

Kazakhstan, officially the Republic of Kazakhstan, is a transcontinental landlocked country located mainly in Central Asia and partly in Eastern Europe. It borders Russia to the north and west, China to the east, Kyrgyzstan to the southeast, Uzbekistan to the south, and Turkmenistan to the southwest, with a coastline along the Caspian Sea. Its capital is Astana, known as Nur-Sultan from 2019 to 2022. Almaty, Kazakhstan’s largest city, was the country’s capital until 1997. Kazakhstan is the world’s ninth-largest country by land area and the world’s largest landlocked country. It has a population of 19 million people and one of the lowest population densities in the world, at fewer than 6 people per square kilometre (15 people per square mile). Ethnic Kazakhs constitute a majority of the population, while ethnic Russians form a significant minority. Kazakhstan is a Muslim-majority country, although ethnic Russians in the country form a sizeable Christian community.
The Healthcare in Kazakhstan is a post-Soviet healthcare system under reform. The World Health Organization (WHO), in 2000, ranked the Kazakhstani healthcare system as the 64th in overall performance, and 135th by overall level of health (among 191 member nations included in the study).The Human Rights Measurement Initiative finds that Kazakhstan is fulfilling 79.7% of what it should be fulfilling for the right to health based on its level of income. When looking at the right to health with respect to children, Kazakhstan achieves 96.1% of what is expected based on its current income. In regards to the right to health amongst the adult population, the country achieves only 80.9% of what is expected based on the nation’s level of income. Kazakhstan falls into the “very bad” category when evaluating the right to reproductive health because the nation is fulfilling only 62.1% of what the nation is expected to achieve based on the resources (income) it has available.
- GLOBAL PRETERM BIRTH RATES – Kazakhstan
- Estimated # of preterm births: 5.18 per 100 live births
- (USA 9.56-Global Average: 10.6)
- Source- WHO 2014- https://ptb.srhr.org/

Through the Looking Glass-Neonatal Womb Warriors-May, 2023
Kathy:
Preemies are people, people that make up over 11 % of our population globally.
Kathryn was born in 1991. At that time, the only publication available to parents in her birth hospital was a pamphlet targeting the needs of parents whose child had died or was dying. In our case, it was pertinent, as Cruz, Kathryn’s twin, did pass following his birth. The community library had nothing for preterm birth families to reference. There were no support groups to provide direction. Enlightenment, a hard path, was a moment by moment experiential journey. Like many of you who may have experienced a preterm birth earlier in time, we lived, we endured, we moved forward, we survived and evolved.
On April 30, 1993 Tim Berners-Lee , a fellow at CERN, released the source code for the world’s first web browser and editor. The browser that he dubbed WorldWideWeb became the first royalty-free, easy-to-use means of browsing the emerging information network that developed into the internet as we experience it now (a magical moment!). Trillions of lights at our Preterm Birth Community fingertips, alive and expansive….. a magnificent opportunity to share, learn, connect, explore, create and collaborate globally.
In February 2016 we shared our first Neonatal Womb Warrior blog. Our outreach was and remains focused towards building a matrix globally that would empower the health and well-being of our preterm birth community, our Family, at large. We are the resources we need! We believe that collaboration towards our mutual benefit and well-being is not only possible, but also “profitable” in every progressive and positive way. Three significant observations were foundational towards the development of our efforts to experience, understand, connect with and serve the Preterm Birth Community:
- In comparison to 1991, preterm birth families had access to rich resources to help them navigate and empower their preterm birth journeys in many parts of the world.
- Preterm birth community members were represented by many critical partner affiliates including but not limited to preterm birth survivors, preterm birth families, healthcare providers, ancillary service providers, inventors, researchers, educators, community/governmental agencies, etc. With increasing necessity and requiring immediate attention within our preterm birth community was a need for appreciating, humanizing, supporting, and advancing/growing our healthcare partner community. We felt a need to explore, identify, and address any and all resistance presented that may deter us from our acknowledgment of the humanity and humane needs of our healthcare provider workforce.
- Preemies are people who deserve and require healthcare and education complimentary to their entrance into life and their pathways throughout their life journeys.
We have a few observations and thoughts about the preterm birth community and it’s evolution we choose to share:
Resources to guide and support Preterm Birth parents/caregivers are currently abundant and growing in many places worldwide. In places globally that lack preterm birth support, education, and care including many rural communities like those in the USA, there is a need for resource development and access, as well as the implementation of comprehensive care planning and facilitation.
There remains at times within the Global healthcare community an attitude toward the preterm birth survivors that implies “ you are lucky to be alive, a lot of time and money were spent on you already, enough is enough, get over it”. This is especially apparent in the lack of resource development towards pre-verbal PTSD, a condition very relevant to the preterm birth survivor community, the non-development of preterm birth life span medical specialization and identification, and the lazy and likely misdiagnoses of preterm birth learning and psychosocial development based on research related to symptom expression as opposed to the gathering of objective information gained from the preterm birth survivor community itself during development over lifespans and based on research that provides an opportunity to explore brain development, socialization, health, etc. from a clean and relevant platform.
In 1991, and even in 2016, the Preterm Birth Community was significantly compartmentalized. Doors were significantly closed between families, healthcare providers, researchers/inventors/suppliers/ancillary service providers, and our preterm birth survivor members. Healthcare providers were and remain dehumanized to a significant extent by the Public. We believe that bringing attention to the humanity/personal experiences of our healthcare providers is required if we want access to healthcare for ALL of our community members. With more preterm births occurring globally and given the overwhelming shortages of and the current exodus of healthcare providers, now more than ever we are called to show our appreciation and offer support to our healthcare community partners. The hard cold fact is that without healthcare provider access and presence in our lives the number of our community members who would have/may die and the families damaged by the loss of a child is unfathomable (but we should try to “fathom” it) and unnecessary.
Dehumanization of any limits ALL. Numerous health care providers involved in preemie care reported that they had never or had rarely interacted with the preemie survivors they had so diligently and lovingly cared for. There is sorrow in their reporting. We can fix that and each of us can choose to do so in some unique way.
When Kat and I first started the blog, some practitioners expressed alarm that we were sharing information with the Public that even they, preterm birth healthcare specialists, had not been aware of. Their fear of not being in control of the information and therefor their scope of responsibility was significant. From our perspective progressive change directed towards supporting our preterm birth community at large was a more compelling pathway. Discomfort and progression are well-orchestrated partners when moving towards positive advancement and change. Opening doors and windows, letting in light and air, gives life opportunity and supports human advancement.
In 1991 when a NICU baby in the USA was discharged from the neonatologist, nurses, and staff to the care of a pediatrician, the pediatrician likely had little to no education regarding providing medical evaluation and care to a developing preterm birth survivor. Preterm birth infants and children were treated with no targeted attention to their pathway into this human experience. The situation has not changed significantly although specialty training in becoming more available to medical residents, neonatologists, pediatricians, therapists, scientists, innovators and nurses. The nursing profession has been extremely proactive in this regard, especially within their specialty. While collaboration is advancing between healthcare specialties locally and globally, increased collaboration between neonatologists, medical residents, and nursing staff is imperative and encouraged.
Opportunity is something we create through our inner and interpersonal expansion of vision and the sharing of perspectives. We find our Neonatal Womb Warrior-Preterm Birth Family/Community to be inspired, optimistic, creative, while carrying a certain lightness of being as we expand our horizons and explore the possibilities within our life stories. We are grateful for your presence in our lives.
KAT’s Summary:
As a preemie survivor, growing up as a pediatric and adult patient I experienced a lack of holistic clinical care wherein the impact and potential implications of my prematurity remained unacknowledged and/or simply side-lined to fulfilling a standard checklist. Within society and the medical community, certain ideologies, and theories pathologizing myself and other preemie survivors’ quality of life conditions and intellectual capabilities or classifications have often been mislabeled or placed into a box where the true etiology of our long-term health, mental and physical capacities are not fully realized. For instance, I like many micro-preemies experienced “learning difficulties” due to dyslexia, and dyscalculia and was thought to experience challenges in feeling and outwardly expressing my emotions. However, when I reached my later twenties, I experienced an outburst of intellectual growth making me question my true neurodevelopment and that of other preemies who historically have been highlighted for experiencing the same “brain revolution.”
For example, I am cautiously hesitant to buy into the common thought that preemies may have a higher rate of falling along the autism spectrum. Had I been born in 2019 vs 1991 I feel quite confident I would have fallen into this category. While I too agree that this domain of research is critical for those especially who meet all of the criteria, I believe firmly that there is vastly more research that needs to be performed so that the clinical and Public neonatal community does not limit itself and those of us born early into a categorical box that fails to address the full range of our developmental health as a whole.
I highly encourage longitudinal research that thoroughly examines preterm birth survivor long-term development to fully examine our etiology and health development broadly. Studies ranging from 1 month-5 years of age are inadequate. Moreover, making strides to engage our clinical research & ancillary community in collaboratively establishing specialized pediatric and adult care for preemie survivors is critical towards advancing neonatal lifespan healthcare. We are living longer; we are surviving the odds at a rate higher than ever before. We are empowered to change the life course of millions. Let’s get to it!

COMMUNITY

America deliberately limited its physician supply—now it’s facing a shortage
Why we’re more worried than ever about a physician exodus – Daily Briefing
Posted on February 16, 2022 Updated on March 18, 2023

Historically, the number of physicians in the United States has been deliberately limited in an attempt to avoid massive physician surpluses—but now, there is a growing shortage of doctors, which negatively affects the country’s health care system and people’s health, Derek Thompson writes for The Atlantic.
How the U.S. capped its physician supply
According to Thompson, the United States has one of the lowest number of physicians per capita, largely due to deliberate efforts to limit the overall physician workforce.
“There’s a huge scarcity of primary care doctors, like pediatricians, and many of us are operating in a scarcity framework without enough resources,” said Elizabeth Erickson, a professor at Duke University‘s School of Medicine.
In 1981, a report from the Graduate Medical Education National Advisory Committee concluded that the country would soon face a massive physician surplus and recommended actions to limit the number of new domestic physicians, as well as immigrant physicians. In response to the report, the federal government reduced funding for both medical school scholarships and residency training programs.
In addition, U.S. medical schools enacted a moratorium from 1980 to 2005, which limited the number of new medical schools and restricted medical school class sizes. Although the U.S. population grew by 60 million people during that period, the number of medical school graduates remained mostly stagnant and has not completely rebounded even after the moratorium ended, Thompson writes.
Separately, the process to become a physician in the United States is more arduous and expensive than other peer countries, particularly those in Europe. According to Thompson, the United States requires doctors to earn a four-year bachelor’s degree, as well as attend four years of medical school, but most European countries have one continuous six-year medical program instead. In addition, many medical school graduates have between $200,000 and $400,000 in student loans when they enter the workforce.
However, American doctors’ longer training periods have not translated into better health for Americans as a whole, Thompson writes. In fact, a recent study found that Americans die earlier than their European counterparts at every age and income level.
Ways to address the U.S. physician shortage
Growing the physician workforce over the next few years will be critical, Thompson writes, not only to deal with the effects of the current Covid-19 pandemic, but also to care for the United States’ older and aging population. In 2018, the Association of American Medical Colleges predicted that the United States would be short between 43,000 and 121,000 physicians by 2030.
According to Robert Orr, a policy analyst who studies health care policy at the Niskanen Center, one way to increase the number of physicians is to expand medical residency programs. “This might be the key bottleneck,” he said. More funding for residency programs would allow medical schools to grow, which will mean more medical students and, ultimately, more doctors.
Aside from just increasing the number of doctors, states could also increase the total supply of care available, Thompson writes. For example, states could allow more nurse practitioners to substitute for doctors and expand telemedicine services, particularly to rural and underserved areas.
The United States also needs to build its health care infrastructure, such as clinics and hospitals, as it works to expand its physician workforce. “We need a system of health care development banks that issue guaranteed loans for infrastructure projects,” Orr said. “That’s how the health care system was originally built up until the 1980s, with government-backed finance.”
Although Thompson notes that there are several potential downsides of having too many doctors, including lower physician wages and more student debt, he ultimately argues that “[s]ick, aging, and buckling under two years of pandemic mayhem, America desperately needs more physicians.” (Thompson, The Atlantic, 2/14; Orr, Niskanen Center, 9/8/2020)
Source:https://www.advisory.com/daily-briefing/2022/02/16/physician-shortage

Give Health Care Workers the Mental Health Support They Deserve
States must do more to help clinicians access mental health care. Their lives depend on it.
By Corey Feist, Arianna Huffington, Deborah Marcus, and Michelle A. Williams – Nov. 29, 2022, at 11:36 a.m.

Advocating for health care workers has become an essential part of our day-to-day. In March, we were proud to see the Dr. Lorna Breen Health Care Provider Protection Act enacted to provide $135 million for programs aimed at supporting the mental health and well-being of health workers. However, while this was a welcome first step, it’s only the beginning of the work needed to protect our clinicians.
READ:
The next crucial step falls to the states: They must remove language in their licensing and credentialing processes that stigmatizes health care professionals who have sought treatment for mental health concerns.
Our research has identified 31 states, plus the District of Columbia, that may still use invasive or stigmatizing language requiring applicants to disclose any history of mental health concerns or to explain why they have taken breaks from work. Some require applicants to disclose any past psychiatric impairment, potentially going back decades, even to adolescence. These questions might violate the Americans with Disabilities Act. They certainly violate applicants’ privacy. And there is significant evidence that they deter clinicians from seeking the care they need – at tremendous risk to their well-being and their lives.
Indeed, a survey of more than 1,500 physicians conducted this year found that 80% agree there is stigma around doctors seeking mental health care. Nearly 40% reported that either they personally or a colleague they know has been scared to seek mental health care because that treatment would need to be disclosed on their licensure, credentialing or insurance applications.
This is unacceptable.
Like everybody, health workers deserve the right to pursue the care they need whenever they need it, without fear of losing their license or job. This is especially important now, as health care workers have reported sharp increases in emotional exhaustion due in large part to the extraordinary strain of caring for patients, while also enduring a surge of intimidation, threats and physical violence during the COVID-19 pandemic.
Mental health questions were often added to licensing applications out of a misplaced desire to protect the public from clinicians who might not be fit to give care. Yet there is no evidence that these questions serve that function.
On the contrary, the public interest is harmed by these questions, since we know that when doctors, nurses and other clinicians are afraid to seek the care they need, they may find themselves unable to work due to depression or burnout. Some may turn to drugs or alcohol. And tragically, some will turn to suicide. In fact, stigma associated with seeking – or even discussing – behavioral health care is a primary driver of suicide among the health care workforce.
The Dr. Lorna Breen Act is named after the sister-in-law of Corey Feist, a co-author of this piece. An emergency room physician, Lorna died by suicide in April 2020, after weeks of incredibly intense work caring for patients in the first wave of COVID-19. At one point during that surge, Lorna called her sister to confide that she was overwhelmed with exhaustion and grief – but she was fearful that she would lose her medical license or be ostracized at work if she acknowledged that she needed help.
In the years since Lorna’s death, we have heard from many families who have lost physician loved ones to suicide. We recently connected with an emergency medicine doctor in Florida who reported that four of her physician colleagues died by suicide this summer. In too many of these cases, the clinicians have acknowledged to friends or family that they are reluctant to get treatment because of the stigma around mental health issues.
One such tragedy involves Dr. Matthew Gall, a devoted oncologist who practiced medicine for 16 years in Minnesota, one of the states that until recently used invasive questions on licensing applications. In 2019, Matthew moved to North Carolina with his wife and their three children. The move to a new practice was difficult, and Matthew struggled with depression, yet he declined to seek help. His wife, Betsy, told an interviewer that her husband felt “ashamed and embarrassed” about his depression, and feared he would lose his medical license and his livelihood if he sought treatment. “He honestly thought that he’d no longer be able to be a practicing oncologist,” Betsy said. “The fear was real, and being a doctor meant everything to him.” Matthew died by suicide on Thanksgiving Day 2019.
A terrible irony in this tragedy is the fact that North Carolina does not actually ask intrusive questions about mental health treatments in its licensure process. But having just moved to the state, Matthew was not aware of that fact. Lorna, too, was unaware that New York does not use invasive questions.
These stories are painful. They are powerful reminders that we must work toward universal reform of licensure applications, as our team did in Minnesota, which updated its questions to be less stigmatizing after testimony from Lorna’s sister and brother-in-law. It’s also clear that simply changing the language on applications is not enough. We must also get the word out widely, so no clinicians ever fear they will lose their job if they seek the help they need. In addition, we must continue to change the culture inside health care systems so that physicians, nurses, pharmacists and other health care workers feel comfortable being open about their mental health concerns and their need for support.
We are fighting for those reforms through our campaign ALL IN: Well Being First for Healthcare, which brings together more than a dozen organizations including the American Medical Association, the American Hospital Association, the American Nurses Foundation and the Physicians Foundation. Thousands of individuals have joined us in contacting state medical boards to demand change.
We are also working to address clinician burnout through common-sense reforms that we expect will eliminate some of the bureaucracy that can consume so much of a clinician’s time and remove the joy from patient care.
Ensuring that health care workers can access necessary mental health care is critical for their well-being and for the health of our entire country. Let’s do our part to support them. Together, we can show our vital health care workforce that they aren’t alone in this fight for their lives.

*** One of the GREATEST vocalists we have ever experienced. A CRUSHING performance! Don’t miss this truly amazing artist….
Dimash – SOS | 2021

11,326,999 views Sep 21, 2021 #dimashkudaibergen #dimash #dqhttps://band.link/Dimash_Qudaibergen On January 16, the TIXR streaming platform hosted an online concert DIMASH DIGITAL SHOW, where the artist performed ‘SOS D’un Terrien En Détresse’. Dimash Qudaibergen performed the song “SOS” in the 1st round of the Chinese contest” I am a Singer ” in 2017. The next day, more than 600 million viewers learned about Dimash


Amid Healthcare’s Great Resignation, Burned Out Workers Are Pursuing Flexibility And Passion
Deb Gordon Contributor

The Great Resignation—the mass exodus of unsatisfied workers—has hit few industries harder than healthcare. According to some reports, the field has lost an estimated 20% of its workforce, including 30% of nurses.
This year alone, nearly 1.7 million people have quit their healthcare jobs—equivalent to almost 3% of the healthcare workforce each month, according to the U.S. Bureau of Labor Statistics.
And a recent survey of 1,000 healthcare professionals showed that 28% had quit a job because of burnout.
These departures not only create current and fear of future staffing shortages, they raise another question: Where are all those highly skilled workers going?
Many healthcare workers who quit take other healthcare jobs, though sometimes under substantially different circumstances.
Lauren Berlin, RN, 45, has been a nurse in Wisconsin and Florida for 21 years, most recently employed as director of nursing for long-term care facilities. In that role, she says she was expected to be available at all times, every day of the year.
“My phone was never off,” she said. “I was burned out. I loved bedside nursing, but I desperately needed work-life balance.”
Berlin quit her full-time job and now takes shifts through CareRev, a staffing app which allows clinicians to sign up for shifts online based on their schedule, preferences, and availability.
This flexibility allows Berlin to focus on her other passion: coaching track and field in inner-city Milwaukee.
“If your home calendar is your priority, then you schedule your work shifts around your home calendar…You want to take a vacation? Go ahead, you don’t need to ask anyone,” Berlin said. “I work for myself, on my own terms.”
According to Will Patterson, CEO and founder of CareRev, Berlin reflects a growing trend among clinicians.
“Today’s worker expects greater flexibility. They expect to have a greater degree of freedom over when they work and for whom,” Patterson said. “Clinical professionals are no exception.”
A former trauma nurse, Patterson saw firsthand the impact of inflexible hospital scheduling, which could leave the ICU short-staffed when patient volume peaked.
“When you’re taking on responsibility for more lives than you can reasonably handle—for days at a time—you burn out quickly,” he said. “Now, after over two years of fighting the pandemic, that burnout is at an all-time high. And as the nurse shortage worsens, that burnout is only going to continue to accelerate.”
According to Patterson, many burned out clinicians haven’t lost their passion for healthcare, they just want more autonomy and work-life balance.
Lack of work-life balance caused Jill Bowen, 45, to quit her job as a director of physical therapy in the home health industry. Her productivity was measured by the number of visits completed with no credit for all the time she had to spend on phone calls, documentation, and scheduling.
“Payment, regulations, and all the red tape is the most stressful part of the job,” Bowen said. “When an agency is driven by profitability, marketing promises or non-compliant provider demands, clinicians are pressed to comply, and patient care suffers.”
Now, Bowen works as an implementation consultant with Axxess, a software company that serves home health agencies. She encourages other clinicians to recognize—and use—their transferrable skills.
“There are lots of jobs available for people with the skills developed in the healthcare field,” Bowen said. “We have skills that can be transferred to other professional areas, such as being organized, effective communicators, and a team player.”
Some burned out workers are using their transferrable skills to launch their own ventures.
Taylor Bonacolta, 28, of Fort Myers, Florida, quit her job as a registered nurse in a pediatric intensive care unit a year ago due to the stresses of the pandemic combined with having two young children. Instead of getting another job, Bonacolta launched June and Lily, a business to provide support for new mothers.
“If there are any other healthcare workers out there considering quitting, I would remind them that there are so many different ways we can help others as nurses,” Bonacolta said.
The pandemic also prompted Jackie Tassiello, 34, to rethink her career. A licensed, board-certified art therapist in New Jersey, Tassiello was employed for almost four years in the pediatric cancer department at NewYork-Presbyterian Komansky Children’s Hospital. Before the pandemic, she often carried a caseload of 25 children in a day, all navigating cancer, blood disorders, or gastrointestinal diseases.
During the pandemic, Tassiello was redeployed to provide emotional support and meet basic needs for frontline medical staff working in Covid-19 units. She said she remembers seeing staff in hazmat suits responding to a patient in distress and thinking, “That could be me; that could be anyone I love.”
Those experiences caused Tassiello’s own priorities to change.
“I decided that I wanted to scale down in order to be more present. I also needed time off to recalibrate and heal,” she said.
Now running her own psychotherapy practice, Tassiello has some advice for healthcare organizations hoping to retain staff: “Hospitals need to solve issues at the core, not with gift cards and lunches,” she said. “There are systemic problems that no amount of bonuses can fix.”
Some healthcare workers are giving up clinical work altogether and turning to creative pursuits.
Cari Garcia, LCSW, 38, most recently worked as a psychiatric emergency room social worker in a large Florida hospital. She says she quit due to a toxic work environment, unsupportive administration, verbally and physically abusive patients, and pay that did not justify the level of stress she had to endure.
Garcia turned a food blog she’d run as a hobby for ten years into her primary source of income and now says she makes more money than she would as a social worker. Garcia encourages other healthcare workers considering quitting to take the leap.
“The minute you’re on the other side, you’ll ask yourself why you didn’t do it sooner,” she said. “I sleep better, I’m able to be present for my family, and my quality of life is through the roof.”
The Great Resignation isn’t just about clinicians. Christopher K. Lee, MPH, 31, had been working in healthcare management for more than a decade. Last month, he resigned from a senior manager role at UCLA Health after being required to be in the office every day since October 2021.
“I tried to make it work, but in March I decided I couldn’t do it anymore,” Lee said. “Like many people, during the pandemic I reflected on my priorities, and spending 3+ hours commuting a day no longer aligned with what I envisioned for my life.”
Now, Lee says he is writing a book about professional networking and doing advocacy work in teen and young adult mental health, projects he always wanted to do “someday.”
Lee said, “In the shadow of the pandemic, I decided: If I don’t do them now, what if I never get a chance?”

Nursing Post Pandemic: The Path Forward
Vallire Hooper, PhD, RN, CPAN, FASPAN, FAAN⁎
J Perianesth Nurs. 2023 Feb; 38(1): 1–2.
Published online 2023 Jan 23. doi: 10.1016/j.jopan.2022.12.001

As we move into 2023, we are, I hope, moving into a brave new future. COVID-19, while still evolving and highly prevalent, is moving into more of an endemic, flu-like state as opposed to a pandemic presentation. The health care system, to include the nursing profession, however, has been left in a shambles. The reality, as we all know, is that the health care system was teetering on the edge of disaster prior to the onset of the pandemic. COVID-19 was essentially the “straw that broke the camel’s back.” This statement is particularly true for the nursing profession.
The nursing profession, and thus health care as we know it, is on the brink of implosion. Nurses of all ages are leaving at record numbers. Many are retiring, and taking decades of experience with them. Many newer nurses, however, are leaving the bedside within a year to two years of hire; some to advance their education and move out of the acute care setting, but many are leaving the profession entirely. The number of nursing students in the pipeline is in no way sufficient to fill the gap, and current nurse retention strategies are inadequate and outdated. The nursing profession, and particularly the future of health care in the acute care setting, is at a tipping point. If we, as the nursing profession, do not take the lead in staving off disaster, someone else will fix it for us, and we will likely not be happy with the results. Nurses, as a profession, must find a new path forward.
The numbers as they currently stand are not pretty, yet, not surprising. A Becker’s report published in October of 2022 reported some disturbing statistics:
- Regional RN turnover percent rate changes from 2020 to 2021 ranged from 3.2% to 12.2%.
- The overall nursing turnover rate in 2021 was 27.1%, up 8.4% over the previous year.
- RN turnover rates in step down units, emergency departments, behavioral health, and telemetry increased from 101.3% to 111.4% over the last five years.
- Average turnover cost for a nurse is $46,100.00, up 15%.
- 60% of survey respondents reported an RN vacancy rate of 15%.
- It now takes an average of 3 months to recruit an experienced RN.
A 2022 survey of physicians, registered nurses, and advanced practice providers showed that 25% of respondents were considering switching careers. To no surprise, 89% of those considering leaving the profession cited burnout as the primary reason. These statistics confirm what is now common knowledge: clinician burnout is a real threat to the stability of the US health care system. Wellbeing is also commonly acknowledged as the antithesis to that burnout. Yet how we define wellbeing, and how we enhance nursing wellbeing, is in need of some clarity and consensus building.
Wellbeing has many components: personal, spiritual, physical, mental, financial, etc, but what does well-being mean for the nurse? A recent concept analysis defined nurse wellbeing as “being the best “you” that you can be, and bringing the best “you” to your work, to your team, unit, and/or organization.3” On face value, this definition implies a personal perspective or ownership. It is “your” responsibility to attain wellbeing. Many nursing leaders and national nursing organizations have fallen victim to this attitude….if one only took better care of themselves, took time for meditation, attended wellness classes, etc, then the nurse could attain that ever elusive goal of wellbeing. The reality, however, is that nurse wellbeing cannot be obtained through individual pursuit. Nurse wellbeing is primarily a consequence of work environment issues, of having one’s basic human needs met in the work environment.
Nurse wellbeing emanates from a work environment in which one is adequately paid, protected, and supported. An environment where one’s workload is manageable and the nurse is able to provide the nursing care that the patient requires. An environment where the nurse can take a break without interruption, where the nurse has control of their schedule, where they are respected and have a sense of belonging, and where they feel protected and safe from harm. Nurses do not need wellbeing officers and classes. The evidence clearly supports that nurses are looking to be treated and supported as professionals….as the guardians of safe, quality health care. A work environment must be created in which nurse wellbeing can flourish. The work environment must support the basic needs of nurses. Nurse burnout does not result from an individual’s failure to pursue wellbeing; nurse burnout is a result of a failed health care system.
In my opinion, the first step down the pathway to a new nursing reality is in the recognition of the significant impact of nursing care that we provide impacts patient outcomes. This work begins in the C-suite. Nursing must no longer be considered as the primary cost center in the hospital. The care that nursing provides must no longer be wrapped up in the bed charge. Nursing must be recognized for what we are, the major revenue generator for the hospital. Without a nurse, there is not a hospital bed. The one and only reason that a patient is admitted to the hospital is because they require 24/7 nursing care. If a patient does not require 24 hour nursing care, then they can be managed via services in an outpatient setting. Nursing leaders and nursing administrators must own this power and make their voice known in the boardroom. They must support the bedside nurses they lead and no longer cave to pressures to “cut costs” in the nursing department. The nursing department is the center to which all other departments connect. We are the core that holds the acute care setting together. Nursing must own our positive impact on safe, quality patient outcomes and be reimbursed accordingly. Might this mean that nursing should be held accountable for critical nurse-sensitive quality measures? Yes. But this also means that nursing must be supported with adequate resources to deliver quality nursing care. Might nursing care delivery models need to be restructured to provide cost-effective care delivery at the bedside? Yes. Must federal policy and reimbursement structures be modified to reflect the criticality of nursing care to safe, patient care delivery? ABSOLUTELY!
The path forward to a new nursing reality will not be easy. It will not be without wrong turns, but we must traverse this long and difficult journey together. The new reality, the new future of nursing, will require significant changes in approaches to nursing leadership, nursing education, and the individual nurse’s approach to patient care. Nothing, and I mean nothing, will be the same as before the pandemic, but with hard work and collaboration, a new future can be obtained.
Source:https://www.ncbi.nlm.nih.gov/pmc/articles/PMC9868216/

HEALTHCARE PARTNERS
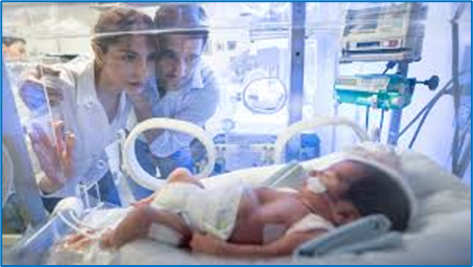
Is NICU Care Unnecessary for Some Premature Infants?
Apr 5, 2023 Michele Meyer

Findings reported this month in Pediatrics add to the evidence suggesting that neonatal intensive care units (NICUs) may be overused. Routine NICU care for low-acuity premature infants may be unnecessary and have a negative effect on breastfeeding, conclude the authors.
More than half (56%) of infants born at 35 weeks gestation are admitted to neonatal intensive care units (NICU). But is that precaution always medically needed — and could it cause harm among America’s 75,000 such early arrivals each year?
Even with rates of 20% for some areas, the number of NICU admissions has been increasing across all birth weights. That is “raising concern about NICU overuse,” said Andrea Wickremasinghe, M.D., neonatal specialist for Kaiser Permanente in Santa Clara, California.
Factors fueling such concerns include a California study showing that 34.5% of NICU admissions were for mild conditions, “and that hospitals with more NICU beds had an increased likelihood of NICU admissions,” she said.
To learn if rising NICU care for babies born at 35 weeks gestation is needed, Wickremasinghe and her colleagues studied chart data for 5,929 premature babies born from 2011 to 2021 at 13 Kaiser Permanente Northern California hospitals. They reported their results in the April 2023 issue of Pediatrics.
A normal pregnancy can range from 38 to 42 weeks. Infants born before 37 weeks are considered premature.
The study excluded premature babies with congenital anomalies or who needed antibiotics or respiratory support within two hours of birth. Instead, researchers focused on the remaining 15% of babies born at 35 weeks gestation.
Researchers found significant tradeoffs for those cared for in the NICU out of what they determined was “likely discretionary or hospital policy.”
Babies in NICU were hospitalized 58 hours longer than other newborns, and babies admitted to NICU within two hours of being born were over three times more likely (67% vs. 21%) to be hospitalized for four days or longer.
On the other hand, the babies taken care of the NICU babies were half as likely (3% vs. 6%) to be readmitted within a month of being discharged.
The study said many readmissions were for “transient conditions that are more prevalent in the first week after birth.” Those include jaundice (74.6%), hypothermia and failure to thrive.
“Many of these morbidities are mild and could be managed in a mother/baby unit,” Dr. Wickremasinghe said. Such babies then could benefit from being with their mothers versus being isolated in NICU.
Mothers are affected, too. Those with infants in NICU “were more likely to be stressed, depressed and anxious, all of which impact breast milk production” and, ultimately, the bonding created by breastfeeding.
By contrast, infants staying with their mothers instead of going to NICU caused less emotional and financial stress for their families.
The takeaway from Wickremasinghe and her colleagues: “Routine NICU admission may be unnecessary for low-acuity infants born at 35 weeks’ gestation.”

Parents Are Not Visiting. Parents Are Parenting
Bracht, Marianne RN, RSCN; Pediatrics; Franck, Linda S. PhD, RN, FRCPCH, FAAN; O’Brien, Karel MB, BCh, BAO, FRCPC, MSc; Pediatrics; Bacchini, Fabiana MSc, BJ
Advances in Neonatal Care 23(2):p 105-106, April 2023.

In their article “A Quality Improvement Project to Reduce Events of Visitor Escalation in the Intensive Care Nursery” (Vol 22, No. 1), the authors make repeated references to “visitors” to the neonatal intensive care nursery (NICU).
As seasoned healthcare professionals and advocates for parents of premature and sick infants, our position is this: Parents are not visitors. Parents are parents—their child’s first and most important caregiver.
Globally, healthcare organizations have traditionally positioned parents as visitors. This language is used not just in articles like this one but also frequently present in hospital documents, signage, and in the ways parents are spoken to and about in the hospital.
Preterm birth is traumatic. Often unexpected and unplanned, a preterm delivery to a medically fragile infant can leave a mother feeling like her body has failed. Parents are typically separated immediately from their infant, robbing them of that “moment” they have been waiting for—the moment they become parents. In the hours and days that follow, parents may not be allowed to hold or touch their infant. The clinical terms used to talk about their infant seem like a foreign language, everything is unfamiliar and sterile, and parents do not have any idea what to say, do, or ask. Parents of premature and sick infants are scared and anxious. They can feel powerless, alienated, alone—outsiders in their own infant’s life.
Therefore, language is so important. Calling parents visitors contributes to a culture of experts versus guests and us versus them.3 It evokes feelings for parents that this is the hospital’s infant, not your infant.4 Healthcare professionals decide who can touch and care for your infant, when, and for how long. The word “visitor” and how we use it to describe parents—in writing as well as verbally—is simply inaccurate. Parents are an infant’s primary caregiver. The words we use, as well as our tone, body language, and communication style, strongly affect how healthcare professionals see parents—and how parents see themselves. The culture of “allowing” parents’ permission to care for their premature or sick infants must shift.
Instead, healthcare providers’ words, actions, and knowledge should be a tool for helping parents learn to care for their sick newborn, build trust and rapport, and enable open communication.5 The first days and weeks in the NICU are formative for the parent–infant relationship and can make or break parents’ feelings of confidence, competence, and connection to their new infant. Parents must be at the center of a premature or sick infant’s care team.
Changing the language, we use, to talk about parents is a simple, cost-effective way to promote a culture of inclusion and involvement and improve outcomes. Looking at the wording in unit policies, notice boards, signage, parent education materials, staff presentations, in-services, training, and orientation is a good start.
Calling parents “visitors” is exclusionary. Parents are not visiting. Parents are parenting.

About 100,000 nurses left the workforce due to pandemic-related burnout and stress, survey finds

About 100,000 registered nurses in the US left the workplace due to the stresses of the Covid-19 pandemic, according to the results of a survey published Thursday by the National Council of State Boards of Nursing.
Another 610,388 registered nurses, who had more than 10 years of experience and an average age of 57, said they planned to leave the workforce by 2027 because of stress, burnout or retirement. The same was true of 189,000 additional nurses with 10 or fewer years of experience and an average age of 36.
The survey found that there were over 5.2 million active registered nurses and 973,788 licensed practical nurses or vocational nurses in the US in 2022. The researchers analyzed data from 29,472 registered and advanced nurses and more than 24,000 licensed practical or vocational nurses across 45 states. More than a quarter of those surveyed said they plan to leave the industry or retire in the next five years, the study says.
About 62% of the nurses surveyed said their workload increased during the pandemic, and 50.8% said they felt emotionally drained at work.
Almost half of nurses said they felt fatigued or burnt-out: 49.7% and 45.1%, respectively. These concerns were seen most in nurses with less than 10 years of experience.
Maryann Alexander, chief officer of nursing regulation at NCSBN and one of the authors of this study, said she is shocked by the findings of the study, especially related to younger nurses.
Soon, the industry will rely on nurses with less than 10 years of experience to act as mentors, managers and leaders in nursing care, Alexander said.
“It will send us into a health care crisis of huge proportions,” Alexander said.
She said that while it is common to see young nurses leaving the industry to go back to school and get more education, it is uncommon to see young nurses leaving due to stress and burnout.
“That is a huge cause for concern,” Alexander said.
This exhausted tone was a driving factor behind a strike in New York in January, when over 7,000 nurses took to the streets to call attention to staffing shortages and burnout.
Enter your email to sign up for the Stress, but less newsletter.
Bottom of Form
“We are sick and tired of the hospital only doing the bare minimum,” said Danny Fuentes, a union official who spoke to the crowd during the strike. “Time and time again, we are forced to take unsafe patient loads. We are humans, and we are burnt-out. And we are tired. And the hospital doesn’t seem to care. All they see are profits. We don’t want to be out here. We would much rather be with our patients. We need a fair contract to protect our patients.”
deals with the two hospitals involved, Mount Sinai Health System and Montefiore Health System. The union said the deal would provide enforceable “safe staffing ratios” for all inpatient units at Mount Sinai and Montefiore.
Montefiore agreed to financial penalties for failing to comply with agreed-upon staffing levels in all units.
The researchers on the new survey say their findings pose a threat to the US workforce, especially among younger and less experienced nurses. The National Council of State Boards of Nursing says hospitals and policymakers should be quick to enact solutions and address these challenges.
Source:https://www.cnn.com/2023/04/13/health/nurse-burnout-post-pandemic/index.html

PREEMIE FAMILY PARTNERS

A New Patient Population for Adult Clinicians: Preterm Born Adults
Amy L. D’Agata Carol E. Green Mary C. Sullivan
Open Access Published: January 28, 2022DOI:https://doi.org/10.1016/j.lana.2022.100188

What if a single event could sway health, exercise capacity, learning style, social interactions, and even personal identities–yet individuals had no memory of the event? Adults born preterm are an under-recognized and vulnerable population. Multiple studies of individuals born prematurely, including our 35-year longitudinal study, have found important health concerns that adult healthcare providers should consider in their assessments. Concerns include increased rates of cardiovascular disease, metabolic syndrome, depression, anxiety and attention problems, lower educational attainment and frequency of romantic relationships.
A Nordic study of over six million individuals found a linear relationship between gestational age and protection against early adult mortality, with preterm individuals showing 1⋅4 times increased likelihood of early mortality as full-term peers.
At the same time, surviving premature birth has become increasingly common. For the last several decades, nearly one in nine U.S. babies is born early, and now more than 95% survive.
Global prevalence and survival data indicate more than 15 million preterm birth survivors annually reach adulthood.
This suggests a new population of individuals with emerging healthcare needs for adult health providers.
Birth history should be part of every patients’ medical record.
Due to the varied risks and prevalence of premature birth, all healthcare practitioners should be aware of the potential for long-term effects. With one in ten 30-year-old patients born preterm, clinical specialists who treat long-term complications of prematurity (i.e., neurology, psychiatry, cardiology) may have more preterm-born patients. Recognizing preterm birth as a cumulative, lifelong risk factor is the first step.
As clinicians and researchers, we have observed the medical community, like society at-large, tends to view prematurity as a health event localized to infancy-something kids outgrow. Ironically, some pediatric providers report limited training and understanding of health complications for children born preterm, and little evidence exists regarding adult practitioners’ knowledge to care for these adults.
Preliminary adult primary care guidelines were recently created to screen and manage prematurity-related health complications.
Health risks from prematurity are also risks to equality and justice. Women who bear social risk factors are more likely to give birth early. This includes Black women, those living in socio-economically depressed areas, and women with two or more Adverse Childhood Experiences.
The many arms of racism and caste-based inequalities can complicate and worsen the health of people already at risk from preterm birth.
Attention also needs to be drawn to the prematurity research community. To date, research has focused on younger age groups and predominantly White populations. Future research needs to seek out ethnically diverse populations and comprehensively examine potential life course complications of early birth. This is especially important when considering how socioeconomic factors may influence the allostatic load of individuals.
For many born preterm, prematurity is not just a health concern, it’s a matter of who they are. Their perception of health over time, or health related quality of life (HRQL), is a critical outcome. To date, this evidence varies with age, degree of prematurity and reporter; clinicians and parents tend to rate HRQL more negatively than survivors.
Preterm-born individuals may not have event memories but, early birth repercussions can reverberate through family narratives and unique life experiences. Some identify as typically developed individuals who happen to have been born early, others as functional and well-adapted “preemies”, and others see prematurity as having colored their lives in negative ways.
As prematurity researchers, we aim to uncover and bring awareness to the health outcomes and risks from early birth. A critical need exists for more evidence about adult health following preterm birth and yet, how do we protect individuals with statistically increased risk without unnecessarily pathologizing them?
In clinical practice and research settings, we can take the opportunity to listen to people who were too young as patients to speak for themselves but have riveting and complex stories about preterm birth’s effects. We are aware of just one other published qualitative study about the experiences of adults born preterm.
Because most adult healthcare providers have yet to acknowledge and factor this experience into patient care, individuals born preterm are finding alternative avenues to be seen. Adults born preterm report seeking online community and support, connecting globally with people over shared early life experiences, while simultaneously making their needs and identities known.
As a research team, we strive to avoid labels for people born early but have nonetheless found that they are, in often subtle ways, a special group. They beat the odds as infants. Their birth and subsequent survival affected their families and communities in unprecedented ways. As clinicians and researchers, we can attend to the health risks of those born premature while acknowledging and celebrating their unique strengths and perspectives, often resulting from their early life experiences.
Source:https://www.thelancet.com/journals/lanam/article/PIIS2667-193X(22)00005-9/fulltext

Health Topics: Positioning

The muscle tone is defined as the strength or tension of the muscle. Due to their immaturity, preterm babies usually have a lower muscle tone compared to term born babies. Maintaining a position can be quite challenging for a preterm baby. Movements are sometimes jerky and disorganised. Comfortable, supportive positioning and handling of the baby are important for the development of the skeletal and muscle system. Optimised positioning also helps to minimise stress, to promote breathing, digestion, and circulation, to preserve energy, and to promote the development of crawling, standing and walking.
So called nests can be built by folding rolled-up sheets or bedding into a wide, thick band long enough to surround the baby. A nest provides the baby with boundaries with a surface to touch and brace against. These boundaries are similar to the situation in the womb which makes the baby feel more secure. At the same time, the nest can help to keep legs and arms in a developmentally supportive position.
Lying positions for the baby: There are different comfortable lying positions for the baby:
The supine Position:
The supine position (i.e. lying on the back) is often used, if babies are unstable and need to be observed regularly. It facilitates access to the baby, for example to initiate procedures if necessary. This position is also recommended to use at home to ensure safe sleep. The caregivers usually support the baby’s head, shoulders and hips with additional pillows under the head and the shoulders.
The lateral Position:
The lateral position (lying on one side) supports a flexed position with bended arms and legs and allows the baby to adjust his or her own position. Usually, shoulders are rounded and relaxed, legs are bent with boundaries and hands can reach the mouth and face more easily. This position is often used to reduce stress during caregiving activities (e.g. mouth care, nappy change, or tube feeding), medical procedures, and lifting).
The prone Position:
The prone position (lying on the tummy/breast) may improve oxygen saturation, respiratory function, digestion, and sleep. Babies may lose less heat and energy. However, this position should only be used when the baby is monitored continuously and should not be used at home due to the risk of Sudden Infant Death Syndrome (SIDS).
source:https://www.efcni.org/health-topics/in-hospital/developmental-care/positioning/
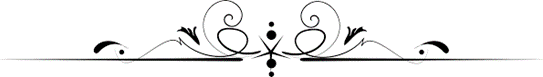

A Stay in Neonatal Care – Preparing to Take Your Baby Home
Oct 14, 2021
Funded by The NICU Foundation and created in partnership with The South West Neonatal Network, this animation was created to support parents, as they navigate their journey home following a stay in neonatal care with a premature or sick baby.


INNOVATIONS

Epidemiology of Retinopathy of Prematurity in the US From 2003 to 2019
April 13, 2023

Key Points
Question How have changes in the incidence of retinopathy of prematurity (ROP) varied across subpopulations and locations in the US between 2003 and 2019?
Findings In this cohort study of 125 212 ROP discharges from over 23 million births, there was an 86% increase in ROP incidence found among the at-risk population. Incidence was persistently higher with a relatively greater increase in newborns who were database-reported as Black race, born in lower-income households, or born in the South or Midwest.
Meaning This study found that ROP incidence nearly doubled in the US over the past 2 decades, particularly in traditionally underserved populations.
Abstract
Importance Retinopathy of prematurity (ROP) is a potentially blinding retinal disease with poorly defined epidemiology. Understanding of which infants are most at risk for developing ROP may foster targeted detection and prevention efforts.
Objective To identify changes in ROP incidence in the US from 2003 to 2019.
Design, Setting, and Participants This retrospective database cohort study used the Healthcare Cost and Utilization Project Kids’ Inpatient Databases. These nationwide databases are produced every 3 years, include data from over 4000 hospitals, and are designed to generate national estimates of health care trends in the US. Participants included pediatric newborns at risk for ROP development between 2003 and 2019. Data were analyzed from September 30, 2021, to January 13, 2022.
Exposures Premature or low-birth-weight infants with relevant International Classification of Diseases, Ninth Revision or Tenth Revision codes were considered ROP candidates. Infants with ROP were identified using relevant codes.
Main Outcomes and Measures ROP incidence in selected subpopulations (based on database-reported race and ethnicity, sex, location, income) was measured. To determine whether incidences varied across time or subpopulations, χ2 tests of independence were used.
Results This study included 125 212 ROP discharges (64 715 male infants [51.7%]) from 23 187 683 births. The proportion of premature infants diagnosed with ROP increased from 4.4% (11 720 of 265 650) in 2003 to 8.1% (27 160 of 336 117) in 2019. Premature infants from the lowest median household income quartile had the greatest proportional increase of ROP diagnoses from 4.9% (3244 of 66 871) to 9.0% (9386 of 104 235; P < .001). Premature Black infants experienced the largest increase from 5.8% (2124 of 36 476) to 11.6% (7430 of 63 925; P < .001) relative to other groups (2.71%; 95% CI, 2.56%-2.87%; P < .001). Hispanic infants experienced the second largest increase from 4.6% (1796 of 39 106) to 8.2% (4675 of 57 298; P < .001) relative to other groups (−0.16%; 95% CI, −0.29% to −0.03%; P = .02). The Southern US experienced the greatest proportional growth of ROP diagnoses, increasing from 3.7% (3930 of 106 772) to 8.3% (11 952 of 144 013; P < .001) relative to other groups (1.61%; 95% CI, 1.51%-1.71%; P < .001). ROP diagnoses proportionally increased in urban areas and decreased in rural areas.
Conclusions and Relevance This cohort study found that ROP incidence among premature infants increased from 2003 to 2019, especially among Black and Hispanic infants. Infants from the lowest-income areas persistently had the highest proportional incidence of ROP, and all regions experienced a significant increase in ROP incidence with the most drastic changes occurring in the South. These trends suggest that ROP is a growing problem in the US and may be disproportionately affecting historically marginalized groups.
Source:https://jamanetwork.com/journals/jamaophthalmology/article-abstract/2803759

A German study on the impact of stress on interparental relationship strain after preterm birth
A Reimer, L Mause, J Hoffmann, A Hagemeier, N Scholten
European Journal of Public Health, Volume 32, Issue Supplement_3, October 2022, ckac130.204, https://doi.org/10.1093/eurpub/ckac130.204
Published: 25 October 2022
Abstract
Background
Relationship satisfaction is an important predictor of well-being. Few studies address the effects of stress on interparental relationships of parents with preterm infants. However, the experience of a preterm birth represents an extreme, stressful event and therefore may place a strain on a relationship. Our aim is to examine the impact of postnatal stress on maternal and paternal perceptions of relationship strain.
Methods
As part of the Neo-CamCare project, a retrospective cross-sectional study was conducted targeting parents with infants with a birth weight below 1,500 g. Linear regression was used to analyse the influence of stress on relationship strain.
Results
437 mothers and 301 fathers participated. Data indicate that interparental relationship strain experienced by fathers (M = 2.61, SD = 1.46) is lower than strain experienced by mothers (M = 3.43, SD = 1.7). The stress level due to the infant’s behaviour and appearance is lower in fathers (M = 2.53, SD = 0.95) than in mothers (M = 2.98, SD = 1.05). Stress due to parental role change is higher in mothers (M = 3.37, p = 1.04) than in fathers (M = 2.49, SD = 0.99). Regression analyses show that stress due to behaviour and appearance, as well as parental role change, can be associated with relationship strain in mothers. For fathers, only stress experienced due to the behaviour and appearance can be associated with relationship strain, whereas parental role change is not significant.
Conclusions
Our data illustrate that relationship strain can result from stress in mothers and fathers, indicating the need for stress prevention measures for both. Only mothers show relationship strain due to stress in their parental role. Although it is unclear what mechanisms underlie these findings, we assume that the maternal role is still primarily associated with child care. One way to relieve maternal stress could be to increase psychological support and the promotion paternal involvement in the postnatal period.
Key messages
- Understanding the extent to which stress affects relationships helps to address mothers and father equally.
- Based on the findings, parent-centred interventions can be developed to manage relationship strains.
Source:https://academic.oup.com/eurpub/article/32/Supplement_3/ckac130.204/6766720?searchresult=1


The 14 Coolest Things Invented by Kids
Lisa Milbrand Updated: Jan. 20, 2023
You don’t have to be a grown-up to have a really great idea! Check out the amazing things the 18-and-under set dreamed up.
Inventions from imagination
Every time you eat a Popsicle, decorate a Christmas tree, or put on earmuffs, you can thank the creativity of a kid or teenager! These kids had some brilliant ideas about how to fix common problems—or just make things more fun!—and they made them a reality. Here are some things you see all the time that were dreamed up by kids.
Trampoline
If you love to bounce, you can thank George Nissen. At age 16, he invented the trampoline after watching trapeze artists drop into the safety nets beneath them. He thought it would be cooler if they could bounce out of the net instead. The trampoline turns 90 years old this year; it was invented way back in 1930. Find out the most famous invention from your state.
Makin Bacon
A lack of paper towels helped inspire Abbey Fleck to create a new way to make crispy bacon fast. When her family didn’t have paper towels to soak up the excess grease from microwave-cooked bacon one Saturday morning in 1993, the eight-year-old decided to figure out a better way to cook bacon. After a little trial and error, she came up with the Makin Bacon, a microwave safe stand that allows you to drape bacon over it as you cook. The bacon is able to crisp up while the bacon fat pools in a bowl underneath it. Her brilliant idea helped make her a millionaire as a teenager.
Earmuffs
In 1877, 15-year-old Chester Greenwood was tired of having cold ears when he went ice skating. So, he built a wire frame and had his grandmother help sew pieces of beaver skin to it to keep his ears warm. The muffs were a hit— especially with soldiers during World War I. Check out 20 other everyday things that were actually invented for World War I.
Christmas lights
Christmas trees used to be a big fire hazard, back in the day when lit candles adorned the trees. But in 1917, 15-year-old Albert Sadacca helped put an end to that by inventing less expensive strings of light bulbs to add pizazz to the holiday—without the potential for burning the house down. Get the inside scoop on some of the most ironic inventions ever.
Toy trucks
One of the very youngest inventors was Robert Patch, who was granted the patent for the toy truck when he was just six years old, back in 1963. He built his prototype out of bottle caps and cardboard, and his invention was meant to be taken apart and refashioned into different types of trucks, like a very early Transformer.
Popsicles
Like many amazing foods, Popsicles were created by mistake. Eleven-year-old Frank Epperson accidentally left a cup filled with soda powder, water, and a stirring stick on his porch overnight, where it froze—and the delicious dessert was born. Nearly 20 years after his accidental discovery in 1905, he started selling his sweet treats. Now, we eat more than 2 billion every year. In fact, Popsicles are one of the items whose brand name has become synonymous with the thing itself—we call all frozen fruit pops “Popsicles,” even though “Popsicle” is a specific brand. Not bad for an 11-year-old!
Superman
The Man of Steel was first imagined by a pair of 17-year-olds, Jerry Siegel, and Joe Shuster, in 1933 and made his first appearance in comics in 1938. Some comic book historians believe the origin of the idea came from the death of Siegel’s father Mitchell in an armed robbery at his store.
Hot Seat
Alissa Chavez was upset about the stories of children who died when they were accidentally left in hot cars—and she wanted to do something to help prevent it. In 2014, at age 14, she came up with the idea of the Hot Seat, a small cushion with a sensor that’s placed in the car seat and connects to the parent’s smartphone. If the cushion senses that the smartphone has moved more than 20 feet from the car with the baby still in the seat, it sounds an alarm. Here are some more inventions that have changed the world in the last decade.
Early television
One of the pioneers who helped bring us this life-changing technology was just 15 years old when he first dreamed it up. Philo T. Farnsworth created diagrams for an electronic television system in 1921, and it transmitted its first image six years later. Check out these world-changing ideas that came from dreams.
Water skis
At 18, Ralph Samuelson wanted to combine his passion for snow skiing with his love of the water and aquaplaning. In 1922, he built his first water skis from strips of wood by softening the ends and bending them up.
Magnetic Locker Wallpaper
If you’re big into locker decor, you can thank inventor Sarah Buckel for dreaming up this easy way to dress up your school storage back in 2006. As a 14-year-old, Sarah Buckel was tired of having to scrape her locker door clean of decorations at the end of every school year, so she came up with the idea of easy-to-swap Magnetic Locker Wallpaper instead. (It didn’t hurt that her dad was the chief operating officer of MagnaCard, which manufactured magnets!)
Snowmobiles
Joseph-Armand Bombardier, 15, strapped a car engine to four ski runners and a propeller to create the very first of these fun wintertime vehicles way back in 1922. He tinkered with it for years, before releasing the ultra-popular SkiDoo.
Swim fins
Noted inventor and Founding Father Benjamin Franklin was just 11 years old when he fashioned fins to make swimming easier. However, unlike today’s rubbery fins on your feet, his 1717 invention was hard paddles that were attached to your hands. Impress your friends with this bit of trivia next time you go snorkeling!
Source:https://www.rd.com/list/things-kids-invented/



Toadstools and Fairy Dust
Try, try again. She can make a magnificent thing if she puts her engineering mind to it and doesn’t give up. Please join us for a dramatic read of The Most Magnificent Thing by Ashley Spires read by Miss Jill.

Hang Gliding Kazakhstan & Russia Championships 2016

056 views Sep 12, 2016 Stepan Zubashev

Чемпионаты Казахстана и России по дельтапланеризму 2016 в г. Алматы. Pilots: Zubashev Stepan, Nurbek Koibulatov, Dmitry Testov, Alexandr Barvinsky, Elena Barvinskaya. August 2016, Kazakhstan, Almaty. Music: Paper Navy – Swan Song, Audionautix – Atlantis

