
Somaliland, officially the Republic of is an unrecognised sovereign state in the Horn of Africa, internationally considered to be part of Somalia. Somaliland lies in the Horn of Africa, on the southern coast of the Gulf of Aden. It is bordered by Djibouti to the northwest, Ethiopia to the south and west, and Somalia to the east. Its claimed territory has an area of 176,120 square kilometres (68,000 sq mi), with approximately 5.7 million residents as of 2021. The capital and largest city is Hargeisa. The government of Somaliland regards itself as the successor state to British Somaliland, which, as the briefly independent State of Somaliland, united in 1960 with the Trust Territory of Somaliland (the former Italian Somaliland) to form the Somali Republic.
Since 1991, the territory has been governed by democratically elected governments that seek international recognition as the government of the Republic of Somaliland. The central government maintains informal ties with some foreign governments, who have sent delegations to Hargeisa. Ethiopia also maintains a trade office in the region. However, Somaliland’s self-proclaimed independence has not been officially recognised by any country or international organisation. It is a member of the Unrepresented Nations and Peoples Organization, an advocacy group whose members consist of indigenous peoples, minorities and unrecognised or occupied territories.
Source:https://en.wikipedia.org/wiki/Somaliland
Healthcare in Somaliland, as with other Somalia ‘zones’, is largely in the private sector, regulated by the Ministry of Health of the Federal Government of Somalia. The system is largely staffed by undertrained, under-supervised and -paid staff, dependent upon donations from international agencies.
Source: https://bmchealthservres.biomedcentral.com/articles/10.1186/s12913-020-5049-2
PRETERM BIRTH RATES – Somaliland
The self-declared country of Somaliland remains largely unrecognized by the rest of the world. We were not able to gain preterm birth rates for Somaliland.
We “recognize” Somaliland as a respected member of our global Neonatal Womb Warrior/preterm birth community.
Rank: unknown –Rate: unknown Estimated # of preterm births per 100 live births
(USA – 12 %, Global Average: 11.1%)
COMMUNITY
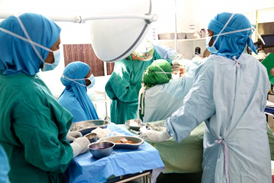
These Female Doctors Are Changing the Lives of Fistula Survivors In Somaliland
MEGAN IACOBINI DE FAZIO 3 May 2018

On one day in March dozens of people gathered in a hospital in Hargeisa, Somaliland. The bright room was decorated with flowers and banners in red, green and white, the colours of Somaliland’s flag. Doctors –foreign and Somali – ministers, medical students, former patients and journalists filed in, greeting each other, standing in little groups and talking animatedly. A man walked to the front, bowed his head, and intoned a prayer over the crackly microphone, and the murmur turned to silence as people took to their seats.
Minutes later, a woman dressed in an elegant blue gown took to the podium. Edna Adan, the face of Somaliland’s healthcare and founder of the hospital where this event took place, is in her 80s, but the passion in her voice and her strong demeanour make her seem decades younger.
We were all gathered to celebrate the 16th anniversary of the Edna Adan Hospital, which has been a shining example of healthcare and education since its inception.
“I always felt there was a need to provide Somalilanders with better healthcare,” says Edna, whose doctor father she credits with inspiring her to pursue medicine. “And that’s why, as a child, I decided I would build a hospital.”
Before she retired in 2002, Edna — who worked with the World Health Organization in the region after a working as a nurse — founded the hospital with the view of drastically reducing child and maternal mortality in the country.
“Women in Somaliland have the world’s highest mortality rates because there are no health facilities and few health professionals,” she says. “Seeing the magnitude of the problem and knowing the limited resources, I decided to put everything I could into reproductive health, and it’s the most rewarding thing that we’ve done.”
Since opening its doors, the hospital has delivered thousands of healthy babies, and its maternal mortality rate is a tiny fraction of the national average. The hospital has also become a centre for the treatment of obstetric fistula, one of the most devastating conditions faced by women in developing countries.
“Fistula can happen when women go through a long labour, and especially when they deliver at home, far from hospitals, in rural areas with no facilities or doctors,” explains 32-year-old Dr. Shukri Mohamed Dahir, Somaliland’s first female fistula surgeon.
“Pressure between the pelvic bone and fetal head kills the tissue of the bladder and rectum, and a small hole develops,” says Dr. Dahir. This hole – the fistula – can cause the woman to uncontrollably leak bodily waste, with shattering health and social consequences.
Shukri studied midwifery and nursing at Edna Adan Hospital, which later sponsored her through medical school. After she graduated in 2011, Dr. Dahir returned to Edna Adan’s hospital to learn about surgery.
“I always wanted to solve women’s problems myself, rather than hand them off to a male doctor to solve,” says Dr. Dahir. “And I also realized how important it was to have woman surgeons so women can feel free.”
Unfortunately, getting her degree wasn’t always enough to convince patients of her expertise: “People were not used to seeing women doctors, and wouldn’t trust us to do the operations. Once, during a consultation with a woman suffering with fistula, I had to pretend to be a student, while my male student posed as the surgeon. After the surgery, I told her I was the one who had cured her, so she let me take over.”
Because of the hospital’s great results, patients are now used to seeing female surgeons, and many of those suffering from obstetric fistula even request to be seen by other women. And, thanks to the Edna Adan University, which was formally established in 2009, it is not only women in the capital who are now receiving world-class healthcare. Graduate doctors from all Somaliland are coming here for training, and returning to their rural clinics with newfound life-saving skills.
“I am glad we are turning 16,” says Dr. Dahir of the hospital. “We have made a huge change in this country.”
Source:https://www.mhtf.org/geography/somaliland/

Learn how to boost your baby’s brain from a Harvard Professor
Feb 25, 2019 From an international health authority Learn how experts define health sources in a journal of the National Academy of Medicine

Dr. Jack Shonkoff, Professor of Child Health and Development at Harvard University, shares his important play tips to boost your child’s brain. In the first 1,000 days of life, a baby’s brain forms 1,000 new connections every second. Just 15 minutes of play can spark thousands of brain connections. Learn more: https://uni.cf/2Sk1yEn

Preterm births cost Australian Government $1.4 billion Annually

Monday, 19 July 2021
A new study has shown that the annual cost of preterm birth to the Australian Government is approximately $1.4 billion with one quarter of this arising from the need for educational assistance for those born too soon.
Conducted by the Women & Infants Research Foundation (WIRF) and the Australian Preterm Birth Prevention Alliance, the study was developed to estimate the costs of preterm birth in the first 18 years of life for a hypothetical cohort of 314,814 children – the number of live births in 2016.
Being born too early is the single greatest cause of death in young children in Australia and all similar societies. It is also one of the major causes of disability, both in childhood and adulthood. These disabilities include cerebral palsy, deafness, blindness and learning and behavioural problems.
Recently published in the Australian and New Zealand Journal of Obstetrics and Gynaecology (ANZJOG), the study revealed two thirds of the costs were borne by health care services with costs of preterm birth inversely related to gestational age at birth. Extremely preterm births were most expensive at $236,036 each, very preterm birth at $89,709, and late preterm birth at $25,417.
Chair of the Australian Preterm Birth Prevention Alliance and WIRF’s Chief Scientific Director, Professor John Newnham AM said assessments of economic costs were critical to inform evaluations of interventions aimed at the prevention or treatment of preterm birth.
“Discovering how to safely lower the rate of preterm birth and then evaluating the impact of that effectiveness needs to be one of our highest priorities in contemporary healthcare,” Professor Newnham said.
“The consequences of preterm birth for individuals, families and societies are considerable, both in terms of human suffering and economic consequences.”
Whilst previous international studies had quantified direct medical expenditure, this latest analysis also sought to measure the significant costs to educational services.
“The benefits of preterm birth prevention include fewer children with behavioural and learning problems, including the need for special education assistance,” Professor Newnham said.
“In our study, additional costs at school were calculated to contribute 25% of the cost of preterm birth. Promotion of programs to safely prevent preterm birth needs to include the educational advantages at school, as well as the profound benefits for families that arise from avoidance of behavioural problems.”
Professor Newnham, the 2020 Senior Australian of the Year, explained that it should no longer be assumed that the high costs of preterm birth are an inevitable consequence of our reproduction.
“The rate of preterm birth has been rising dramatically in Australia and elsewhere over the last two decades. There are many pathways to untimely early birth, each requiring a different clinical approach, and we have discovered some are now amenable to prevention.” Media Release
In 2014, WIRF launched the WA Preterm Birth Prevention Initiative was launched – the world’s first whole-of-state and whole-of-population program to prevent preterm birth.
Results from the first year of this program revealed a reduction in the rate of preterm birth across WA by 8% and by 20 per cent at the major tertiary level centre – King Edward Memorial Hospital.
The success of the WA program, which has also extended to the ACT as part of their reported 10% reduction of preterm birth rates in 2020, have been underpinned by the development of key interventions to safely lower the rate of early birth.
“When we apply these interventions as part of a multifaceted program across an entire population the rate of preterm birth can be reduced, at least by about 8%. Further advances in potential interventions can be expected to make prevention even more effective,” Professor Newnham said.
“Investing in the prevention of preterm birth is a social and economic investment in our community’s future.”
As accurate data is only available to estimate the costs to 18 years of age, it is reasonable to conclude that the costs to government estimated in the current study represent only a fraction of the eventual overall burden to individuals, families and the nation.
In May 2021, the Australian Government announced $13.7 million in federal funding to bolster the Alliance’s ongoing efforts to lower the rate of preterm birth across Australia.
The funding will support the expansion of a national education and outreach program to safely lower rates of preterm birth in each Australian state and territory.
The study, ‘The health and educational costs of preterm birth to 18 years of age in Australia’, has been published online in the Australian and New Zealand Journal of Obstetrics and Gynaecology.
Authors for the original ANZJOG article are: John Newnham, Chris Schilling, Stavros Petrou, Jonathan Morris, Euan Wallace, Kiarna Brown, Lindsay Edwards, Monika Skubisz, Scott White, Brendan Rynne, Catherine Arrese, and Dorota

Joyful voices to savor from our Somaliland family

Xidigana Geeska Wadani Dhaba Maaha Hargeeisa Book Fair Music Video 2021Jul 29, 2021
Xidigaha Geeska,Najax Nalka,Mubarak October,Suldaan Seeraar, Xariir Axmed, Mursal Muuse, Hodan Abdirahman, Kiin Jamac, Waqal Studio

Breastfeeding status and duration significantly impact postpartum depression risk
Study first to explore current breastfeeding status in association with postpartum depression risk in large national dataset
Date: September 30, 2021 Source: Florida Atlantic University

According to the United States Centers for Disease Control and Prevention, between 11 and 20 percent of women who give birth each year in the U.S. have postpartum depression symptoms, which is the greatest risk factor for maternal suicide and infanticide. Given that there are 4 million births annually, this equates to almost 800,000 women with postpartum depression each year.
Current biological and psychosocial models of breastfeeding suggest that breastfeeding could possibly reduce a woman’s risk for postpartum depression. However, prior studies only have looked at the initiation of breastfeeding and breastfeeding length. In addition, small and often homogenous samples have yielded ungeneralizable results lacking in statistical power with biased results due to higher levels of education, income, and proportions of white participants compared to the general population of the sampled country.
Researchers from Florida Atlantic University’s Christine E. Lynn College of Nursing and collaborators are the first to examine current breastfeeding status in association with postpartum depression risk using a large, national population-based dataset of 29,685 women living in 26 states
Results of the study, published in the journal Public Health Nursing, demonstrate that postpartum depression is a significant health issue among American women with nearly 13 percent of the sample being at risk. Findings showed that women who were currently breastfeeding at the time of data collection had statistically significant lower risk of postpartum depression than women who were not breastfeeding. In addition, there is a statistically significant inverse relationship between breastfeeding length and risk of postpartum depression. As the number of weeks that women breastfed increased, their postpartum depression decreased. An unexpected finding was that there was no significant difference in postpartum depression risk among women with varying breastfeeding intent (yes, no, unsure).
“Women suffering from postpartum depression, which occurs within four weeks and up to 12 months after childbirth, endure feelings of sadness, anxiety and extreme fatigue that makes it difficult for them to function,” said Christine Toledo, Ph.D., senior author and an assistant professor in FAU’s Christine E. Lynn College of Nursing. “Women with postpartum depression who are not treated also may have negative outcomes, including difficulty bonding with and caring for their children, thoughts of harming themselves or their infant, and also are at an increased risk of substance misuse.”
Woman who have experienced postpartum depression have a 50 percent increased risk of suffering further episodes of postpartum depression in subsequent deliveries. In addition, they have a 25 percent increased risk of suffering further depressive disorders unrelated to childbirth up to 11 years later. Postpartum depression increases maternal morbidity and is associated with increased risks for cardiovascular disease, stroke and type-2 diabetes.
For the study, Toledo and collaborators from the University of Miami School of Nursing and Health Studies, University of North Carolina School of Nursing, Chapel Hill, Seattle University of Nursing, and The University of British Columbia School of Nursing, analyzed dataset from the 2016 Pregnancy Risk Assessment Monitoring System (PRAMS) questionnaire to investigate the association of breastfeeding practices taking into consideration significant covariates such as age, race, marital status, education, abuse before and during pregnancy, cigarette smoking, among others.
“Findings from this important study suggest that breastfeeding is a cost efficient and healthy behavior that can decrease a woman’s risk for postpartum depression,” said Safiya George, Ph.D., dean, FAU Christine E. Lynn College of Nursing. “Nurses in particular play an important role in educating and promoting both the maternal health benefits of breastfeeding and infant benefits such as providing necessary nutrients and protecting them against allergies, diseases and infections.”
Florida Atlantic University. “Breastfeeding status and duration significantly impact postpartum depression risk: Study first to explore current breastfeeding status in association with postpartum depression risk in large national dataset.” ScienceDaily. ScienceDaily, 30 September 2021.
Source:https://www.sciencedaily.com/releases/2021/09/210930101408.htm

Dr. Gabor Mate, philosopher, doctor and powerful resource, is accessible to those who seek to explore our inner selves, identify avenues to healing, and gain a broader perspective of emotional support and healing pathways. Not always an easy “listen” and therefore a thought provoking experience, Gabor, as he also travels through his life, shares his insights and perspectives. Dr. Mate invites contemplation as he suggests that a key component of understanding the effects of trauma is not how it affects what we do so much as how it impacts what we do not do. Definitely food for thought…..

Dr Gabor Maté’s Life Advice Will Change Your Future (MUST WATCH)
Jul 12, 2021 #GaborMaté #MotivationThrive
Dr Gabor Maté’s Life Advice Will Change Your Future (MUST WATCH). Who is Gabor Maté? A renowned speaker, and bestselling author, Dr. Gabor Maté is highly sought after for his expertise on a range of topics including addiction, stress and childhood development.

PREEMIE FAMILY PARTNERS

Videos | LIVE series | Preemie Chats
CPBF – Canadian Premature Babies Foundation
Below you can find our virtual educational sessions tailored to NICU parents and healthcare professionals. The sessions are interactive; you can join LIVE every Friday at 1pm EST either on our Facebook or YouTube pages. This is a great opportunity to chat with experts, researchers, and parents from all over the world. There is an abundant collection of interesting videos, and here are a few examples:
–Prematurity and Autism Spectrum Disorder -Vision Development from Infancy to Childhood -LGBTQ+ in the NICU -Preterm Birth and Adult Health
Source:https://www.cpbf-fbpc.org/videos
Below is a great example of a virtual session CPBF provides weekly to educate Preemie Parents and Healthcare Professionals.
An Adult Preemie Tells Her Story

February 2021
Pediatric and Fetal Surgeon, Dr. Timothy Crombleholme Explains Open Fetal Surgery
Jun 25, 2018Fetal Care Center Dallas
Dr. Timothy M. Crombleholme is a pediatric and fetal surgeon recognized worldwide for his experience in fetoscopic surgery, open fetal surgery, image-guided fetal intervention and EXIT procedures. Dr. Crombleholme emphasizes educating his families about what to expect for the surgical procedure and throughout the pregnancy. “Our families are some of the most relaxed families in the newborn nursery because they have processed everything and have been prepared for the delivery and the challenges the baby faces, and nothing is intimidating to them.”

Fortifying Family Foundations
Assistant Professor Ashley Weber’s intervention empowers parents to care for their premature infants
By Evelyn Fleider – July 20, 2021

Imagine you are a new mom or dad whose baby was recently born at fewer than 32 weeks old. Your infant needs weeks-long, round-the-clock support in the hospital, but you do not have the job flexibility that allows you to spend time there, a trusted sitter to care for your other child/children or reliable transportation to get you there. You are overwhelmed, emotional and missing out on critical moments at the hospital, when you could get to know your baby and learn to manage their complex care and needs.
Each year, about 100,000 U.S. women give birth to babies considered very or extremely premature who require long-term stays in a neonatal intensive care unit (NICU) and who are at a high risk of developing chronic conditions. But not all parents get the formal training they need to keep their child healthy, which can cause mental health issues for parents. To address the critical need for an effective, streamlined model of parent-driven care, Ashley Weber, PhD, RN, a practicing NICU nurse and assistant professor at the College, is piloting PREEMIE PROGRESS, a video-based intervention that helps parents understand, monitor and manage their infant’s care while in the NICU.
With the financial backing of a National Institutes of Health (NIH) grant, Weber and the College’s Center for Academic Technologies and Educational Resources (CATER) team designed and built the intervention to deliver education to overwhelmed, high-risk parents with low literacy and education through accessible, platformagnostic videos and optional worksheets. Parents can learn by watching the videos or completing worksheets
while doing laundry or caring for other family members at home. Specifically, PREEMIE PROGRESS provides family management skills including negotiated collaboration, care systems navigation, emotion control, outcome expectancy and more.
“Our mortality rates have significantly gone down over the decades, but long-term complications from prematurity have not changed,” Weber says. “We need to decrease the stress and sensory stimulation that babies experience throughout their NICU stay. Also, research shows that babies do best when they’re with their parents.”
Although parent education interventions exist, socioeconomic barriers, such as the lack of mandated paid family leave in the U.S., often prevent parents from participating in these opportunities and learning about their baby’s complex care during their NICU stay. The need to return to work shortly after birth or lack of transportation to the NICU are some of the various obstacles that prevent parents from being able to focus on their baby’s health and deliver the majority of care in the NICU.
“If you can spend large amounts of time in the NICU, you get to learn; nurses educate you on the plan of care and you participate in rounds, getting to know your baby,” Weber says.
“I wanted to build an intervention that could help disadvantaged families learn outside of the NICU, so that when they are able to be in the NICU, they maximize that time and spend it caring for their baby as opposed to playing catch-up.”
Currently, Weber and her team are refining PREEMIE PROGRESS through iterative usability and acceptability testing. In October, they will start testing feasibility and acceptability of the refined intervention and study procedures in a pilot randomized controlled trial with 60 families over the course of two years. They anticipate the intervention will decrease parent depression and anxiety, increase infant weight gain and receipt of mother’s milk and reduce neonatal health care utilization. Weber then plans to submit a competitive R01 for additional funding to conduct an even larger trial.
PREEEMIE PROGRESS has been years in the making for Weber, who in 2018 worked with the College of Nursing’s instructional designers, technology specialists, videographers and graphic designers to create the first prototype. She hopes the project will eventually evolve into a collaborative partnership among NICUs in Cincinnati, Columbus and Cleveland to conduct research trials centered on improving family care.
Weber’s long-term goal is to become a leader in designing, disseminating and implementing sustainable family management programs to improve health outcomes in the NICU. Regardless of her success, she recognizes that the best thing she can do for her patients is to advocate for universal paid family leave, better childcare and transportation infrastructures.
“We can come up with all sorts of interventions for reducing parent and infant stress and changing the way providers deliver care in the NICU, but if a mom doesn’t have the money to pay for a babysitter so she can get to the NICU or doesn’t have paid leave and has to go back to work a week or two after birth, the chances of parent engagement in care are extremely low,” Weber says. “I hope that PREEMIE PROGRESS empowers families who are at a disadvantage through no fault of their own. We want to give NICU families skills they can use for a lifetime, but these broader public health policies to support the social determinants of family success are really needed in order to move family research forward in the NICU.”
Source:https://www.uc.edu/news/articles/2021/07/fortifying-family-foundations.html

A Day in the Life of the NICU

Apr 25, 2017 Medtronic Minimally Invasive Therapies Group
Watch how staff at Rush University Medical Center combats neonatal stress. (14-RE-0016)

HEALTHCARE PARTNERS

Gaps in Palliative Care Education among Neonatology Fellowship Trainees
Catherine Lydia Wraight Jens C. Eickhoff Ryan M. McAdams
Published Online:27 Jul 2021https://doi.org/10.1089/pmr.2021.0011

Abstract
Background: To provide proper care for infants at risk for death, neonatologists need expertise in many areas of palliative care. Although neonatology training programs have implemented a wide variety of palliative care educational programs, the impact of these programs on trainees’ skills and effective communication regarding end-of-life issues remains unclear.
Objective: To determine whether neonatology fellowship programs are providing formal palliative care education and assess whether this education is effective at increasing fellows’ self-reported comfort with these important skills.
Methods: An anonymous survey was sent to program directors (PDs) and fellows of ACGME accredited neonatology fellowship programs in the United States. Using a 5-point Likert scale, participants were asked about the palliative care education they received, and their comfort level with several key aspects of palliative care.
Results: Twenty-four (26%) PDs and 66 (33%) fellows completed the survey. Fourteen PDs (58%) reported including palliative care education in their formal fellowship curriculum, whereas only 20 (30%) responding fellows reported receiving palliative care education. Of the responding fellows, most (80%) reported being uncomfortable or only somewhat comfortable with all assessed areas of palliative care. Fellows who received formal education were more comfortable than those without it in leading goals of care conversations (p = 0.001), breaking bad news (p = 0.048), discussing change in code status (p = 0.029), and grief and bereavement (p = 0.031).
Conclusions: Most fellows report being uncomfortable or only somewhat comfortable with essential areas of palliative care. Formal palliative care education improves fellows’ self-reported comfort with important aspects of end-of-life care. To promote a well-rounded neonatology fellowship curriculum, inclusion of formal palliative care education is recommended.

Source:https://www.liebertpub.com/doi/10.1089/pmr.2021.0011

STRESS IN THE NICU

Stressful events – a byproduct of life for babies in the NICU – may increase their heart rate and blood pressure, while decreasing their oxygen levels. Even sensory and environmental stimuli we take for granted, such as a simple touch and noise and bright lights, can affect physiologic responses such as heart rate, respiration, and oxygen saturation.
The additive impact of multiple stressors over time may have profound long-term consequences on the lives of NICU babies. In the rapidly developing perinatal brain, repeated neonatal stress may have long-term effects on the central nervous system, including effects on neural structure, function, and development.

Doctor and Two Nurses Drive 2 Miles In Texas Snowstorm To Deliver Premature Baby
Mar 4, 2021 Uplifting Stories in a Minute
Despite being only 24 weeks pregnant, Kimberley Arias went into labor in the middle of the Texas snowstorm. Thanks to the help of Dr. John Loyd and nurses Kelly Clause and Nicole Padden who traveled 2 hours in the blizzard, her baby was delivered safely.

The New Graduate Neonatal Nurse Practitioner’s Transition from Bedside to Head-of-the-Bed
By Chandler Williams, DNP NNP-BC

The Neonatal Nurse Practitioner (NNP) role in the neonatal intensive care unit (NICU) is about to mark its 50th birthday.
According to the Accreditation Council for Graduate Medical Education, there has been an estimated 33% reduction in resident physician NICU rotations (Jnah & Robinson, 2015). This will only increase the need for NNPs in NICUs across the country. A 2020 survey reported that the average NNP is 51 years old, and there are 40 accredited NNP programs in the US with new NNPs entering the workforce every year (Snapp et al., 2021). One thing all these NNPs have in common is the journey of navigating the transition that is from the bedside RN role to the head-of-the-bed NNP role. New graduate NNPs have feelings of anxiety, insecurity, exhaustion, and lack of confidence in decision making.
The transition period can be looked at in terms of the first year of starting as a new graduate NNP; that’s because most NNPs report feelings of competence and viewing themselves as a member of the NICU team at the end of year 1 (Cusson & Strange, 2008). To ease this transition, novice NNPs should seek out mentors, be aware of areas of weakness or fears, seek out strategies to ease the transition, and consider the familiarity of the unit. NNPs are an important part of a neonate’s care team, and easing this transition is important for the future of NNPs’ careers.
There are many strengths and weaknesses of being a new graduate NNP, and it is important to be aware of these strengths to gain confidence through the transition process, as well as the weaknesses to know there is room for growth and to feel not alone. These strengths include strong assessment skills, hard-working, professionalism, previous neonatal nursing experience, compassion, calculations, and internal motivation to learn and excel. Perceived weaknesses include procedural experience, pharmacologic knowledge, limited experience, nervousness about role transition, doubting oneself, and emotional attachments to patients and families (Jnah & Robinson, 2015).
One way that novice NNPs can ease the transition to the workforce is through mentorship. There is an ease in the transition from RN to NNP in those who seek out mentors. A study on mentoring and self-efficacy in the NNP workforce revealed that mentorship facilitates positive self-efficacy for the novice NNP (Jnah & Robinson, 2015). Novice NNPs enter this new world with a passion for neonatal care and a desire to make a difference in the lives of neonates and their families; however, the fear of the unknown can be daunting. Mentorship is a collaborative relationship that is beneficial to both the mentor and the mentee by encouraging the development of long-term relationships between novice NNPs and experienced NNPs. During the orientation period, the novice NNP is generally placed under the guidance of a preceptor assigned to provide direct supervision and teach the novice NNP in their new clinical setting (Jnah & Robinson, 2015). A preceptor differs from a mentor in that a preceptor is time-limited; mentorship has no time limitations. Less experienced NNPs report longing for mentorship and support from other NNPs after their orientation is complete (Beal et al., 1997). Mentorship has reported increased job satisfaction, productivity, and quality of care (Jnah & Robinson, 2015). New graduate NNPs who seek out mentors and invest in these relationships can anticipate an ease in the role transition process.
There are a lot of opinions on whether it is a more difficult transition for a new graduate NNP in the facility or unit where they were an RN versus a new unit. An experienced NNP recruiter once described this phenomenon via a metaphor between ketchup and mustard bottles; stating that a novice NNP on the unit where that person was an RN is like a ketchup bottle that has been emptied and filled with mustard. Even though this person is now filled with different substance (NNP knowledge), others will continue to look at them as ketchup (or their previous role).
However, there is evidence to suggest that RNs returning to their previous unit as an NNP has an easier transition and were benefited by their previous knowledge of the unit. It is also reported that those who accept jobs on units where they completed clinical practicum had a less difficult transition. These NNPs report a sense of familiarity with the hospital, unit, and staff. Challenges in these instances include initially being less accepted by nurses on the unit and, often, being questioned by staff nurses who expect them to prove themselves in their new role. There is evidence to suggest that NNPs who transition to their new role in a completely different unit from training or previous employment are more readily accepted by the staff but face a learning curve with regard to organizational culture and practice styles and routines (Cusson & Strange, 2008).
Strategies to enhance the role transition include developing good relationships with all staff, finding a mentor, becoming an active member of a professional nursing organization, sharing needs and accepting guidance, developing strategies to decrease stress, staying up-to-date in current evidence, and realizing that feelings of inadequacy are normal and will dissipate throughout the transition. Although each person develops in their identity of their new role, overall being open to support and guidance and being an active part of your new role as an NNP can increase confidence in the development of a role identity. A strong nursing identity is vital because it is associated with a successful NNP practice (Cusson & Viggiano, 2002).
The NNP is an important part of the neonatal care team. The average age of an NNP is decreasing as the NNP workload in the NICU is increasing across the country. New graduate NNPs will continue to transition in the role from bedside to head-of-the-bed, and can find support in this transition through mentors, self-evaluation, and careful examination of areas of strength and weakness. This transition period is just that, a transition, and there are ups and downs throughout this process. It is important to recognize that the progression of graduating from school, seeking employment, studying and obtaining licensure, and credentialling does not happen overnight. There are a lot of feelings of anxiety and worry, because it seems as if we have little control over the timeframe or outcome.
As the NNP progresses through orientation, and even in the first months of being “on their own,” they may feel anxious and inadequate and experience self-doubt, manifested primarily through questioning their knowledge and skills, wondering if they can handle a crisis or worse, and fearing making a fatal mistake or missing an important diagnoses (Cusson & Strange, 2008). As new graduate NNPs enter the workforce, it is important to provide support them throughout this process.
Source:http://nann.org/publications/e-news/september2021/special-interest-section

INNOVATIONS

Developing eHealth in neonatal care to enhance parents’ self-management
Annica Sjöström Strand1, Björn Johnsson2, Momota Hena1, Boris Magnusson2, Inger Kristensson Hallström1
Abstract
Background: Discharge from a neonatal care unit is often experienced as a vulnerable time for parents. By communicating through digital technology, it may be possible to improve the support for parents and thereby make the transition from hospital to home less stressful.
Aim: To develop an eHealth device supporting the transition from hospital to home for parents with a preterm-born child in Sweden using participatory design.
Method: Employing a framework of complex interventions in health care using participatory design. Parents of preterm-born infants and professionals at a neonatal department identified specific technical requirements for an eHealth device to be developed in the context of neonatal care and neonatal home care. The prospective end-users – parents and professionals – were continuously involved in the process of designing solution prototypes through meetings, verbal and written feedback, and interviews. The interviews were analysed using thematic analysis.
Results: Technical development was carried out with the perspectives of professionals and parents in mind, resulting in an eHealth application for computer tablets. The findings from the interviews with the parents and professionals revealed three categories: The tablets felt secure, easy to use and sometimes replaced visits to hospital and at home.
Conclusion: The use of participatory design to develop an eHealth device to support a safe transition from hospital to home can benefit parents, the child, the family, and professionals in neonatal care.
Source:https://pubmed.ncbi.nlm.nih.gov/33950534/
“In a Way We Took the Hospital Home”-A Descriptive Mixed-Methods Study of Parents’ Usage and Experiences of eHealth for Self-Management after Hospital Discharge Due to Pediatric Surgery or Preterm Birth
Rose-Marie Lindkvist1, Annica Sjöström-Strand1, Kajsa Landgren1, Björn A Johnsson2, Pernilla Stenström34, Inger Kristensson Hallström1
Abstract
The costly and complex needs for children with long-term illness are challenging. Safe eHealth communication is warranted to facilitate health improvement and care services. This mixed-methods study aimed to describe parents’ usage and experiences of communicating with professionals during hospital-to-home-transition after their child’s preterm birth or surgery for colorectal malformations, using an eHealth device, specifically designed for communication and support via nurses at the hospital. The eHealth devices included the possibility for daily reports, video calls, text messaging, and sending images. Interviews with 25 parents were analyzed with qualitative content analysis. Usage data from eHealth devices were compiled from database entries and analyzed statistically. Parents using the eHealth device expressed reduced worry and stress during the initial period at home through effective and safe communication. Benefits described included keeping track of their child’s progress and having easy access to support whenever needed. This was corroborated by usage data indicating that contact was made throughout the day, and more among families living far away from hospital. The eHealth device potentially replaced phone calls and prevented unnecessary visits. The eHealth technique can aid safe self-treatment within child- and family-centered care in neonatal and pediatric surgery treatment. Future research may consider organization perspectives and health economics.
Source:https://pubmed.ncbi.nlm.nih.gov/34203985/

Engaging Frontline Providers Prevents Hypothermia and Improves Communication in the Postoperative Neonate
Guidash, Judith C. BSN, RN, CPHQ; Berman, Loren MD, MHS; Panagos, Patoula G. MD; Sullivan, Kevin M. MD, MBA, FAAP
Advances in Neonatal Care: October 2021 – Volume 21 – Issue 5 – p 379-386 doi: 10.1097/ANC.0000000000000839
Abstract
Background:
Neonates undergoing surgery are at high risk for perioperative hypothermia. Hypothermia has been associated with increased adverse events. Transfer of care from the operating room (OR) to the neonatal intensive care unit (NICU) adds another layer of risk for this population introducing the potential for miscommunication leading to preventable adverse events.
Purpose:
The aim of this quality improvement initiative is to decrease mean postoperative hypothermia rate and achieve compliance with use of a standardized postoperative hand-off in neonates transferred to the NICU from the OR.
Methods:
An interdisciplinary team identified opportunities for heat loss during the perioperative period. The lack of standardized perioperative communication between the NICU and the OR and postoperative communication between neonatology, anesthesiology, surgery, and nursing were noted. Guidelines for maintaining euthermia in the perioperative period and a standardized interdisciplinary postoperative hand-off communication tool were created.
Findings/Results:
Mean rate for participation in the hand-off process increased from 78.8% to 98.4% during the study period. The mean hypothermia rate improved from 28.6% to 6.3% (P < .0001) and was sustained.
Implications for Practice:
Creating a hypothermia guideline and standardizing temperature monitoring can significantly decrease the rate of postoperative hypothermia in neonates. Standardization of transfer of care from OR to NICU increases consistent communication between the services.
Implications for Research:
Future research and improvement efforts are needed to optimize the management of surgical neonates through their transfers of care.

Nursing Students Create Wearable Night Light
Feb 11, 2021 CBS Pittsburgh
The founders of Lumify Care, Anthony Scarpone-Lambert and Jennifferre Mancillas, have more on the new tool for nurses.

Family-centered music therapy—Empowering premature infants and their primary caregivers through music: Results of a pilot study

Barbara M. Menke, Joachim Hass, Carsten Diener, Johannes Pöschl
Published: May 14, 2021 https://doi.org/10.1371/journal.pone.0250071
Abstract
In Neonatal Intensive Care Units (NICUs) premature infants are exposed to various acoustic, environmental and emotional stressors which have a negative impact on their development and the mental health of their parents. Family-centred music therapy bears the potential to positively influence these stressors. The few existing studies indicate that interactive live-improvised music therapy interventions both reduce parental stress factors and support preterm infants’ development.
The present randomized controlled longitudinal study (RCT) with very low and extremely low birth weight infants (born <30+0 weeks of gestation) and their parents analyzed the influence of music therapy on both the physiological development of premature infants and parental stress factors. In addition, possible interrelations between infant development and parental stress were explored. 65 parent-infant-pairs were enrolled in the study. The treatment group received music therapy twice a week from the 21st day of life till discharge from hospital. The control group received treatment as usual.
Compared to the control group, infants in the treatment group showed a 11.1 days shortening of caffeine therapy, 12.1 days shortening of nasogastric/ orogastric tube feed and 15.5 days shortening of hospitalization, on average. While these differences were not statistically significant, a factor-analytical compound measure of all three therapy durations was. From pre-to-post-intervention, parents showed a significant reduction in stress factors. However, there were no differences between control and treatment group. A regression analysis showed links between parental stress factors and physiological development of the infants.
This pilot study suggests that a live-improvised interactive music therapy intervention for extremely and very preterm infants and their parents may have a beneficial effect on the therapy duration needed for premature infants before discharge from hospital is possible. The study identified components of the original physiological variables of the infants as appropriate endpoints and suggested a slight change in study design to capture possible effects of music therapy on infants’ development as well. Further studies should assess both short-term and long-term effects on premature infants as well as on maternal and paternal health outcomes, to determine whether a family-centered music therapy, actually experienced as an added value to developmental care, should be part of routine care at the NICU.
Source:https://journals.plos.org/plosone/article/comments?id=10.1371/journal.pone.0250071



Keep Your Brain Young with Music

If you want to firm up your body, head to the gym. If you want to exercise your brain, listen to music.
“There are few things that stimulate the brain the way music does,” says one Johns Hopkins otolaryngologist. “If you want to keep your brain engaged throughout the aging process, listening to or playing music is a great tool. It provides a total brain workout.”
Research has shown that listening to music can reduce anxiety, blood pressure, and pain as well as improve sleep quality, mood, mental alertness, and memory.
The Brain-Music Connection
Experts are trying to understand how our brains can hear and play music. A stereo system puts out vibrations that travel through the air and somehow get inside the ear canal. These vibrations tickle the eardrum and are transmitted into an electrical signal that travels through the auditory nerve to the brain stem, where it is reassembled into something we perceive as music.
Johns Hopkins researchers have had dozens of jazz performers and rappers improvise music while lying down inside an fMRI (functional magnetic resonance imaging) machine to watch and see which areas of their brains light up.
“Music is structural, mathematical and architectural. It’s based on relationships between one note and the next. You may not be aware of it, but your brain has to do a lot of computing to make sense of it,” notes one otolaryngologist.
Everyday Brain Boosts from Music
The power of music isn’t limited to interesting research. Try these methods of bringing more music—and brain benefits—into your life.
Jump-start your creativity
Listen to what your kids or grandkids listen to, experts suggest. Often we continue to listen to the same songs and genre of music that we did during our teens and 20s, and we generally avoid hearing anything that’s not from that era.
New music challenges the brain in a way that old music doesn’t. It might not feel pleasurable at first, but that unfamiliarity forces the brain to struggle to understand the new sound.
Recall a memory from long ago
Reach for familiar music, especially if it stems from the same time period that you are trying to recall. Listening to the Beatles might bring you back to the first moment you laid eyes on your spouse, for instance.
Listen to your body
Pay attention to how you react to different forms of music and pick the kind that works for you. What helps one person concentrate might be distracting to someone else, and what helps one person unwind might make another person jumpy.

Wherever the Art of Medicine is Loved there is also Love of Humanity-Hippocrates

Reflecting on the impact of music therapy on preemie infant survivors and parents highlighted above brings me great joy both as a fellow survivor and a Zumba Instructor. For me music has been a vessel where I am able to tune into feeling emotions internally without the need to express them outwardly or verbally. Learning about the ways in which music therapy may influence the reduction of stressor and physiological development of the parents and preemies is an exciting development.
The benefits of having therapies like music therapies that allow both the preemies and parents to engage in activities together is empowering. In the many years working as a Zumba fitness instructor, I have witnessed the impact music can have on others. I know for myself it has greatly contributed to my own development as a young child learning to play guitar, and as a teen and adult participating in and teaching Zumba where a variety of international beats is discovered in each class. Likewise, when I have felt uneasy in times of stress and anxiety music has helped me recenter and ground myself in my body. I am thrilled to learn researchers may now have the ability overtime to scientifically measure its tangible impact on the tiny members and parents in our community today.
My go to music when I am working out and studying is EDM, and for emotional release I may listen to Latin vibes or Alternative pop. What type of music has helped you navigate the waves of your life? Are there songs that aided you along your neonatal community journey? If you are a preemie survivor, I encourage you to consider talking about music with your caregivers/parents. Some interesting stories may be yet to be discovered.
No surfing in Somaliland but definitely the WAVES to do so.

SWIMMING WITH FISHES
11/3/2020 by RiyoTv
Hargeisa to berbera somaliland 2020!! beach vlog. 4k drone and GoPro



