

PRETERM BIRTH RATES –India
Rank: 36 –Rate 13% Estimated # of preterm births per 100 live births (USA – 12 %, Global Average: 11.1%)
India: officially the Republic of India is a country in South Asia. It is the second-most populous country, the seventh-largest country by land area, and the most populous democracy in the world. Bounded by the Indian Ocean on the south, the Arabian Sea on the southwest, and the Bay of Bengal on the southeast, it shares land borders with Pakistan to the west; China, Nepal, and Bhutan to the north; and Bangladesh and Myanmar to the east. In the Indian Ocean, India is in the vicinity of Sri Lanka and the Maldives; its Andaman and Nicobar Islands share a maritime border with Thailand, Myanmar and Indonesia.
India has been a federal republic since 1950, governed in a democratic parliamentary system. It is a pluralistic, multilingual and multi-ethnic society. India’s population grew from 361 million in 1951 to 1.211 billion in 2011. During the same time, its nominal per capita income increased from US$64 annually to US$1,498, and its literacy rate from 16.6% to 74%. From being a comparatively destitute country in 1951, India has become a fast-growing major economy and a hub for information technology services, with an expanding middle class. It has a space programme which includes several planned or completed extraterrestrial missions. Indian movies, music, and spiritual teachings play an increasing role in global culture. India has substantially reduced its rate of poverty, though at the cost of increasing economic inequality. India is a nuclear-weapon state, which ranks high in military expenditure. It has disputes over Kashmir with its neighbours, Pakistan and China, unresolved since the mid-20th century. Among the socio-economic challenges India faces are gender inequality, child malnutrition, and rising levels of air pollution. India’s land is megadiverse, with four biodiversity hotspots. Its forest cover comprises 21.4% of its area. India’s wildlife, which has traditionally been viewed with tolerance in India’s culture, is supported among these forests, and elsewhere, in protected habitats.
India has a universal multi-payer health care model that is paid for by a combination of public and private health insurances along with the element of almost entirely tax-funded public hospitals. The public hospital system is essentially free for all Indian residents except for small, often symbolic co-payments in some services. At the federal level, a national health insurance program was launched in 2018 by the Government of India, called Ayushman Bharat. This aimed to cover the bottom 50% (500 million people) of the country’s population working in the unorganized sector (enterprises having less than 10 employees) and offers them free treatment even at private hospitals. For people working in the organized sector (enterprises with more than 10 employees) and earning a monthly salary of up to Rs 21000 are covered by the social insurance scheme of Employees’ State Insurance which entirely funds their healthcare (along with pension and unemployment benefits), both in public and private hospitals. People earning more than that amount are provided health insurance coverage by their employers through the many public or private insurance companies. As of 2020, 300 million Indians are covered by insurance bought from one of the public or private insurance companies by their employers as group or individual plans. Unemployed people without coverage are covered by the various state funding schemes for emergency hospitalization if they do not have the means to pay for it. In 2019, the total net government spending on healthcare was $ 36 billion or 1.23 % of its GDP. Since the country’s independence, the public hospital system has been entirely funded through general taxation.
Source: https://en.wikipedia.org/wiki/India

COMMUNITY

What Happened With Preterm Birth During the Pandemic?
Some mothers — and their babies — may have fared better than others
Email article by Amanda D’Ambrosio, Enterprise & Investigative Writer, MedPage April 8, 2021
While pregnant women have been warned about their potential for more severe COVID-19 illness, a few early reports have suggested one positive finding for this population — that pandemic lockdown restrictions may have coincided with a decrease in preterm births.
Early studies have observed a decline in preterm birth rates during the lockdowns, highlighting a potential “silver lining” of the pandemic. But while these findings are encouraging, experts say there is still not enough data to know whether the reduction in preterm births was widespread, or what factors may have caused this outcome to drop in the first place.
“The jury is out, in terms of what’s the overall impact [of the pandemic] on preterm birth,” said Rahul Gupta, MD, MPH, chief medical and health officer at March of Dimes. While early data may provide some insight into lifestyle changes such as working from home and remote access to healthcare, Gupta said more information is needed before drawing conclusions about preterm birth reductions — and which populations were most affected.
Globally, preterm birth is the leading cause of death in children under 5 years old, according to the WHO. In the U.S., the preterm birth rate has been on a consistent upward trajectory, with 2019 being the fifth straight year in a row that the rate increased. Between 2018 and 2019, the preterm birth rate rose by 2%, according to the CDC.
Clinicians from Denmark and Ireland first began to notice a decline in preterm births last spring — specifically, those that were earliest and most critical. A preprint study from Denmark, which included more than 31,000 infants born between 2015 and 2020, showed around a 90% decrease in extremely preterm births (those born before 32 weeks’ gestation) during the lockdown period. In Ireland, another study published in BMJ Global Health observed a 73% reduction in extremely low birthweight deliveries, from January to April of last year.
Other studies have found that rates decrease for specific populations. A recent systematic review and meta-analysis in The Lancet Global Health found that while the overall preterm birth rate was not significantly different before and during the pandemic, the rate in high-income countries declined by 9%. Spontaneous preterm births in high-income countries saw an even greater reduction, falling by almost 20%.
“Interestingly, there are happy numbers mainly from high-income countries,” said the study’s lead author, Asma Khalil, MD, of St. George’s University Hospitals NHS Foundation Trust in London.
Some reports from the U.S. also reflected a decline, albeit a smaller one. Last April, Stephen Patrick, MD, MPH, of Vanderbilt University, wrote on Twitter that he noticed a lower number of infants in the neonatal intensive care unit (NICU) at his institution.
Last month, Patrick and colleagues published a study in JAMA Pediatrics showing the relationship between preterm birth and stay-at-home orders in Tennessee. Patrick’s team found that the risk of preterm birth fell nearly 15% during the lockdown period, after controlling for maternal age, race, education level, hypertension, and diabetes.
Naima Joseph, MD, MPH, a maternal-fetal medicine fellow at Emory University School of Medicine, said it could be that the decline is related to the environmental and lifestyle changes that occurred during the early months of the pandemic.
Alison Gemmill, PhD, of Johns Hopkins University, said that a number of changes during lockdown may have been associated with drops in the preterm birth rate. When most cars were off the roads, there may have been a decline in the number of preterm births associated with air pollution. Additionally, as pregnant people shifted to remote work and found themselves at home and off their feet, Gemmill said there may have been a decline in physical stress.
Another hypothesis, Gemmill added, is that the decrease in preterm births may have occurred simultaneously with an increase in stillbirths. Some reports have shown an increase in stillbirths during the pandemic (including Khalil’s analysis), but U.S. data has yet to confirm this increase.
Gemmill and colleagues published a study last week (which has not yet been peer-reviewed) showing that the preterm birth rate in the U.S. was one of several birth outcomes that was lower than expected in March and April of last year. But the group also observed that the rate dipped significantly again in November and December — coinciding with the months when infection rates climbed.
“Something is definitely going on,” Gemmill said in an interview. She added that the rates her group observed are crude, and do not describe how different demographic groups in the U.S. were affected. However, she said her research is “detecting a really important signal that doesn’t occur in birth outcomes research.”
Not all U.S. data confirm this pattern. A JAMA study of nearly 9,000 infants at the University of Pennsylvania showed that mothers in 2020 were at the same risk of preterm birth than they had been in years prior.
Gupta, of March of Dimes, stated that the U.S. is not a homogenous society, and preterm birth rates will look different across different populations. Black parents, for example, have a 50% higher chance of having a premature infant than white or Hispanic parents. And while preterm births may have coincided with remote work, that would not apply for the essential workers who continued their employment throughout lockdowns.
Regarding preterm birth outcomes during the pandemic, Gupta said that once scientists break down data by demographics, social determinants of health, and medical comorbidities, he expects there will be a “variety of outcomes.” There is no real-time, national birth surveillance data in the U.S. — so it will take time to understand these outcomes fully.
As far as the theories about which factors may have impacted preterm birth, Joseph said that “mostly, these data have led to more hypothesis generation than anything else more conclusive.”
Gupta agreed, adding that there is more research to be done about both the impacts of COVID-19 infection, as well as the indirect effects of the pandemic.
“I think we really have to better understand what factors during COVID — including lockdowns, unemployment, social interactions, mental health, adherence to medications, job loss — all played a role,” he said. “I think we should not take any of these one factors for granted.”
Source: https://www.medpagetoday.com/special-reports/exclusives/92000

Rituals
Our favorite rituals have stories to tell.
Strengthening personal rituals that we experience as grounding, foundational, and self-affirmative may help us navigate through these challenging times.
Rituals are a feature of all known human societies. They include not only the worship rites and sacraments of organized religions and cults, but also rites of passage, atonement and purification rites, oaths of allegiance, dedication ceremonies, coronations and presidential inaugurations, marriages, funerals and more.
Source: https://en.wikipedia.org/wiki/Ritual
Healthy rituals provide comfort, stability, connection and empower our personal and collective presence in the world. We all have rituals, although we may not see them as such. A child is born and with it are born many and diverse rituals of interaction between the child and those who care for it. When a loved one dies, time stops as we pick up the phone to check in or share a story with the deceased and suddenly remember that the ritual and rhythm of connecting with our loved one has also transpired, at least in that form.
Communities and cultures share rituals and in sharing may strengthen the ability of the community to heal, grow, and experience prosperity and wellness. Rituals have the capacity to build resilience. Connecting with the self within the Source empowers our capacities to survive and thrive. It is a process of plugging in, recharging, transmitting and receiving.
I like to pick up a local coffee early in the morning. I do not especially like coffee but I love the aroma of coffee beans that have ventured to my neighborhood from so many places in the world. My hands cherish the warmth of the cup they enfold. That first sip of coffee in the morning is my Namaste, my deep breath, my bow to the Divine that connects All. And then …. on with the day.
Your favorite ritual?
Mundan Ceremony

Approved by the BabyCenter India Medical Advisory Board
A mundan or tonsuring is an important ceremony for Hindus. It is also known as chaula or choodakarana. Mundan is shaving off baby’s first hair or the birth hair.
Muslims too shave or trim the baby’s hair and some Sikhs perform the kesi dahi ceremony. This is done by putting curd in the hair of the newborn baby boy.
Among Hindus, the mundan is performed during the first or third year of a child’s life. In some regions, the mundan is done only for the male child. However, in most families girls have a mundan too.
Why is a mundan performed?
In most communities a mundan or first haircut is done in the belief that it purifies the child. Many also believe that a mundan:
- rids the baby of his past life’s negativity
- bestows a long life and a good future
- protects the child from the evil eye
- cleanses the child’s body and soul
- helps to keep the baby’s head cool, especially in hot summer months
- helps relieve headache and pains caused by teething
- improves the growth of the baby’s hair
Source:https://www.babycenter.in/a1015415/imundani-ceremony
Countries that are predominantly composed of nuclear family (father, mother and the children) units represent a limited portion of our global family. In most cultures extended families (grandparents, father, mother, children, aunts, uncles, cousins, other kin and even neighbors are considered to be “family” and hold significant responsibility in supporting the care and development of the child. This joyous ceremony sweetly highlights the extended family engagement in a child’s life journey.
Ronav’s Mundan Ceremony
Jan 20, 2019

PREEMIE FAMILY PARTNERS
The Surgeon and the Mother
Heather Carmichael, M.D
This article was published on January 23, 2021, at NEJM.org

“Just that,” said the fox. “To me you are still nothing more than a little boy who is just like a hundred thousand other little boys. And I have no need of you. And you, on your part, have no need of me. To you, I am nothing more than a fox like a hundred thousand other foxes. But if you tame me, then we shall need each other. To me, you will be unique in all the world. To you, I shall be unique in all the world.” — Antoine de Saint-Exupéry
I did not get to hold you for the first 3 weeks of your life.
I knew this would happen. I was the surgeon, and I was prepared. You were born under the bright fluorescent lights of an operating room, delivered onto a sterile blanket on my belly. There, the intensivist began to work on you before you had taken your first breath. Before you had been separated from me, a tube was placed down your tiny throat. Before I had a chance to cry, you were whisked away to the adjacent room, where all the others — surgeons, intensivists, nurses, fellows, residents, respiratory therapists, students, your father — crowded around. And I was left alone, with the obstetrician and a nurse, waiting under the cold lights to deliver the placenta.
I was prepared. I was a surgeon, or at least a surgeon in training, and I knew this room. My hospital ID was tucked into the pocket of my bathrobe. I knew the timing of morning rounds, the hierarchy, the jargon. I had done this before. I knew how to neatly package my emotions in the glove compartment until the end of the day, avoiding any clutter that might get in the way of sound clinical judgment.
I knew, for example, that I shouldn’t cry in the exam room at my 20-week ultrasound when I heard that you had a congenital diaphragmatic hernia, that your stomach, intestines, spleen, and liver were all up in your chest. I bit back my tears until I reached the safety of my own car on the roof of the parking garage. I had done this before.
Sometime after the delivery, I was taken back to a recovery room. The nurse brought me a breast pump; a lactation consultant walked me through the pages of a pamphlet. I sat in the quiet dark, listening to the tick-tick-tick-tick of the machine counting out the requisite time. I thought about you, but I was the surgeon, and to me you were some other mother’s baby, one of many fighting for your life down that long, narrow hallway of the NICU. The nurse praised me for those few drops of colostrum, filling up the tiny syringe.
You needed to be put on ECMO, a machine to take over for your heart and lungs, sucking all the blood out of your miniature vessels and pumping it back in again. As a surgeon, I knew what this meant. I knew what would happen, the steps of the operation, the risks, the potential benefits, the alternatives, the lack of alternatives. I watched it happen through the glass door, across the hall by the nurses’ station, some strange dream. You under a sea of blue, the surgeon and the fellow with their heads bowed together over your tiny face. When it was over, I was instructed that I could touch your hands, your feet, gently cup the top of your head, but that I should not stroke your dark curls, or kiss your cheek, or squeeze your small fingers. I looked at your body, your eyes closed in a sedated sleep, but I did not experience those instant warm feelings of a mother gazing on her child.
Every 3 hours, I took out the pump and sat on the couch, tucked away in the back of your room, hidden by all the machines but with no true privacy. A steady stream of specialists, nurses, residents came through the glass doors, peering at your quiet form through the mass of wires, tubes, lines, and drains. The soft tick-tick-tick-tick of the pump was drowned out by the engine roar of the ventilator, like steady gunfire. There was no joy in this task, but there was some small comfort in its perfunctory nature, some sense of achievement from the steadily growing volumes collected with small syringes, containers, bottles that I could label and deposit neatly in plastic bags. It had the same routine, familiar steps, boxes to be checked. An echo of the way I kept my life organized at work.
When we were alone, I read to you. Here, there was some hesitation, some fear. I did not know if I wanted you to become a child, my child, whom I could love and therefore lose. It was easier to see you as a patient, to imagine that you were that other baby, the one I cared for in the same room just a few years earlier, when I was an intern diligently holding a retractor for the same operation you had at just 2 days old.
But slowly, over those first weeks, my surgical armor shifted, slipped, cracked. As you gradually opened your eyes and looked into mine, as I felt your tiny but firm hand clasp around my finger, you slowly claimed me as your own. Machines left the room, revealing the soft tick-tick-tick-tick of the breast pump, and the milk that I produced was drawn up neatly into syringes and slowly drained into the tube snaked across your face. Eventually, I could hold you, and bury my face in your hair, and smell your soft-sour scent.
And suddenly you were a child, my son. And I could love and therefore lose you.
Source: https://www.nejm.org/doi/full/10.1056/NEJMp2029239

Parents Are “Essential” Caregivers
Around the world, neonatal intensive care units (NICUs) had to adjust many of their routine practices due to coronavirus disease-2019 (COVID-19) while trying to continue to provide excellent care for newborns and their families. Prior to COVID-19, most NICUs used family-centered care as the framework to engage parents in infant caregiving. However, due to the need for urgent implementation of COVID-19 crisis management procedures in early 2020, family-centered policies regarding parental presence in the NICU were quickly modified to restrict parents’ presence at the bedside. New policies varied from unit to unit and even changed over time, as we learned more about how the virus spreads. Yet, as 2020 turned into 2021, many of the restrictive parent presence policies have been slow to return to prepandemic standards despite an increased understanding of the virus spread, implementing safety protocols for healthcare workers that could have been adapted for parents, and knowing that parents as caregivers are essential to excellent neonatal care. Infants develop best when they are emotionally and physically attached to their parents. Parent presence and participation in care results in improved outcomes for both newborns and parents. Randomized controlled trials that employed family-centered care interventions resulted in increased newborn weight gain, decreased readmissions, and decreased parental anxiety, depression, and stress.
During the pandemic, some of the reported restricted parental presence policies included: allowing only one parent to visit at a time; decreased mothers’ presence to 2 hours per day; and, limiting fathers’ presence to 1 hour per week. In one cross sectional survey of 277 NICUs, parental presence 24 hours per day 7 days per week decreased from 83% to 53%. These strict restrictions have led to parents requesting to be allowed back into NICUs.For example, after an informal survey of parents revealed concerns about family restrictions during the pandemic, the Vermont Oxford Family Faculty spoke out and stated that parents should be allowed back in the NICU to participate in care. Jennifer Canvasser, a former NICU parent who lost her son to necrotizing enterocolitis in 2012 and founder and director of The NEC Society, wrote about the importance of parental presence in the NICU to ensure shared decision-making at the bedside. Both the Vermont Oxford Family Faculty and Canvasser asked that partnerships with parents to be recognized during these complicated times. As NICUs grappled with these decisions, NICUs could have looked to use guidance from experts, such as the Institute for Patient and Family-Centered Care (IPFCC), to help make sure that parents were included in decisions at both the bedside and at the hospital level through the use of the IPFCC’s pandemic planning resources.
As in most pandemic work environments, extended use of technology is already in place in the NICU and new online platforms played a major role in connecting with families due to limited parental presence. Technology may have been an appropriate early solution to parent engagement as units learned about the pandemic, yet it was never meant to replace in-person visits. Seeing their newborn during physical separation may have been helpful to parents; however, it was insufficient. Parental presence as an active caregiver fosters infants’ security and parent–infant attachment.
As neonatal nurses we must continue to advocate for parents to be fully involved in their newborn’s care and ensure that parents feel supported throughout the NICU stay. That is why NANN has joined with the National Perinatal Association and the Association of Women’s Health Obstetric and Neonatal Nurses Association in the Consensus Statement on Family Presence in Neonatal Intensive Care Units.11 During the pandemic, the parent/caregiver role has not been seen as “essential” and parental presence in the NICU was not as hardwired into our culture as many would have liked to believe. We must now fully embrace parents as “essential caregivers” to the care of their infants in the NICU and avoid slipping back into the habit of labeling parents as visitors. Parents need supported in their need to be able to routinely participate in their newborn’s NICU care. We need to advocate for the holistic care of newborns, parents, and families to support our family-centered decisions at the unit, local, and national levels. Parents are essential; they must become the “constant” and not the “visitor.” It is now time for all neonatal clinicians to partner with parents so that infants and families can fully benefit from family-centered care.
Behr, Jodi Herron PhD, APRN, RNC-NIC, ACCNS-P; Brandon, Debra PhD, RN, CCNS, FAAN; Co-Editor; McGrath, Jacqueline M. PhD, RN, FNAP, FAAN; Co-Editor Parents Are “Essential” Caregivers, Advances in Neonatal Care: April 2021 – Volume 21 – Issue 2 – p 93-94 doi: 10.1097/ANC.0000000000000861

7 precautions to be taken by a high-risk pregnancy patient

By Dr Gandhali Deorukhkar –Wednesday, April 21, 2021
Accepting your condition is the first step to dealing with a high-risk pregnancy.
Given the current lifestyle and work culture, many women are undergoing high-risk pregnancies. If you are someone with a high-risk pregnancy, the emotional roller-coaster is a part of the package. Although anxiety and stress are inevitable, there is really no dire need to get too worked up about your high-risk pregnancy. With the development of amazing medical facilities and regular prenatal care, you can have a healthy baby with a safe outcome despite your high risk.
Here are 7 precautions you need to follow to have a healthy baby.
Acceptance
Accepting your condition is the first step to dealing with a high-risk pregnancy. Knowing that you have to handle a high-risk pregnancy makes you well aware and better prepared. You know what you are getting into. You understand all the essential complications well. If you remain in denial, then you cannot judge the red flags and you will miss out on essential treatment.
Trust
The key to handling a high-risk pregnancy is to trust your doctor. Have faith in your physician that they want the best for you and will advise the same. Reading articles on the internet or listening to other family and friends providing their unsolicited advice will only make things worse. You need to listen only to the expert. Avoid reading unnecessary information online and stop confusing your mind. Better option is to get all your queries solved by the gynaecologist herself.
Consistency
Be consistent with your management plan. Take your medicines on time. Do not miss out on any of the supplements. All are essential and critical for the growth of your healthy baby. In case of any adverse side-effects, inform your physician right away. Do not hesitate to consult your physician for any complaint. Give a detailed history of all the issues that you are facing in your high-risk pregnancy.
Strict control
Diet is an essential part of a healthy lifestyle. Given your high-risk pregnancy, it is even more necessary to follow a healthy diet. Do not give in to all your cravings. Moderation is key. Control your portion size and limit your intake of fatty and sugar-filled foods. Junk food is completely off the table. In case you have conditions like gestational diabetes, you may have to go off of sugar entirely. Women with hypertension during pregnancy, which is known as eclampsia and pre-eclampsia, need to be careful about their salt intake. You may also be advised for complete bed rest owing to the severity of your condition. Hence, it is better to follow a strict diet plan to avoid all such added flavours of salt and sugar.
Exercise regime
Exercise helps your body stay fit mentally and physically. But if you have been diagnosed with a high-risk pregnancy and are suffering from a low-lying placenta, it is advised not to carry out yoga and antenatal exercises. Consult your gynaecologist about the exercises that are allowed for your case and follow them to the T.
Vigilance
Know your symptoms well. Understand the side-effects and symptoms of any complications that may arise, so that you are better prepared to inform your physician right away. If there is any kind of spotting or bleeding or any sudden pain with decreased baby movement, report to your gynaecologist right away. This way, you can avoid all complications at an earlier stage itself.
Readiness
Be prepared with all the necessary essential items you require post-delivery. Pack your hospital bag well in advance as you never know when you may deliver with a high-risk pregnancy. Most cases have a proactive birth plan ready. But in case of an emergency, you are ready and good to go without the hassle of packing at the last minute.
Most importantly, have a strong support system with you. You need someone you can communicate with and share all your worries with. They just need to be there listening to you and helping you stay calm and relaxed. Listen to your body and your baby. They will guide you in the right direction. Maintain your regular visits to the gynaecologist and get all your doubts solved. Stay happy and keep smiling for a healthy pregnancy and complication-free delivery. Remember, a stress-free pregnancy is a happy pregnancy.
(The writer is Gynecologist, Wockhardt Hospital, Mumbai Central)

INNOVATIONS

Two Indias: The structure of primary health care markets in rural Indian villages with implications for policy
Available online 15 June 2020, 112799
Abstract
We visited 1519 villages across 19 Indian states in 2009 to (a) count all health care providers and (b) elicit their quality as measured through tests of medical knowledge. We document three main findings. First, 75% of villages have at least one health care provider and 64% of care is sought in villages with 3 or more providers. Most providers are in the private sector (86%) and, within the private sector, the majority are ‘informal providers’ without any formal medical training. Our estimates suggest that such informal providers account for 68% of the total provider population in rural India. Second, there is considerable variation in quality across states and formal qualifications are a poor predictor of quality. For instance, the medical knowledge of informal providers in Tamil Nadu and Karnataka is higher than that of fully trained doctors in Bihar and Uttar Pradesh. Surprisingly, the share of informal providers does not decline with socioeconomic status. Instead, their quality, along with the quality of doctors in the private and public sector, increases sharply. Third, India is divided into two nations not just by quality of health care providers, but also by costs: Better performing states provide higher quality at lower per-visit costs, suggesting that they are on a different production possibility frontier. These patterns are consistent with significant variation across states in the availability and quality of medical education. Our results highlight the complex structure of health care markets, the large share of private informal providers, and the substantial variation in the quality and cost of care across and within markets in rural India. Measuring and accounting for this complexity is essential for health care policy in India.
Source:https://www.sciencedirect.com/science/article/pii/S0277953620300186

Reproductive risks in 35-year-old adults born very preterm and/or with very low birth weight: an observational study
Van der Pal, S.M., van der Meulen, S.A., Welters, S.M. et al. Reproductive risks in 35-year-old adults born very preterm and/or with very low birth weight: an observational study. Eur J Pediatr 180, 1219–1228 (2021).
Abstract
Evidence suggests that increased survival over the last decades of very preterm (VPT; gestational age < 32 weeks)– and very low birth weight (VLBW; birth weight < 1500 g)–born infants is not matched by improved outcomes. The objective of our study was to evaluate the reproductive rate, fertility, and pregnancy complications in 35-year-old VPT/VLBW subjects. All Dutch VPT/VLBW infants born alive in 1983 and surviving until age 35 (n = 955) were eligible for a POPS-35 study. A total of 370 (39%) subjects completed a survey on reproductive rate, fertility problems, pregnancy complications, and perinatal outcomes of their offspring. We tested differences in these parameters between the VPT/VLBW subjects and their peers from Dutch national registries. POPS-35 participants had less children than their peers in the CBS registry. They reported more problems in conception and pregnancy complications, including a three times increased risk of hypertension during pregnancy.
Conclusion: Reproduction is more problematic in 35-year olds born VPT/VLBW than in the general population, possibly mediated by an increased risk for hypertension, but their offspring have no elevated risk for preterm birth.
| What is known: At age 28, the Dutch national POPS cohort, born very preterm or with a very low birth in 1983, had lower reproductive rates than the general Dutch population (female 23% versus 32% and male 7% versus 22%). What is new: At age 35, the Dutch POPS cohort still had fewer children than the general Dutch population (female 56% versus 74% and male 40% versus 56%). Females in the POPS cohort had a higher risk of fertility problems and pregnancy complications than their peers in the Dutch national registries, but their offspring had no elevated risk for preterm birth. |
Source: https://link.springer.com/article/10.1007/s00431-020-03864-5#citeas


Improving thermoregulation in transported preterm infants
POSTED ON 08 MARCH 2021
Infants born preterm (<37 weeks of gestation) or with a low birthweight (<2.5 kg) are at high risk for decreasing body temperature during transportation to the hospital. Hypothermia in preterm infants is a risk factor for increased mortality and morbidity (e.g. respiratory distress syndrome). Therefore, effective thermoregulation during transport is of outmost importance.
In the study by Glenn et al., interventions were developed to increase the efficacy of thermoregulation in transported newborn infants. Close collaboration with the transportation teams at the University Hospitals Rainbow Babies and Children’s Hospital in Cleveland, USA, was key, which lasted from January 2016 to December 2019. A total of 380 infants were included in the study, with a range in gestational age of 22 to 40 weeks and a weight range of 420g to 4220g. 229 of the infants were born preterm or with low birthweight.
The first 17 months of the study were used to gather baseline data, revealing an average of only 60% of preterm or low birthweight infants, who were admitted to the NICU with normal temperature (36.5°C – 37.5°C). Afterwards, together with a multidisciplinary team consisting of neonatologists, transport staff and paediatricians, Glenn et al. reviewed the transport protocols and chose a new set of interventions. These included controlling the heat of the transport incubator, using plastic wrap, exothermic warming mattresses, and temperature monitoring. For the intervention, the team used the Voyager Airborne Transport Incubator and Velcro closure wrap.
Furthermore, interventions included a check of temperature before the start of transport, and checking it continuously if it was outside the acceptable range. Feedback of the transport team indicated that most infants who arrive hypothermic at the NICU were already in this state at the beginning of transport. Staff members had difficulties normalising the temperature during transportation. Therefore, a supply checklist, increase of temperature in the operating room and immediate notification of the transport team of an upcoming delivery were implemented to address these difficulties. Additionally, and in response to the feedback, the heat of the transport incubator was made adjustable from 32-37°C depending on the infant’s weight and age (<1 day or >1 day) to meet their individual needs.
Overall, the interventions resulted in an increase by 36% (from 60% to 96%) of infants admitted within normal temperature range This could be achieved through educating staff on the importance of temperature control and by making only minor changes to thermoregulation. Especially when resources are low, interventions like using the plastic wrap are an effective way to prevent hypothermia in neonates during transport.
One of the limitations of this study is its dependency on the documentation of the transport staff. Thus, in some cases, performed interventions may not have been recorded. Nevertheless, the great increase in newborns who were admitted to the NICU within the goal temperature of 36.5°C to 37.5°C shows that the interventions were successful.
Paper available at: Journal of Perinatology
Full list of authors: Tara Glenn, Rhonda Price, Lauren Culbertson, Gulgun Yalcinkaya
DIO: 10.1038/s41372-020-0732-z
Source: https://www.efcni.org/news/improving-thermoregulation-in-transported-preterm-infants
Scientific Duo Gets Back To Basics To Make Childbirth Safer
February 18, 2019
Their research is still in early stages, but Kristin Myers (left), a mechanical engineer, and Dr. Joy Vink, an OB-GYN, both at Columbia University, have already learned that cervical tissue is a more complicated mix of material than doctors ever realized. –Adrienne Grunwald for NPR
Brittney Crystal was just over 25 weeks pregnant when her water broke.
It was her second pregnancy — the first had been rough, and the baby came early.
To try to avoid a second premature birth, Dr. Joy-Sarah Vink, an obstetrician and co-director of the Preterm Birth Prevention Center at Columbia University Medical Center, arranged for Crystal to be transported by ambulance from her local Connecticut hospital to New York City, where Vink could direct her care.
Two weeks later Crystal started having contractions. She was given magnesium sulfate to stop them, and made it through the night. Crystal believed there was a future for her coming baby, whom she had named Iris.
“I went to the mirror and I talked to Iris,” Crystal says. “I said, ‘you know, this was a rough day. … You’re going to have them. But then the next day comes and the sun comes up and we move forward.’ “
That evening, however, the contractions started again. Crystal was whisked to an operating room for a Cesarean section. She was a little under 28 weeks pregnant.
“I think I knew before I opened my eyes that she had died,” Crystal says, her voice cracking as she reaches for a tissue.
Afterward, as she was recovering in the hospital and mourning the loss of Iris, Crystal and her family asked a lot of questions. Why can’t you seal up the amniotic sac if your water breaks early? Why can’t you reliably stop preterm labor?
“And that’s when Dr. Vink told us that, you know, rare diseases are being cured in this day and age, but we don’t know what triggers full-term labor,” Crystal recalls. “That just collectively blew away everyone in the room.”
It was surprising but true. When it comes to pregnancy, research on some basic questions stalled decades ago, Vink says. If a pregnancy is normal, that doesn’t matter much. But when things go wrong, those gaps in knowledge become issues of life and death.
“It’s mind-boggling that in this day and age, we still don’t understand [even] in a normal pregnancy how women go into labor — what triggers labor,” Vink says. “Because we don’t understand the normal fundamental mechanisms, we can’t identify how things go bad — and then how we fix it when things go bad.”
Crystal, for example, had undergone a procedure called cervical cerclage: Vink had stitched Crystal’s cervix closed in hopes of preventing it from opening too soon. The technique has been around for more than 40 years, and it’s about the only treatment available for what doctors call “an incompetent cervix.” But much of the time, it’s not enough to stop a premature birth.
Most basic knowledge about pregnancy comes from research performed in the 1940s, Vink says, and she’s working hard to update that information.
She’s focused first on the cervix, she says, because if doctors can get the cervix to stay closed in those final, crucial weeks of gestation, the baby won’t be born too soon, even if the amniotic sac breaks.
“So, what is the cervix made out of? What proteins are there, what cells are there? How are all these things interacting? How do they change in pregnancy?” she asks, laying out some of the unknowns. By the end of pregnancy, a woman’s cervix goes from being stiff, like the tip of a nose, to very soft. But how?
To help answer those questions, Vink and her graduate researchers are taking, for analysis, cervical tissue samples from women in her medical practice who are at different stages of pregnancy.
One of her first findings, she says, is that the cervix is not made mostly of collagen, as doctors long thought. It also has a lot of muscle, especially near the very top.
While Vink studies what the cervix is made of, one of her university colleagues, mechanical engineer Kristin Myers, is trying to determine how it works.
“I’m kind of an oddball in the department of obstetrics and gynecology,” Myers says. “I teach mechanics classes and design classes here at Columbia.”
Myers got her start as an undergraduate, doing materials research in the automobile industry. Back then she tested how tires respond to heat.
“So if you take rubber and you heat it up and you pull on it, it gets really, really soft — and then it breaks,” Myers says.
That reaction reminded her adviser of how a bulging aneurysm bursts. He suggested she focus her curiosity on the mechanics of the human body. When she arrived at MIT for her graduate studies, Myers worked with researchers who were interested in the mechanics of pregnancy.
“It’s an important area — an understudied area — and a basic part of pregnancy physiology,” says Dr. Michael House, an OB-GYN at Tufts Medical Center who also has a background in engineering. “There is just lots to learn.”
House has been a mentor to Myers and continues to collaborate with her. He says the focus on the cervix is particularly important, “because a cervix problem can affect the pregnancy very early.”
About 1 in 10 babies are born prematurely in the U.S. each year. If those babies are born close to term — after around 35 weeks — they can do quite well. But a woman with a problematic cervix can go into labor much sooner, which can lead to miscarriage or a baby born so early that the child may die or face lifelong health problems.
Myers is investigating several aspects of the biomechanics of pregnancy — from how much the uterus can stretch, to how much pressure pregnancy exerts on the cervix, to how much force a baby’s kick puts on the whole system.
“We’re building computational models of female pregnancy to answer those questions,” Myers says.
She has two labs at Columbia — one at the hospital and one in the engineering school. In the lab at the engineering school there are a variety of microscopes and scalpels and slides. There’s one machine that can inflate the uterine membranes like a balloon, and another, about the size of a microwave, that stretches uterine tissue between two grips.
“These [are] types of machines you’ll see in all different kinds of material testing labs,” Myers explains. “In civil engineering you can have one of these machines that is like two or three stories high and they’re testing the mechanical strength of, [say], railroad ties.”
She is measuring just how much the cervical tissue changes during pregnancy — starting out with the capability and consistency of a tendon, and becoming something more like a loose rubber band.
“We’ve mechanically tested various pregnant tissues and nonpregnant tissues of the cervix,” Myers says, “and its stiffness changes by three orders of magnitude.”
All those measurements go into a databank. And when women in Vink’s practice get an ultrasound, the technicians spend an extra few minutes measuring the mother’s anatomy, as well as the baby’s, and send that information to Myers, too.
Then the team uses their computer models to look at how the various factors — shape, stretch, pressure and tissue strength — interact as a woman moves toward labor and childbirth.
Their goal is to be able to examine a pregnant woman early on, and accurately predict whether she will go into labor too soon. It’s a first step, Vink hopes, toward better interventions to stop that labor.
That’s what Brittney Crystal is aiming for as well. After baby Iris died, Crystal started a foundation called The Iris Fund, which has raised more than $150,000 for Vink’s and Myers’ research.
“She didn’t get to have a life,” Crystal says. “But we really want her to have a very strong legacy.”

LuSi Video Brochure
Apr 16, 2021 LuSi neosim
LuSi is a Lung simulator to train clinicians in the assessment of lung function and the application of respiratory therapy without risk to patients. LuSi responds to treatment without operator intervention and can simulate pathologies like RDS, lung collapse, weak muscular activity, pneumothorax, airway obstruction, etc. The vital signs parameters are calculated based on actually measured values such as pressure, flow and volume plus case-specific pathology like dead space, CO2 production and lung compliance. LuSi reacts to therapy without need for an operator – no technician is needed in the background to change oxygen saturation or arterial PCO2 – because LuSi is autonomous. The embedded real-time artificial intelligence makes her the only autonomous lung simulator in the world. LuSi can be used in the hospital setting or out of hospital in any training facility because it does not need CO2 gas nor actual monitoring equipment.

HEALTHCARE PARTNERS
Who’s on First? Split and Shared Services in the NICU
Scott D. Duncan, MD, MHA Professor and Chief Division of Neonatal Medicine University of Louisville
The baseball analogy is appropriate in neonatology, as the provision of neonatal care is a team sport, including, but not limited to, physicians, advanced practice providers, nursing, nutritionists, pharmacists, respiratory therapists, speech therapists, physical therapists, and social workers. In many instances, the neonatologist’s role has undergone significant modifications, with an increasing role of advanced practice providers, as well as a reduction in trainee rotations and restrictions on work hours.
Scenario
In the batter’s box, the delivery team attends the delivery of a 32- week gestation infant due to maternal gestational diabetes and pre-eclampsia. The delivery team includes two nurses, a respiratory therapist, and a neonatal nurse practitioner (NNP) as the team leader. In the delivery room, the infant requires intubation and positive pressure ventilation. The infant is admitted to the NICU on a ventilator. By 30 minutes of age, the infant demonstrates increasing respiratory distress, hypercarbia, and the CXR reveals severe RDS. The NNP orders surfactant therapy.
While making rounds with the fellow and resident team, the neonatologist asks the NNP about the patient. The NNP gives the neonatologist a verbal report and completes the electronic medical record’s history and physical (EMR). Following rounds, the neonatologist examines the infant and places a macro-based attestation used for resident documentation on the H&P, co-signs the note, and uses the charge capture feature on the EMR to place a 99468 code for the date of admission.
A Strikeout
Strike One – The neonatologist provided limited services in the assessment and care plan.
Strike Two – A NNP is not a trainee, and Physician at Teaching Hospital (PATH) guidelines do not apply for documentation and attestations.
Strike Three – The service for the day is an initial critical care charge, and split/shared services are prohibited with critical care delivery.
Discussion
In this Scenario, the neonatologist made multiple errors as related to split/shared services and supervision. A split/shared service is an encounter where a physician and the NNP from the same group and same specialty each personally perform a portion of an Evaluation and Management (E/M) visit. As applied to in-patient neonatology, the split/shared E/M rule applies only to selected E/M visits such as these in the hospital settings:
• hospital admissions (CPT® codes 99221-99223)
• subsequent hospital visits (CPT® Codes 99231-99233)
• discharge management (CPT® Codes 99238-99239).
In the case of critical care, split/shared services are not allowed. The guidance provided by the US Department of Health and Human Services states, “Critical care services are reflective of the care and management of a critically ill or critically injured patient by an individual physician or qualified non-physician practitioner for the specified reportable period of time. Unlike other E/M services where a split/shared service is allowed, the critical care service reported shall reflect the evaluation, treatment, and management of a patient by an individual physician or qualified non-physician practitioner [NPP] and shall not be representative of combined service between a physician and a qualified NPP.” (1)
Appropriate documentation must substantiate the nature of the admission. Per the recommendations of the AAP Committee on Coding and Nomenclature, (2) the medical record documentation should include:
• Documentation of the critical status of the infant
• Documentation of the bedside direction and supervision of all aspects of care
• Review of pertinent historical information and verification of significant physical findings through a medically indicated, focused patient examination
• Documentation of all services provided by members of the care team and discussion and direction of the ongoing therapy and plan of care for the patient
• Additional documentation of any major change in a patient course requiring significant hands-on intervention by the reporting provider
Split/shared services may be utilized for E/M services, hospital admissions, subsequent hospital visits, and discharge, as noted above. In these instances, the providers should each document their portion of the service provided. Charges may be placed using the following rules:
• When the physician provides any face-to-face portion of the encounter, use either provider’s NPI
• When the physician does not provide a face-to-face encounter, use the NNP’s NPI
Revised Scenario – a pinch hitter At the plate, the delivery team attends the delivery of an infant of 32-week gestation due to maternal gestational diabetes and preeclampsia. The delivery team includes two nurses, a respiratory therapist, and a neonatal nurse practitioner (NNP) as the team leader. In the DR, the infant requires PPV and intubation. The infant is brought to the NICU on assisted ventilation. By 30 minutes of age, the infant demonstrates increasing respiratory distress, hypercarbia, and the CXR reveals severe RDS.
While making rounds with the fellow and resident team, the neonatologist asks the NNP about the patient. The NNP gives the neonatologist a verbal report, and the neonatologist leads the rounding team to the patient’s bedside, where a complete examination is performed. The neonatologist orders surfactant replacement, and following rounds completes a history and physical, including the assessment and plan, in the EMR, independent of documentation by the NNP. The neonatologist uses the charge capture feature on the EMR to place a 99468 charge for the date of admission. A Home Run!
Source: http://neonatologytoday.net/newsletters/nt-apr21.pdf

Preterm birth, neonatal therapies and the risk of childhood cancer

Laura K Seppälä1, Kim Vettenranta2, Maarit K Leinonen3, Viena Tommiska4, Laura-Maria Madanat-Harjuoja5doi: 10.1002/ijc.33376. Epub 2020 Nov 11.
Abstract
Our aim was to study the impact of preterm birth and neonatal therapies on the risk of childhood cancer using a nationwide, registry-based, case-control design. Combining population-based data from Finnish Medical Birth Registry (MBR) and Finnish Cancer Registry, we identified a total of 2029 patients diagnosed with cancer under the age of 20 years and 10 103 age- and sex-matched controls over the years 1996 to 2014. Information on the prenatal and perinatal conditions was obtained from the MBR. Gestational age was categorized into early (<32) and late preterm (32-36) and term (≥37 weeks). Cancer risk among the preterm compared to term neonates was evaluated using conditional logistic regression. We identified 141 cancers among the preterm (20.8% of 678) vs 1888 cancers in the term children (16.5% of 11 454). The risk of any cancer was increased for the preterm (odds ratio [OR] 1.28, 95% confidence interval [CI] 1.06-1.57), especially for the early preterm (OR 1.84, 95% CI 1.16-2.92). The risk of acute myeloid leukemia (AML; OR 2.33, 95% CI 1.25-4.37), retinoblastoma (OR 3.21, 95% CI 1.22-8.41) and germ cell tumors (OR 5.89, 95% CI 2.29-15.18) was increased among the preterm compared to term. Germ cell tumors were diagnosed at a significantly younger age among the preterm. Neonatal therapies, for example, mechanical ventilation, were associated with an increased risk of childhood cancer independent of gestational age. Preterm, especially early preterm birth, is associated with an increased risk of childhood cancer, especially germ cell tumors and AML. Respiratory distress requiring neonatal intervention also appears to be associated with an increased risk.
Source: https://pubmed.ncbi.nlm.nih.gov/33128776/
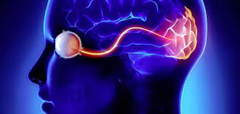
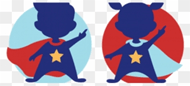
Preterm Birth and the Development of Visual Attention During the First 2 Years of Life

A Systematic Review and Meta-analysis
Or Burstein, MA1; Zipi Zevin, BA1; Ronny Geva, PhD1,2
JAMA Netw Open. 2021;4(3):e213687. doi:10.1001/jamanetworkopen.2021.3687 – March 30, 2021
Key Points
Question Is preterm birth associated with visual attention impairments in early life, and if so, in which attention functions?
Findings This systematic review and meta-analysis of 53 studies including 2047 preterm-born and 1951 full-term–born neonates and infants found that preterm birth was significantly associated with impairments in visual attention functioning. Despite a short-term advantage in visual-following in preterm infants, deficits cascaded from basic orienting responses to focused attention during the first 2 years of life.
Meaning The findings suggest that preterm birth is associated with challenges in the development of visual attention beginning in the early stages of life.
Abstract
Importance Preterm birth is associated with an increased risk for long-lasting attention deficits. Early-life markers of attention abnormalities have not been established to date but could provide insights into the pathogenesis of attention abnormalities and could help identify susceptible individuals.
Objective To examine whether preterm birth is associated with visual attention impairments in early life, and if so, in which attention functions and at which developmental period during the first 2 years of life.
Data Sources PubMed and PsycINFO were searched on November 17, 2019, to identify studies involving visual attention outcomes in infants born preterm vs full term.
Study Selection Peer-reviewed studies from the past 50 years met the eligibility criteria if they directly assessed visual attention outcomes until the age of 2 years in generally healthy infants born preterm or full term. The selection process was conducted by 2 independent reviewers.
Data Extraction and Synthesis The Meta-analysis of Observational Studies in Epidemiology (MOOSE) reporting guideline was followed. Random-effects models were used to determine standardized mean differences. The risk of bias was assessed both within and between studies.
Main Outcomes and Measures Five nascent indices of visual attention were analyzed, including very basic functions—namely, the abilities to follow and fixate on visual targets—and more complex functions, such as visual processing (ie, habituation), recognition memory (ie, novelty preference), and the ability to effortfully focus attention for learning.
Results A total of 53 studies were included, with 69 effect sizes and assessing a total of 3998 infants (2047 born preterm and 1951 born full term; of the 3376 for whom sex was reported, 1693 [50.1%] were girls). Preterm birth was associated with impairments in various attention indices, including visual-following in infancy (Cohen d, −0.77; 95% CI, −1.23 to −0.31), latency to fixate (Cohen d, −0.18; 95% CI, −0.33 to −0.02), novelty preference (Cohen d, −0.20; 95% CI, −0.32 to −0.08), and focused attention (Cohen d, −0.28; 95% CI, −0.45 to −0.11). In the neonatal period, preterm birth was associated with superior visual–following (Cohen d, 0.22; 95% CI, 0.03 to 0.40), possibly owing to the additional extrauterine exposure to sensory stimulation. However, this early association waned rapidly in infancy (Cohen d, –0.77; 95% CI, –1.23 to –0.31).
Conclusions and Relevance The findings suggest that preterm birth is associated with impingements to visual attention development in early life, as manifested in basic and then complex forms of attention. Advancements in neonatal care may underlie improvements found in the current era and accentuate several early protective factors.

Building capacities of Auxiliary Nurse Midwives (ANMs) through a complementary mix of directed and self-directed skill-based learning—A case study in Pune District, Western India
Shilpa Karvande, Vidula Purohit, Somasundari Somla Gopalakrishnan, B. Subha Sri, Matthews Mathai & Nerges Mistry Human Resources for Health volume 18, Article number: 45 (2020)

Abstract
Auxiliary nurse midwives (ANMs) play a pivotal role in provision of maternal and newborn health at primary level in India. Effective in-service training is crucial for upgrading their knowledge and skills for providing appropriate healthcare services. This paper aims at assessing the effectiveness of a complementary mix of directed and self-directed learning approaches for building essential maternal and newborn health-related skills of ANMs in rural Pune District, India.
Methods
During directed learning, the master trainers trained ANMs through interactive lectures and skill demonstrations. Improvement and retention of knowledge and skills and feedback were assessed quantitatively using descriptive statistics. Significant differences at the 0.05 level using the Kruskal-Wallis test were analysed to compare improvement across age, years of experience, and previous training received. The self-directed learning approach fulfilled their learning needs through skills mall, exposure visits, newsletter, and participation in conference. Qualitative data were analysed thematically for perspectives and experiences of stakeholders. The Kirkpatrick model was used for evaluating the results.
Results
Directed and self-directed learning was availed by 348 and 125 rural ANMs, respectively. Through the directed learning, ANMs improved their clinical skills like maternal and newborn resuscitation and eclampsia management. Less work experience showed relatively higher improvement in skills, but not in knowledge. 56.6% ANMs either improved or retained their immediate post-training scores after 3 months.
Self-directed learning helped them for experience sharing, problem-solving, active engagement through skill demonstrations, and formal presentations. The conducive learning environment helped in reinforcement of knowledge and skills and in building confidence. This intervention could evaluate application of skills into practice to a limited extent.
Conclusions
In India, there are some ongoing initiatives for building skills of the ANMs like skilled birth attendance and training in skills lab. However, such a complementary mix of skill-based ‘directed’ and ‘self-directed’ learning approaches could be a plausible model for building capacities of health workforce. In view of the transforming healthcare delivery system in India and the significant responsibility that rests on the shoulder of ANMs, a transponder mechanism to implement skill building exercises at regular intervals through such innovative approaches should be a priority.
Source: https://human-resources-health.biomedcentral.com/articles/10.1186/s12960-020-00485-9



Get easily out of breath? It may be because you were small at birth, study finds

January 31, 2020 Karolinska Institutet
FULL STORY:
Babies born with low birth weights are more likely to have poor cardiorespiratory fitness later in life than their normal-weight peers. That is according to a study by researchers at Karolinska Institutet in Sweden published in the journal JAHA. The findings underscore the importance of prevention strategies to reduce low birth weights even among those carried to at term delivery.
Having a good cardiorespiratory fitness — that is ability of the body to supply oxygen to the muscles during sustained physical activity — is important for staying healthy and can reduce the risk of numerous diseases and premature death. Alarmingly, cardiorespiratory fitness is declining globally, both for youths and adults. A recent study showed that the proportion of Swedish adults with low cardiorespiratory fitness almost doubled from 27 percent in 1995 to 46 percent in 2017.
Given its implications for public health, there has been a growing interest in understanding the underlying causes of poor cardiorespiratory fitness. Researchers have identified both physical inactivity and genetic factors as important determinants. Preterm delivery, and the low birth weight associated with it, has also been linked to low cardiorespiratory fitness later in life. In this study, the researchers wanted to examine if low birth weights played a role for cardiorespiratory fitness in individuals born after pregnancy of 37-41 weeks.
They followed more than 280,000 males from birth to military conscription at age 17-24 using Swedish population-based registers. At conscription, the men underwent a physical examination that included an evaluation of their maximal aerobic performance on a bicycle ergometer. The researchers found that those born with higher birth weights performed significantly better on the cardiorespiratory fitness test. For every 450 grams of extra weight at birth, in a baby born at 40 weeks, the maximum work capacity on the bicycle increased by an average of 7.9 watts.
The association was stable across all categories of body mass index (BMI) in young adulthood and was largely similar in a subset analysis of more than 52,000 siblings, suggesting that BMI and shared genetic and environmental factors alone cannot explain the link between birth weight and cardiorespiratory fitness.
“The magnitude of the difference we observed is alarming,” says Daniel Berglind, researcher at the Department of Global Public Health at Karolinska Institutet and corresponding author. “The observed 7.9 watts increase for each 450 grams of extra weight at birth, in a baby born at 40 weeks, translates into approximately 1.34 increase in metabolic equivalent (MET) which has been associated with a 13 percent difference in the risk of premature death and a 15 percent difference in the risk of developing cardiovascular disease. Such differences in mortality are similar to the effect of a 7-centimeter reduction in waist circumference.”
The researchers believe the findings are of significance to public health, seeing as about 15 percent of babies born globally weigh less than 2.5 kilos at birth and as cardiorespiratory fitness have important implications for adult health.
“Providing adequate prenatal care may be an effective means of improving adult health not only through prevention of established harms associated with low birth weight but also via improved cardiorespiratory fitness,” says Viktor H. Ahlqvist, researcher at the Department of Global Public Health and another of the study’s authors.
Source: https://www.sciencedaily.com/releases/2020/01/200131074207.htm


Pets have been shown to ease stress, anxiety, and provide emotional support to their owners/families. Like many, as I have adjusted to the new normal of being at home 24/7. On days when the isolation of being separated from friends, mentors, colleagues, peers, and family has felt endless, our PTSD survivor cat Gannon has reminded me to be grateful for the little moments in time that bring joy into mundane daily tasks. While vaccination rollouts have ignited our hope for progressing towards increased in-person gathering, we still have a way to go. When working out seems like a drag I nab Gannon, put him in his big outdoor see-through tent, and enjoy his companionship and entertaining, hilarious behaviors. We are buddies. Following our recent move to Seattle, Gannon (a house cat) has managed to make countless neighborhood friends with other cats without leaving the home. Throughout the day and especially at night, he entertains and socializes with frequent “visitors” through our various small and large windows. He prefers we leave the living room and adjoining office area by 11:30 PM so he can enjoy his social time with his new friends who gather on the front porch. Observing him forming these mysterious connections fascinates me. As we progress towards increased in-person socialization Gannon continues to inspire me to be open to forming new and exciting friendships and reminds me that some barriers we anticipate are actually doors and windows we can open.
Adopting a pet may seem like a selfless act, but there are plenty of selfish reasons to embrace pet ownership. Research has shown that caring for a pet may provide numerous health benefits. An article by John Hopkins Medical Director Jeremy Barron, M.D reveals the positive effects a pet can have towards reducing stress, lowering blood pressure, increasing activity, and easing loneliness and depression.
Enjoy Dr. Barron’s pet suggestions

https://www.hopkinsmedicine.org/health/wellness-and-prevention/the-friend-who-keeps-you-young
Meet Ishita Malaviya, India’s first woman surfer | Her Game
Mar 25, 2021
When Ishita started surfing, there were no other known women surfers in India. Now, every boy and girl in her village has access to free surfing lessons. Watch her inspiring story.



