NIGERIA
PRETERM BIRTH RATES – Nigeria
Rank: 50 –Rate: 12.2 Estimated # of preterm births per 100 live births
(USA – 12 %, Global Average: 11.1%)

Nigeria, officially the Federal Republic of Nigeria, is a country in West Africa. It is the most populous country in Africa; geographically situated between the Sahel to the north, and the Gulf of Guinea to the south in the Atlantic Ocean; covering an area of 923,769 square kilometres (356,669 sq mi), with a population of over 211 million. Nigeria is a federal republic comprising 36 states and the Federal Capital Territory, where the capital, Abuja, is located. The largest city in Nigeria is Lagos, one of the largest metropolitan areas in the world and the second-largest in Africa.
Nigeria is a multinational state inhabited by more than 250 ethnic groups speaking 500 distinct languages, all identifying with a wide variety of cultures. The three largest ethnic groups are the Hausa–Fulani in the north, Yoruba in the west, and Igbo in the east, together comprising over 60% of the total population. The official language is English, chosen to facilitate linguistic unity at the national level. Nigeria’s constitution ensures freedom of religion and it is home to some of the world’s largest Muslim and Christian populations, simultaneously. Nigeria is divided roughly in half between Muslims, who live mostly in the north, and Christians, who live mostly in the south; indigenous religions, such as those native to the Igbo and Yoruba ethnicities, are in the minority.
Health care delivery in Nigeria is a concurrent responsibility of the three tiers of government in the country, and the private sector. Nigeria has been reorganising its health system since the Bamako Initiative of 1987, which formally promoted community-based methods of increasing accessibility of drugs and health care services to the population, in part by implementing user fees. The new strategy dramatically increased accessibility through community-based health care reform, resulting in more efficient and equitable provision of services. A comprehensive approach strategy was extended to all areas of health care, with subsequent improvement in the health care indicators and improvement in health care efficiency and cost. The Nigerian health care system is continuously faced with a shortage of doctors known as ‘brain drain‘, because of emigration by skilled Nigerian doctors to North America and Europe. In 1995, an estimated 21,000 Nigerian doctors were practising in the United States alone, which is about the same as the number of doctors working in the Nigerian public service. Retaining these expensively trained professionals has been identified as one of the goals of the government.
https://en.wikipedia.org/wiki/Nigeria
The countries with the greatest numbers of preterm births are India – 3,519,100; China – 1,172,300; Nigeria – 773,600; Pakistan – 748,100; Indonesia – 675,700; United States – 517,400; Bangladesh – 424,100; Philippines – 348,900; Democratic Republic of the Congo – 341,400; and Brazil – 279,300.
Source:https://www.who.int/pmnch/knowledge/publications/preterm_birth_report/en/index3.html
COMMUNITY
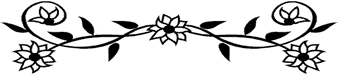
We were very excited to discover the article below to share in our blog and with our Community to reference. It is heart-breaking to consider the pain a preterm birth baby may experience and worse yet, incomprehensible that we have denied our children recognition as deserving care towards healing their wounds related to their preterm birth experience. We have made gains towards reducing noise and light and interference/overstimulation in the NICU, we have made some progress in lessening preemie pain; pain that may be unavoidable if their lives are to be saved. We have figured out that separation of preemie babies from the parents/caregivers may not only create long term psychological damage to the preemie infants but may also reduce the growth and development opportunities that loving touch provides.
Kat was born at 24 weeks gestation and at 3 ½ weeks old, weighing 1 lb. 3 ounces, she underwent open heart surgery without anesthesia under the care of a brilliant, brave, strong and guided surgeon. We are so blessed to have had this heroic female surgeon in our lives. Our Preterm Birth healthcare partner community is rich with skilled, heroic, gifted providers who also need our support.
Our Preterm Birth/Neonatal Womb Community must develop targeted treatment for preterm birth survivors to specifically address and treat preverbal trauma so that our children have access to therapy and therapists who are available and able to provide curative nonpharmaceutical treatments to support the healing, growth, and quality of life for our preemie population at large. This will be difficult to accomplish, and we must not borrow a convenient but ineffective treatment designed to treat other conditions that did not generate in the way anxiety, depression, non-attachment, etc. develops in much of the preemie population. The time to move forward in creating curative treatment to address preverbal stress for our Preterm Birth Survivors/Neonatal Womb Warriors is now. With 11 to 12 % of our global population born preterm the need is imminent, the availability to research the associated conditions and solutions is vast, and the potential to create therapies to address preverbal trauma is viable and necessary.



Why it’s so hard to treat pain in infants
For decades physicians believed that premature babies didn’t experience pain. Here’s what doctors know now – and the innovative solutions being embraced by today’s caregivers.
By Sharon Guyup Published November 11, 2021
Doctors once believed that infants—especially premature babies—did not feel pain, and if they did, they would not remember it.
This might sound like Medieval medicine. But as recently as the 1980s, babies undergoing surgery were given a muscle relaxant to paralyze them while in the operating room but were not given any pain medication, says Fiona Moultrie, a pediatrician and researcher at the University of Oxford who focuses on neonatal pain. “At the time, it was assumed that most of the behaviors that infants were exhibiting were just reflexes.”
Over the next decades, studies documented changes in infant behavior, stress hormones, and brain activity, proving that even the tiniest babies did indeed suffer pain. Research also revealed that continued pain could derail a child’s short- and long-term neurological, social, and motor development, especially in fragile, preterm babies born earlier than 37 weeks, says Björn Westrup, a neonatologist and researcher at the Karolinska Institute near Stockholm, Sweden.
Rapid advances in medicine now allow very fragile, tiny, preterm babies to survive. But preemies may spend weeks or months in the hospital undergoing the constant, often painful procedures needed to save their lives. Strategies to make such procedures less traumatic are vital, as premature births are rising globally. In the United States alone, about 380,000 babies are born prematurely each year, or about one in 10 births. Worldwide, it’s about 15 million.
The medical profession tries to manage or prevent infant suffering with drugs such as ibuprofen (for mild to moderate pain) and fentanyl (used to alleviate extreme pain). For most analgesic drugs, though, the proper dosage, effectiveness, or effects on the brain remain unknown, so increasingly, hospitals are incorporating non-pharmaceutical interventions that center on techniques known as developmental care, which keep babies and their families together rather than isolating infants in incubators.
That’s critical, says Manuela Filippa, a researcher at the University of Geneva who studies prematurity because separating sick babies from their parents compounds pain with toxic stress that creates serious developmental problems. Inside a neonatal intensive care unit, or NICU, lights are bright and monitors blink. It’s loud, with machines beeping, alarms going off, people talking, and ventilators thumping and hissing.
“Brain maturation is based on sensory experience,” Filippa explains, “and the [traditional] neonatal intensive care unit is very stressful.”
How do babies express pain?
Babies born extremely early are whisked from the delivery room to the NICU. The youngest, those under 36 weeks, have underdeveloped lungs and may be intubated and hooked up to a ventilator. They are too weak to suckle and must be fed through tubes in the nose or mouth. Nurses need to lance their tiny heels for blood tests up to 10 times a day, and they are engulfed in IV lines, tubes, and wires.
In the early 1980s, Canadian newborn medicine researcher Celeste Johnston, an emeritus professor at McGill University in Montreal, was approached by nurses working in the NICU who wanted a way to measure pain in infants. In 1986, she was among the first to publish evidence that infants’ heart rates and oxygen levels changed when they were subjected to painful procedures. Their cries and facial expressions revealed what she calls “honest signaling,” behaviors that babies are born with that communicate distress.
“There is a particular grimace that was described by Darwin in the 1800s that is recognized universally as pain,” she says. That’s ironic, Moultrie notes, “as Darwin’s celebrated work on evolutionary theory and the expression of emotions in man promoted the concept of infants as primitive beings with under-developed senses and merely reflexive behaviors.”
Johnston was later horrified to learn that in intensive care, babies averaged about 14 painful procedures each day.
But understanding how these small, nonverbal beings experience pain is extremely difficult. “One of the biggest challenges in caring for preterm and sick infants is that they can’t tell us,” says Erin Keels, a nurse practitioner and director of advanced neonatal providers at Nationwide Children’s Hospital in Columbus, Ohio. “We can only infer by their behaviors and their vital signs.”
Forty different pain scores have been compiled over the last three decades, which can be used to evaluate pain levels. They each include various combinations of heart rate, oxygen saturation, facial expressions, or body movements. But since physiology can change for many reasons, and a baby may be too sick or too medicated to grimace, these are not always objective markers. There is an ongoing quest to better understand how infants perceive and experience painful stimuli.
“Although there has been great progress, we still don’t fully understand pain in neonates,” says the University of Oxford’s Moultrie. She and others have been trying to measure pain by observing bursts of electrical activity in the brain using electroencephalogram (EEG) testing. They identified a pain-related pattern of brain activity in infants, which is now being used in clinical trials to test the efficacy of medications. It could revolutionize pain treatment.
In a later studies, researchers at the University of Oxford used MRI scans to pinpoint brain activity. They found that 20 out of 22 brain regions activated in an adult’s brain in response to pain are also activated in a newborn baby’s brain. One area that did not register was the amygdala, which is associated with fear and anxiety, likely because days-old babies may not yet make these associations, Moultrie says.
But there’s still a lot researchers still don’t know about exactly what’s going on in the infant brain. “When you’re tiny and underdeveloped, differentiation between pain and stress is not clear,” says Johnston.
At the same time, researchers are uncovering the potential long-lasting physiological consequences of preemie pain, Filippa notes. The amount of pain-related stress predicts the thickness of the brain’s cortex, for instance. One study found that at school age, children who were born very preterm—at 24 to 32 weeks gestational age—had a thinner cortex in 21 of 66 cerebral regions, predominately in the frontal and parietal lobes. This has been linked to motor and cognitive impairments.
Preterm babies also face significant risk for lowered IQ, attention deficit disorder, memory issues, and difficulty with social interactions and emotional control. Heidelise Als, a pioneer in understanding physical and behavioral risks for both preterm and sick infants, attributes this at least partly to the vastly altered sensory experiences that can influence preterm babies’ immature nervous systems.
Alternatives to alleviate pain
Without an accurate way to measure pain, though, it’s tough to test how effective any given drug is. By the 1990s, doctors understood that using anesthesia during major surgeries improved outcomes. Babies that were intubated and on ventilators were—and still are—given morphine, though there’s ongoing controversy over whether it reduces their pain, says Moultrie. Meanwhile, the risks of pharmacological interventions include opioid addiction, withdrawal, difficulty breathing, and possible impacts on neurodevelopment.
The downside of painkillers has spurred the search for alternate treatments. One method gives babies sucrose before procedures because it can release endorphins and potentially ease pain. While it seems to soothe them and lower physical response to painful stimuli, the baby’s stress hormones and reactive brain signals remain high, says Nils Bergman, a researcher and pediatric specialist also at Karolinska Institute. Other work has found that breastfeeding during needle-related procedures provides more pain relief than interventions such as swaddling, being held, topical anesthetics, music therapy, or a pacifier.
The physical environment also matters in reducing a baby’s stress during painful procedures. In 2000, a trial in Sweden compared the progress of babies cared for in a traditional intensive care ward versus a darkened, quiet, more womb-like room with parents present. The latter group was discharged quicker and had grown slightly more by the end of their stay.
Today, many neonatal experts think this kind of family-centered care is the wave of the future. One of the most effective methods is Kangaroo Mother Care, which involves wrapping an infant skin-to-skin on its mother’s or father’s chest.
The method was developed in Colombia by pediatrician Edgar Rey, who began using it at Bogotá’s Maternal and Child Institute in 1978. At the time, some 70 percent of preemies died in their overcrowded neonatal ward. Rey had stumbled upon a report describing how a kangaroo raised its peanut-size underdeveloped joey to about a quarter of her own weight, raising it inside her pouch and keeping it warm through skin-to-skin contact.
Rey discovered that human babies also thrived in this way, and after implementing the technique, preemie death rates plummeted. The World Health Organization recently estimated that annually, kangaroo care could save 450,000 lives.
Years later in Canada, Johnston found that skin-to-skin contact provided a calming situation for conducting routine procedures in the NICU and babies both showed a milder pain response and recovered more quickly .
Filippa has studied the effects of other family-based interventions, including how the sound of a mother’s voice might mitigate her child’s pain. Her team monitored 20 premature babies at the Parini Hospital in Italy during their daily heel-prick blood tests, with mothers talking to them or singing to them. Hearing their mother’s voice during a medical procedure significantly improved the infant’s pain score. Singing also helped, but less so.
When the team examined hormonal changes triggered when a baby hears its mother speaking to them, they found that oxytocin levels rose substantially. Oxytocin, sometimes called the attachment hormone, is produced in the hippocampus and plays a crucial role in modulating pain, stress, and social behaviors. It also protects against inflammation in a preterm infant’s brain, Filippa explains.
With lower oxytocin levels, the emotional brain – the hypothalamus – is less developed. The result is that “you’re less able to face stressful events and have higher reactions to pain,” says Filippa. “Oxytocin is strong neuroprotection against the short- and long-term effects of pain.”
Toward zero separation
In 2010 Westrup revealed that even the smallest, sickest babies benefitted from having parents with them 24/7. Notably, there were fewer lung issues and much shorter hospital stays. Sweden has since incorporated this knowledge by redesigning many NICUs so parents can live with their baby, even in high intensive care situations. Pre-COVID-19, siblings could also visit.
This type of “zero separation” approach requires a holistic mindset that also cares for mothers: At least 50 percent of those who birth early have other health conditions and need obstetric care. In a number of countries, new NICUs are being built with individual rooms to house families. But government support is needed for most people to devote months to caring for their sick child.
In Sweden, nationalized medicine covers costs, and the government pays parental benefits up to 35 weeks; extended benefits can stretch to 61 weeks. In Canada, which also provides medical coverage, both mother and father are entitled to 240 days of paid leave.
The situation is far different in the U.S., where mothers are entitled to 12 weeks of unpaid leave if they work for a company with 50 or more employees. The U.S. is one of just six countries that has no national paid leave. Currently, Congress is considering four weeks of paid family leave as part of a $1.85 trillion domestic policy bill, which faces opposition. The U.S. also lacks nationalized health coverage – and has the world’s most expensive health care system.
Westrup and Bergman emphasize that we should not just wait until neonatal units are rebuilt or all the economic conditions are in place to act. Ultimately, there is substantial evidence that we need to change the system to embrace zero separation, they say. Teaching nurses and doctors how to provide this kind of developmental care will give children a healthier future.
Keels of Nationwide Children’s Hospital is optimistic about the evolution in preemie care and the research that will continue to inform best practices. “I’m hopeful that in the near future, we’ll have greater knowledge and better ways of evaluating pain so we can do really individualized medicine right at the bedside.”
Source:

Rural Midwives Fill Gap as Hospitals Cut Childbirth Services
Stateline Article -December 8, 2021 By: Aallyah Wright

Editor’s Note: The story has been updated to clarify that Sharon Hospital will shut down its labor and delivery unit over the next year
For the past year or so, Toni Hill, a midwife in the lowlands of northern Mississippi, has received an influx of calls from women across the state who live in areas with no hospitals and only a smattering of health care providers.
As COVID-19 rates increased, some pregnant women did not feel safe receiving care in a hospital or were unable to contact their providers. Others, who lived in the Mississippi Delta, did not have transportation for the three-plus hour trip to Jackson, the state capital. Hill quickly found herself very overwhelmed, she said.
On most days, Hill is stretched thin: conducting home and clinic visits, which can be up to three hours away, while being a mother and running a nonprofit. Hill is one of at least 30 certified midwives and nurse midwives in Mississippi, a state where 84% of the areas with shortages of primary care health professionals are in rural counties, according to a health department report published this year.
Many rural hospitals across the country are struggling to stay afloat amid the coronavirus pandemic. Facing workforce shortages, financial challenges and more patients than beds, some have had to cut or suspend obstetric services.
Midwives, trained professionals who specialize in maternity care, are picking up the slack. In interviews with Stateline, midwives from rural areas say they’re overwhelmed and facing burnout because of an uptick in patients—even as they’re eager to help. Doulas, who assist parents during childbirth but don’t provide medical care, also are seeing an increase in demand.
Some states, recognizing a dire need for midwifery and doula support services, have passed laws to expand care, while members of Congress are considering federal investment. Rural health experts and leaders stress that policies should focus on the challenges of affordability, insurance coverage and lack of providers in rural areas.
This year, at least eight states—Arizona, Arkansas, California, Colorado, Connecticut, Louisiana, Nevada and Rhode Island—have passed laws that aim to improve birthing outcomes. Many of the laws have expanded Medicaid and other health insurance coverage for midwifery and doula services, required health facilities to allow doulas to attend births or increased pathways for students to become licensed midwives.
The Biden administration’s proposed Build Back Better Act would provide additional funding for postpartum Medicaid coverage as well as financial and programmatic support for doulas and nursing students.
The pandemic has revealed longstanding issues of “innate systemic racial basis” within health systems that have contributed to the maternal health crisis in the United States, said Louisiana state Rep. Matthew Willard, a Democrat. Willard sponsored a bill, signed into law by Democratic Gov. John Bel Edwards this summer, that created a state doula registry committee and required that all health insurance plans with maternity benefits cover midwifery services.
Nationwide, midwives attend less than 10% of hospital births, but in rural hospitals the figure is 30%, according to a 2019 brief by the federal Centers for Medicare and Medicaid Services.
In Nevada, legislators expanded Medicaid coverage for doula services along with pandemic-related health care bills. And in Arkansas, lawmakers passed legislation granting certified nurse midwives full practice authority without an agreement with a consulting physician.
The legislation can help, but it’s going to take more rural-centric, comprehensive policies to fix health infrastructure needs in rural America that have been exacerbated by the pandemic, said Katy Kozhimannil, health researcher and director of the Rural Health Research Center at the University of Minnesota.
Those needs include recruiting and retaining a skilled workforce and finding ways to keep labor and delivery units open despite relatively few births. Many rural hospitals have taken a financial hit, Kozhimannil said, and the pandemic has caused them to reduce services.
“In some cases, the hospital obstetric unit can’t remain open or won’t because not all communities can have a hospital that provides birth services,” she said. “And in those places, it’s very important not to turn a blind eye to the consequences that we know, [such as] more pre-term babies.”
Even before the pandemic, rural areas lacked maternal health services. In 2014, after a decade of steady decline, nearly 54% of rural U.S. counties had no hospital-based obstetric services, according to a 2020 study published in the Journal of the American Medical Association. Between 2014 and 2018, researchers found, the number of rural hospitals with obstetric services declined by another 3%.
The rural counties that were more likely to lose their hospital-based obstetric care services were less populated, more remote, had fewer doctors, had “less generous” Medicaid programs and had higher proportions of Black residents compared with White residents, said Kozhimannil, who co-authored the study.
Since January 2020, at least 21 hospitals in rural areas have closed, according to data from the Cecil G. Sheps Center for Health Services Research at the University of North Carolina at Chapel Hill.
When hospitals close or shut down their obstetric services, the loss can lead women to deliver on their own or in ambulances on the way to a hospital, said Jennifer Cameron, a certified nurse midwife in rural Michigan.
“They go into labor. They call 911, and they get transported to the closest facility with a labor and delivery unit. For some people it may be 45 minutes away,” Cameron said. “If someone is having a heart attack, there’s no ambulance to take them.”
After the local hospital in Manistee, Michigan, where Cameron practices, stopped offering obstetric services, she conducted more out-of-hospital births at her freestanding birth center. She is usually on call every hour of the day because she has just one part-time office assistant. Prenatal visits, labor and delivery and up to six weeks of postpartum care can cost more than $4,000. Many of her patients don’t have insurance and can’t afford to pay out of pocket.
“It isn’t sustainable. Midwives burn out. There are a lot of midwives that only take cash-pay clients and if they can’t afford to pay, then they can’t get their care,” Cameron said. “I do take someone that can’t pay me a certain percentage. I do allow a couple births per month that I know I’m not going to get paid for, because it’s the right thing to do.”
Medicaid paid for a larger share of births in rural than urban areas and for people of color than White people in 2018. The program helps to alleviate rising mortality and morbidity rates and racial disparities in maternal health outcomes, according to a 2020 fact sheet by the Medicaid and CHIP Payment and Access Commission, a nonpartisan legislative agency that provides policy and data analysis to federal and state governments about Medicaid and the Children’s Health Insurance Program.
But the reimbursement Cameron gets from Medicaid isn’t enough to cover the cost of her services, she said.
Hill, the midwife in Mississippi, said even if she did receive Medicaid payments, she still wouldn’t be able to accept more patients with her small staff.
“They’d be covering maybe $1,300 for a birth. That’s less than half of what I get paid,” Hill said.
Hill said states and policymakers will need to take more action to address the economy and well-being of rural communities overall.
“We want people to come into care healthier. I’ve talked to pregnant women who don’t even have primary care physicians,” she said. “We need more midwives [in the hospitals and birth centers] in theory, but we have to look at the community health piece, too.”
Smaller hospitals have cited decreased births, financial woes and staffing issues as primary reasons for cutting back on services in the past year. Sharon Hospital in rural Connecticut is among those that this year made plans to halt labor and delivery services. Hospital officials plan to phase out the services over the next eight to 12 months pending regulatory approval.
Over the past few years, the hospital has seen an average of about 200 deliveries per year, said Dr. Mark Hirko, president of Sharon Hospital. He had hoped to see an influx of childbirths, but with an aging population, the “numbers remain essentially flat,” he said.
Instead of keeping the labor unit, the hospital will expand on other primary care services.
“Everything pointed us in the direction that we needed to refocus and redirect our efforts towards where the population is taking us,” Hirko told Stateline. Parents-to-be now will have to travel to other birthing centers and hospitals to receive care.
Other rural health systems that cut services have lost employees as a result of the federal COVID-19 vaccine mandate for health care workers, which has been temporarily blocked by federal judges in Missouri and Louisiana.
Lewis County General Hospital in Lowville, New York, stopped delivering babies after losing at least six employees over the mandate. A similar instance occurred in rural Lamar, Colorado, which forced the Prowers Medical Center to suspend services at its maternity ward.
The staffing shortage in hospitals is placing an added burden on midwives. There were more than 12,000 certified nurse midwives and about 100 certified midwives in 2019, according to the American College of Nurse-Midwives.
The demand for midwives and other maternal care providers is higher than the supply, said Erin Ryan, a certified professional midwife and secretary for the National Association of Certified Professional Midwives. The need has increased with obstetric unit closures, she added.
According to the federal Centers for Medicare and Medicaid Services, the United States is expected to have a shortage of 22,000 obstetricians and gynecologists by 2050.
The worst shortages, the agency noted, are expected in rural areas.

2Baba Ft. Syemca – Target You
1,391,852 views Premiered Nov 5, 2020
Target You is an instant fan favourite from the Warriors album released in March 2020.
Indoor Air Pollution Is a Major Culprit in Preterm Births
Tara Haelle – October 26, 2021
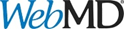
Scientists have long known that exposure to air pollution during pregnancy increases risks for preterm birth or low birth weight. New findings suggest that pollution exposures are higher in low- and middle-income countries and especially from indoor sources.
In 2019, for example, about half the world’s population breathed household air pollution from cooking fires. In addition, 92% of the global population lived in areas in which the air quality did not meet World Health Organization recommendations.
For this latest report, published in PLOS Medicine, researchers analyzed data from 124 studies on air pollution, birth weight, and preterm birth. They wanted to be sure distinguish exposures to indoor air pollution, which often is overlooked. (A preterm birth is defined as before 37 weeks of pregnancy; low birth weight is about 5.5 pounds, or less than 2,500 grams).
Most of the studies they assessed came from the United States, Europe, and Australia, with a scattering of findings from India, China, South America, and sub-Saharan Africa. The researchers specifically included reports from Africa and Asia because indoor fire cooking is more common in these regions.
About a third of the air pollution causing preterm birth came from the outside air, so that most of it was from indoor air pollution, largely in low-income countries.
The results showed that air pollution accounted for 16% of all babies born with a low birth weight and 36% of preterm births. The findings imply that one out of every three preterm births could be prevented if air pollution exposure during pregnancy could be eliminated. The study authors estimate that about 5.9 million preterm births worldwide in 2019 could instead have been delivered at term if air pollution were kept to levels associated with minimum risk.
In sub-Saharan African countries, for example, more than half of all preterm births (52.5%) were attributable to air pollution exposure. Keeping air pollution at the minimum risk level could reduce both preterm births and incidence of low birth weight by 78% in this region, the study authors estimate.
Low birth weight and preterm birth increase the risk of death before age 1 and can have additional lifelong consequences. These infants have a greater likelihood of intellectual and developmental disabilities and of other disabilities, such as vision, lung, or hearing problems. Asthma, digestion difficulties, and infections are also more common in those born preterm.
Source PLOS Medicine: “Ambient and household PM2.5 pollution and adverse perinatal outcomes: A meta-regression and analysis of attributable global burden for 204 countries and territories.” https://www.medscape.com/viewarticle/961571

PREEMIE FAMILY PARTNERS
Day in the life of a DOCTOR: Shadowing NICU NURSE PRACTITIONER (ft. premature babies)
Violin MD Nov 27, 2021
Babies born at 22 weeks (5.5 months) can survive!! Join me in the largest NICU in Canada and learn about the lifesaving treatments for premature babies! I’ll be shadowing Nikki, a nurse practitioner who works in the neonatal ICU. Plus you’ll meet baby Kalani who was born at 23 weeks and her mother, Paola. **note: at the time this video was filmed, Nikki was a nurse practitioner candidate. She will be fully licensed after passing her final exam. For simplicity, I have referred to her as a nurse practitioner.
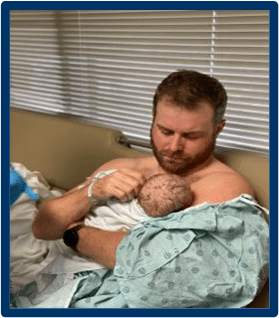
Increasing Early Skin-to-Skin in Extremely Low Birthweight Infants
POSTED ON 09 NOVEMBER 2021
Although the benefits of skin-to-skin care (SSC) for preterm and low birthweight infants are known to the neonatal community, some health centres still struggle with implementation. To increase SSC within the first 72 hours of life among extremely low birthweight (ELBW) infants, a multidimensional approach was chosen at a Level IV university-based regional intensive care nursery (ICN).
SSC has many benefits for mothers and infants, especially those born preterm. Previous studies showed that in extremely low birthweight (ELBW) babies, early and frequent infant-parent SSC increases life expectancy and improves short- and long-term health outcomes. Unfortunately, many health centers still do not regularly implement this practice as early or as frequently as evidence supports.
As an example, in a 58-bed, Level IV ICN at a children’s teaching hospital, the implementation of SSC during the first 72 hours of ELBW infants’ lives has only been achieved 7% of the time. Motivated to increase this rate to 80% within one year, a multidisciplinary team of neonatal providers conducted an intervention to encourage SSC from July 2018 to December 2019, using the Institute of Healthcare Improvement quality improvement methodology.
Following this approach, unit policies and guidelines were updated to facilitate early skin-to-skin. A readiness checklist was developed, and the education of parents, staff and providers on SSC was prioritised. The balancing measure was the rate of severe intraventricular haemorrhage (IVH), a risk commonly associated with SSC. Data collected from monthly chart reviews were used to analyse the changes in SSC rate during the intervention.
Ultimately, 52 infants born under 28 weeks’ gestation or weighing less than 1,000g were included in the project. After the intervention, there was a significant improvement in the rate of early SSC from 7% to 84%. Furthermore, the analysis showed no difference in the balancing measure of severe IVH, encouraging the practice of early SSC among the staff.
The initiative was successful, and the team calls for future efforts to measure long-term health and neurodevelopmental outcomes from the practice of early SSC on extremely low birth weight babies.

This Dad Spends Every Christmas With Babies In The NICU | Dads Got This! | TODAY Original
Dec 18, 2019 TODAY
On this episode of “Dads Got This!” TODAY’s Craig Melvin spotlights a dad who dresses up as Santa Claus to give back to the same NICU where his son was a patient.

BRAIN BLEEDS IN PREMATURE BABIES
March of Dimes – November 9, 2021

Preterm birth can lead to many different health complications. Brain bleed, also called an intraventricular hemorrhage (IVH), is one type of serious problem that can happen in babies who are born too early, smaller and sicker. If you or someone you know has a baby with a brain bleed, it can be a very scary and upsetting experience.
Bleeding in the brain is most common in preterm babies who weigh less than 3 pounds, 5 ounces). A baby born before 32 weeks of pregnancy is at the highest risk of developing a brain bleed. This is because the tiny blood vessels in a baby’s brain are very fragile and can be injured easily. The bleeds usually happen in the first few days of life.
How are brain bleeds diagnosed?
In IVH, bleeding occurs near the fluid-filled spaces (ventricles) in the center of the brain. An ultrasound test can show if a baby has a brain bleed and how severe it is. All babies born before 30 weeks should have an ultrasound of the head to screen for IVH, according to MedlinePlus.gov. The test is typically done between 7 and 14 days of age. Babies born between 30 weeks and 34 weeks also may be screened if they have symptoms of IVH.
Are all brain bleeds the same?
Brain bleeds usually are given a number grade (1 to 4) based on where in the brain it’s happening in and how big the brain bleed is. The right and left sides of the brain are graded separately. Most brain bleeds are mild (grades 1 and 2) and resolve themselves with few lasting problems. More severe bleeds (grades 3 and 4) can cause difficulties for your baby during hospitalization as well as possible problems in the future.
What happens after your baby leaves the hospital?
Every child is unique. How well your baby will do depends on several factors. Many babies with IVH will need to be seen by a pediatric neurologist or another specialist (such as a developmental-behavioral pediatrician) during infancy and early childhood. Some children may have seizures or problems with speech, movement or learning.
If your baby is delayed in meeting their developmental milestones, they may benefit from early intervention services. Early intervention services such as speech, occupational and physical therapy may help your child catch up.
Where can parents find support?
Having a baby with a brain bleed can be overwhelming. The March of Dimes online community, Share Your Story, is where parents can find comfort and support from other parents who have (or had) a baby in the NICU with a brain bleed. Just log on and post a comment, and you will be welcomed.
Source: https://newsmomsneed.marchofdimes.org/baby/brain-bleeds-in-babies/

Tour the NICU at Sharp Mary Birch with Dr. Anup Katheria
Dec 4, 2019 Sharp HealthCare
Join Dr. Anup Katheria, Director of the Neonatal Research Institute at Sharp Mary Birch Hospital for Women & Newborns, on a tour of the hospital’s 84-bed NICU and see a few of the many technologies and therapies used to help give preterm infants the best start in life.
HEALTH CARE PARTNERS

Global Health Education and Best Practices for Neonatal-Perinatal Medicine Trainees
PERSPECTIVE| DECEMBER 01 2021
Sharla Rent, MD; Krysten North, MD; Ellen Diego, MD; Carl Bose, MD
Neoreviews (2021) 22 (12): e795–e804.https://doi.org/10.1542/neo.22-12-e795

Neonatal-perinatal medicine (NPM) trainees are expressing an increased interest in global health. NPM fellowship programs are tasked with ensuring that interested fellows receive appropriate training and mentorship to participate in the global health arena. Global health engagement during fellowship varies based on a trainee’s experience level, career goals, and academic interests. Some trainees may seek active learning opportunities through clinical rotations abroad whereas others may desire engagement through research or quality improvement partnerships. To accommodate these varying interests, NPM fellows and training programs may choose to explore institutional partnerships, opportunities through national organizations with global collaborators, or domestic opportunities with high-risk populations. During any global health project, the NPM trainee needs robust mentorship from professionals at both their home institution and their partner international site. Trainees intending to use their global health project to fulfill the American Board of Pediatrics (ABP) scholarly activity requirement must also pay particular attention to selecting a project that is feasible during fellowship and also meets ABP criteria for board eligibility. Above all, NPM fellows and training programs should strive to ensure equitable, sustainable, and mutually beneficial collaborations.
Study Finds Healthcare Lacks Female Leadership, Opportunities
Aine Cryts November 29, 2021

A new study on diversity, equity, and inclusion in the healthcare leadership structure of organizations in the United States has found that women are underrepresented, despite making up a majority of the overall healthcare workforce. Fifteen percent of health system and health insurer CEOs are women, according to the study, which was published online today in JAMA Network Open. Representation by women as chairpersons of the board of directors at health systems and health insurers was just slightly better: 17.5% of chairpersons at health systems are women, and 21.3% of boards of directors have chairpersons who are women.
The study also found that having a woman as a health system CEO was associated with a higher proportion of women on the board of directors or in roles as senior executives. Having more women in senior leadership roles at health insurance companies was also associated with increased representation of women as CEOs, per the study.
Researchers also learned that more than half (58.1%) of the leadership positions in the US Department of Health and Human Services (HHS) are held by women.
Bismarck Odei, MD, lead author of the study, told Medscape Medical News that he was most surprised that “the healthcare system in one of the largest populated countries in the world, where women form a slight majority, has so few women leaders influencing the day-to-day healthcare realities of women.”
Still, he points to the gender diversity of healthcare organizations’ boards of directors as “not a trivial statistic.”
“It may be one of the more important parameters that can increase the representation of women in the CEO position across healthcare organizations,” said Odei, a radiation oncology resident at the Ohio State University Comprehensive Cancer Center.
Healthcare Organizations Are More Diverse Than Fortune 500
As a benchmark, women are more likely to serve as CEO at healthcare organizations than at Fortune 500 companies. Fortune reported in June that only 8.1% of these companies are led by women CEOs. Barron’s reported in July that 29% of US board directors were women in 2020, which is up from 19% in 2014.
In addition, a 2019 analysis by consulting firm McKinsey revealed that organizations in the top quartile in terms of gender diversity on executive teams were 25% more likely to deliver above-average profitability than companies in the fourth quartile.
The JAMA study authors wrote that the underrepresentation of women on leadership teams, especially since women make up slightly more than half (50.8%) of the US population, “likely diminishes their role in policy decisions that affect population and women’s health.”
Putting the study in the larger context of research in this area, Odei observes that increased diversity improves organizational performance. “The US healthcare system has been valiantly trying to reach its full potential for some time now, and strengthening its leadership ranks with diverse and innovative voices will be key to achieving its goals.”
Source:https://www.medscape.com/viewarticle/963741
Please enter full article below to access excellent resource information to reference regarding pregnancy loss and ED staff empowerment.
Interdisciplinary Guidelines for Care of Women Presenting to the Emergency Department with Pregnancy Loss

Abstract: Members of the National Perinatal Association and other organizations have collaborated to identify principles to guide the care of women, their families, and the staff, in the event of the loss of a pregnancy at any gestational age in the Emergency Department (ED). Recommendations for ED health care providers are included. Administrative support for policies in the ED is essential to ensure the delivery of family-centered, culturally sensitive practices when a pregnancy ends.
Full Resource access

Sleep-Disordered Breathing In High-Risk Pregnancies Is Associated With Elevated Arterial Stiffness And Increased Risk For Preemcampsia

Published:December 01, 2021 DOI:https://doi.org/10.1016/j.ajog.2021.11.1366
ABSTRACT
Background
Impaired vascular function is a central feature of pathologic processes preceding the onset of preeclampsia. To this end, arterial stiffness, a composite indicator of vascular health and an important vascular biomarker, has been found to be increased throughout pregnancy in those destined to develop preeclampsia and at the time of preeclampsia diagnosis. While sleep-disordered breathing in pregnancy has been associated with increased risk for preeclampsia, it is unknown if sleep-disordered breathing is associated with elevated arterial stiffness in pregnancy.
Objectives
This prospective observational cohort study aimed to evaluate arterial stiffness in pregnant women with and without sleep-disordered breathing and assess the interaction between arterial stiffness, sleep-disordered breathing, and preeclampsia risk.
Study Design
Women with high-risk singleton pregnancies were enrolled at 10-13 weeks’ gestation and completed the Epworth Sleepiness Score, Pittsburgh Sleep Quality Index, and Restless Legs Syndrome questionnaires each trimester. Sleep-disordered breathing was defined as loud snoring or witnessed apneas (≥3 times/week). Central arterial stiffness (carotid-femoral pulse wave velocity, the gold standard measure of arterial stiffness), peripheral arterial stiffness (carotid-radial pulse wave velocity), wave reflection (augmentation index, time to wave reflection), and hemodynamics (central blood pressures, pulse pressure amplification) were assessed non-invasively using applanation tonometry at recruitment and every four weeks from recruitment until delivery.
Results
High-risk pregnant women (n=181) were included in the study. Women with sleep-disordered breathing (n=41; 23%) had increased carotid-femoral pulse wave velocity across gestation independent of blood pressure, and body mass index (p=0.042). Differences observed in other vascular measures were not maintained after adjustment for confounders. Excessive daytime sleepiness, defined by Epworth Sleepiness Score >10, was associated with increased carotid-femoral pulse wave velocity only in women with sleep-disordered breathing (pinteraction=0.001). Mid-gestation (first or second trimester) sleep-disordered breathing was associated with a 3.4 odds ratio (0.9-12.9) for preeclampsia, which increased to 5.7 (1.1-26.0) in women with sleep-disordered breathing and hypersomnolence, while late (third trimester) sleep-disordered breathing was associated with a 8.2 odds ratio (1.5-39.5) for preeclampsia.
Conclusions
High-risk pregnant women with mid-gestational sleep-disordered breathing had greater arterial stiffness throughout gestation compared with those without. Sleep-disordered breathing at any time during pregnancy was also associated with increased preeclampsia risk, and this effect was amplified by hypersomnolence.
Source:https://www.ajog.org/article/S0002-9378(21)02626-0/fulltext

INNOVATIONS
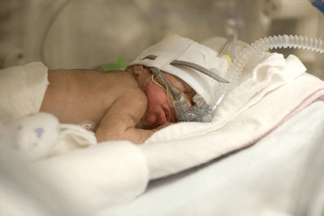
Study Links Air Pollution to Nearly 6 Million Preterm Births Around the World
Data on Indoor and Outdoor Pollution Comes from All Inhabited Continents

September 28, 2021
Air pollution likely contributed to almost 6 million premature births and almost 3 million underweight babies in 2019, according to a UC San Francisco and University of Washington global burden of disease study and meta-analysis that quantifies the effects of indoor and outdoor pollution around the world.
The analysis, published Sept. 28, 2021, in PLOS Medicine, is the most in-depth look yet at how air pollution affects several key indicators of pregnancy, including gestational age at birth, reduction in birth weight, low birth weight, and preterm birth. And it is the first global burden of disease study of these indicators to include the effects of indoor air pollution, mostly from cook stoves, which accounted for two-thirds of the measured effects.
A growing body of evidence points to air pollution as a major cause of preterm birth and low birthweight. Preterm birth is the leading cause of neonatal mortality worldwide, affecting more than 15 million infants every year. Children with low birthweight or who are born premature have higher rates of major illness throughout their lives.
The World Health Organization estimates that more than 90 percent of the world’s population lives with polluted outdoor air, and half the global population is also exposed to indoor air pollution from burning coal, dung and wood inside the home.
“The air pollution-attributable burden is enormous, yet with sufficient effort, it could be largely mitigated,” said lead author Rakesh Ghosh, PhD, a prevention and public health specialist at the Institute for Global Health Sciences at UCSF.
The analysis, which was conducted with researchers at the Institute for Health Metrics and Evaluation (IHME) at the University of Washington, quantified preterm birth and low birthweight risks based on total indoor and outdoor pollution exposure, while also accounting for the likelihood that the negative effects taper off at higher levels.
The study concluded that the global incidence of preterm birth and low birthweight could be reduced by almost 78 percent if air pollution were minimized in Southeast Asia and sub-Saharan Africa, where indoor pollution is common and preterm birth rates are the highest in the world.
But it also found significant risks from ambient air pollution in more developed parts of the world. In the United States, for example, outdoor air pollution is estimated to have contributed to almost 12,000 preterm births in 2019.
Previously, the same research team quantified the effects of air pollution on early life mortality, concluding that it contributed to the deaths of 500,000 newborns in 2019.
“With this new, global and more rigorously generated evidence, air pollution should now be considered a major driver of infant morbidity and mortality, not just of chronic adult diseases,” Ghosh said. “Our study suggests that taking measures to mitigate climate change and reduce air pollution levels will have significant health co-benefit for newborns.”
Authors of the study include Kate Causey, Katrin Burkart, Sara Wozniak, Aaron Cohen and Michael Brauer, of the Institute for Health Metrics and Evaluation, University of Washington, Seattle.

Studio 24 launches Purple Baby Project to reduce spate of premature mortality
Health By Chukwuma Muanya 25 November 2021

STUDIO 24, a digital photography company, has launched Purple Baby Project in a bid to reduce premature births and the rising mortality of preterm babies in Nigeria.
The project was launched at the Lagos University Teaching Hospital (LUTH) to commemorate this year’s World Prematurity Day, with the theme: “Zero Separation, Act now! Keep parents and babies born too soon together.”
Speaking on the project, the Chief Executive Officer of Studio 24, Christopher Ifeanyi Oputa, said the company is embarking on a journey to save lives and raise awareness for a cause it strongly believes is grossly neglected in Nigeria.
He said over the years, Nigeria has witnessed the dire rise of mortality in babies caused by lack of awareness, insufficient equipment, lack of maintenance programme for equipment in use, and knowledge on how to handle premature babies before transferring them to the hospital.
He said despite inventions and adoption of new technologies by countries across the world to reduce the mortality rates globally, Nigeria is still lagging behind, with statistics placing the country as the second highest in premature deaths.
Oputa also pointed at the lack of knowledge on the part of healthcare givers in knowing the right care to give to premature babies at the point of birth, adding that Studio 24 will equip the health providers in rural areas with new technologies and new safe practices of managing premature babies.
The Studio 24 boss explained that the focal points of the project include, to convert educational materials into a step-by-step audio and visual training resource for health professionals in caring/teaching expectant and newborn mothers, adding that this is also in line with the vision of training neonatal nurses.
Others are to facilitate the Purple Baby Equipment Maintenance Program in the Neonatal Intensive Care Units (NICU) across selected hospitals, starting with Lagos State, and spanning across Nigeria, as well as arresting public attention by promoting content that inspires public awareness, engagement and goodwill for the Preterm New-Born and Vulnerable Baby Care in hospitals.
The Head, Neonatal Unit, Lagos University Teaching Hospital, Prof Chinyere Ezeaka, lamented that Nigeria carries a disproportionate burden, as it records the highest numbers of newborn deaths in Africa and the second highest in the world.
She said while prematurity is the leading cause of deaths in all children less than five years old, three-quarters of these deaths could be prevented with current, cost-effective interventions.
Ezeaka said with early and good antenatal care, some of these conditions could be identified and managed appropriately to prevent preterm delivery.
She stressed that while the economic burden and the physical demand on the parents are often unquantifiable, the healthcare system is often overburdened, as their care is usually very intensive and requiring more staff than older children and adults.
Ezeaka said to prevent preterm births there is need to strengthen the healthcare systems and provide essential drugs and equipment.
She said all stakeholders must come together to promote low cost, effective, innovative medical equipment, adding that due to the immediate challenges to the survival of preterm babies, they require assistance to maintain temperature, breathe and in the area of nutrition.
This equipment, she said, include radiant warmer, oxygen concentrators, respiratory support breathing machines-bubble to aid their breathing; and more invasive mechanical ventilation for tertiary centres, phototherapy machines, pulse oximeters to monitor oxygen levels, glucose meter checks, infusion units, suction machines.
Source:https://guardian.ng/features/studio-24-launches-purple-baby-project-to-reduce-spate-of-premature-mortality/

Temporal Trends in Neurodevelopmental Outcomes to 2 Years After Extremely Preterm Birth

Cheong JLY, Olsen JE, Lee KJ, Spittle AJ, Opie GF, Clark M, Boland RA, Roberts G, Josev EK, Davis N, Hickey LM, Anderson PJ, Doyle LW; Victorian Infant Collaborative Study Group. Temporal Trends in Neurodevelopmental Outcomes to 2 Years After Extremely Preterm Birth. JAMA Pediatr. 2021 Oct 1;175(10):1035-1042. doi: 10.1001/jamapediatrics.2021.2052. PMID: 34279561; PMCID: PMC8290336.
Abstract
Importance: Survival of infants born extremely preterm (EP) (<28 weeks’ gestation) has increased since the early 1990s. It is necessary to know whether increased survival is accompanied by increased neurodevelopmental disability.
Objective: To examine changes in major (ie, moderate or severe) neurodevelopmental disability and survival free of major neurodevelopmental disability at 2 years in infants born EP.
Design, setting, and participants: Four prospective longitudinal cohort studies comprising all EP live births at 22 to 27 weeks’ gestation from April 1, 2016, to March 31, 2017, and earlier eras (1991-1992, 1997, and 2005), and contemporaneous term-born controls in the state of Victoria, Australia. Among 1208 live births during the periods studied, data were available for analysis of 2-year outcomes in 1152 children: 422 (1991-1992), 215 (1997), 263 (2005), and 252 (2016-2017). Data analysis was performed from September 17, 2020, to April 15, 2021.
Exposures: Extreme preterm live birth.
Main outcomes and measures: Survival, blindness, deafness, cerebral palsy, developmental delay, and neurodevelopmental disability at 2 years’ corrected age. Developmental delay comprised a developmental quotient less than -1 SD relative to the control group means on the Bayley Scales for each era. Major neurodevelopmental disability comprised blindness, deafness, moderate to severe cerebral palsy, or a developmental quotient less than -2 SDs. Individual neurodevelopmental outcomes in each era were contrasted relative to the 2016-2017 cohort using logistic regression adjusted for gestational age, sex, birth weight z score, and sociodemographic variables. Changes in survival free of major neurodevelopmental disability over time were also assessed using logistic regression.
Results: Survival to 2 years was highest in 2016-2017 (73% [215 of 293]) compared with earlier eras (1991-1992: 53% [225 of 428]; 1997: 70% [151 of 217]; 2005: 63% [170 of 270]). Blindness and deafness were uncommon (<3%). Cerebral palsy was less common in 2016-2017 (6%) than in earlier eras (1991-1992: 11%; 1997: 12%; 2005: 10%). There were no obvious changes in the rates of developmental quotient less than -2 SDs across eras (1991-1992: 18%; 1997: 22%; 2005: 7%; 2016-2017: 15%) or in rates of major neurodevelopmental disability (1991-1992: 20%; 1997: 26%; 2005: 15%; 2016-2017: 15%). Rates of survival free of major neurodevelopmental disability increased steadily over time: 42% (1991-1992), 51% (1997), 53% (2005), and 62% (2016-2017) (odds ratio, 1.30; 95% CI, 1.15-1.48 per decade; P < .001).
Conclusions and relevance: These findings suggest that survival free of major disability at age 2 years in children born EP has increased by an absolute 20% since the early 1990s. Increased survival has not been associated with increased neurodevelopmental disability.
Source:https://pubmed<a href=”http://Abstract Importance: Survival of infants born extremely preterm (EP) (<28 weeks’ gestation) has increased since the early 1990s. It is necessary to know whether increased survival is accompanied by increased neurodevelopmental disability. Objective: To examine changes in major (ie, moderate or severe) neurodevelopmental disability and survival free of major neurodevelopmental disability at 2 years in infants born EP. Design, setting, and participants: Four prospective longitudinal cohort studies comprising all EP live births at 22 to 27 weeks’ gestation from April 1, 2016, to March 31, 2017, and earlier eras (1991-1992, 1997, and 2005), and contemporaneous term-born controls in the state of Victoria, Australia. Among 1208 live births during the periods studied, data were available for analysis of 2-year outcomes in 1152 children: 422 (1991-1992), 215 (1997), 263 (2005), and 252 (2016-2017). Data analysis was performed from September 17, 2020, to April 15, 2021. Exposures: Extreme preterm live birth. Main outcomes and measures: Survival, blindness, deafness, cerebral palsy, developmental delay, and neurodevelopmental disability at 2 years’ corrected age. Developmental delay comprised a developmental quotient less than -1 SD relative to the control group means on the Bayley Scales for each era. Major neurodevelopmental disability comprised blindness, deafness, moderate to severe cerebral palsy, or a developmental quotient less than -2 SDs. Individual neurodevelopmental outcomes in each era were contrasted relative to the 2016-2017 cohort using logistic regression adjusted for gestational age, sex, birth weight z score, and sociodemographic variables. Changes in survival free of major neurodevelopmental disability over time were also assessed using logistic regression. Results: Survival to 2 years was highest in 2016-2017 (73% [215 of 293]) compared with earlier eras (1991-1992: 53% [225 of 428]; 1997: 70% [151 of 217]; 2005: 63% [170 of 270]). Blindness and deafness were uncommon (<3%). Cerebral palsy was less common in 2016-2017 (6%) than in earlier eras (1991-1992: 11%; 1997: 12%; 2005: 10%). There were no obvious changes in the rates of developmental quotient less than -2 SDs across eras (1991-1992: 18%; 1997: 22%; 2005: 7%; 2016-2017: 15%) or in rates of major neurodevelopmental disability (1991-1992: 20%; 1997: 26%; 2005: 15%; 2016-2017: 15%). Rates of survival free of major neurodevelopmental disability increased steadily over time: 42% (1991-1992), 51% (1997), 53% (2005), and 62% (2016-2017) (odds ratio, 1.30; 95% CI, 1.15-1.48 per decade; P .ncbi.nlm.nih.gov/34279561/


“Movement is my medicine, my meditation, my metaphor and my method, a living language we can rely upon to tell us the truth about who we are, who we are with, and where we are going. There is no dogma in the dance.”
— Gabrielle Roth

COME join me on my daily walk to seminar classes in Denmark Hill, London and we will witness a kaleidoscope of inspiring sounds, colors, and movement of children and teachers as we pass London’s primary school playgrounds.
Are you as shocked and excited as I was to hear music blasting from loudspeakers while children (and some teachers) danced and sang during recess? Brilliant! Education in action, and collaborative activity that feeds the mind, body and spirit.
Watching the weekly recess dance battles at the various schools I pass has brought small moments of joy into my daily life. I love witnessing this promise of a healthy and evolved humanity as I walk through this dynamic and beautiful city and observe an impressive educational system in action. I had a great laugh on one occasion as a child, singing his favorite song loudly, was reminded to sing the “clean” version. As a Zumba instructor, this particular requirement really resonated with me.
My hope is that now and into the New Year, we remember to cherish the small moments that draw us into pure presence and fuel the true meanings of our existence.
My New Year resolution this coming year is to grow my heart through attentive immersion in and reflection on the moments in my life that bring me comfort, ignite my vitality, engage my soul.
What actions did you take or witness that brought joy into your day? What small steps can you imagine that may inspire you to cultivate more happiness in your daily life?
The innocent, noisy, exuberant and chaotic joy of children playing at recess in London reminds me that when we just let go and choose to be authentically present we experience our wholeness, if only for a moment. Thank you, children and teachers of the magnificent city of London.
We heartily wish you All a Healthy, Safe and Joyful 2022!
Bishops Down Primary School
6,689,340 views Stephen Brewin
In May 2017, the children and staff at Bishops Down Primary School made a school video – we are very proud of everyone involved – we hope you enjoy watching it as much as we enjoyed making it! – Clare Owen, Headteacher
Left in Lagos – A Nigerian Surf Film
Sep 9, 2017 Calvin Thompson
Professional surfer’s Luke Davis and William Allioti embark on the most unlikely of surf adventures, missioning through Africa’s largest city in search of a wedging left-hander.









