PORTUGAL

Preterm Birth Rates – Portugal
Rank: 138 –Rate: 7.7% Estimated # of preterm births per 100 live births (USA – 12 %)
Source: https://www.marchofdimes.org/mission/global-preterm.aspx
Portugal, officially the Portuguese Republic is a country located mostly on the Iberian Peninsula, in southwestern Europe. It is the western most sovereign state of mainland Europe, being bordered to the west and south by the Atlantic Ocean and to the north and east by Spain. Its territory also includes the Atlantic archipelagos of the Azores and Madeira, both autonomous regions with their own regional governments. The official and national language is Portuguese.
Portugal ranks 12th in the best public health systems in the world, ahead of other countries like the United Kingdom, Germany or Sweden. The Portuguese health system is characterized by three coexisting systems: the National Health Service (Serviço Nacional de Saúde, SNS), special social health insurance schemes for certain professions (health subsystems) and voluntary private health insurance. The SNS provides universal coverage. In addition, about 25% of the population is covered by the health subsystems, 10% by private insurance schemes and another 7% by mutual funds.
Source: https://en.wikipedia.org/wiki/Portugal
COMMUNITY
TAG: PORTUGAL – Covid Story 5
Posted on June 13, 2020
Joana Mendes, São Francisco Xavier Hospital, Lisbon, Portugal
I am a NICU nurse since I left nursing school. It was my big and only passion. I work now for about 18 years with babies and families. My main areas of expertise are ethics and palliative care. When Covid-19 was spreading quickly in Europe, I was doing a pediatric palliative care clinical practice in Cardiff. One of the first challenges, was returned home safely, when boarders where closing, all over the world. I got to Portugal 2 days just before the lockdown. The news, papers and social posts on internet, arriving from China, Italy and Spain, were really scary. Portuguese boards (medical, nursing and even veterinary’s) asked for health care professionals, from all backgrounds and scenarios, to come and help in human medicine, especially in adult emergency department and intensive care, if needed. They even asked the retired ones to volunteer. And they came. Neonatal nurses knew in advance, one could be mobilized anywhere, anytime. If the situation turned really bad, some would have to go and work in adult department. It sounded very unreal. Some of us when to the pediatric emergency department, when a lot of nurses were home due to quarantine needs. How would we help in adults? The second challenge faced, was the decision to left my sons (2- and 7-years old) with my husband and fathers in law. I felt heartbroken with all the uncertainty. I experienced strong and mixed feelings. Like never before, I listened the silence shouting and felt time passing in a very painful slow-motion way. In the hospital I work, one building was converted in a Covid-19 area. The other, the maternity, neonatal and pediatric building, was considered the non-Covid-19. NICU would admit babies that where born from mothers that tested positive or babies, during neonatal period, suspected to be or tested positive. Since, labor and delivery unit started testing all women, some, with no symptoms or risk factors, tested positive. Evidence was lacking, but the risk of vertical transmission seemed to be low (hopefully).
Neonatal health care team were daily, adapting, adjusting and reframing institutional guidelines. Would using CPAP would increase the risk for professionals’ transmission as suggested in adult literature? Was it possible to do the test properly to smaller babies, if the swab used is the same size in adults and newborns? Planning was very dynamic and all we were learning from one another, around the globe.
When the time came, NICU nurses, that had previous working experience in adult ICU and had with no risk factors for Covid-19, went to work full time there. NICU also admitted a nurse from ICU that had a chronic condition. The others non-risk nurses, like me, would be the first to take care of Covid-19 babies. First admissions came in Easter time. NICU nurses were committed to promote mother-baby bonding, holding concept and family centered care. Even before the first baby was born, were all brainstorming. A mobile phone or a tablet was identified as a good option to send video, photo or promote face time with the mother, if possible. Nurses phone called mother’s, each shift, to update about baby’s situation, lactation advices and other areas of counselling and promote emotional support.
Full protection equipment use was hard. No possibility to eat, drink or use toilets to optimize the deficiency in the number of equipment’s available. Even for a couple of hours, makes you feel hot, dehydrated, sometimes dizzy, with fogged glasses and with a sort of shortness of breath. After you remove it bruises and pressure zones in your face can remains for hours or days. All babies that were born during this pandemic time, not only Covid-19, suffered touch and human face interaction deprivation. Parents stayed in the NICU for short periods of time, because they were afraid. Professional were all wearing masks and gloves. The noxious sensory hyper stimulation seemed to gain preponderance to Kangaroo care, holding or breastfeeding. Difficult balance: health safety or human healthy development? What will be the consequences of this new crazy reality for next generation? What lessons do we have to learn, in order to elevate the quality of nursing care in the near future? This would be, the huge, third challenge. It was really inspired to feel that neonatal and pediatric palliative care were supporting one another in the globe. I felt we were really as one, sharing emotions and difficulties and being inspired to move forward.
Source: https://nna.org.uk/tag/portugal/

Violence Against Healthcare Workers: A Worldwide Phenomenon With Serious Consequences

Sandro Vento1*, Francesca Cainelli1,2 and Alfredo Vallone3
1Faculty of Medicine, University of Puthisastra, Phnom Penh, Cambodia, 2Raffles Medical Group Clinic, Phnom Penh, Cambodia, 3Infectious Diseases Unit, G. Jazzolino Hospital, Vibo Valentia, Italy
Introduction
Verbal and physical violence against healthcare workers (HCWs) have reached considerable levels worldwide, and the World Medical Association has most recently defined violence against health personnel “an international emergency that undermines the very foundations of health systems and impacts critically on patient’s health”. Two systematic reviews and meta-analyses published at the end of 2019 found a high prevalence of workplace violence by patients and visitors against nurses and physicians , and show that occupational violence against HCWs in dental healthcare centers is not uncommon .
Recent Studies
In the first study , the authors systematically searched PubMed, Embase, and Web of Science from their inception to October 2018, and included 253 eligible studies (with a total of 331,544 participants). 61.9% of the participants reported exposure to any form of workplace violence, 42.5% reported exposure to non-physical violence, and 24.4% experienced physical violence in the past year. Verbal abuse (57.6%) was the most common form of non-physical violence, followed by threats (33.2%) and sexual harassment (12.4%). The prevalence of violence against HCWs was particularly high in Asian and North American countries, in Psychiatric and Emergency departments, and among nurses and physicians .
In the second study , a systematic review and analysis of the literature was done using PubMed, ScienceDirect, Scopus, Web of Science, Cochrane Library and ProQuest. Original articles published between January 1992 and August 2019 and written in English were included in the analysis. The violence experienced by dental healthcare workers was both physical and non-physical (shouting, bullying, and threatening) and also included sexual harassment , and in most cases, male patients, or coworkers were responsible. Violent events ranged from 15.0 to 54.0% with a mean prevalence of 32%, and physical abuse ranged from 4.6 to 22% .
Most recently, the World Medical Association has condemned the increasingly reported cases of health care workers being attacked because of the fear that they will spread SARS-CoV-2. The situation in India is particularly shocking, with health care workers stigmatized, ostracized, discriminated against, and physically attacked, but incidents have been reported across the world, for instance from France, Mexico, Philippines, Turkey, UK, Australia, and USA.
Discussion
The recent systematic reviews and meta-analyses and the World Health Organization condemnation of the attacks against HCWs treating patients with COVID-19 have confirmed the seriousness of the situation regarding violence against doctors and nurses worldwide. Many countries have reported cases of violence, and some are particularly affected by this problem. A Chinese Hospital Association survey collecting data from 316 hospitals revealed that 96% of the hospitals surveyed experienced workplace violence in 2012, and a study done by the Chinese Medical Doctor Association in 2014 showed that over 70% of physicians ever experienced verbal abuse or physical injuries at work . An examination of all legal cases on violence against health professionals and facilities from the criminal ligation records 2010–2016, released by the Supreme Court of China, found that beating, pushing, verbal abuse, threatening, blocking hospital gates, and doors, smashing hospital property were frequently reported types of violence. In India, violence against healthcare workers and damage to healthcare facilities has become a debated issue at various levels , and the government has made violence against HCWs an offense punishable by up to 7 years imprisonment, after various episodes of violence and harassment of HCWs involved in COVID-19 care or contact tracing . In Germany, severe aggression or violence has been experienced by 23% of primary care physicians . In Spain, there has been an increase in the magnitude of the phenomenon in recent years . In the UK, a Health Service Journal and UNISON research found that 181 NHS Trusts in England reported 56,435 physical assaults on staff in 2016–2017 . In the USA, 70–74% of workplace assaults occur in healthcare settings . In Italy, in just one year, 50% of nurses were verbally assaulted in the workplace, 11% experienced physical violence, 4% were threatened with a weapon ; 50% of physicians were verbally, and 4% physically, assaulted . In Poland, Czech Republic, Slovakia, Turkey many nurses have been physically attacked or verbally abused in the workplace . According to the South African Medical Association, over 30 hospitals across South Africa reported serious security incidents in just 5 months in 2019 , and in Cape Town violence against ambulance crews is widespread . In Iran, the prevalence of physical or verbal workplace violence against emergency medical services personnel is 36 and 73% respectively . The World Health Organization lists Australia, Brazil, Bulgaria, Lebanon, Mozambique, Portugal, Thailand as other countries where studies on violence directed at HCWs have been conducted .
The consequences of violence against HCWs can be very serious: deaths or life-threatening injuries , reduced work interest, job dissatisfaction, decreased retention, more leave days, impaired work functioning , depression, post-traumatic stress disorder , decline of ethical values, increased practice of defensive medicine . Workplace violence is associated directly with higher incidence of burnout, lower patient safety, and more adverse events .
Which are the most at-risk services and what are the underlying factors of this growing violence? Emergency Departments, Mental Health Units, Drug and Alcohol Clinics, Ambulance services and remote Health Posts with insufficient security and a single HCW are at higher risk. Working in remote health care areas, understaffing, emotional or mental stress of patients or visitors, insufficient security, and lack of preventative measures have been identified as underlying factors of violence against physicians in a 2019 systematic review and meta-analysis .
In public hospital/services, insufficient time devoted to patients and therefore insufficient communication between HCWs and patients, long waiting times, and overcrowding in waiting areas , lack of trust in HCWs or in the healthcare system, dissatisfaction with treatment or care provided , degree of staff professionalism, unacceptable comments of staff members, and unrealistic expectations of patients and families over treatment success are thought to contribute. Indeed, in public hospitals worldwide, staff shortages prevent front-line HCWs from adequately coping with patients’ demands. In private hospitals/services, too extended hospital stays, unexpectedly high bills, prescription of expensive and unnecessary investigations are key factors. Finally, the media frequently report extreme cases of possible malpractice and portray them as representative of “normal” practice in hospitals .
What can be done to reduce the escalating violence against HCWs? HCWs worldwide generally advocate for more severe laws, but harsher penalties alone are unlikely to solve the problem. Importantly, evidence on the efficacy of interventions to prevent aggression against doctors is lacking, and a systematic review and meta-analysis found that only few studies have provided such evidence . Just one randomized controlled trial indicated that a violence prevention program decreased the risks of patient-to-worker violence and of related injury in hospitals , whereas contrasting results in violence rates after implementation of workplace violence prevention programs have been observed from longitudinal studies . There is no evidence on the effectiveness of good place design and work policies aimed to reduce long waiting times or crowding in waiting areas . More studies are clearly needed to provide evidence-based recommendations, and interdisciplinary research with the involvement of anthropologists, sociologists, and psychologists should be encouraged. However, certain measures have to be taken and can be corrected, should they be shown as ineffective in properly conducted studies.
Security measures have been advocated for years and should be taken to safeguard particularly the most at-risk services. First, staff shortages, so common in public hospitals worldwide, should be acted upon, and increased funding should be allocated to employ more doctors and nurses. Hence, the duration of each patient encounter would be augmented, particularly in overburdened public hospitals, allowing the (often young) doctors to develop a meaningful relationship with the patient. Second, healthcare organizations and universities should considerably improve the communication skills of current and future HCWs to reduce unrealistic expectations or misunderstanding of patients and families. Third, HCWs who denounce any verbal or physical violence should be fully supported by their healthcare organizations; this would reduce the huge issue of under-reporting of workplace violence . Good courses should be organized for HCWs to learn how to identify early signs that somebody may become violent, how to manage dangerous situations, and how to protect themselves.
Prompt communication about delays in service provision should be given to patients and their relatives when waiting times are long because certain conditions are prioritized. Alarms and closed-circuit televisions should be placed in the higher-risk departments and in areas where doctors and/or nurses work in isolation. Sanctioning of violence by patients, relatives or visitors must be imposed. Staff should be increased and security officers should be placed, particularly at night, in remote Health Posts and Emergency Departments and at particular times (violence tends to happen in the evenings/nights, when more patients under the influence of drugs and alcohol present); the number of night shifts should be limited . Efforts should be made to improve job satisfaction of HCWs . Finally, media should cease to contribute to the general public’s distrust toward HCWs and institutions. Many patients report their negative experiences of medical care to news or media outlets which are highly interested in these stories and very often do not check the information before publishing it . These biased media reports may exacerbate the tension.
All workers have a right to be safe on their job, and healthcare workers are no exception. The idea that violence is inherent to doctors and nurses’ work, especially in certain departments, needs to be fought; urgent measures must be implemented to ensure the safety of all HCWs in their environment, and the needed resources must be allocated. Failure to do so will worsen the care that they are employed to deliver and will ultimately negatively affect the whole healthcare system worldwide.
Source: https://www.frontiersin.org/articles/10.3389/fpubh.2020.570459/full
Self-care during COVID-19

The Partnership for Maternal, Newborn & Child Health (PMNCH, the Partnership) is the world’s largest alliance for women’s, children’s and adolescents’ health (WCAH), bringing together over 1,000 partner organizations across 192 countries.
Emerging evidence has shown how critical and effective self-care can be. When women, children and adolescents are empowered to adopt healthy self-care practices, they can play a critical role in protecting their own health.
To promote self-care practices around key sexual, reproductive, maternal, newborn, child and adolescent health issues during the COVID-19 pandemic, PMNCH is partnering with WHO and other UN partner agencies to develop a series of short animated videos to promote healthy behaviours during the pandemic. These videos help translate the latest WHO guidance on self-care practices for women, children adolescents and their families in relation to key issues arising in the context of COVID-19.
Source: https://www.who.int/pmnch/media/videos/self-care-series/en/
PREEMIE FAMILY PARTNERS

Breastfeeding during COVID-19
This video demonstrates how mothers with Covid-19 can breastfeed safely, providing their newborn with the best source of nutrition and protection to survive and thrive. The 60-second film was produced by award-winning Studio Eeksaurus of Mumbai with UK-based Medical Aid Films. It has reached more than 40 million viewers on social media since the launch on 28 May 2020. The video is also available in the five official languages of the United Nations (Arabic, Mandarin, French, Russian and Spanish).

Is This Normal? How the NICU Impacts Your Emotional Health
by Hand to Hold Staff | Jun 7, 2018

Having a baby in the neonatal intensive care unit is a traumatic experience. No one is ever really prepared. You have probably felt emotions during your baby’s NICU stay that you never imagined feeling. You have celebrated things you never knew you would and seen things you never imagined.
All of the emotions that you experience in the NICU – grief, guilt, depression, anxiety, fear – are normal and appropriate. They are natural responses to traumatic events. They are not a sign of weakness. They are a healthy part of adapting and adjusting to being your baby’s parent.
Here are some of the things you may be feeling or may feel in the coming weeks and months. While all these feelings are normal, it is important for you and your family to recognize if they become a problem and know how to get the help and support you need if they do.
Grief & guilt
Grief is what you feel when you lose something that is important to you. If your baby is in the NICU, it is normal to grieve. You are allowed to feel sad and angry that your pregnancy didn’t go as you expected and that your baby needs critical care. Maybe you feel guilty that you might have done something to cause this. The truth is that you can do everything right and still end up in the NICU, and you can do everything wrong and still have a healthy birth. Talk to your doctors and ask questions. You may or may not be able to find reasons why this happened. Most of the time we don’t know the reason. While it’s important to find out what you need to do to take care of your baby and yourself, it is also important for you to forgive yourself and your body.
Depression
Sometimes it can be hard to tell the difference between feeling tired and feeling depressed. While your baby is in the NICU, you are probably trying to keep up with a busy schedule of driving back and forth to the hospital and managing things both in the NICU and at home. It’s understandable if you’re feeling emotional and exhausted. It is important for you to recognize signs of depression and to know what to do if the symptoms persist.
Postpartum depression is common. If you feel any of these symptoms for more than a month or two, talk to someone and make a plan. There are things you can do to feel better and medications that can help. You may have depression if you have these symptoms:
- Exhaustion – You feel tired and overwhelmed by everything you need to do.
- Inability to Sleep – You have difficulty falling asleep or staying asleep.
- Loss of Appetite – You make time to eat, but aren’t interested in food, and you don’t get hungry when you should.
- Sadness and Mood Swings – You feel like you are sadder than you should be or you feel like your emotions are more than you can manage.
- You Know Something is Wrong – You know how you are feeling is not right and doesn’t make sense.
Anxiety & acute stress
While your baby is in the NICU, you learn to be hyper-vigilant. You wash your hands hundreds of times and watch the monitors and equipment to keep track of everything your baby is doing. It can all make you feel a little crazy. Anxiety can feel like:
- Nervousness – You’re aware of all the things that can go wrong and feel like you’re waiting for the next bad thing to happen.
- Fearfulness – You are afraid of what happens in the NICU and worried about what your baby is feeling.
- Anger and Irritation – You are either mad at the people around you or mad at the situation, but you can’t stop feeling annoyed.
Many NICU parents will experience symptoms of a condition called Acute Stress Disorder (ASD). ASD develops when you witness traumatic events. You may feel:
- Frightened – You may have witnessed terrible and terrifying things.
- Disconnected – You might feel like this isn’t “real” and that this isn’t possible.
- Surprised by What You’re Feeling – A sound or smell might trigger an overwhelming reaction or make you feel like you’re reliving something that already happened.
Acute Stress Disorder is a normal physiological response. It is how our brains and bodies react to trauma. The symptoms usually appear within a month and get better over the next few weeks. If your symptoms don’t get better – or they get worse – you may have developed a more serious condition called PTSD.
Post-traumatic stress disorder (PTSD)
PTSD is an anxiety disorder characterized by persistent, debilitating physical and emotional symptoms. The symptoms are grouped into three types:
- Intrusive Memories – Having flashbacks or feeling like you’re reliving the experience over and over again.
- Avoidance & Numbing – Trying not to feel the intense emotions that you fear you might.
- Increased Anxiety & Emotional Arousal – Feeling like you can’t relax because something bad might happen.
How to get help
There are two important things you need to know about these feelings and conditions. They are normal, and they are temporary. You will feel better. All of these people can help:
- Your doctor – Talk to your doctor, OB/GYN or pediatrician. Print this screening tool to take with you.
- Social worker – Call the NICU social worker. They will know how to get help.
- Professional counselor – Many professionals specialize in helping with these conditions.
- Community resources – Support is available online and by phone. Connect with Hand to Hold’s online communities for valuable resources and support.
- Family and friends – They want to help even if they’re not sure how. Tell them what you need. Read how you can help a loved one.
- Peer support – Hand to Hold can connect you with families just like yours who know what you’re feeling and how to get better.
Caring for your emotional and mental health is an important part of taking care of yourself. You don’t deserve to feel this way. You deserve to feel healthy, and you can get better.
3 Resources you should know
Postpartum Support International provides resources about perinatal mood and anxiety disorders.doing
Postpartum Progress is a community website that shares the stories of other women and men who have experienced PPD, as well as valuable resources and information about perinatal mood disorders.
NICU Family Forum is Hand to Hold’s online peer support group for NICU parents who are going through or who had a NICU experience with their preterm or full-term infants. Join us on Facebook.
Source: handtohold.org/nicu-emotional-health/
Why language development is especially challenging for premature babies and what the team at the Montreal Children’s Hospital’s Neonatal Intensive Care Unit (NICU) is doing to help parents interact with their babies.

McGill University Health Centre (MUHC) Sep 15, 2020
INNOVATIONS
Catching infections in premature babies before they happen using AI
04/07/20
Using Artificial Intelligence to help premature babies stay healthy is the aim of a European research project.… READ MORE : Source:https://www.euronews.com/2020/04/07/c…

Maternal Work and Spontaneous Preterm Birth: A Multicenter Observational Study in Brazil

Scientific Reports volume 10, Article number: 9684 (2020) Published 16June2O
Abstract
Spontaneous preterm birth (sPTB) is a major pregnancy complication involving biological, social, behavioural and environmental mechanisms. Workload, shift and intensity may play a role in the occurrence of sPTB. This analysis is aimed addressing the effect of occupational activities on the risk for sPTB and the related outcomes. We conducted a secondary analysis of the EMIP study, a Brazilian multicentre cross-sectional study. For this analysis, we included 1,280 singleton sPTB and 1,136 singleton term birth cases. Independent variables included sociodemographic characteristics, clinical complications, work characteristics, and physical effort devoted to household chores. A backward multiple logistic regression analysis was applied for a model using work characteristics, controlled by cluster sampling design. On bivariate analysis, discontinuing work during pregnancy and working until the 7th month of pregnancy were risks for premature birth while working during the 8th – 9th month of pregnancy, prolonged standing during work and doing household chores appeared to be protective against sPTB during pregnancy. Previous preterm birth, polyhydramnios, vaginal bleeding, stopping work during pregnancy, or working until the 7th month of pregnancy were risk factors in the multivariate analysis. The protective effect of variables compatible with exertion during paid work may represent a reverse causality. Nevertheless, a reduced risk associated with household duties, and working until the 8th-9th month of pregnancy support the hypothesis that some sort of physical exertion may provide actual protection against sPTB.
Full Article: https://www.nature.com/articles/s41598-020-66231-2
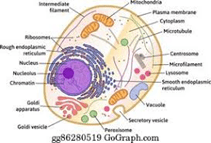
Therapeutic approach of stem cell transplantation for neonatal white matter injury
Received: 31 March 2020; Accepted: 24 July 2020; Published: 31 August 2020.

Ling Ma1, Xiaoli Ji1, Chuanqing Tang2, Wenhao Zhou1,3, Man Xiong2,3
1Department of Neonatology, Children’s Hospital of Fudan University, Shanghai, China; 2Stem Cell Research Center, Institute of Pediatrics, Children’s Hospital of Fudan University, Shanghai, China; 3Key Laboratory of Neonatal Diseases, Ministry of Health, Children’s Hospital of Fudan University, Shanghai, China
Abstract: The white matter in brain are mainly composed of oligodendrocytes and myelinated axons, and are important for the transmission of neural signals in central nervous system. White matter injury (WMI) is a leading cause of neurocognitive deficits in premature infants as the oligodendrocytes progenitors are easily attacked by hypoxia-ischemia (HI). Various clinical methods are used to treat this disease, while none of them could reverse the sequelae of WMI completely. With the development of stem cell technology, stem cell therapy has attracted huge interest as a novel treatment for WMI. A number of investigations have demonstrated the potential therapeutic effects of stem cell transplantation on WMI. Different types of stem cells have also been used by many researchers to test the therapeutic effect on WMI animal models, such as neural stem cells (NSCs), glial progenitor cells, mesenchymal stem cells (MSCs). In addition, some clinical trials have been conducted. Evidence suggests that transplantation of these stem cells into animals contributes to functional recovery after experimental WMI. The mechanisms of stem cells therapy may include differentiation into neurons and glial cells to replace lost cells, activation of endogenous NSC regeneration, and promotion of the release of neurotrophins. In this review, we summarized effects of different types of stem cells transplantation, the underlying mechanisms, the unsolved problems and concerns before clinical trials and transformation of stem cell therapy for WMI.
ARTICLE

Full Article: http://pm.amegroups.com/article/view/5604/html

Dr. Stephen Porges: What is the Polyvagal Theory
Apr 23, 2018
Dr. Stephen Porges explains Polyvagal Theory in his interview with PsychAlive.org.
Learn More about Dr. Porges at https://www.stephenporges.com/
HEALTH CARE PARTNERS
The World Health Organization says that there is currently a global shortage of more than seven million health workers and that number could rise to nearly 13 million by 2035. We rely on our Healthcare Partners to provide lifesaving and ongoing medical care to our Warriors, Family Partners, Community Partners and to the Healthcare Partners themselves. Our Global preterm birth community must actively support the development, training, safety, retainment, health and wellness, and Global collaboration of our Healthcare Partners in order to support the needs of the Preterm Birth Community at large. We need each other.
2020 Infant Health Policy Summit

Sep 29, 2020
The sixth annual Infant Health Policy Summit welcomed health care providers, parents, policymakers, advocates and other stakeholders to explore how policy solutions can improve the health and lives of infants and their families. This year’s event, held virtually, examined issues such as:
- Disparities in infant health
- Congenital gut disorders
- Human milk.
- Late preterm infants
- Respiratory syncytial virus and COVID-19
- Isolation and disruption during COVID-19
- Vaccines
The summit, which included a series of panel discussions, individual stories and interviews, was convened by the National Coalition for Infant Health and co-hosted by the Institute for Patient Access and Alliance for Patient Access. Read the report and watch the summit recording to learn more.
Full Article: http://www.infanthealth.org/summit
VIEW SUMMIT RECORDING:



Pasteurization inactivates COVID-19 virus in human milk: new research
August 11, 2020 – University of New South Wales – A new study has confirmed what researchers already suspected to be the case: heat inactivates SARS-CoV-2 in human milk.

A team of medical researchers has found that in human milk, pasteurisation inactivates the virus that causes COVID-19, confirming milk bank processes have been safe throughout the pandemic, and will remain safe going forward, too.
The study — published this month in the Journal of Paediatrics and Child Health — was a partnership between UNSW and a multidisciplinary team from Australian Red Cross Lifeblood Milk.
There are five human milk banks in Australia. As the COVID-19 pandemic evolves, these milk banks continue to provide donated breast milk to preterm babies who lack access to their mother’s own milk. Donors are screened for diseases, and milk is tested and pasteurised to ensure that it is safe for medically fragile babies.
“While there is no evidence that the virus can be transmitted through breast milk, there is always a theoretical risk,” says Greg Walker, lead author and PhD candidate in Professor Bill Rawlinson’s group at UNSW Medicine.
“We’ve seen in previous pandemics that pasteurised donor human milk (PDHM) supplies may be interrupted because of safety considerations, so that’s why we wanted to show that PDHM remains safe.”
For this study, the team worked in the Kirby Institute’s PC3 lab to experimentally infect small amounts of frozen and freshly expressed breast milk from healthy Lifeblood Milk donors.
“We then heated the milk samples — now infected with SARS-CoV-2 — to 63?C for 30 minutes to simulate the pasteurisation process that occurs in milk banks, and found that after this process, they did not contain any infectious, live virus,” Mr Walker says.
“Our findings demonstrate that the SARS-CoV-2 virus can be effectively inactivated by pasteurisation.”
The researchers say their experiments simulated a theoretical worst-case scenario.
“The amount of virus we use in the lab is a lot higher than what would be found in breast milk from women who have COVID-19 — so we can be really confident in these findings,” Mr Walker says.
Dr Laura Klein, Research Fellow and Lifeblood Milk senior study author, explains that the purpose of the research was to provide evidence behind what people already expected.
“Pasteurisation is well known to inactivate many viruses, including the coronaviruses that cause SARS and MERS,” she says.
“These findings are also consistent with a recent study that reported SARS-CoV-2 is inactivated by heat treatment in some contexts.”
Kirby Institute researcher and study co-author, Associate Professor Stuart Turville, says this work was a first.
“We’ve been working in real time to grow and make tools against this new pathogen, which has been an exponential learning curve for everyone involved. This work and many others that are continuing in the PC3 lab tell us how we can be safe at the front line working with this virus in the real world.”
Cold storage doesn’t inactivate the virus
The researchers also tested if storing SARS-CoV-2 in human milk at 4°C or -30°C would inactivate the virus — the first time a study has assessed the stability of experimentally infected SARS-CoV-2 in human milk under common storage conditions.
“We found that cold storage did not significantly impact infectious viral load over a 48-hour period,” Mr Walker says.
“While freezing the milk resulted in a slight reduction in the virus present, we still recovered viable virus after 48 hours of storage.”
The researchers say the fact that SARS-CoV-2 was stable in refrigerated or frozen human milk could help inform guidelines around safe expressing and storing of milk from COVID-19 infected mothers.
“For example, we now know that it is particularly important for mothers with COVID-19 to ensure their expressed breast milk does not become contaminated with SARS-CoV-2,” Dr Klein says.
“But it’s also important to note that breastfeeding is still safe for mothers with COVID-19 — there is no evidence to suggest that SARS-CoV-2 can be transmitted through breastmilk.”
Donated breast milk is recommended by the World Health Organisation when mother’s own milk is not available to reduce the risks of some health challenges premature babies can face. Lifeblood Milk has provided donor milk to over 1500 babies born premature in 11 NICUs across New South Wales, South Australia, and Queensland since launching in 2018.
Source: https://www.sciencedaily.com/releases/2020/08/200811120217.htm

Shining a light on physician suicide
Sep 17, 2020 – 12:25 PM by Elisa Arespacochaga – vice president of the AHA Physician Alliance.
The COVID-19 pandemic makes working in health care especially exhausting both physically and mentally. These front-line care workers face putting their families and colleagues at risk for exposure to the virus, working extended shift hours and confronting an unimaginable death toll.
The number of Americans who have died from COVID-19 is approaching 200,000, and due to the nature of the virus, the vast majority occur in the hospital, a place for healing and hope. The pandemic’s staggering death count blankets all caregivers in heavy sadness. Unlike so many of the disasters that hospitals and their teams are ready to help address, this one isn’t lasting just a few days. Our caregivers are experiencing a protracted state of grief over six months and counting. The ongoing challenges are making it difficult to find time to grieve, address stress and deal with feelings of distress.
Each year roughly 400 physicians die by suicide. Hundreds more harbor serious thoughts of suicide. The suicide completion rate among doctors is 44% higher than the expected population; female physicians have a higher suicide completion rate than male doctors[i]. Stress, burnout, and trauma all contribute to this devastating toll. And, COVID-19 will likely intensify those emotions.
We must tackle these grim statistics head on. “Shine a Light, Speak its name” is the theme for National Physician Suicide Awareness Day, Sept. 17.
To shed light on the issue and highlight prevention strategies, the AHA’s Physician Alliance and the Education Development Center (EDC) have produced the Be Well: Preventing Physician Suicide podcast series. It shares stories of recovery and ideas for supporting colleagues struggling with thoughts of suicide. Other resources to foster well-being include the AHA Physician Alliance’s Well-Being Playbook, as well as EDC’s Suicide Prevention Resource Center which provides technical assistance, training and materials.
AHA’s Caring for Our Health Care Heroes During COVID-19 offers real-world examples of how hospitals and health systems are helping care for, and support, their workforce during the pandemic. It also provides a list of national well-being programs and resources developed for health care workers.
In this AHA Members in Action case study, ChristianaCare of Newark, Del., shares its multi-year journey to create the Center for WorkLife Wellbeing, that has spawned numerous innovative programs, such as a calming OASIS room, COMPASS (Clinician-Organized Meetings to Promote and Sustain Satisfaction), and the Care for the Caregiver peer support program.
By acknowledging the heavy sadness caused by the pandemic’s death toll and shining a light on the problem of physician suicide and openly addressing the issue, we can help support and care for physicians. Does your hospital have a formal clinician well-being program? If so, please share your story with me at elisa@aha.org.
If you or anyone you know is struggling, please reach out to the National Suicide Prevention Lifeline at 1-800-273-8255 (TALK) to speak to a trained professional.
Source: https://www.aha.org/news/blog/2020-09-17-shining-light-physician-suicide

Fast Five: Strategies for Addressing Moral Distress in Frontline Health Care Workers

In this Fast Five from the Center to Advance Palliative Care (CAPC), Dr. Ira Byock, Chief Medical Officer for the Providence Health System Institute for Human Caring shares three practical initiatives that can foster human connection among patients, families, and clinical care teams when in-person visits are restricted or the heavy use of personal protective equipment limits the ability to connect in a meaningful way.


WARRIORS:

KAT’S CORNER
Historically mental health for youth and adolescents has been overlooked and under-valued. Covid-19 has resulted in elevated levels of mental health disparities and stress among the Global community. For our youth, mental health support has been challenging to gain as many schools have transitioned to online platforms for some and for others school has been cancelled all together. While families and individual’s grapple to find ways to navigate pandemic challenges we have an opportunity to move forward in creative and resilient ways. The pandemic is a direct challenge to our Warriors to take action towards building and strengthening their personal and community well-being.
If you are a youth, or interact with youth, who may need and benefit from mental-health resources we encourage you to review the article below, understand the impact the pandemic may have on youth mental health and explore the variety of recommendations the article offers to youth worldwide.
OPINION: In this time of COVID-19 a new consensus on how we should be working to improve adolescent well-being is long overdue
5 October 2020 – By Enes Efendioğlu and Souzana Humsi, Adolescents and Youth Constituency Board Members
Every generation of adolescents grapples with the difficult transition from childhood into adult life: juggling social and academic pressures at school; coping with changing dynamics within family and friendship groups; experiencing the physical and mental transformation of puberty; and making crucial decisions about whether to pursue further education or embark on careers.
This generation of 10-19-year olds is no exception – except they are also having to navigate adolescence during a global pandemic that is causing unprecedented harm to people’s health, and damaging the social and economic fabric of countries world-wide.
Adolescents have been among the worst affected by the indirect consequences of the pandemic. It has severely disrupted education provision, which can have adverse effects on adolescents’ social skills at a critical time in their development. When adolescents are unable to attend schools, they may experience depression, social anxiety and stress that can lead to deeper mental health issues, or even push them toward risky behaviours, including drug abuse and self-harm.
With so many pressures on governments to address the direct health consequences of COVID-19, limit its transmission and kick-start economies, finding time and resources to tackle its indirect consequences, including those affecting adolescents, is a challenge.
Adolescents are sometimes underserved by policies intended to improve their health and well-being, and sometimes are not consulted when interventions for their benefit are being developed. A recent study, for example, estimated that development assistance for adolescent health only accounted for 1.6% of all development assistance between 2003 and 2015.
Occasionally, issues that are of importance to young people are under-resourced, or not addressed in the appropriate way. For example, in some countries, comprehensive sexuality education interventions can be very limited, or actively restricted. Many young people are denied access to age-appropriate information to protect themselves from unintended pregnancy and sexually transmitted infections, or to avoid situations that put them at risk of domestic or gender-based violence or sexual exploitation, which have also increased during the pandemic. If they do access helpful information, they may often find that they don’t have any youth-friendly services to address the repercussions of these issues.
Another major issue that has made work in the field of adolescent well-being more complex than it needs to be has been the lack of a specific unified framework for addressing the issues. This can affect the quality of strategies and interventions being developed for adolescents, because having piecemeal guidelines, research, toolkits and documents covering broadly similar issues – all claiming to be authoritative – inevitably leads to costly duplication and confusion for programme implementers about the right approaches to take.
Fortunately, a recent, extremely welcome initiative is seeking to reframe the narrative around adolescent well-being, and lay the foundations for improved interventions that fully take account of young people’s self-articulated needs.
After the introduction and adoption of the Sustainable Development Goals (SDGs) in 2015, one big objective was to provide access to universal healthcare for people of all ages, everywhere in the world. The task before the coalition of governments, UN organizations, non-governmental organizations and academic institutions who have come together to support a Call to Action for Adolescent Wellbeing, backed by a new definition and conceptual framework, was to define what adolescent well-being looks like.
The resulting definition and conceptual framework for adolescent health is published this week in the Journal of Adolescent Health. The paper defines adolescent wellbeing as being a state where: ‘Adolescents have the support, confidence, and resources to thrive in contexts of secure and healthy relationships, realizing their full potential and rights’ and also stresses the importance of five interconnected domains:
- Good health and optimum nutrition
- Connectedness, positive values and contribution to society
- Safety and a supportive environment
- Learning, competence, education, skills and employability
- Agency and resilience.
The five domains encompass both objective and subjective terminology, and are underpinned by gender, equity and rights considerations. Collectively, the definition and framework provide a new basis for building global consensus around working to improve adolescent well-being.
One key challenge in this process was to ensure that those with the deepest insights to what this generation of adolescents need – adolescents and young people themselves – were fully consulted.
As Board Members representing an Adolescents and Youth Constituency at one of the key organisations involved in this process, the Partnership for Maternal, Newborn & Child Health (PMNCH), the co-authors of this opinion are proud to have driven the consultation process to develop the framework.
Carrying out a global consultation in the time of COVID-19 is challenging, as many adolescents could only be reached online, so additional outreach was required towards some marginalised groups, including indigenous youth and young migrants, to ensure their perspectives were included. Consultations continue, however, and under-represented groups, particularly those without internet access, will be reached.
The framework provides a new way of working, by looking at adolescent well-being through a comprehensive lens, which is even more important in these dynamic and critical times.
Ultimately, the aim is to have a globally adopted, evidence-based definition and framework governing how best to partner with adolescents and young people in designing interventions they will access and use, because they should be owned by and for them. This will be presented in a UN Summit on Adolescent Well-being, which partners such as PMNCH are working closely with Member States to mobilize towards in 2022 or 2023, the mid-way point towards the SDGs 2030 Agenda.
Since COVID-19 began, we have seen an immense amount of co-operation and collaborations, both within and between countries, such as the COVAX mechanism, the international partnership to distribute any COVID vaccine equitably, regardless of any country’s ability to pay.
Hopefully this spirit of international collaboration will be seen as the global definition and conceptual framework for adolescent wellbeing is rolled out.
Not only will such collaboration help to avoid costly duplication of effort. It will also enable programme managers to plan and co-ordinate their efforts around particular domains, so that collectively they will have a greater chance of meeting more international targets for adolescent health and wellbeing by 2030.
Source: https://www.who.int/pmnch/media/news/2020/covid-improving-adolescent/en/
The Medical Home organization recommends the following APP friendly resources to kids coping with anxiety. Each of the following Apps may be accessed directly via the hyperlinks listed below. For additional information on The Medical Home Portal and a summary of each APP please follow the Full-Article link listed below.
Apps to Help Kids and Teens with Anxiety
- Breathe, Think, Do with Sesame Street
- Breathe 2 Relax
- CBT Tools for Youth
- Cosmic Kids
- DreamyKid
- HappiMe and HappiMe for Young People
- Healing Buddies Comfort Kit
- Manatee & Me
- Moshi: Sleep and Mindfulness
- Smiling Mind
- SuperBetter
- Super Stretch Yoga


La gigantesca OLA de 35 Metros en Nazaré Portugal 🌊The largest WAVE EVER Nazaré Portugal 115 feet🌊

Sep 20, 2020 Berna SUPer SURFers
Big Wave Surfer, Hugo Vau, surfed the largest wave ever in Nazare, Portugal. This beautifully poetic and intimate documentary follows Hugo Vau as he recalls the strength, ambition and fears that lead up to the day that forever changed his life and career. Directed by Nina Meredith