190212120108.htm
 HEALTH CARE PARTNERS
HEALTH CARE PARTNERS 
 New research identifies potential PTSD treatment improvement-
New research identifies potential PTSD treatment improvement-
University of Texas at Austin – March 18, 2019
 Regions of the brain associated with stress and posttraumatic stress disorder. Credit: National Institutes of Health Researchers may have found a way to improve a common treatment for post-traumatic stress disorder (PTSD) by changing how the brain learns to respond less severely to fearful conditions, according to research published in Journal of Neuroscience.
Regions of the brain associated with stress and posttraumatic stress disorder. Credit: National Institutes of Health Researchers may have found a way to improve a common treatment for post-traumatic stress disorder (PTSD) by changing how the brain learns to respond less severely to fearful conditions, according to research published in Journal of Neuroscience.
The study by researchers at The University of Texas at Austin Dell Medical School suggests a potential improvement to exposure therapy—the current gold standard for PTSD treatment and anxiety reduction—which helps people gradually approach their trauma-related memories and feelings by confronting those memories in a safe setting, away from actual threat.
In a study of 46 healthy adults, researchers compared participants’ emotional reactions to replacing an unpleasant electric shock on the wrist with a surprise neutral tone, instead of simply turning off the shocks. Omitting the feared shocks is the current norm in exposure therapy. The participants’ brain activity was measured by functional magnetic resonance imaging (fMRI). Their emotional reactions were measured by how much they were sweating from their hands.
Compared with simply turning off the shocks, replacing the feared shocks with a neutral tone was associated with stronger activity in the ventromedial prefrontal cortex—an area critical for learning safety and inhibiting fear. Replacing the feared shock with a simple tone also lowered participants’ emotional reactions to pictures that previously had been associated with the electric shock when participants were tested the next day.
“This simple treatment of replacing an expected threat with an innocuous sound resulted in a long-lasting memory of safety, which suggests that the brain may be able to better control its fear response by means of a pretty straightforward, nonpharmaceutical intervention,” says lead study author Joseph Dunsmoor, Ph.D., an assistant professor in the Department of Psychiatry at Dell Medical School.
In the study, Dunsmoor’s team randomly divided participants to two groups—those who had the shock turned off and those who had the shock replaced by a neutral tone. Both groups were exposed to a picture of a face paired with an electric shock on the wrist on day one of the study. The groups were then exposed to the pictures with the shock turned off, or with the shock replaced by the surprising tone. Both groups returned the next day to measure brain activity and emotional reactions to the fear-conditioned pictures.
The researchers measured participants’ brain activity to the fear-conditioned pictures using fMRI scans. They also measured participants’ emotional responses to the threat of receiving an electric shock based on the amount of sweat recorded from a hand.
“It is well known that the brain learns by surprise,” says Dunsmoor. “Our study suggests that replacing expected aversive events with neutral and unexpected events, even a simple tone, is one way to capture attention so that the brain can learn to regulate fear more effectively.”
More information: Joseph E. Dunsmoor et al, Role of human ventromedial prefrontal cortex in learning and recall of enhanced extinction, The Journal of Neuroscience (2019). DOI: 10.1523/JNEUROSCI.2713-18.2019
Journal information: Journal of Neuroscience
SOURCE:https://medicalxpress.com/news/2019-03-potential-ptsd-treatment.html

Sensors are first to monitor babies in the NICU
 NorthwesternU Published on Feb 28, 2019
NorthwesternU Published on Feb 28, 2019
No wires, more cuddles: Sensors are first to monitor babies in the NICU without wires: Soft, flexible sensors provide clinical-grade measurements, allow physical bonding between baby and parent
An interdisciplinary team has developed a pair of soft, flexible wireless sensors that replace the tangle of wire-based sensors that currently monitor babies in hospitals’ neonatal intensive care units and pose a barrier to parent-baby cuddling and physical bonding. After completing a series of human studies, the researchers concluded that the wireless sensors provided data as precise and accurate as that from traditional monitoring systems.
SOURCE: https://www.sciencedaily.com/releases/2019/02/190228141243.htm
A Friend of ours, a great Nurse and a fellow Zumba instructor, recently posted about her visit to a local retreat center that provides Health Professional Programs, Wellness Programs, Cancer Retreats, etc. within our local community. Harmony Hill Healing Retreat seeks to transform lives within our Healthcare community as they “ help physicians, nurses, social workers and other clinicians – as well as entire workplace teams — enhance their own resilience and wellbeing”. If You know of similar programs where you live please share the information with your community as we reach out to support our Healthcare Partners!
PROGRAM LINK: https://www.harmonyhill.org/programs/

![]()
Association of Nurse Workload With Missed Nursing Care in the Neonatal Intensive Care Unit (Abstract)
Heather L. Tubbs-Cooley, PhD, RN1,2; Constance A. Mara, PhD3,4; Adam C. Carle, MA, PhD4,5,6; et alBarbara A. Mark, PhD, RN7; Rita H. Pickler, PhD, RN8
January 2019 – A Pediatr. 2019;173(1):44-51. doi:10.1001/jamapediatrics.2018.3619
Key Points-
Question Does the workload of neonatal intensive care unit nurses influence the likelihood that a nurse will miss necessary care for assigned infants?
Findings In this study of 136 nurses caring for 418 infants during 332 shifts, increased infant-to-nurse ratio during a shift was associated with increased missed nursing care in about half of the measured missed care items. When a measure of subjective workload was considered, the associations of ratios were mostly attenuated; increased subjective workload was consistently associated with increased missed care.
Meaning Focusing exclusively on infant-to-nurse ratios to address missed care may be limiting; nurses’ subjective workload is typically unmeasured but has promise for tailored workload interventions.
Abstract-
Importance Quality improvement initiatives demonstrate the contribution of reliable nursing care to gains in clinical and safety outcomes in neonatal intensive care units (NICUs); when core care is missed, outcomes can worsen.
Objective To evaluate the association of NICU nurse workload with missed nursing care.
Design, Setting, and Participants A prospective design was used to evaluate associations between shift-level workload of individual nurses and missed care for assigned infants from March 1, 2013, through January 31, 2014, at a 52-bed level IV NICU in a Midwestern academic medical center. A convenience sample of registered nurses who provided direct patient care and completed unit orientation were enrolled. Nurses reported care during each shift for individual infants whose clinical data were extracted from the electronic health record. Data were analyzed from January 1, 2015, through August 13, 2018.
Exposures Workload was assessed each shift with objective measures (infant-to-nurse staffing ratio and infant acuity scores) and a subjective measure (the National Aeronautics and Space Administration Task Load Index [NASA-TLX]).
Main Outcomes and Measures Missed nursing care was measured by self-report of omission of 11 essential care practices. Cross-classified, multilevel logistic regression models were used to estimate associations of workload with missed care.
Results A total of 136 nurses provided reports of shift-level workload and missed nursing care for 418 infants during 332 shifts of 12 hours each. When workload variables were modeled independently, 7 of 12 models demonstrated a significant worsening association of increased infant-to-nurse ratio with odds of missed care (eg, nurses caring for ≥3 infants were 2.51 times more likely to report missing any care during the shift [95% credible interval, 1.81-3.47]), and all 12 models demonstrated a significant worsening association of increased NASA-TLX subjective workload ratings with odds of missed care (eg, each 5-point increase in a nurse’s NASA-TLX rating during a shift was associated with a 34% increase in the likelihood of missing a nursing assessment for his or her assigned infant[s] during the same shift [95% credible interval, 1.30-1.39]). When modeling all workload variables jointly, only 4 of 12 models demonstrated significant association of staffing ratios with odds of missed care, whereas the association with NASA-TLX ratings remained significant in all models. Few associations of acuity scores were observed across modeling strategies.
Conclusions and Relevance The workload of NICU nurses is significantly associated with missed nursing care, and subjective workload ratings are particularly important. Subjective workload represents an important aspect of nurse workload that remains largely unmeasured despite high potential for intervention.
https://jamanetwork.com/journals/jamapediatris/article-abstract/2714281

The preterm heart: a unique cardiomyopathy?
Pediatric RESEARCH – Published: 19 January 2019 Adam J. Lewandowski
Preterm birth affects ~10% of births worldwide. Due to current advances in perinatal clinical care, survival rates >90% are regularly achieved for preterm neonates, meaning the population of adults born preterm has risen sharply in recent decades. Consequently, the first opportunities to assess longer-term disease risk of modern cohorts of smaller, more developmentally immature preterm-born survivors are only just emerging. Epidemiological studies have now identified preterm birth as an independent risk factor for cardiovascular disease, including hypertension, atrial fibrillation, stroke, and early heart failure. This increased risk is believed to be partly due to disrupted organ development as a result of an early transition from a lower resistance placental circulation during foetal development to a higher resistance arterial circulation postnatally, which is exacerbated by preterm-related complications. In line with an increased cardiovascular risk, studies using cardiovascular magnetic resonance (CMR) imaging in young adults born preterm were the first to show that they have potentially adverse alterations in both left ventricular (LV) and right ventricular (RV) structure and function. More recent studies have demonstrated that the early postnatal period may be a key developmental window during which these cardiac geometric and functional changes first emerge.
In this issue of Pediatric Research, Cox et al. provide further, detailed insight into the remodelling pattern of the preterm heart during the critical postnatal window. Thirty-four preterm infants underwent CMR scans of the LV and RV within the first week following delivery (postnatal age 3–7 days) and 29 were scanned again at term-corrected age (postnatal age 33–136 days; 37–42 weeks’ corrected gestational age). Ten term-born controls underwent the same CMR scan protocol at a single time point (postnatal age 2–7 days). The authors showed that preterm-born individuals had significantly elevated weight-indexed LV mass and LV end-diastolic volume (EDV) at term-corrected age. Furthermore, weight-indexed RV mass and RVEDV trended towards being greater in the preterm group at term-corrected age, which reached statistical significance in the cohort born at 29–32 weeks’ gestational age. Cox et al. used the CMR scans in order to create computational atlases of the LV and RV from end-diastolic phases, demonstrating that preterm hearts have a more globular LV shape with more spherical blood pool. Interestingly, the degree of prematurity, requirement for respiratory support >48 h and the administration of antenatal glucocorticoids were all independently correlated with increased LV wall thickness in the preterm-born infants.
In humans, the heart undergoes substantial remodelling over the first days and weeks of postnatal life, with the RV switching from being a thick-walled chamber that provides two-thirds of cardiac output into the systemic circulation to being the relatively thinner walled, crescent-shaped chamber that supplies the lower pressure pulmonary circulation. Although follow-up of the preterm cohort in the study by Cox et al. was at term-corrected age (37–42 weeks’ corrected gestational age), there was large variation in postnatal age for their second scans (33–136 days). We and others have shown that the LV and RV in both preterm-born and term-born individuals undergoes extensive cardiac remodelling postnatally, thus additional follow-up in the term-born group after several weeks of exposure to the extrauterine environment using the same methodology would be required to fully understand differences in physiological adaptation related to birth gestational age. Nevertheless, Cox et al.’s findings related to ventricular volumes in the preterm group at term-corrected age may be a reflection of the further enhanced physiological adaptation to increased pulmonary venous return in those born at earlier gestations. Given that LV and RV volumes are reduced in those born preterm in childhood and young adulthood, the current study highlights the need for longitudinal cardiac imaging studies tracking the same individuals over time to better understand the evolution of these remodelling patterns throughout development.
Cardiac changes in preterm-born individuals are of clinical concern. In longitudinal studies, the 20% increase in LV mass seen in young adults born moderately preterm based on CMR imaging is equivalent to >50% increased risk of cardiovascular clinical events in later adult life. The 64% increase in LV mass seen in those born at less than 29 weeks’ gestation in the study by Cox et al. is therefore of particular concern if these changes track throughout development. The nature of this myocardial thickening remains to be determined, but animal studies of preterm suggest that both cardiomyocyte hypertrophy and fibrosis are early pathophysiological adaptations, even in the absence of the normal inflammatory and stress signals present in human preterm pregnancies. Studies have also identified that RV systolic function is reduced from early in life,4 with clinically significant reductions in young adulthood that may directly contribute to the onset of clinical heart failure. Indeed, Carr et al. have demonstrated in a large Swedish register-based epidemiological study of 2.67 million individuals that those born preterm are at increased risk of incident heart failure from childhood through to young adulthood, with a fourfold increased risk in those born at 28–31 weeks’ gestation (very preterm) and 17-fold increased risk in those born at <28 weeks’ gestation (extremely preterm). Given the absolute number of incident heart failures was still greater in those born at term, this may be due to the altered myocardial development in those born preterm, as a reduced myocardial reserve would make them more susceptible to acute insults commonly causing early heart failure. In accordance with this hypothesis, we recently demonstrated using echocardiography imaging at prescribed exercise intensities that preterm-born young adults have impaired LV functional response to physical exercise. Additionally, using right heart catheterisation, Goss et al. demonstrated that young adults born preterm were significantly less able to augment cardiac index or right ventricular stroke work during exercise. Despite the independence of the changes in LV and RV structure and function from blood pressure, exposure to the known sustained blood pressure elevation, hypertension and other cardiovascular risk factors in preterm-born individuals might have a greater impact over time in these individuals due to this abnormal pattern of cardiac remodelling and reduced myocardial reserve.
The findings from Cox et al. and others have demonstrated the importance of this early postnatal window for growth, development and cardiac remodelling in preterm infants. As such, it may be an ideal period for intervention to prevent future risk of cardiovascular disease. In a hyperoxia-exposed rat model mimicking preterm birth-related stress conditions, early treatment with an angiotensin II type 1 (AT1) receptor antagonist, Losartan, prevented the development of cardiac alterations in later life, including fibrosis and hypertrophy. These findings suggest that intervention in the first days and weeks postnatally can alter the long-term course of cardiac disease risk. Though humans are more likely to be faced with a greater number of confounding variables and environmental factors affecting development and risk throughout life, our previous work has shown the possible benefits of intervention during the early postnatal window using a more practical approach for human infants. By performing a follow-up study in a cohort of preterm-born young adults who had been randomised to different milk feeding diets at birth between 1982–1985, we were able to investigate the potential long-term cardiac remodelling benefits of an exclusive human milk diet in immediate preterm postnatal life. We performed detailed cardiac phenotyping using CMR imaging and computational cardiac atlas formation to explore cardiac remodelling patterns in young adulthood. Comparison of young adults who were fed exclusively human milk versus those who were fed exclusively on formula as infants revealed that the LV and RV end-diastolic and stroke volumes in the group fed exclusively human milk approached values seen in term-born controls, with particularly striking findings for the RV. The findings implicate early preterm postnatal life as a potentially tractable period of cardiovascular development, relevant to long-term outcomes, and support promotion of human milk for the care of preterm infants to reduce long-term cardiovascular risk. Future work is needed to understand potential benefits of different variations of supplemental feeding and fortifiers to support normal growth and development in very and extremely preterm-born neonates. Furthermore, whether other interventions during the perinatal period or throughout life, such as pharmacological and prescribed dietary and exercise advice, can help preferentially reduce adverse cardiac remodelling in preterm-born individuals remains to be determined but should be a primary focus of current research in the field.
In conclusion, Cox et al. provide further evidence of a unique cardiac phenotype in offspring born preterm and should be commended for their sophisticated methodological approach using CMR and cardiac atlas formation in neonates and infants to better define these patterns of geometric remodelling. The increasing body of evidence from animal models and humans born preterm demonstrating a unique cardiac morphology and abnormal functional stress response provides mechanistic insight to the findings from epidemiological studies. On the whole, this supports the notion that being born preterm is associated with a unique cardiomyopathy. Understanding which individuals born preterm are at greatest risk and what leads to the heterogeneity in the preterm cardiac phenotype remains to be further explored, but immediate consideration for long-term clinical cardiovascular follow-up in preterm-born individuals is warranted.
Pediatric RESEARCH: Aims and scope of journal
Pediatric Research publishes original translational research papers, invited reviews, and commentaries on the etiologies and treatment of diseases of children and disorders of development, extending from basic science to epidemiology and quality improvement
SOURCE:https://www.nature.com/articles/s41390-019-0301-3
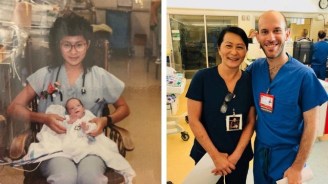
WARRIORS:
Nurse realizes she cared for doctor when he was a preemie baby in the NICU
 By: Shelby Lin Erdman, Cox Media Group National Content Desk – Updated: Sep 5, 2018 – 11:41 AM
By: Shelby Lin Erdman, Cox Media Group National Content Desk – Updated: Sep 5, 2018 – 11:41 AM
Nurse realizes she cared for doctor when he was a preemie baby in the NICU
PALO ALTO, Calif. – A nurse at Lucile Packard Children’s Hospital in Palo Alto, California, had a heartwarming reunion with a premature baby she helped care for when he returned to the hospital as a pediatric resident 28 years later. Probably the most unusual part of the story, though, is Vilma Wong actually remembered Brandon Seminatore and recognized his name
“His last name sounded very familiar,” Wong told the Mercury News.
Seminatore, a second-year pediatric resident, was in the Neonatal Intensive Care Unit about three weeks ago, according to a post on the hospital’s Facebook page, when Wong asked him who he was.
“I kept asking where he was from and he told me that he was from San Jose, California, and that, as a matter of fact, he was a premature baby born at our hospital. I then got very suspicious because I remember being the primary nurse to a baby with the same last name,’’ Wong told the newspaper.
Wong asked if his father was a police officer, and after a stunned silence, Seminatore asked if she was Vilma.
The young resident said he was shocked when he realized Wong was the primary care nurse who helped keep him alive all those years ago. “Meeting Vilma was a surreal experience,” he said in a hospital statement. “When Vilma recognized my name, it truly sunk in that I was one of these babies. I’ve come full-circle and I’m taking care of babies with the nurse that took care of me.”
Seminatore weighed just 2 pounds and 6 ounces when he was born by emergency C-section at 29 weeks gestation in 1990 and spent 40 days in the NICU, according to hospital officials.
Seminatore immediately alerted his parents, who had attended annual NICU reunions at the hospital over the years, that he had run into Wong. Seminatore’s mother, Laura Seminatore, called Wong and her colleagues “the most wonderful nurses,” and told the Mercury News “they helped calm a lot of fears.”
Her son said he realized after meeting her how much dedication and love Wong has for her career.
“She cares deeply for her patients, to the point that she was able to remember a patient’s name almost three decades later. Not all of us will get the chance to see our patients grow up, and I was so happy to be able to share that moment with her,” Brandon Seminatore said.
Wong, who has been working as a nurse for 32 years and has no plans to retire, told the Mercury News that she was overjoyed meeting Brandon Seminatore for the second time.
“As a nurse, it’s kind of like your reward.”
SOURCE:https://www.kiro7.com/news/trending-now/nurse-realizes-she-cared-for-doctor-when-he-was-a-preemie-baby-in-the-nicu/827786777
 This sleep meditation has been effective and energizing. We recommend you give it a go!
This sleep meditation has been effective and energizing. We recommend you give it a go!
Sleep Meditation: 21 Days of Letting Go, Guided Spoken Meditation for Letting Go of The Past
209,925 views 
Jason Stephenson – Sleep Meditation Music Published on Feb 8, 2019
30 Minutes spoken sleep meditation followed by 30 minutes of gentle music for sleeping. Wishing you better sleep, peaceful meditations before sleep and inspired living.
 KAT’S CORNER
KAT’S CORNER
While seeking growth along my healing journey it has come to my attention that I have a difficult time acting with the courage to fully enjoy being alive and present in my personal life and therefore in feeling confident about being in charge of my overall wellness and health. I notice some part of my ego that seeks to protect me engages in a pattern of self-sabotage when I begin to feel expanded responsibility and passion in areas related to my personal vitality and presence. On occasion I am hesitant to increase my personal intimacy with myself and others. I seem at times to be afraid that feeling more alive in life may lead to the disappointment of dying or the pain of being fully alive. I believe this may have resulted from my brother’s death and my painful beginning. Each day I am working to remind myself that the more I explore the PTSD associated with my birth more repressed feelings may arise in my consciousness. Daily I choose to be aware of my actions and to be kind with myself as I embrace my healing step by step. Healing and wholeness is what I wish for myself and all of my preterm birth brothers and sisters. Together we can choose courage, optimism, joy and presence.








